.jpeg)



.svg)
.jpeg)



.svg)
The Covid-19 pandemic revealed the limited understanding of immunity that most people have. There was so much ambivalence around the conversation of immunity, or the idea that your body has in-built mechanisms to prevent or limit an infection after catching the virus once.
Just like the rest of the systems in your body, your immune system works on feedback loops – if you serve it well, it will serve you well. So, let’s take a brief dive into this magical defense system and learn how to strengthen it with the right nutrition!
First, let’s understand that there are two types of immunity: innate immunity and acquired immunity. Your innate immunity is the one that you are born with; it is your body’s first line of defense against germs entering the body. It acts very quickly and has a similar response to all microorganisms. For instance, it takes only a few hours to detect and destroy any bacteria that has entered your body through a small wound.
Whereas acquired immunity takes over when the innate immune system is not able to destroy the germs. It consists of specialised cells that target the type of microbe that is causing the infection. It also has memory cells to remember the germs so that it can fight the infection when the pathogen hits again. This memory is also why you can catch some illnesses only once in your life.
However, the innate immune system still plays a crucial role to initiate and direct the adaptive immune responses, and to remove the pathogens targeted by them. Since the adaptive immune system takes 4-7 days to do its job, the innate immune response steps in to control infections during this period.
Most people associate weak immunity with just catching a fever or cold too often. But immunity is all-encompassing: feeling fatigued, having digestive issues like constipation, delayed wound healing, skin issues like psoriasis, eczema, and acne are also signs of a weakened immune system. These issues indicate that your immune system is having a tough time dealing with the toxins and pathogens in your surroundings. Now, let’s look at some ways in which you can boost your immunity!
Garlic enhances the functioning of the immune system by stimulating certain cell types that help fight viruses and other microbes. One of the most important components in garlic is allicin, which is known to be a powerful antioxidant and fight against several bacterial and fungal infections. Similarly, ginger acts as an anti-oxidant and the most relevant compound found in it is gingerol that exhibits antimicrobial and antiviral properties.
Vitamin D has the ability to regulate immunity through effects on both the innate and adaptive immune systems. Various immune cells contain vitamin D metabolizing enzymes and receptors. It also pairs well with vitamin A to boost immunity. Vitamin D3 is its naturally occurring form and is synthesized in the skin by exposure to sunlight. It is obtained in diet chiefly through fish liver oils and salt water fish. Make sure to soak yourself in the sun for at least 30 minutes a day and remember that sunscreen use also prevents the synthesis of vitamin D in the skin.
Vitamin C, E, and A act as powerful antioxidants and are known to enhance resistance against infectious microbes such as bacteria, viruses, and parasites. A lack of these nutrients in the diet can weaken the immune system, and ultimately, its ability to defend the body against diseases.
Food sources rich in antioxidants:
Zinc affects multiple aspects of the immune system, from the barrier of the skin to gene regulation within white blood cells (WBC) called lymphocytes. Zinc deficiency also affects the development of acquired immunity by inhibiting the growth and functions of certain WBCs. Some foods rich in zinc include beef, lamb liver, pork liver, chicken heart, turkey neck, crab, oysters, and lobster. Some vegetarian sources include beans, lentils, chickpeas and pumpkin seeds and zinc supplements. Make sure to have enough protein in your diet to enhance zinc absorption.
Keeping the gut healthy influences the immune system and virtually every aspect of your health. A diet rich in fiber and resistant starch, bone broth, probiotics and fermented foods, and a variety of colorful fruits and vegetables can help promote gut health.
Several mushrooms like lion’s mane and shiitake have immunological benefits. But if you are looking to specifically target the immune system, then reishi mushrooms are the way to go as they potentiate and stimulate the production of different immune cells in the body.
Including these foods in your diet along with enough movement and exercise can help you enhance your immune system. We will end this article with a pro tip - ensure your toxin levels are low as an overload of toxins in the body compromises the immune system. All in all, working on your health holistically can strengthen this master defense system in your body.
References:
https://www.ithrivein.com/blog/how-to-boost-the-immune-system
https://www.ncbi.nlm.nih.gov/books/NBK279396/
https://www.ncbi.nlm.nih.gov/books/NBK27090/
https://tv.greenmedinfo.com/10-natural-ways-boost-immune-system/
https://www.sciencedirect.com/science/article/pii/S0002916523006251
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4417560/
https://pubs.rsc.org/en/content/articlehtml/2022/fo/d1fo03180e
https://www.sciencedirect.com/science/article/pii/S2095754821000661
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3738984/




