



.svg)




.svg)
If you’ve been told that you have autoimmune gastritis, there is a chance you have already tried eating bland, avoid spicy foods, or even survive on tea and toast for weeks. Yet the heaviness, bloating, constant fatigue, strange hunger pains, and burning keeps coming back. Some of you also notice that your gastritis gets worse when hungry. Others feel terrible after consuming alcohol, foods they thought were healthy, or dairy. That is because autoimmune gastritis is not just “an irritated stomach”. It is rather an autoimmune condition in which the body itself attacks the parietal cells of the stomach. These are known to be the very cells that are responsible for making stomach acid and intrinsic factor, the protein that is required for the absorption of vitamin B12. Over time, this develops a vicious cycle. You can’t digest food appropriately, you become deficient in key nutrients, the stomach lining also gets weaker, and the immune system becomes much more reactive.
Here at iThrive, we often see clients who have spent years and years treating symptoms while missing the real trigger. They have been prescribed antacids, told to avoid chilli, and lastly sent home. But nobody explained exactly and due to what reasons gluten, conventional dairy, refined oils, processed foods, and hidden gut inflammation keeps the immune systems switched on.
One thing for sure is that gastritis can heal. But healing autoimmune gastritis needs much more than just removing a few foods. It also needs adequate understanding of which food continues to trigger the immune attack, what the stomach actually needs to repair itself, and which supplements can bypass the problems of absorption developed by the condition itself.
Unlike temporary gastritis or simple acidity after an infection, autoimmune gastritis has a much deeper root cause. The immune system has become confused. It begins attacking the stomach lining as if it were a threat. Many of the foods commonly eaten every day can make this worse as they increase intestinal permeability, also called leaky gut.
When the gut lining becomes more permeable, food proteins can cross into the bloodstream before they are completely broken down. The immune system reacts to these proteins, and in few people, those proteins look surprisingly similar to the stomach tissue itself. This entire process is known as molecular mimicry.
That is why a true autoimmune gastritis diet plan isn’t only about avoiding irritation. It is rather about reducing immune confusion.

If there is one food group that deserves entire removal in auto mind gastritis, it has to be GLUTEN. Barley, rye, and wheat contain a protein called gliadin. Gliadin has been observed to damage the intestinal barrier and then stimulate inflammatory immune responses.
Many of you with autoimmune gastritis notice that your heaviness, upper stomach discomfort, brain fog, and bloating improves drastically within a couple of weeks of eliminating gluten entirely. Even small amounts can continue to trigger the immune response. This involves breads, pasta, sauces, bakery products, biscuits, and hidden gluten in packaged foods.
This is why one of the very first recommendations here at iThrive is a strict trial without gluten for at least 8 to 12 weeks. For many of you, it is the first time they realise how much a “normal” food was quietly making them feel unwell.
Many of our clients ask us, “If I have gastritis, what can I eat?” and presume curd, paneer, and milk are safe as they seem to be soft and soothing. But conventional dairy mostly contains A1 casein, a protein that can behave very similarly to gluten in sensitive people.
A1 casein might stimulate inflammatory chemicals and worsen digestive distress. For someone whose stomach lining is already under attack, this can further make the symptoms more persistent. Few of you also witness that you’ll feel more nauseous, heavy, or bloated after milk based foods even if you are not lactose intolerant.
For this very reason, most of you with autoimmune gastritis do better avoiding conventional milk, processed cheese, flavoured yoghurt, and commercial dairy for a period of time. Some of you might also tolerate small amounts of ghee because it contains almost no casein. Others may do better with goat milk or A2 dairy later in the healing process, but only after the gut has calmed down.
There is a major reason why many of you with gastritis feel worse after packaged snacks, sugary drinks, sweets, or bakery foods. Refined sugar feeds inflammatory bacteria and yeast inside the gut. It also causes sudden blood sugar spikes, which in return increases stress hormones and inflammation.
Ultra processed foods contain a lot of additives, preservatives, artificial flavours, gums, and refined flours that put even more pressure on a digestive system that is already damaged. These foods don’t provide the nutrients that are needed for repair, rather they simply increase irritation.
If your stomach burns more when hungry, it can be tempting to grab biscuits or something quick. Unfortunately, these foods often make the cycle even worse. They may give you temporary relief, but they keep inflammation going beneath the surface, so beware.
One of the major overlooked foods to avoid with autoimmune gastritis is refined seed oils. Soybean oil, sunflower oil, canola oil, and corn oil are found in the majority of packaged foods, restaurant meals, as well as fried snacks.
These oils are rich in unstable omega 6 fats that are easily damaged inside the body. When this happens, they develop compounds that increase inflammation and weaken the cell membranes.
Most of our clients in the start are often surprised to learn that even “healthy” foods can become problematic if they are cooked in these oils. Replacing them with ghee, coconut oil, or good quality A2 butter can make a noticeable difference over time.
If you have noticed worsening gastritis when drinking alcohol, you aren’t just imagining it. Alcohol directly irritates the stomach lining and then increases intestinal permeability. It also interferes with the ability of the liver to store and activate eminent nutrients like B vitamins.
For someone with autoimmune gastritis, even smaller amounts of alcohol can slow healing. This is specifically true if you already struggle with low B12, iron deficiency, fatigue, or nausea. One of the hardest parts of healing is accepting that some foods are not “just occasional treats” for your body anymore. If you are trying to truly heal gastritis, alcohol often needs to be removed completely for a period of time.

Once you hear what you actually need to avoid, you often feel very overwhelmed. You might also reconsider thinking “what is left?” But the goal isn’t a restriction forever. The goal is to give your stomach the environment it needs to repair itself.
An autoimmune gastritis diet plan should always focus on simple, nutrient dense foods that are quite easy to digest and very rich in the building blocks needed for healing.
Your stomach lining repairs itself utilizing amino acids, healthy fats, and minerals. This is why most of you do better when each meal includes quality protein like chicken, slow cooked meat, wild fishes, free-range eggs and lamb.
Organ meats, specifically liver, can prove to be extremely powerful if you can tolerate it because they naturally contain vitamin A, B vitamins, iron, and folate. Healthy fats like ghee, coconut oil, avocado, and olive oil are beneficial as it helps calm inflammation and offer stable energy.
Many of you with autoimmune gastritis feel extremely exhausted because you are literally surviving on tea, plain rice, and crackers. The body can’t ever heal without nourishment.
The best carbohydrates for gastritis to heal are the ones that are easy on the stomach and less likely to spike blood sugar. Cooked veggies, pumpkin, ripe banana, a very small amount of raw honey, sweet potato, rice, and berries are usually easier to digest.
If you want grains, choose naturally gluten free options like ragi, jowar, bajra, and white rice. Ideally these should be well soaked or fermented because then it reduces the compounds that makes digestion harder.
People with autoimmune gastritis are often very low in magnesium, B12, zinc, and selenium. Foods like seafood, leafy greens, one Brazil nut a day, and cooked cruciferous vegetables can help replenish these nutrients.
Broccoli, onions, garlic, and cabbage might also support the natural detoxification process of the body, specifically when cooked well. They are often gentler on the stomach when eaten in stews, soups, or broths rather than raw.