.svg)
Nature is full of rhythms. Day and night. The seasons. The ocean tides. Planetary movements. The lunar cycle. The song of a bird. The beating of your heart. Everything around us and within us follows a rhythm that keeps the natural world in balance and togetherness. While there exists a larger, universal rhythm that threads through all the natural entities of the universe, every entity on its own has a natural rhythm it has to adhere to. For example, the moon follows a cycle where it waxes and wanes over a period of 29.5 days. Plants follow the sun’s movement over a day to maximize photosynthesis and even follow rhythmic patterns of blooming. Crabs that live by the shore, adjust their living patterns based on the ocean tides.
Similarly, humans also have a biorhythm to follow, called the circadian rhythm. The circadian rhythm is the most significant biorhythm for all living organisms and sets the pace for biological processes to happen at regular intervals.
The word ‘circadian’ is derived from the Latin phrase ‘circa diem’ meaning ‘around the day’. Circadian rhythms are 24-hour cycles that are part of the body’s internal clock that runs in the background, enabling essential biological functions and processes. Different systems of the body follow different circadian rhythms, which means your body has multiple circadian rhythms that are all then synchronized with an internal clock in the brain. A very well-known circadian rhythm is the sleep-wake cycle that governs the states of sleep and wakefulness. Another example is the rhythmic changes in your body temperature over a 24-hour cycle. Factors such as light, darkness, colors, and other environmental factors can influence circadian rhythms. Circadian rhythms enable the brain to receive signals based on the environment and aid in the production of certain hormones, regulate your metabolism, and allow for the seamless functioning of certain biological processes. For example, circadian rhythm ensures that your digestive system produces digestive juices to match the typical timing of your meals.
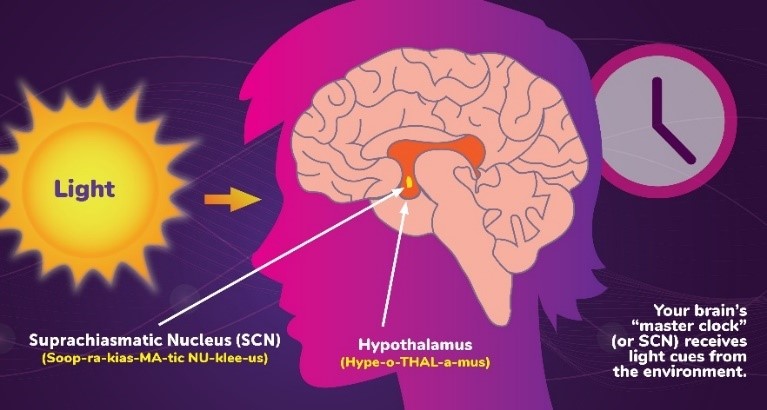
Circadian rhythms across the body are connected to the internal clock found in the suprachiasmatic nucleus (SCN) located in the hypothalamus of the brain. The SCN acts as the central pacemaker of the body’s circadian timing system and regulates most circadian rhythms in the body. While light affects the SCN to a great extent, other factors like temperature, social activity, and exercise can also impact the SCN thus influencing the circadian rhythms. [1]
As mentioned earlier, circadian rhythms are present in different systems of the body and play a role in the overall optimal functioning of your body. The most prominent circadian rhythm is the sleep-wake cycle and is perhaps the most studied as well. The SCN is receptive to signals of light and darkness. When morning light sets in, the optic nerves in your eyes send signals to the SCN which in turn triggers the release of cortisol and other hormones to help you wake up. When darkness sets in, the SCN sends signals to the pineal gland which triggers the release of melatonin which makes you feel sleepy and hit the sack. In this manner, the circadian rhythm aligns wakefulness and sleep with day and night and creates a cycle of stability and restorative rest that enables you to stay active during the day. [2]
When the Circadian Rhythm is disrupted, the optimal functioning of the body is disrupted as well. A disrupted sleep-wake cycle can
Recent studies have also identified disrupted sleep-wake cycles are potential contributors to obstructive sleep apnea (OSA), a sleep disorder marked by repeated lapses in breathing. OSA reduces the body’s oxygen levels and causes numerous sleep interruptions throughout the night. [3], [4]
In short, when circadian rhythms are disrupted, there are significant consequences to your overall health and productivity.
Circadian rhythms can be disrupted by singular/multiple events on a prolonged basis. Some of the commonly observed causes of circadian rhythm disruption are as follows: -
Having established the importance of the circadian rhythm, here are some ways to restore and maintain a healthy circadian rhythm. [5]
Bottomline, your circadian rhythm is fundamental to your body’s natural way of operating on its 24-hour body clock, thus adhering to its natural rhythm. Maintaining a healthy, active lifestyle in tandem with regular routines can help you maintain your circadian rhythm enabling better health.




.svg)
Contents from this article were shared in an article published in HerZindagi on 06.04.2023 featuring Mugdha. This article was written to serve as input for the same following a query from HerZindagi.
Low appetite is usually a sign of some kind of health issue. Women are supposed to consume approximately 2000 calories a day. Requirements vary from person to person and are higher if your physical activity level and muscle mass are higher. Our food environment today is such that we are all tempted to eat more since there is such a wide variety of highly palatable foods easily available. This is why the overwhelming problem today for the vast majority of people is the overconsumption of calories. In this situation, having a low appetite and struggling to eat more becomes a significant indicator of underlying problems.
The possible underlying reasons for it are vast and can be both physiological and mental. A comprehensive health assessment and root cause analysis is required to identify the problem. The most common problems include:
Gut issues: Gut issues, such as irritable bowel syndrome (IBS) or inflammatory bowel disease (IBD), can cause appetite loss by disrupting the normal functioning of the digestive system. This can lead to abdominal pain, nausea, and changes in bowel movements, all of which can decrease appetite. When the digestive system is not functioning properly and is under pressure, the body doesn’t feel like ingesting any food.
Thyroid and other hormonal issues: Thyroid and other hormonal imbalances can cause appetite loss by disrupting the normal balance of hormones in the body. Leptin, Ghrelin, and Cortisol are all hormones that play a role in regulating appetite. Leptin is a hormone produced by fat cells that helps to suppress appetite, while Ghrelin is a hormone produced by the stomach that stimulates appetite. Cortisol, a stress hormone, can also affect appetite by increasing cravings for unhealthy foods. When these hormones are out of balance, it can lead to changes in appetite.
Hypothyroidism, or an underactive thyroid gland, is a common cause of appetite loss.
Slow metabolism: A slow metabolism can cause appetite loss by reducing the body's energy needs, leading to decreased hunger and appetite. This is related to the previous point since it is commonly caused by low thyroid function and hormonal issues. It is also aggravated by aging and a sedentary lifestyle.
Psychological issues: Psychological issues can cause appetite loss by altering an individual's relationship with food and their perception of hunger. Anorexia is a mental health condition characterized by appetite loss due to the individual’s irrational obsession with being thin. Clinical depression is also very commonly associated with loss of appetite.
Loss of appetite is a serious issue and should not be ignored. One should seek immediate medical advice if the problem persists. Functional nutrition is one of the most sustainable treatments to rectify the root cause of chronic health conditions. With proper guidance and healthy lifestyle changes, anyone can reverse their problems and live a quality life.