As autoimmune gastritis damages the very cells that are responsible for nutrient absorption, food alone isn’t enough. This is exactly where the right supplements can make a significant difference.
One of the major dangers of autoimmune gastritis is vitamin B12 deficiency. Without intrinsic factors, the body cannot absorb B12 appropriately from food. Over time, this can also result in tingling, memory issues, nerve damage, fatigue, anxiety, and even hair fall.
This is exactly why you need sublingual B12 or, in more serious cases, B12 injections or IV support. Here at iThrive, this is mostly one of the very first deficiencies we look for because correcting it completely changes how someone feels.
Zinc is quite essential for the health of the gut lining. Forms like zinc glycinate or zinc carnosine are specifically useful because they support tissue repair and reduce irritation.
Many people with gastritis have been deficient for years without even realising it. You might have poor immunity, white marks on your nails, slow healing of wounds, and a very low appetite. Restoring zinc can be beneficial for the stomach as it will begin to repair itself.
Vitamin D isn’t just important for bones. It is one of the most powerful immune regulators for the body. When levels are low, the immune system is more likely to stay stuck in an overactive state.
Vitamin D3, specifically when paired with K2, can be beneficial as it guides the immune system away from attacking healthy tissue. This doesn’t work overnight, but over time it can surely become an eminent part of how gastritis can be cured at the root.
BPC 157 is a peptide that is originally derived from a protective protein found in the stomach. It has gained a lot of attention because of its ability to support the repair of the gut lining and also reduce inflammation.
Some of our clients have had years of burning, food sensitivity, and pain and they noticed a lot of improvement when it was utilized correctly as part of their complete healing plan.
One of the strangest things about autoimmune gastritis is that you might feel both burning as well as poor digestion at the very same time. That is because many of you actually have too little stomach acid, and not too much.
Digestive enzymes and herbal bitters can be beneficial for breaking down food more effectively. This often reduces the burping, heaviness, and uncomfortable fullness after meals.
Certain soil based probiotics might help in improving the balance of bacteria inside the gut. Black cumin seed oil well combined with raw honey also supports people who have underlying H. pylori related irritation.
However, this is truly where personalisation matters a lot. Not every probiotic suits every person, and not every supplement should be taken blindly. What works beautifully for one person might irritate another.
Perhaps the most frustrating thing about autoimmune gastritis is how different it actually looks from one to the other. One might tolerate eggs, another might feel terrible when hungry, another struggles during pregnancy and wonders about gastritis when pregnant, and someone just notices symptoms after alcohol.
That is why healing cannot come from a generic food list that is copied from the internet.
Here at iThrive, we focus on identifying the deeper pattern. Is there hidden gluten sensitivity? H. pylori? Severe B12 deficiency? A gut microbiome issue? Are you under-eating protein? Are you so afraid of food that your body is now running on stress alone?
Sometimes the most healing thing is finally understanding that your symptoms make sense.
If you feel like you have been trying everything and still don't know what to eat, this is the right time to Book a Root Cause Analysis or Book a Free Consult. The goal is not simply to manage symptoms, it is to understand why your stomach stopped feeling safe in the first place.
For the ones that need deeper support, the iThrive Alive 3 Months Program is specifically designed to help you rebuild digestion, calm the immune system, restore nutrient levels, and finally develop a food plan that works for your body.
Autoimmune gastritis does not heal because you avoided spicy food for a week. It heals when you remove the foods that keep triggering the immune system, repair the gut lining, and restore the nutrients your body can no longer absorb properly. Gluten, conventional dairy, alcohol, refined sugar, processed foods, and seed oils are often the biggest obstacles. At the same time, targeted support through protein rich meals, healthy fats, mineral rich foods, vitamin B12, zinc, vitamin D, digestive support, and a personalized plan can change the entire direction of your health. If you have been feeling unheard, dismissed, or confused by conflicting advice, please know that your body is not broken. It is asking for a different kind of support.




.svg)
There are some of you who’ve spent years feeling dizzy, exhausted, forgetful, and even strangely unlike yourselves, yet you’ll never receive a real explanation for that. You are told that you are just stressed, maybe you need more sleep, or that the numbness in their hands and the very strange brain fog are simply a part of you getting older. Some of you are even told that it’s “just anxiety”. And yet, underneath all of this, something deeper might be taking place.
I have seen our clients go from doctor to doctor for years and years before they finally turn to us for looking beyond the surface. One of our clients was repeatedly treated for low iron, fatigue and then depression. Another had been told she was simply burnt out because she could no longer focus on her work. Both eventually discovered the very same hidden problem that was autoimmune gastritis.
Let me start off by stating that autoimmune gastritis is not a condition that gets talked about commonly. In fact, it can also quietly progress for around 7 to 14 years before it becomes quite obvious. During that period, the stomach eventually loses its ability to absorb vitamin B12 and other nutrients. By the time you are finally diagnosed, you might already be dealing with issues such as memory changes, fatigue, tingling in their feet and hands, and a very strong sense that your body has been changing without any explanation.
This is why autoimmune gastritis B12 deficiency deserves more attention. Here, at iThrive, we don’t see autoimmune gastritis as just a stomach issue. We see it as a deeper breakdown in communication between the immune system, nutrient absorption, and gut. The goal is not simply to suppress the symptoms. It is in fact to This is why autoimmune gastritis B12 deficiency deserves more attention. Here, at iThrive, we don’t see autoimmune gastritis as just a stomach issue. We see it as a deeper breakdown in communication between the immune system, nutrient absorption, and gut. The goal is not simply to suppress the symptoms. It is in fact to understand why your immune system began attacking the stomach in the very first place. in the very first place.
This is why autoimmune gastritis B12 deficiency deserves more attention. Here, at iThrive, we don’t see autoimmune gastritis as just a stomach issue. We see it as a deeper breakdown in communication between the immune system, nutrient absorption, and gut. The goal is not simply to suppress the symptoms. It is in fact to understand why your immune system began attacking the stomach in the very first place.
Autoimmune gastritis is a condition in which the immune system attacks the stomach lining by mistake. Specifically, it attacks the parietal cells. These are the cells that are responsible for making stomach acid and a very eminent protein called intrinsic factor. In absence of an intrinsic factor, the body can’t really absorb vitamin B12 appropriately.
So basically, in autoimmune gastritis, the immune system becomes very confused. Instead of protecting the body, it begins to see the parietal cells of the stomach as a threat. These are the very cells that are responsible for making stomach acid and an intrinsic factor, the protein that is needed for absorption of vitamin B12.
There are certain research works that have stated that this mostly begins because of something called molecular mimicry. Certain infections, specifically H. pylori, long standing gut imbalances, and viruses, might resemble parts of the stomach lining. The immune system reacts to the infection, but over time it can accidentally begin attacking the stomach as well.
This helps in overall explaining why autoimmune gastritis symptoms develop so slowly and steadily. For years, the body keeps losing parietal cells. The stomach gradually produces less acid and intrinsic factor, and then the nutrients stop being absorbed appropriately. But, since the changes happen slowly at a low pace, many of you actually start adapting to feeling worse without even realising that their stomach may be at the centre of it.
Most of you think stomach acid just matters for digestion. But in reality, it is one of the most crucial foundations of health.
• Breaking down the protein
• Releasing B12 from food
• Absorbing nutrients like iron, zinc, and magnesium
• Protecting against harmful bacteria
• Signalling the rest of the digestive tract to work appropriately
When stomach acid becomes quite low, food might sit heavily in the stomach. You then might feel bloated, full quickly, or even uncomfortable after meals. But because these symptoms can look so ordinary, they are always ignored.
Many of you with digestive discomfort are prescribed with acid reducing medications like proton pump inhibitors. While these drugs might temporarily reduce reflux or burning to a very great extent, they can also make autoimmune gastritis worse over time. And that is because the problem in autoimmune gastritis is usually not too much acid, it is rather too little. Therefore, reducing acid even further can make it harder to absorb B12, magnesium, calcium, and even iron. This is one of the reasons why so many of you still continue to feel unwell despite being on medications.
When you search for autoimmune gastritis B12 deficiency, you are most probably already feeling the consequences. The reason B12 levels fall so dramatically in this condition has somewhat less to do with what you are consuming and more to do with what your stomach can no longer do.
Vitamin B12 can’t be absorbed on its own. After B12 is released from food in the stomach, it must necessarily attach to an intrinsic factor. This protein is made by the similar parietal cells that are damaged in autoimmune gastritis. Without intrinsic factor, B12 just passes through the digestive system but never really reaches the cells. You might consume meat, eggs, chicken everyday and yet develop severe deficiency.
Over time, low B12 begins to start affecting your entire body, one of the very common outcomes is pernicious anemia. Pernicious anemia develops when your body no longer makes healthy red blood cells because there is not sufficient vitamin B12 available.
The red blood cells become unusually large and less effective, which means now less oxygen reaches the tissues. This is exactly when you start noticing profound weakness while climbing stairs, pale or slightly yellow skin, fatigue, dizziness, or shortness of breath. We have had clients describe it as a feeling as though their body suddenly aged by around 10 years, almost overnight.
What makes this so much frustrating is that many of you are prescribed iron tablets or just told to “rest more” without anyone asking why the deficiency keeps returning. By the time the real cause is discovered, the B12 deficiency might have been present in your body for years.
What worries me personally is that B12 deficiency doesn’t just affect the energy level, it can also affect the entire nervous system.
• Tingling or numbness in the feet and hands
• Burning feet at night
• Brain fog
• Memory lapses
• Mood swings or even depression
• Difficulty in concentrating
Sometimes these symptoms appear even before anemia does. This is why so many of you are told you have anxiety, stress, or even early neurological disease before anyone checks your B12 properly.
This is another layer that mostly gets missed. Conditions such as small intestinal bacterial overgrowth and H. pylori can make autoimmune gastritis deficiency a lot worse. Certain bacteria actually compete with you for B12. Others damage the gut lining and make it even harder to absorb nutrients.
At iThrive, we always recommend deeper testing first through Book a Root Cause Analysis when any of you stated unexplained B12 deficiency, ongoing fatigue, and digestive issues despite taking supplements.