.svg)
Contents from this article were shared in an article published in TV9 Hindi on 04.01.2023 featuring Mugdha. This article was written to serve as input for the same following a query from TV9.
Modern nutrition research can be very difficult to interpret. Studies that control food intake are very challenging to conduct and often create conflicting outcomes. Despite the conflicts, there are some things that we know to be true based on repeated evidence over the years. We share with you the basic principles of healthy eating based on medical and nutrition science literature and our own clinical data in 2023.
Eat whole unprocessed foods: Irrespective of what specific diet plan you follow, avoiding processed food is the first and foremost step to eating healthy. Industrial processing in most cases creates very harmful effects and such foods should be eliminated.
Eat adequate well-sourced protein: You should focus on getting a minimum of 0.8g of protein per kg of your target body weight Pasture-raised animal meat and eggs are the healthiest sources. Animal sources of protein are fully bioavailable(get absorbed in the body) and have a complete amino acid profile.
Eat Healthy Fats: Eating healthy fats like butter, ghee, and coconut oil, is important for overall health. These fats provide energy and support the absorption of fat-soluble vitamins and minerals. They play an important role in brain health, hormone and enzyme production, and immune function.
Avoid refined seed oils: Refined seed oils like soybean oil and sunflower oil are highly processed and may contain unhealthy trans fats and residues of solvents. They also contain high levels of omega-6 fatty acids, which can contribute to inflammation.
Avoid Refined Sugars: Consuming refined sugar can cause rapid spikes in blood sugar levels, which can lead to a range of health issues. These spikes can cause problems with metabolism, leading to weight gain and increased risk of metabolic conditions such as diabetes and heart disease. It is also recommended to not eat too many carbohydrates in general and focus more on proteins and fats.
Plant foods: Some amounts of plant foods are also important to consume because they have antioxidants and phytonutrients, which are plant compounds that have a range of health benefits. Plant foods also contain prebiotic fiber, which helps to support the health of the gut microbiome. While plant foods offer many health benefits, some plant foods can also contain toxins and anti-nutrients like lectins, and oxalates, which can have a negative impact on health. That’s why it is recommended to avoid plant foods high in anti-nutrients. Some food preparation methods like soaking and fermenting also help reduce antinutrient content.




.svg)
Boop boop poop. As much as we freely use those poop emojis on text, we shy away from talking about poop health. A sense of disgust and discomfort pops in every time there is a discussion on poop, or when your doctor questions you about your bowel movements. But let me tell you something – everyone poops, but not everyone enjoys great poop health and your poop can give away a whole host of information that can help a practitioner better assess your health. And so, my dear reader, let us dive deeper into the world of poop – not quite literally though.
Fecal matter or poop as we know it, is formed from the remains of the solid parts of food that are not digested in the small intestine, and have been broken down by bacteria in the large intestine. About 75% of fecal matter is just water. The rest of the 25% is a mix of fiber, protein, fats, live and dead bacteria, intestinal mucus, salts, a variety of other cells, and discarded cell parts in varying proportions. This mix of waste is pushed into your large intestine where it solidifies along with water until the defecation reflex starts wherein your rectal muscles contract causing you to poop.
Poop health is important because it can tell a lot of things about a person’s health. The color, shape, texture, smell, and time taken for a bowel movement are key indicators that determine your poop health. These indicators can help determine the following: –
Overall, your poop can tell you if there are any underlying, unidentified issues in your overall state of health – think infections, digestive issues, or even more serious issues such as cancer. Keep in mind that poop health is not a single indicator that can help determine a health issue, rather it is one of the many key indicators that should be used to determine a health issue. [1]
When it comes to poop, there is no single universal definition that indicates what healthy poop looks like. Just like you are unique, your poop is also unique. Regardless, a key indicator of a healthy poop is how easy it is for your stools to pass and regularity. Your bowel movement should not take more than a couple of minutes. In terms of regularity, you should have at least 1-2 bowel movements per day. [2] In addition, there are science-based tools that can help you understand if your poop falls in the spectrum of what is considered healthy poop. The most common tool used by medical professionals is the Bristol Stool Form Scale (BSFS). [3]
BSFS is simply a stool chart that categorizes faeces into seven broad categories based on the time taken for poop to form in your colon and its transit time through your digestive system.
If your poop looks more like type 1 or 2, it indicates constipation. Your poop in this case is usually hard, and difficult to pass through.
Types 3, 4, and 5 are considered healthy. While the texture across the 3 types are slightly different, they are more or less soft, and can easily pass through your intestines.
Types 6, and 7 without a doubt indicate diarrhea.
To summarize, anything other than types 3, 4, and 5 is considered unhealthy.

The color of your poop also indicates the health of your body. The normal color of your poop is brown, but you may also observe colors like green, red, white or black. [4]
Green-colored poop indicates that your food may have been digested too fast, or that you are eating a lot of leafy green vegetables, both of which are not cause for concern.
Yellow-colored poop indicates your gut isn’t absorbing nutrients from the food you’re eating and is finding it difficult to digest fats, both of which need intervention. Malabsorption is detrimental in the long run and needs to be addressed with a good supplementation of digestive enzymes, and changing your lifestyle and eating habits to improve the secretion of digestive enzymes.
Black-colored poop occurs usually when you consume too much iron, more particularly when you are on supplementation of iron. If that is not the case and you still observe black-colored poop, it warrants a visit to your doctor to rule out any case of bleeding.
White-colored poop indicates that your body is not producing enough bile or there is a gall-bladder obstruction. It could also mean the presence of a gut infection like Candida overgrowth or SIBO resulting in bile issues. Regardless, you need medical intervention if you continue to see white-colored poop.
Red-colored poop occurs when you consume a lot of red-colored foods such as beets, cranberries, tomatoes, etc. or it could be simply blood in your stool. This can indicate a gut infection or colon cancer and could be a serious issue, and hence needs to be looked at by a doctor.
Maintaining healthy bowel patterns starts with a healthy, happy gut. Here are some things you can incorporate into your everyday life to support healthy bowel patterns.
In conclusion, your poop can tell a lot about your overall state of health, and where you need to focus to shift to an optimal state of health. So, make sure to pay extra attention to your poop, and talk to your medical practitioner when you spot abnormalities.
.jpeg)