One of the very first reasons autoimmune gastritis stays hidden is because the symptoms can seem unrelated to many. You might have stomach issues, poor memory, low energy, and numbness at the very same time without even realising they all connect back to the stomach.
In the beginning, the signs are often subtle.
• Feeling unusually full after meals
• Mild bloating
• Reduced appetite
• Occasional nausea
• Fatigue that feels out of proportion
Because trust me when I say these symptoms are not dramatic, they are often brushed aside.
As B12 levels continue to fall further, the symptoms of the same become harder to ignore.
• Tingling in hands and feet
• Sore or like smooth tongue
• Slight cracks at the corners of the mouth
• Hair thinning as well as brittle nails
• Low mood or even irritability
• Difficulty remembering certain words or conversations
This is often the point wherein you might feel frightened because you know something is wrong, but no one has explained why.
Women are especially likely to have their symptoms dismissed. Fatigue is mostly blamed on factors like motherhood, hormones, stress, or even busy schedules. Brain fog might be called burnout. Low iron might be treated without even asking why it keeps returning.
I have seen women spend years and years trying to push through symptoms because they felt guilty for not being capable of “coping up”. If this sounds anywhere familiar to you, please know that your symptoms deserve to be taken seriously.

Many of you assume the answer is simply to take more B12. But if the stomach can’t absorb B12 appropriately, swallowing more capsules is often not enough. A real autoimmune gastritis treatment plan needs to surely address not the deficiency as well as the reason because of which it developed.
As absorption is impaired, many of you feel drastically better with B12 injections or IV nutrient therapy. These methods bypass the stomach entirely and deliver the nutrients directly into the bloodstream. I’ve seen clients coming to it as describing feeling clearer, and more energetic, and rather more like themselves within a span of a couple of weeks. At iThrive, we always use accurate nutrient support as part of a larger plan rather than just a temporary quick fix.
As absorption is impaired, many of you feel drastically better with B12 injections or IV nutrient therapy. These methods bypass the stomach entirely and deliver the nutrients directly into the bloodstream. I’ve seen clients coming to it as describing feeling clearer, and more energetic, and rather more like themselves within a span of a couple of weeks. At iThrive, we always use accurate nutrient support as part of a larger plan rather than just a temporary quick fix.
The right autoimmune gastritis diet isn’t about eating less or following another restrictive plan. It is about removing what might be irritating the immune system and developing an environment wherein the stomach lining has a chance to repair.
Many of you might notice a major improvement when they start eliminating dairy, excess sugar, gluten, alcohol, and processed and packaged foods for a given period. These foods can increase inflammation, make it tough for the immune system to settle, and irritate the gut lining.
At the very same time, the body mostly responds well to foods that are nourishing, gentle, and easy to digest. Well cooked vegetables, slow cooked proteins, bone broth, vitamin D rich foods, and zinc rich foods can altogether support the entire healing. Anti-inflammatory herbs like turmeric and ginger also calms the irritation in the digestive tract.
The goal here is not perfection in any sense, it is to make the stomach feel safe enough to begin functioning properly again.
If you just like me are wondering how to improve autoimmune gastritis, the answer usually involves several layers.
The stomach lining needs support, the immune system needs to calm down, the gut microbiome needs to be repaired, and most importantly stress needs to be addressed.
• Testing for H. pylori or SIBO
• Supporting the gut with probiotics
• Improving sleep as well as reducing stress
• Correcting zinc and vitamin D deficiency
• Following a personalised anti-inflammatory nutrition plan
For people who have been struggling for years without any answers, we at iThrive offer you with Book a Consult so that we can help you uncover what has been missed.

Autoimmune gastric is one of the most overlooked causes of severe B12 deficiency. It can quietly progress for years while a person feels increasingly numb, tired, forgetful, and unlike themselves. One best thing is that these symptoms aren’t “all in your head,” and they are not always permanent. When the real cause is recognised early, many of you start feeling drastically better.
One thing is very clear: the body is not failing you, it is just trying to communicate something to you. If you have unexplained fatigue, brain fog, low B12, or digestive symptoms that no one has been able to explain, it is genuinely the time to look deeper.




.svg)
If you have lived or still live with psoriatic arthritis, you surely know how exhausting it gets to explain your symptoms to other people.
There are some mornings when your joints feel locked before you even step out of your bed. Then there are also days when the fatigue is so deep that even the simplest of the tasks feel overwhelming. You might notice your fingers swelled enough, your nails changing, and a very strange stiffness that seems worse after rest. And then obviously there is frustration of being told that your blood tests look “quite normal” while your body signals something else.
Psoriatic arthritis isn’t a joint problem. It’s not about the skin either. It is in fact an autoimmune condition where the immune system starts attacking healthy tissues by mistake, specifically the skin and the joints. This is the very reason people often ask, “Is psoriatic arthritis autoimmune?” The answer is YES. But what most people aren’t told is that this autoimmune attack is mostly made worse by the hidden nutrient deficiencies.
At iThrive Alive, we have seen our clients come to us after trying multiple medications. In many of them, we found silent nutritional gaps underneath the surface. These deficiencies don’t cause psoriatic arthritis on their own for sure, but they make the inflammation causing it louder, the pain even more stronger, and recovery slower.
This is where a true psoriatic arthritis root cause approach becomes crucial. Instead of answering what medicine suppresses symptoms, we rather pay attention to what is missing in the body that’s preventing it from calming down?
Most people think psoriatic arthritis begins in the joints. In reality, it’s different. The process mostly starts much earlier, inside the immune system and the gut.
There is a reason the keyword “psoriatic arthritis gut health” has such a high volume.
Your gut is home to trillions of microbes that help in training the immune system. When the gut lining is damaged, unwanted particles from the bacteria and the food can enter the bloodstream. This particular process is called intestinal permeability or leaky gut.
Once that happens, the immune system becomes highly reactive. In someone already genetically prone to psoriasis or psoriatic arthritis, this extra immune stimulation can surely become the spark that drives inflammation in joints and the skin.
At the same time, poor gut health can reduce how well your body absorbs important nutrients. So even if you’re eating well, your body might still be running low on zinc, selenium, vitamin D, or omega 3.
When the body is low in key nutrients the frustrating symptoms of psoriatic arthritis can even become worse.
What surprises many people is that these symptoms aren’t always about the disease on its own. Sometimes they are also the clues that the body is missing what it really needs to control inflammation.
Of all the deficiencies we see in the people with autoimmune issues, low vitamin D is the most common. That is why people are largely searching for vitamin D3 psoriatic arthritis and vitamin D supplements autoimmune have become so common.
Vitamin D is not just a random vitamin. It rather behaves like a hormone.
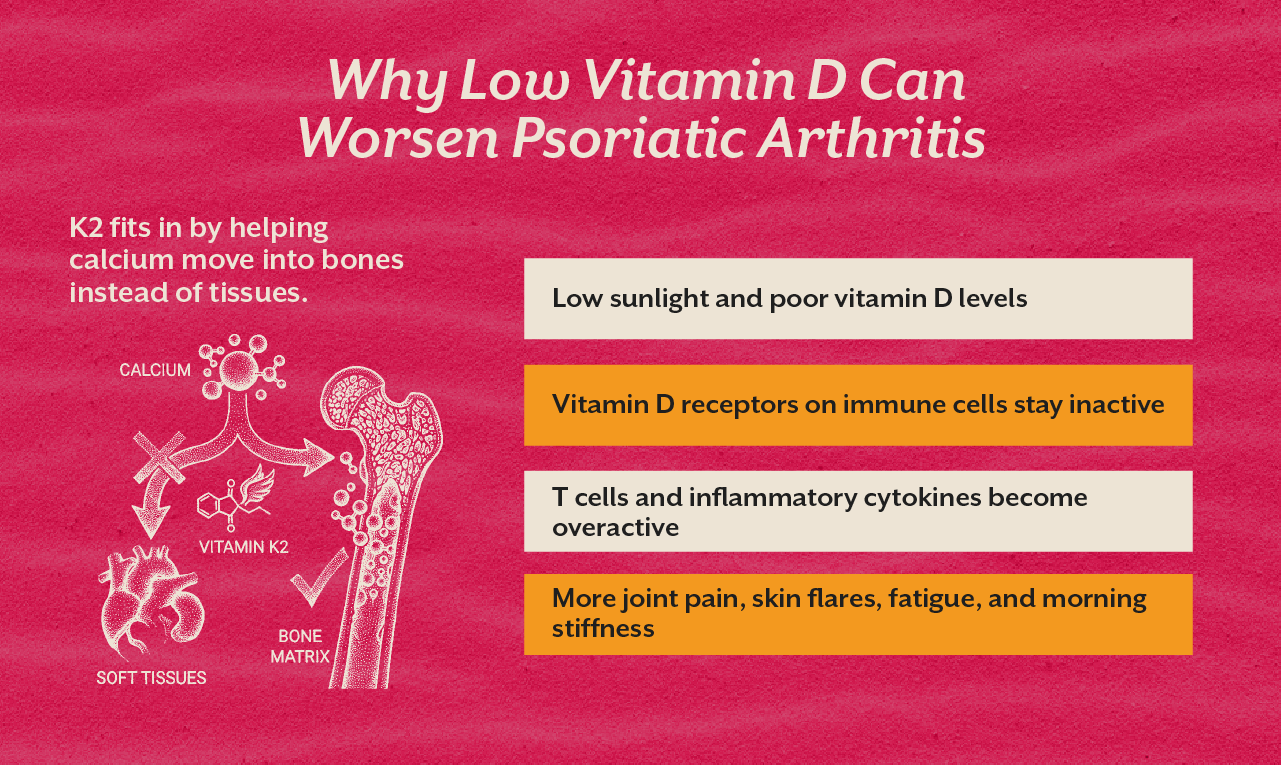
Your immune cells has special receptors called VDRs. When sufficient vitamin D is present, these receptors convey the immune system to slow down after a threat has passed. In psoriatic arthritis, that “OFF switch” mostly stops working properly.
Low vitamin D has been closely linked to higher levels of inflammatory chemicals, specifically those involved in joint pain and psoriasis. It might also efficiently contribute to more severe psoriatic arthritis morning stiffness and stronger flare ups during winter.
I have myself seen clients with psoriatic arthritis who’ve spent years and years thinking their worsening symptoms are simply “part of the condition,” only to discover at iThrive via root cause analysis that their vitamin D levels were severely low.
The truth is that many Indians are deficient even if they spend most of their time outside.
Darker skin naturally needs more sunlight to make vitamin D. Add factors like indoor jobs, immense pollution, sunscreen, construction sites, very limited midday sun exposure, and the gap becomes even bigger.
This is why simply saying “sit enough in the sunlight” is surely not something that makes sense.
One of the most common things people make is taking larger amounts of vitamin D without K2.
Vitamin D helps the body absorb calcium effectively. But vitamin K2 helps direct that calcium into the bones instead of permitting it to build up in soft tissues.
K2 works like a traffic controller. It activates proteins that tell the calcium where to go. Without adequate K2, taking high dose vitamin D might not support the body in the way you have expected it to.
I’ve heard many of you always asking, “How much vitamin D for psoriatic arthritis?”
There is no single answer to it because the right amount is entirely dependent on your blood levels. However, many practitioners working with autoimmune conditions always aim for a vitamin D level between 50 and 80 ng/ml.
Testing is important, so stop guessing and take the right step which is to book a consult with our nutritionist.
If you have frequent flares, persistent fatigue, worsening pain in winter, or low mood, it is surely worth exploring this deeply via our Root Cause Analysis which will just cost you
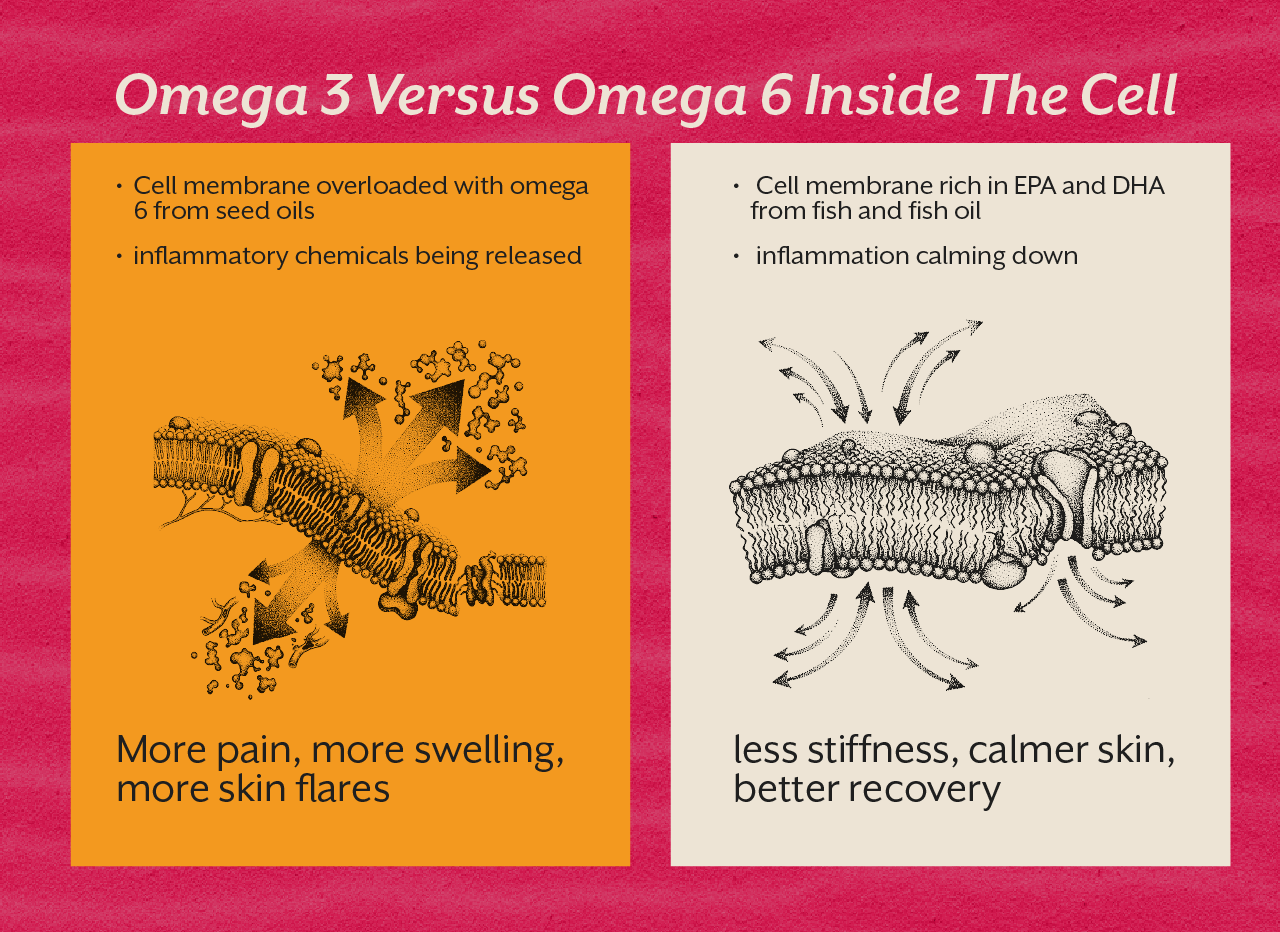
When most of you hear the word inflammation, you often imagine redness or swelling right? But in psoriatic arthritis, inflammation is constantly happening at a cellular level all the time.
That is where omega 3 becomes eminent.
The forms of omega 3 that matters the most for psoriatic arthritis are EPA and DHA. These are found majorly in fatty fish and high quality fish oil.
EPA DHA psoriasis research recommends that these facts are helpful in reducing the inflammatory pathways that drive both the symptoms of joint pain as well as skin.
One of the eminent ways they work is reducing the activity of Th17 cells. These are the immune cells that are strongly involved in psoriatic arthritis.
Most of you are consuming far more omega 6 as compared to omega 3.
Refined seed oils like sunflower oil, corn oil, and soyabean oil are now everywhere. They increase arachidonic acid inside the cell membranes. Arachidonic acid is one of the raw materials that the body utilises to develop inflammatory chemicals.
When there is too much of arachidonic acid and not sufficient EPA, the body stays stuck in an inflammatory state.
This is why omega 3 and inflammation are so close to each other.
Many people try increasing omega 3 through flax seeds and chia seeds. These foods contain ALA, which the body has to actively convert into DHA and EPA.
The problem is that the conversation rate is poor. And for someone with active autoimmune inflammation, depending entirely on plant omega 3 is rarely enough. In such cases fatty fish like salmon and sardine, fish oil, or krill oil are mostly far more effective.
You might want to look more closely at omega 3 if you certainly have:
At iThrive Alive, improving omega 3 intake is mostly one of the very first changes in a psoriatic arthritis nutrition plan as people frequently notice quite reduced stiffness and better energy within a couple of weeks.
Omega 3 and Vitamin D get most of the attention. But there are two other nutrients that are mostly overlooked in people with psoriatic arthritis: zinc and selenium.
If you have psoriatic arthritis nail changes, your body might need more of zinc.
Zinc is far more important for healthy skin, stronger nails, and proper immune function. It also helps repair tissues and maintain the skin barrier.
The most frustrating part is that standard blood tests don’t always catch mild zinc deficiency.
Selenium is needed to develop glutathione peroxidase, one of the body’s most important antioxidant enzymes.
This enzyme protects mitochondria, those tiny energy factories that are present inside your cells.
If mitochondria are constantly under inflammatory stress, it becomes tough for the body to make energy. This is one of the reasons why psoriatic arthritis fatigue can feel so crushing.
Sometimes people think their fatigue isn’t just emotional burnout or like poor sleep. But underneath it, their cells might simply not just have the nutrients that are needed to produce energy in an efficient manner.
There are a few reasons you now see more selenium and zinc deficiencies than ever before.
Modern soil contains very few minerals. Highly processed diets contain very few nutrient dense foods. And certain healthy foods, such as excessive spinach or say almonds, can at times make things even worse because they contain compounds that reduce absorption of minerals.
The best food sources involve seafood, red meat, brazil nuts, eggs, and organ meats.