.svg)
The menstrual cycle is a natural occurrence in biological females. It is a monthly cycle of changes that the body goes through in order to prepare for pregnancy. The whole process of menstruation is different for individual female bodies. And due to the widespread lack of knowledge about this fundamental biological process, many women still need clarification about what is expected and what is abnormal about their menstrual cycle. So let’s dive into menstruation and related disorders to get a better understanding of what constitutes an abnormal cycle and to learn when you should seek help from a professional. While suffering, many women do not realise when to see a doctor because their condition has been left undiagnosed.
Menstrual disorders are characterised by disruptive physical and emotional symptoms that occur right before and during menstruation, such as severe bleeding, missed periods, and uncontrollable mood swings.
Your monthly period is part of your menstrual cycle, a sequence of changes in your body (ovaries, uterus, vagina, and breasts) that occur every 28 days on average. Some menstrual periods are slightly longer than others. The first day of your menstrual cycle is the first day of your menstrual period. The usual menstrual cycle lasts between five and seven days.
But not all biological females have a normal menstrual cycle, some might be undergoing irregular periods or irregular menstruation which might be a result of changes in hormone levels, stress, medication or some underlying health conditions and more.
Here are some of the common Menstrual Disorders that every woman should know about –
This disorder is the absence of menstruation during a woman's reproductive years. The reasons for this illness are numerous, and it can be divided into primary and secondary amenorrhea. This is not a life-threatening condition.
Primary amenorrhea is the lack of menstruation in a person who has not had a period by age 16. It is mainly caused by a disorder in your endocrine system regulating your hormones. This can occur due to low body weight caused by eating disorders, extreme activity, or drugs.
Causes of Primary Amenorrhea
Secondary amenorrhea refers to the absence of periods (3 or more in a row) in a female who has had periods in the past. It can be caused by problems that affect estrogen levels, including stress, weight loss, exercise, or illness.
Causes of Secondary Amenorrhea

This collection of physical, emotional, and behavioural symptoms occurs in most cycles during the last week of the luteal phase (a week before menstruation). The symptoms usually do not appear until at least day 13 of the period cycle and disappear within 4 days of the onset of bleeding. (2)
Some women get their periods with no or just minor symptoms of PMS. Others may experience PMS symptoms that are so severe that going to work or school becomes difficult. Severe PMS symptoms may indicate premenstrual dysphoria (PMDD). When you no longer have a period, such as after menopause, PMS fades away. PMS may return after pregnancy, although you may experience distinct PMS symptoms.
Premenstrual dysphoric disorder is far more severe than the typical PMS (Premenstrual symptoms). PMDD patients experience PMS symptoms (bloating, headaches, and breast soreness) in the weeks prior to their period. Symptoms can be alleviated with hormonal birth control and medications. Experts believe that decreasing levels of estrogen and progesterone hormone after ovulation and before menstruation may trigger the symptoms.
Signs of the conditions include:
Dysmenorrhea is characterised by intense cramping during menstruation. The pain starts in the lower abdomen and spreads to the lower back and thighs. It can be classified into Primary and Secondary dysmenorrhea.
Primary dysmenorrhea begins with your first period and continues throughout your life. It is typically permanent. It might result in severe and frequent menstrual cramping due to irregular uterine contractions.
Secondary dysmenorrhea is the pain caused by menstruation due to another medical or physical condition, like endometriosis or uterine fibroids. Other causes include uterine fibroids, pelvic inflammatory disease (PID), infection, tumours, or polyps in the pelvic cavity.
Some common symptoms of dysmenorrhea include
This disorder is characterised by heavy menstrual bleeding which lasts more than 7 days. Several factors can cause this condition. The average woman who is not undergoing menorrhagia sheds roughly 1 ounce (30 mL) of blood and changes her sanitary products 3 to 5 times daily during a regular menstrual cycle. Clot formation is also widespread and often menorrhagia is accompanied by dysmenorrhea as passing the large clots can be painful.
Causes of menorrhagia:
Seek the help of a healthcare professional if you think you experience the conditions mentioned above. A professional can examine your medical history to establish whether another medical condition causes a menstruation problem. For example, Appendicitis, Urinary Tract Infections, Ectopic Pregnancy, and Irritable Bowel Syndrome are examples of non-menstrual illnesses that can cause abdominal pain. Heavy bleeding and severe pain can be caused by Endometriosis and Uterine Fibroids.
This was all about some common menstrual disorders. In part 2 of this series, let's look at the diagnosis and treatment given for each of the aforementioned conditions.
REFERENCES:




.svg)
Before reading this article, ask yourself one fundamental question:
Who is responsible for your health?
It is this question that has split the realm of healthcare into two worlds for decades. On one hand, we have the Biomedical world, where the responsibility to treat and improve our illnesses lies entirely in the hands of healthcare professionals. Doctors, naturopaths, functional medicine doctors, alternative medicine practitioners, and the like.
Then there is the Biopsychosocial world, which posits that healthcare practitioners can help our health to a certain degree, but it is the collective onus of ours and our society to take care of ourselves and to create a socioeconomic atmosphere that is conducive to healing.
The healing journey does not end when you stop seeing your practitioner or taking medication – it begins at birth and ends at death. Health itself is treated as a spectrum, where a person moves between states of illness and wellness on a “health continuum”, instead of being unwell or well at one particular moment of time.
This seemingly logical argument has torn the world of healthcare in two because of one central factor: is illness only caused by external factors?
Let’s start by traveling back in time and looking at historical perceptions of illness.
Archaeologists have found skulls from the Neolithic period (10,000 BCE - 4,500 BCE) that have had holes drilled into them using stone tools, in a prehistoric surgical procedure we now call Trepanning or Trepanation.
It’s thought that the prehistoric humans of the stone age era would think of illnesses as the result of evil spirits being trapped inside their heads. This was also done to release pooled-up blood under the skull after a head injury due to hunting or falls, etc.(1)
Fast forward to the Ancient Greek era, and we distance ourselves from the idea of illness = evil spirits.
Hippocrates is now popularizing his theory of the 4 bodily fluids called humours – yellow bile, phlegm, black bile, and blood – which were influenced by the four elements of fire, water, earth, and air. The balance of these humours was thought to be regulated by conditions of hotness-coldness and dryness-wetness. It was believed that the balance or imbalance of these bodily fluids influenced a person’s health and temperament, and this theory of humourism became the crux of Western medicine for centuries. Eating foods that meet these categories of hot-cold/dry-wet and living in the right environment would affect one’s health.
Further developed by Galen, this theory led medical practitioners ranging from the ancient Greek era well into the medieval ages to associate mental symptoms such as anger, irrationality, depression, and other psychological problems as “illnesses”. Galen also associated the theory of bodily fluids with Plato’s theory of the tripartite soul, which stated that the soul is made up of 3 essential elements – spiritedness, wisdom, and desire.
In the Ayurvedic world as well, there was a similar theory of the Tridoshas (त्रिदोष) which stated that health was maintained by a balance of Vata, Pitta, and Kapha – the three doshas which corresponded with the elements of aether, fire, water, and earth.(2)
We come now to the Middle Ages.
In the Western world, religion was intertwined with the state, and dissecting the human body without explicit permission from a religious authority was banned. Medical knowledge (especially anatomy) had come to a standstill with the humoural theory having prevailed for 1400 years and practitioners having no way of actually looking inside a human body to find out what was going on.(3)
As a result, more and more people believed illnesses – especially seizures and mental illnesses – to be an act of the devil’s work. Their conventional forms of treatment (bloodletting, cupping, or leeching – based on the humoural theory) were deemed insufficient and treatment was often provided by monks who figured exorcism was the way to go. Treatment became a punishment; if you were ill, it meant you had lived a sinful life that let the devil in and now you must pay for it with your health. This was particularly so in the case of women’s health, as practitioners and monks alike took little to no interest in learning or even wanting to learn about this vital topic. Is someone behaving “oddly”? It’s probably demons. Burn the witch!(4, 5, 6)
[Unrelated (not-so) fun fact: Contrary to popular belief, both men and women were victims of witch-hunts, and execution styles were not limited to burning at the stake.
Yeah…it took a while, but healthcare eventually got back on track once “medical practitioners” stopped trying to exorcise illnesses out of people. Ultimately, Humourism was disproved in 1858 as the theory that microbes (germs) exist and could be causing illnesses gained more traction. The Ayurvedic Tridosha theory is still practised by many today. While the theory of bodily fluids may not be true in a literal sense, it brought attention to the fact that the world around us – especially the food that we eat – has a great impact on our health. This idea is now studied extensively in the field of Functional Medicine, where diet and lifestyle are used as primary treatments for diseases.
As Hippocrates rightly said, “Let food be thy medicine, and medicine be thy food.”
Long before modern medicine took over and wiped out any correlation of the world around us and our health, Galen had intertwined humourism with the Platonic concept of a tripartite soul, and this led to him achieving a greater understanding of the human body’s organs and systems. The Ancient Greek and Ancient Indian Ayurvedic theories of medicine correlated bodily fluids, natural elements, and a ‘soul’. This was, in its own way, an early holistic approach to health that was impeded only by the fact that the world lacked the fundamental understanding of anatomy as we know it today. We now know that it is blood that flows through veins, not air. But the correspondence of something in our bodies going wrong, causing something in our temperament or mental health to go wrong, based on the environment we live in, was an idea truly ahead of its time.(7, 8, 9, 10) The value of this core thought cannot be overestimated.
With the invention of the microscope and autopsies, as modern medicine took over, the holistic belief that the body and mind had anything to do with each other was ruled out, and in our opinion, this has dealt a significant blow to the progression of healthcare.
The Biomedical Model of Illness is the basis of all modern medicine. It includes multiple factors, the most pertinent ones being that
These postulates are where the biomedical model goes wrong.
The Biomedical Model states that all illnesses have a single, underlying cause (disease); reduces illness to processes of pathological interactions only, and health is achieved if the disease-causing agent is removed.(11)
It does not consider the impact of stress on the body. It ignores social and psychological processes which control the direct and indirect behaviours that can worsen or improve the health status of an individual. It prioritizes removing illness over maintaining health and does not consider that every individual has a unique body that requires unique treatment. It believes in a one-size-fits-all approach.
In summation, the Biomedical Model believes:
It is plain to see how this model of illness does not deserve to be the basis of all modern healthcare, as it has been for the past century.
It wasn’t until decades later, with advancements in medicine and psychology, that people began to notice correlations between increased mental stress and increased susceptibility to disease – especially chronic disease.(12) Prolonged periods of high stress with little to no control over one’s situation, and a lack of support systems demonstrated a physiological, observable effect on a person’s health. This focus on stress brought the world’s eye back to holistic approaches (finally).
A series of large-scale studies called the Whitehall Studies revealed that stress affects the heart rate, the neuroendocrine function, as well as the autonomous nervous system. These interactions could increase the risk of an individual’s likelihood of having a heart attack and developing other chronic diseases due to the high stress they experience on a regular basis. The lower the individual’s socioeconomic status, the higher the mortality rate from a wide range of diseases.
This study was conducted among British Civil Servants and it was found that they were more predisposed to chronic health issues than those who worked in superior positions, doing less work and in less stressful environments. It is thought that their higher social class and lower workload resulted in lower stress, which is why those in lower economic strata – working hard to earn money to subsist off of – were more likely to die of a heart attack than those who don’t need to work as hard to earn much more and live comfortably.(13) The behaviours of those in lower economic strata were also responsible for their health decline, such as smoking or alcohol consumption, which is driven by psychological factors.
In summation, the Whitehall Studies showed that social problems resulted in psychological stress which led to biological effects through nervous system responses and behaviors like smoking or drinking.