A very good psoriatic arthritis nutrition plan is not at all about following another restrictive trend diet. It is clearly about developing an environment inside the body wherein the inflammation has less room to thrive.
The most helpful foods are often the least processed and the most nutrient dense.
Many people with psoriatic arthritis witness that they feel worse after consuming certain foods.
This doesn’t mean that every person needs to prevent and avoid these forever. But it surely means they may be worth testing, specifically if your symptoms are not improving.
For people who feel extremely stuck trying many things, this is often where a more structured approach such as the iThrive Alive Program or a Book a Consult can prove to be beneficial for you to identify what your body is reacting to.
No two people with psoriatic arthritis are exactly the same.
One person might struggle majorly with psoriatic arthritis morning stiffness. Another might have fatigue, nail changes, and gut symptoms. This is exactly why we at iThrive believe that a real psoriatic arthritis root cause plan should always be extremely personalized.
Here at iThrive, we don’t look just at the symptoms, no it has never been like that. We look at vitamin D levels, inflammation markers, stress, gut health, sleep, and in fact how your symptoms change throughout the year.
If you have psoriatic arthritis and feel like your body is constantly fighting against you, please know that you are not imagining it. The pain, fatigue, stiffness, and frustration are real. But so is the possibility that your body may be missing some of the very nutrients it needs to calm the inflammation.
One thing we have to mention is that vitamin D, selenium, omega 3 and zinc are not at all the magic cures. But when they are low, they can quietly make psoriatic arthritis worse. Addressing these deficiencies doesn’t replace medical care. It strengthens the core foundation beneath it.
Sometimes the most crucial question is not just what medicine should you take, but what your body needs that it’s not getting is far more important.




.svg)
If your fingers keep aching in the morning, your nails have suddenly started changing, or you often keep brushing off swelling just as “stress” or a sign of “getting older,”it might be worth paying closer attention to.
Psoriatic arthritis isn’t just a joint problem. It is an autoimmune condition in which the immune system attacks the nails, joints, skin and even the eyes, by mistake. For a lot of people, the first signs are quite subtle. They often start months or even years before a diagnosis is made.
One of the major reasons psoriatic arthritis is missed early is because the symptoms don’t always arrive together. You might witness flaky patches on the scalp years before you develop knee pain. You might have nail pitting long before your fingers swell. Few people witness severe fatigue along with morning stiffness without even realising that an inflammatory process is already underway.
The earlier you recognise the first signs of psoriatic arthritis, the greater is the chance of slowing down the progression before permanent damage occurs. At iThrive Alive we often view women who were told that they had vitamin deficiency, stress, rheumatoid arthritis, or even aging, only to discover that the real issue was always the developing psoriatic arthritis in the background.
Psoriatic arthritis early symptoms can look quite different depending on person to person. Some people first develop psoriasis on the skin. Others might notice a rash and instead begin with painful heel pain, fingers, or even extreme stiffness after waking up.

Unlike the conditions that appear promptly, psoriatic arthritis mostly builds gradually. You might have one or two symptoms for a long time before more obvious signs appear.
For instance:
Because of this, many people spend a lot of years treating each symptom solely without connecting the dots.
When psoriatic arthritis is left untreated for a while, ongoing inflammation can initiate damage to the joint permanently. Over time, this can also result in deformity, minimised mobility, and difficulty performing daily tasks.
The goal is not simply just to manage the pain. It is also to identify the disease early, understand what’s driving the immune response and then intervene before deeper damage takes place.
The most common and earliest symptom is persistent joint pain. Unlike soreness due to intense workout or a temporary strain, this specific discomfort tends to keep returning. It might affect the knees, toes, fingers, lower back, wrists, or ankles.
How psoriatic joint pain feels different
The pain is often destined as achy, deep, and inflammatory. It might improve slightly with movement and worsen after long periods of resting.
• Fingers and toes
• Knees
• Ankles
• Lower back and hips
• Wrists
If you already have psoriasis and develop unexplained joint pain, don’t ignore it. This is often the very first sign of psoriatic arthritis.
Psoriatic arthritis morning stiffness is one the most evident clues that inflammation is involved. Many people wake up feeling as though their joints are unusually heavy or “stuck”.
Unlike ordinary stiffness, which improves within a couple of minutes, inflammatory stiffness mostly lasts for 30 minutes or longer.
Why does morning stiffness happen?
During sleep, inflammatory chemicals build up around the joints. When you wake up in the morning, it takes time & movement for the fluid and inflammation to settle.
When to pay attention
If your stiffness improvises once you move around but returns soon after long periods or inactivity, it is worth discussing with a functional nutritionist.
One of the most distinctive symptoms is psoriatic arthritis dactylitis. This refers to swelling of an entire toe or finger rather than just one joint.
The digit becomes entirely swollen right from top to bottom and might feel tender, and difficult to bend.
In many other forms of arthritis, only the joints are affected. In psoriatic arthritis, the inflammation can also involve the tendons, soft tissue, and ligaments around the entire digit.
Signs of psoriatic arthritis dactylitis
This symptom is specifically crucial because it is much more strongly linked with psoriatic arthritis than with other types of arthritis.
Not everyone experiences dramatic swelling. Sometimes the inflammation is subtle and appears as puffiness around the knees, wrists, knuckles, or ankles. You might notice that rings no longer fit you properly or that your shoes feel tighter by the end of the day.
The hidden inflammation triggers behind swelling.
Joint swelling occurs because the immune system is attacking the joint lining. Over time, this inflammation can erode cartilage and also affect the bones.
Your nails can mostly reveal psoriatic arthritis way before your joints do.
Nail pitting refers to those tiny dents or depressions on the nail surface. Some people also notice crumbling, ridges, or nails that entirely lift away from the nail bed.
The nail and the joint beneath are closely linked. Inflammation around the nail matrix can be a very early sign that the immune system is already affecting the joints.
Early nail changes to watch first:
If you have unexplained changes in the nail along with joint symptoms, it might point towards psoriatic arthritis rather than a fungal infection.
Beyond pitting, many people also notice that their nails start becoming darker, thicker, or slightly separated from the skin beneath.
This mostly happens slowly, which is why it is very commonly dismissed.

One of the significant differences in psoriatic arthritis vs rheumatoid arthritis is that rheumatoid arthritis mostly doesn’t cause major nail changes.
If you have both joint pain and unusual nails, psoriatic arthritis becomes much more likely.
Most people with psoriatic arthritis either have psoriasis already or they do develop it at some point of time.
Psoriasis usually appears as raised, red, scaly patches called plaques. These may show up on the elbows, knees, scalp, lower back, or behind the ears.
Psoriasis mostly appears as red, raised, scaly patches called plaques.
When skin symptoms come before joint symptoms.
For quite a few people, skin lesions appear years before the arthritis even begins. In others, the joint symptoms come first.
The plaques might burn, crack, flake, or even itch.
Scalp psoriasis is one of the most overlooked early signs. It can also look like stubborn dandruff, but unlike most of the ordinary dryness, the scalp becomes quite inflamed, red, and itchy.
Why is the scalp important?
Improvement of scalp is very strongly associated with a higher risk of developing psoriatic arthritis. If you have persistent scalp flaking along with joint pain, stiffness, or like fatigue, it is definitely worth investigating further.
One of the earliest but most least discussed symptoms is fatigue
Long before the joints become swollen, many people describe feeling unusually exhausted, drained, or foggy. This is not just tiredness, rather it is a deeper sense that the body is struggling.
Why psoriatic arthritis can affect energy levels?
Inflammation doesn’t stay confined to the joints. The immune system utilises enormous amounts of energy, and ongoing inflammation can also affect factors such as mood, sleep, blood sugar stability, and even mitochondrial function.
At iThrive Alive, we always look far beyond the joint itself and always ask why the immune system became overactive in the very first place.
Treating symptoms is crucial, but it is not enough if the deeper triggers are not addressed.
Studies have shown that many autoimmune conditions begin in the gut. Intestinal permeability, low microbial diversity, gut infections, and chronic digestive inflammation can all maximize the activation of the immune system.
This is why a highly comprehensive approach mostly includes:
You may also find our blog “Psoriatic Arthritis: The Skin-Joint Connection Your Doctor Probably Never Explained” helpful here.
Refined sugar, gluten, processed oils, and dairy products are known to be the most common triggers for inflammation in susceptible individuals.
Low magnesium, vitamin D, omega 3, and zinc can all together make it tough for the immune system to regulate itself.
Chronic stress raises inflammatory signalling and can also worsen autoimmune flares. Sleep deprivation also affects the way the immune system behaves.