The Biopsychosocial model of health was put forth by George Engel in 1977. It considers biological, psychological, and social factors as the determinants of an individual’s health outcomes. Most people will hear about the Biopsychosocial model in psychology, particularly in Health Psychology – which is a field concerned with how psychology affects health, and vice versa. But this approach to healthcare utterly deserves much more attention in the mainstream because of its valuable insights and holistic framework.
The Biopsychosocial model considers:
→ Biological Factors
Such as pathogens, lesions, disease
→ Psychological Factors
Such as behaviour, belief systems, coping mechanisms, stress, pain
→ Social Factors
Such as class, ethnicity, employment status, environment, gender, age
This model puts forth some very important points about Public Health and that we – as a collective society – need to improve the standards of living, the mental health crisis – and as a result, the biological health – of individuals. It suggests that psychosocial stress resulting from an individual’s living situation, such as workplace, workload, support system, socialization (or lack thereof), income, environment, and lifestyle factors like diet, exercise, substance abuse, etc., have an impact on his/her physical health, and not just pathogens or other agents of disease.
It is a useful framework or concept to consider when practicing healthcare, especially in the case of chronic diseases that often tend to have multiple root causes working together. These root causes are physiological issues, such as chronic inflammation, organ dysfunction, nutritional deficiencies, etc. But these root causes are themselves caused by other factors like diet, which is influenced by psychological health, which is influenced by social health.
This model also propagates the idea that for an individual to be truly healthy, they need to continue taking care of their health even outside of a professional healthcare space i.e., even when not seeking treatment from a professional.
The individual needs to recognize the kind of behaviours that are worsening their health and stop engaging in them, such as smoking, drinking, poor dietary habits, and thrill-seeking behaviours (rash driving, and self-harm in some cases).
The individual is responsible for their own behaviour and surroundings. It is our own responsibility to identify harmful and toxic situations, and then take the necessary steps to correct them for the sake of our health. Prolonged mental stress can manifest itself as physical problems through brain-body pathways. The Hypothalamic-Pituitary-Adrenal Axis (HPA) is one such example of a brain-body pathway that demonstrates the human stress response.(14) By handling our mental stress levels, we can help our bodies stay healthier.
In summation, contrary to the Biomedical Model of Illness, the Biopsychosocial Model of Health believes:
This model brings the main focus of healthcare back to the patient and goes back to a health approach where the effects of the mind on the body are not ignored. It is a far more inclusive framework, that can help to improve the mental health crisis that’s gripped the world for decades. The monster of chronic diseases continues its rampage unchecked, and one of the biggest reasons healthcare practitioners have failed to bring improvements is the huge ignorance of how socio-psychological factors affect our lives. Improvements in social qualities and living standards will inevitably bring about improvements in psychological well-being, which has an indubitable impact on our physical health.
At every level, since ancient times, the responsibility for treatment and healthcare has been in the hands of professionals who refused to acknowledge that what they believe in could possibly be erroneous. Often, conventional systems get so firmly set in place that even when budding new ideas that could bring about massive improvements do come up, they are invalidated and shut down due to the obstinate refusal to let go of convention. The result? The patients suffer at the hands of people who refuse to let go of tradition and problematic belief systems.
Those deeply rooted in the system cannot realize that the system is problematic.
How can something that’s been the norm for centuries be wrong? Well, it can. Scientific thought is built on the foundation of questioning beliefs and proving and disproving theories. Man is a fledgling in the cosmos, learning about everything as he goes along.
And historically, this realization has come at a costly price –
Hungary, 1840s: Ignaz Semmelweiss and other doctors are noticing a worrying increase in the mortality of new mothers. They performed multiple autopsies to investigate, but found no relevant answers. The next day, they would help more mothers deliver babies, only for those mothers to pass away. This fatal sickness was called “childbed fever”, or puerperal fever. Doctors did not know how to help young mothers avoid this death sentence.
When Ignaz Semmelweiss – now known as the “saviour of mothers” – told the doctors that the prevailing system of patient care was the reason dozens of new mothers were dying, the entire medical industry ostracized him.
Semmelweiss had immersed himself in the study of this fever and noticed that doctors, after performing autopsies on patients who died of childbed fever, would perform child deliveries the next day. He theorized that disease-causing microbes are spreading from patients to doctors, and from doctors to new patients. He suggested that doctors should wash their hands with a chlorinated lime solution in between and after patient care.
His idea was considered outrageous. How could these esteemed doctors with years of experience in medicine be the cause of patient death?
The medical industry refused to give any credit to his ideas. His peers rejected him, and he lost his medical license. He was kicked out of his field, while doctors continued to tend to patients without disinfecting themselves, causing more deaths.
Semmelweiss succumbed to the pressure of society’s rejections and lost his mind. He was admitted to an asylum, where he eventually lost his life. He did not have the opportunity to learn that he was right, and centuries later, the world of patient care now revolves around his crucial discovery.
“When I look back upon the past, I can only dispel the sadness which falls upon me by gazing into that happy future when the infection will be banished...The conviction that such a time must inevitably sooner or later arrive will cheer my dying hour.”
– Semmelweiss.
The current world of healthcare needs a revolution. It is based on century-old beliefs that deprive us of the healthcare we deserve. By the time errors are discovered and fixed, it is usually too late. It takes a disaster for those in the system to learn that the system is faulty.
The Biomedical Model needs to be integrated with the Biopsychosocial Model to create a new model of healthcare, where unique patients receive unique treatments, on a holistic level that considers their sociological, psychological, and biological factors. The patient-practitioner relationship needs to be personalized for the best results.
We are hopeful that as knowledge becomes more easily accessible, as developments are made in the fields of medicine and psychology, the developments yet to come will hold great promise for those of us who will be at the receiving end of treatment. And we are excited to see the start of a beautiful health-revolution where everyone comes out happy, healthy, and thriving.
Other references:




.svg)
We know the word itself might make you pause and raise an eyebrow, but fear not! We're here to debunk any myths surrounding this process and make it as relatable as we can. Grab a coffee, settle in, and join us as we embark on an interactive journey to learn more about hysterectomy, including what it is, why women might need one, and what it means for our bodies and lives. Prepare to embrace your curiosity because, as a team, we can overcome this obstacle because knowledge is power.
A hysterectomy is a significant surgical procedure that removes the uterus and, in some cases, additional reproductive organs like the ovaries and fallopian tubes.While this surgery may appear intimidating, it is critical for women to have a thorough awareness of the operation and its repercussions. Women must understand the procedure in order to make educated decisions about their health. Almost 6% of the women population in India of age category 39-45 has undergone this surgery. Significant physical and psychological side effects of hysterectomy can include altered hormone levels and potential effects on sexual function. Therefore, before having this surgery, women must talk to their healthcare provider about alternative treatments and possible risks. To ensure a speedy recovery, post-operative care and recovery procedures should also be carefully followed. Women can successfully navigate this with the right information and assistance 1.
Hysterectomy is recommended for various medical conditions that affect the uterus. Some of these conditions include uterine fibroids, endometriosis, adenomyosis, and certain types of cancer. Other factors like an unbalanced diet, eating canned food, following a sedentary lifestyle, smoking, consuming alcohol etc., can bring adverse effects to the reproductive organs thus leading to a need for surgery. Women who experience heavy or prolonged menstrual bleeding, pelvic pain, or other symptoms that significantly impact their quality of life may also be candidates for a hysterectomy.
Non-cancerous growths called uterine fibroids can grow inside the uterus and cause pain, heavy bleeding, and pressure on nearby organs. In endometriosis, the tissue that normally lines the uterus expands outside of it, causing excruciating pain and impairing fertility. Adenomyosis, which causes painful periods and copious bleeding, happens when the tissue lining the uterus grows into the muscular wall. Hysterectomy may occasionally be suggested as a treatment for specific cancers, such as uterine or cervical cancer. A hysterectomy is also an option for women who have tried other treatments for their symptoms but have not experienced relief to enhance their quality of life 2.
There are various hysterectomy procedures, and the selection of one depends on the underlying condition, the patient's general health, and the surgeon's experience. Vaginal hysterectomy, laparoscopic hysterectomy, and total abdominal hysterectomy (TAH) are the three primary hysterectomy procedures 3.
The uterus is removed through the vagina during a vaginal hysterectomy and it is a minimally invasive procedure. A shorter hospital stay, a quicker recovery, and minimal scarring are just a few benefits of this kind of surgery. Women who have a normal-sized uterus and no significant pelvic adhesions are typically advised to have a vaginal hysterectomy. When there are no additional complicating factors and the uterus is not noticeably enlarged, it is frequently the preferred option.
Women with certain medical conditions or previous surgeries that make the procedure more difficult may not be candidates for vaginal hysterectomy 4.
A laparoscope, a thin instrument with a camera, is inserted through tiny abdominal incisions to perform a laparoscopic hysterectomy. With the help of this method, the surgeon can see the uterus and its surrounding structures without making a significant incision. Laparoscopic hysterectomy advantages include less scarring, a shorter hospital stay, quicker recovery, and reduced postoperative pain. But not all women are good candidates for this procedure, and the surgeon will take into account things like the patient's general health, the size of the uterus, and the presence of adhesions. However, it might not be appropriate for all patients, particularly those with significant fibroids or pelvic adhesions 5.
A lower abdomen incision is used in the traditional surgical procedure known as a total abdominal hysterectomy (TAH) to remove the uterus. This kind of hysterectomy enables the removal of larger uterine fibroids or other pathologies and gives the surgeon a clear view of the pelvic organs. When vaginal or laparoscopic approaches are impractical or when additional procedures, like the removal of the ovaries or fallopian tubes, are required, TAH may be advised.
Compared to minimally invasive procedures, recovery from TAH typically takes longer, and there may be more postoperative discomfort and scarring 6.
A radical hysterectomy is a surgical procedure for gynecologic cancers, such as cervical or ovarian cancer, that have spread outside the uterus. In this extensive procedure, the uterus, cervix, upper vagina, and nearby lymph nodes are removed. A radical hysterectomy, which removes all cancerous tissue, is frequently combined with other therapies like chemotherapy or radiation. Gynecologic oncologists should be consulted by women who have been diagnosed with gynecologic cancer in order to determine the best course of treatment, which may entail a radical hysterectomy 7.
Hysterectomy carries some risks and potential complications, just like any surgical procedure. These include the potential for infection, bleeding, harm to the organs in the area, blood clots, and unfavorable anesthetic reactions. Before making a choice, it is crucial for women to discuss these potential risks with their healthcare provider and fully comprehend the advantages and disadvantages of the procedure. Women should also be aware of the possible long-term consequences of hysterectomy, including hormonal changes and the impact on sexual function 8.
The time it takes to recover from a hysterectomy can vary depending on the procedure's particulars and the patient. It's critical for women to adhere to postoperative recommendations from their healthcare provider and take the necessary actions for a speedy recovery. This might entail taking the recommended medications, increasing physical activity gradually, and avoiding strenuous exercise or heavy lifting during the first few weeks of recovery. In addition, women should prioritize their own needs by getting enough sleep, eating a balanced diet, and seeking out emotional support when necessary. The secret to a successful recovery is patience and realizing that the process takes time 9.
While a hysterectomy may be necessary in certain cases, there are alternative treatments that women can explore before opting for surgery. These alternatives may include hormonal therapies, uterine artery embolization, endometrial ablation, or other minimally invasive procedures.
Functional nutrition approaches include having foods rich in Vitamin C like strawberries and blueberries as well as consuming lean meat during the recovery period or even for maintaining the condition of the uterus. It is important for women to consult with their healthcare provider to discuss the potential benefits and limitations of these alternative treatments and determine if they are suitable for their specific condition 10.
For many women, having a hysterectomy can be an upsetting and difficult experience. Finding resources and support is crucial to completing this journey successfully. Women can turn to friends, family, or support groups designed especially for those undergoing hysterectomy for assistance. Women can connect with others who have had the procedure through a variety of online forums and resources. Asking open-ended questions and communicating honestly with medical professionals can also yield useful knowledge and support 11.
A hysterectomy is a significant medical procedure that can significantly enhance many women's quality of life. Women can take control of their health and make informed decisions by learning about the various hysterectomy procedures, the risks and side effects associated with them, and the available alternative treatments. To ensure the best outcome, it is essential to speak with healthcare professionals, look for emotional support, and gather pertinent data. Giving women the knowledge and tools they need to make the best decisions for their wellbeing is essential.
Speak with a health professional to go over your options and determine the best course of action if you or someone you know is thinking about having a hysterectomy. Always keep in mind that information is a powerful tool when it comes to making decisions about your health.