At iThrive Alive, we don’t believe that each person with psoriatic arthritis has the very same root cause. Two people might have similar symptoms but entirely different drivers.
This is why our approach initiates with an in-depth evaluation of food triggers, metabolic health, gut health, stress, nutrient status, inflammation, and sleep.
A whole food anti-inflammatory diet emphasised on healthy fats, high quality protein, along with gut healing foods.
Omega 3, curcumin, vitamin D, zinc, gut support, and magnesium might be utilised strategically based on the individual.
Morning sunlight, stress regulation, minimising toxin exposure, better sleep, and gentle movement can all together help calm an overactive immune response.
If you are witnessing few of these symptoms and still don’t have answers, it is time for you to Book a Root Cause Analysis rather than waiting for the condition to progress further.
For more personalized support, you shall consider with our team to understand whether our 3 months Alive Program might be the very right fit for you.
The very first signs of psoriatic arthritis are rarely dramatic. More often, they appear as very small clues that seem quite unrelated at first: a stiff hand in early morning, unusual changes in nail, fatigue, a swollen toe, or even itchy scalp patches that no one can really explain. But these symptoms matter a lot. They are often the earliest warning of the body that inflammation is building beneath the surface.
The best part is that early intervention can truly make a real difference. When you recognise psoriatic arthritis early, understand what’s really driving it, and support the body via smart nutrition, targeted supplementation, and lifestyle interventions, it is possible to minimise symptoms and slow progression before lasting joint damage occurs.




.svg)
You have had psoriasis for years. The plaques come and go and you have learned to live with the skin flares. But lately something else has started. Your fingers swell in the morning. Your lower back aches in a way that feels entirely different from muscle soreness. Your nails have begun to pit and crumble at the edges. You mention this to your dermatologist and they refer you to a rheumatologist. The rheumatologist sends you back. And somewhere in that handoff, nobody explains what is actually happening inside your body.
What is happening is psoriatic arthritis. And in India, where psoriasis affects an estimated 0.44 to 2.8% of the population, studies show that 8.7 in every 100 people with psoriasis will go on to develop this joint condition, most of them between the ages of 30 and 50. That is not a small number. That is a significant portion of the psoriasis population developing a condition that can cause permanent joint damage if left unaddressed for too long.
This blog is for anyone living with psoriasis who has started noticing unexplained changes in their joints, nails, spine, or face. It is also for anyone with joint inflammation whose skin has been treated as a separate problem. These are not two separate problems. They are one autoimmune story told across two organs.
Before understanding the condition itself, it helps to understand how common and how underdiagnosed it actually is in the Indian context.

That nail involvement figure stands out. In 87% of Indian PsA patients, the nails show visible changes. This is a symptom that dermatologists see every day and that is almost universally attributed to fungal infection or nutritional deficiency. The missed diagnosis happens right there, in plain sight, under the nail plate.

Psoriatic arthritis meaning, at its most fundamental, is an inflammatory arthritis occurring in association with psoriasis. It is seronegative, meaning unlike rheumatoid arthritis, it does not produce a positive rheumatoid factor on blood testing. This single fact is why it gets missed so often. A doctor runs a standard arthritis panel, RF comes back negative, and the joint symptoms are attributed to something else entirely.
The condition is autoimmune at its core. The same immune dysregulation driving inflammatory skin plaques also drives inflammation at the joints, tendons, and entheses, the points where tendons and ligaments attach to bone. The immune system, in a state of chronic activation, attacks the body's own tissue across multiple sites simultaneously. The skin is the most visible site. The joints, spine, and nails suffer in parallel.

Psoriatic arthritis symptoms present in several distinct patterns. Some people develop a symmetrical polyarthritis that closely resembles rheumatoid arthritis, affecting multiple joints on both sides of the body. Others develop asymmetric oligoarthritis, where one or two joints flare in an unpredictable pattern. Indian research shows that symmetrical polyarthritis is the most common pattern, accounting for 58% of cases, while asymmetric oligoarthritis appears in 21%.
One of the most characteristic joint signs is dactylitis, diffuse swelling of an entire finger or toe. The digit swells uniformly from base to tip, giving the classic sausage appearance. This is not seen in most other forms of arthritis and should immediately raise suspicion for psoriatic arthritis when present alongside skin or nail changes.
Nail involvement is one of the most diagnostically important features of this condition and one of the most frequently misread. Psoriatic arthritis nails show pitting (small depressions across the nail surface), onycholysis (separation of the nail from the nail bed), subungual hyperkeratosis (thickening under the nail), and oil drop discolouration (a yellowish patch visible through the nail). These changes affect 87% of Indian PsA patients. They are almost never caused by fungal infection alone. If your nails look this way and you have psoriasis, you need a rheumatology assessment, not another antifungal prescription.
Psoriatic arthritis face involvement is less widely discussed but clinically real. Uveitis, inflammation of the eye's middle layer, causes redness, pain, and light sensitivity in a subset of patients. Temporomandibular joint involvement causes jaw pain and difficulty chewing. Psoriatic plaques on the scalp, around the ears, and along the hairline are frequently dismissed as seborrheic dermatitis rather than recognised as part of the wider psoriatic disease picture.
Psoriatic arthritis spondylitis refers to inflammatory involvement of the spine and sacroiliac joints. In Indian studies, 49% of PsA patients show spondyloarthropathy patterns. The hallmark is morning stiffness lasting more than 30 minutes that improves with movement rather than rest. This is the opposite of mechanical back pain. Inflammatory back pain beginning before age 45 that responds to anti-inflammatory treatment warrants sacroiliac joint imaging and a rheumatology assessment.

Imaging is where psoriatic arthritis reveals its most distinctive features and where a skilled radiologist can clearly differentiate it from rheumatoid and osteoarthritic changes.
A psoriatic arthritis hand x-ray shows findings that appear almost paradoxical: bone erosion alongside new bone formation occurring simultaneously. The classic pencil-in-cup deformity, where the end of one bone erodes into a point and the adjacent bone cups around it, is pathognomonic for severe PsA. Periostitis which is the inflammation of the bone lining causing a fluffy appearance along the bone edge, and enthesophytes (bone spurs at tendon attachment points) are also frequently visible.
Psoriatic arthritis radiology of the sacroiliac joints shows asymmetric sacroiliitis, distinguishing it from ankylosing spondylitis which affects both sides equally. MRI is increasingly used to detect early bone marrow oedema at entheses before structural damage is visible on plain X-ray. Ultrasound of tendons and entheses can show thickening and power Doppler activity confirming active inflammation. These imaging tools are available in most Indian tertiary centres and should be requested when clinical suspicion is high.
Psoriatic arthritis is not simply the result of having psoriasis for a long time. It reflects a deeper immune imbalance involving the IL-17 and IL-23 inflammatory pathways, gut microbiome dysbiosis, genetic predisposition (HLA-B27 and related alleles), and environmental triggers including trauma, infection, and metabolic dysfunction.
The gut connection is particularly significant. Research consistently shows that intestinal permeability and microbiome imbalance precede and perpetuate psoriatic disease activity. Immune cells educated in a dysbiotic gut carry inflammatory memory into the skin and joints. This is why dietary patterns, stress regulation, and gut health are not peripheral to PsA management. They sit at its biological centre.
If you are experiencing a cluster of autoimmune symptoms across multiple body systems alongside joint and skin changes, a root cause analysis can map the full inflammatory picture rather than managing each organ in isolation.
Psoriatic arthritis is a whole-body autoimmune condition wearing two faces, one on the skin and one in the joints. The fact that 83% of Indian PsA patients are newly diagnosed at the time of rheumatology referral tells us the years between psoriasis onset and arthritis diagnosis are filled with missed signals the body was already sending.
The nails were pitting. The fingers were swelling. The back was stiff every morning. And nobody connected the dots because skin and joints are treated as separate departments in a system that was not designed to see the whole person.
Understanding psoriatic arthritis symptoms, recognising psoriatic arthritis nails, knowing what psoriatic arthritis spondylitis looks like, and understanding what imaging can and cannot reveal all contribute to shortening the diagnostic gap. The earlier this condition is identified, the greater the chance of preventing the joint damage that makes it irreversible.
If the symptoms described in this blog feel familiar and you are not sure where to start, book a consult and begin with the right questions rather than another prescription for a condition that has not yet been properly named.