.svg)
With all the noise from the holistic health influencers on Instagram, I am sure you are no stranger to the term ‘autoimmune disease’. But it’s very likely that you are a stranger as to what an autoimmune disease really is, and how functional medicine aims to reverse an autoimmune condition, so, let me demystify that for you.
Clinically, an autoimmune disease is one where your immune system mistakenly attacks the healthy cells of your body. While this definition can translate to mean that your body is devoid of any sort of threats – think of allergens, toxins, microbial (bacterial/viral/fungal) infections, etc., that would be a grossly inaccurate interpretation. Your immune system does not react unless there is a perceived threat. When there is a perceived threat, your body does everything in its power to adapt and survive in a hostile environment. During this, it ends up attacking your skin, joints, brain, and perhaps even your whole body. This mechanism is called molecular mimicry by which infectious agents (or other exogenous substances) trigger an immune response against the host antigens (i.e., foreign matter that the body does not recognize).
As of today, around 80 diseases have been identified as autoimmune diseases, and an estimated 4% of the world’s population is affected by one or more of them. Some of the common autoimmune diseases are rheumatoid arthritis, lupus, psoriasis, celiac disease, Addison’s disease, Crohn’s disease, Sjögren’s syndrome, etc.
The conventional approach to treating autoimmune diseases works simply by mitigating symptoms with the administration of steroids, anti-inflammatory drugs, analgesics, and/or immunosuppressant drugs. This approach temporarily helps with your symptoms by stopping the pain signals from being sent to the brain and suppressing the immune system. It essentially shuts down the signals from your body that indicate that something is wrong and does not actually resolve the root cause of the issue. Additionally, the usage of anti-inflammatory drugs and immuno-suppressants can potentially cause intestinal bleeding, kidney failure, depression, psychosis, osteoporosis, muscle loss, and diabetes, not to mention overwhelming infection and cancer. So while you will experience a state of no symptoms over time, that doesn’t necessarily translate to your body having been healed. The root cause of your autoimmune disease persists in your body and chances are that it may evolve into something else that manifests with a whole new different set of symptoms.
When it comes to treating diseases of any kind, conventional medicine approaches diseases by suppressing, covering over, blocking, or otherwise interfering with the body’s biology. There is no attempt made to understand and address the underlying cause, which is usually one or more of these – infections, poor liver functioning and/or gut health, stressed nervous system, food allergies, sensitivities, chemical and heavy metal toxicities, hormonal imbalance. These imbalances, foreign bodies, toxic substances, etc., are perceived as threats by the human body and the body indicates that something is wrong in the body via pain, neurological symptoms such as fatigue, depression, insomnia, anxiety, mood fluctuations, etc., digestive symptoms such as constipation, indigestion, etc. and skin & hair symptoms such as psoriasis, eczema, hair loss, etc. ultimately throwing the body out of balance.
While conventional medicine treads on shallow waters, functional medicine asks 2 key but simple questions and dives deeper into understanding the disease – a) Why is the body out of balance? b) How do we help the body regain its balance/homeostasis?
By asking and answering these two questions, a functional medical practitioner helps identify what perceived threat your body is reacting to, develops an individualized protocol to remove that threat, and restores homeostasis. Functional medicine views the human body as a system on its own, seeks to find the cause of illness, understands the fundamental functions of the different systems that make up the human body, how they can go askew, and how to bring them back to balance, and understands the different interconnections between symptoms, organs and functions. Functional medicine also takes a far more holistic approach in that it takes into account factors such as genetics, and environmental factors to paint a clearer picture of all possible causes and develop healing protocols that work best for you.
As a first step, your functional medicine practitioner prescribes a diagnostic assessment to detect key pathogens resulting in autoimmune diseases, along with a blood work to identify any deficiencies. This diagnostic tool helps
Your functional medical practitioner will also ask you questions to understand your medical history, overall medical conditions, diet, lifestyle, etc. to get a complete sense of what may be going on with you. Once they have all of this information, in combination with the results of your diagnostic assessments, they will then prescribe a protocol that works on detoxing, healing, and supplementing any deficiencies. Detoxing helps eliminate any pathogens and toxins that are perceived threats to the body. This involves a combination of natural anti-microbial, anti-viral herbs that are chosen based on the outcomes of the diagnostic assessment, along with binder agents to help flush them out of your system. In addition, you will also work on shifting to a healthier lifestyle by including exercises, relaxation practices, and getting sufficient sleep. You will also have to adopt a diet protocol where you identify and remove any food sensitivities and eat more cleaner, healthier foods. Supplementation involves supplementing certain nutrients that your body is deficient in, and that you are unable to get from food. Typically, in the case of autoimmune diseases, it is a vitamin D3, or a B12 deficiency, however, it is not limited to either of them.
After the protocol is kicked off, you are monitored on a periodical basis to measure progress and modify protocol as needed.
The Functional medicine approach of addressing root causes, in almost all cases, is able to put the autoimmune condition into remission. A lot of factors determine the degree of remission – the severity of the condition, the damage caused, your practitioner’s accuracy of diagnosis and strength of treatment protocol, and most importantly, your conviction to make the necessary changes to your lifestyle, routine, and stay committed to the treatment protocol for as long as needed. The functional medicine approach to autoimmune diseases drastically improves the quality of your life, reduces your symptoms, and helps you get back to living your life in the best possible way.


The blog covers functional nutrition, chronic conditions, gut health, hormonal health, autoimmune conditions, sleep, mental health, and root cause analysis. Every article is written to help you understand what is actually happening inside your body, not just manage symptoms.

All articles are written by the content writers in collaboration with iThrive's clinical team of functional nutritionists, guided by the same methodology used in the ALIVE programme. The content is rooted in functional medicine and real clinical experience, not generic health advice.

No. The blog is an educational resource to help you understand your health more deeply. If you are experiencing symptoms or managing a chronic condition, a personalized Root Cause Analysis with a functional nutritionist is the right next step.

Book a Root Cause Analysis. For ₹2,500, a dedicated functional nutritionist will assess 60+ blood markers using optimal ranges and explain exactly what is driving your condition. It is the natural next step after reading about what might be happening in your body.

Yes. Many of our readers come with existing diagnoses and find the blog helps them understand why their condition developed and what their body actually needs. The articles are designed to give you clarity, not replace the guidance of a practitioner.