.svg)
Picture a 28 year old woman in India. Her periods have been irregular for over a year. She has been told she probably has PCOS. Her thyroid panel came back normal. She has been put on birth control to regulate her cycle, but the moment she stops, the irregularity returns. Nobody has checked her prolactin yet.
This is not a rare story. Research shows that between 25 and 37% of women presenting with unexplained infertility have elevated prolactin levels, yet a prolactin test is still not universally included in early hormonal workups.
Hyperprolactinemia, chronically elevated prolactin, is one of the most underdiagnosed hormonal disruptions in women of reproductive age. It derails periods, blocks ovulation, feeds mood instability, and creates a confusing symptom picture that points in every direction except the right one.
Before diving into symptoms, it is worth pausing on how widespread this condition actually is in India.

That last row is particularly striking. In a 2025 Indian study of 110 women with PCOS, over half had hyperprolactinemia. These are not numbers from a rare endocrine condition. They are the everyday hormonal reality of Indian women.
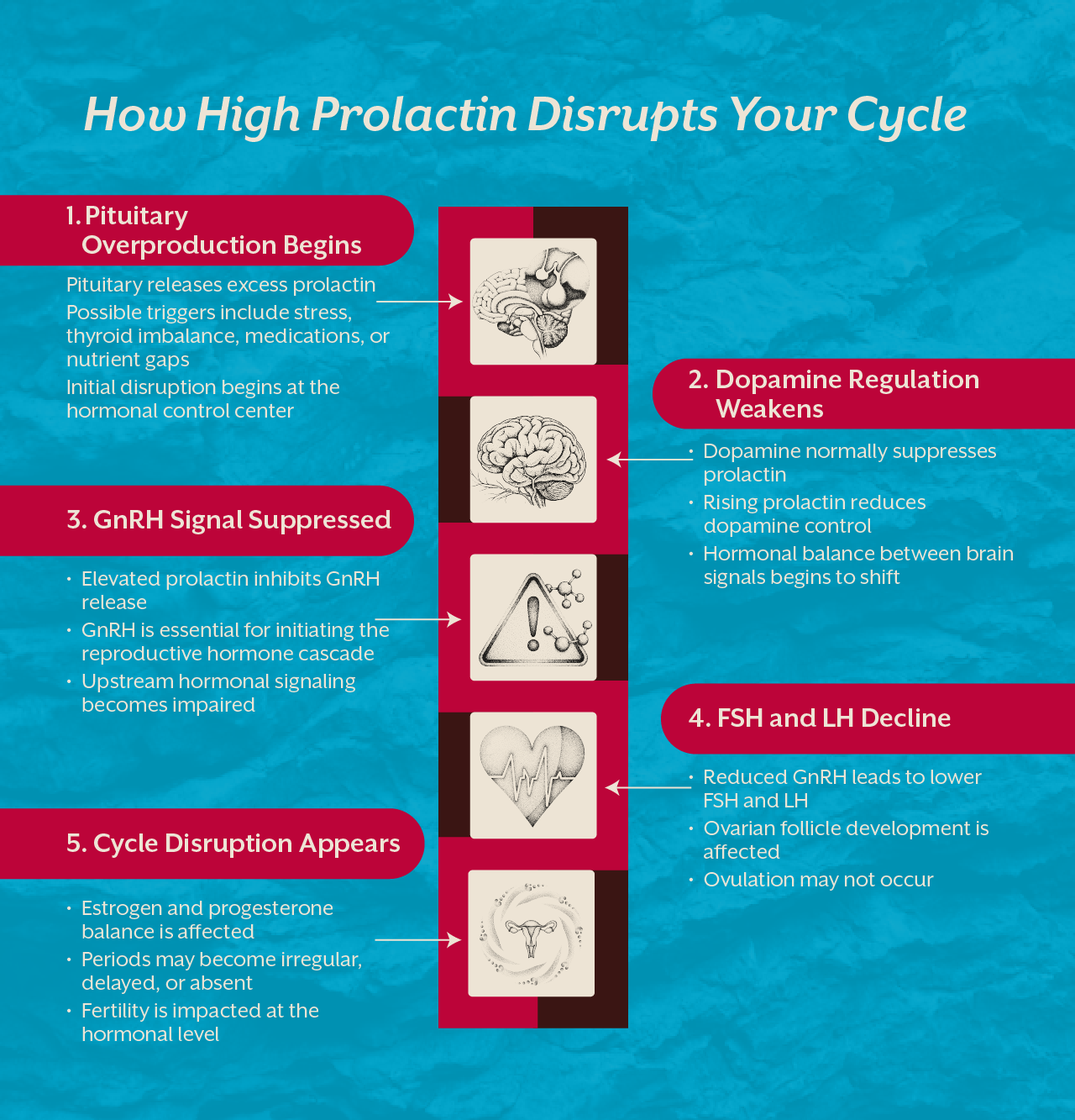
Prolactin is a hormone made by the pituitary gland. Its primary role is to trigger breast milk production after childbirth. Outside of pregnancy and nursing, prolactin should stay low. When it rises without a biological reason, the consequences are significant because prolactin directly suppresses FSH and LH, the two hormones that govern the menstrual cycle.
When prolactin climbs, FSH and LH fall. When FSH and LH fall, ovulation stops. And when ovulation stops, the period disappears or grows erratic. This is the central mechanism driving hyperprolactinemia symptoms in females, and why the period is always the first thing to go.
Women carry a far greater burden of this condition than men. The female hormonal system is simply more sensitive to prolactin fluctuations because the reproductive cycle depends on getting it right.
The cause is not always the same and treatment depends entirely on finding the right driver.
The most common structural cause is a prolactinoma, a benign pituitary tumour that overproduces prolactin. These account for nearly half of all pathological cases and are more common in women than men. Women typically develop smaller microprolactinomas that are harder to detect on routine imaging, which is one reason diagnosis is so often delayed.
When the thyroid is underactive, excess TRH directly stimulates prolactin secretion. A woman with poorly managed hypothyroidism may have elevated prolactin purely as a downstream consequence. Treating the thyroid often normalises prolactin entirely, without any direct prolactin intervention at all.
Antipsychotics, certain antidepressants, blood pressure medications, and antiemetics raise prolactin by blocking dopamine, the brain chemical that normally keeps prolactin suppressed. This dopamine connection is central to understanding the condition and why nutritional support can genuinely make a difference.
Prolactin rises with physical stress, poor sleep, and sustained high cortisol. Women who are consistently overworked and under-rested often carry mild to moderate prolactin elevation that nobody connects to their symptoms. The overlap with burnout is real. Read our blog on Addison's Disease Symptoms in Women Mistaken for Burnout for a fuller picture of how stress-related hormonal conditions disguise themselves.

The relationship between prolactin and irregular periods is direct. Elevated prolactin suppresses GnRH, which reduces FSH and LH from the pituitary. Without these signals, the ovaries do not ovulate. Periods arrive late, become very light, or stop entirely. The cycle irregularity is the symptom. Elevated prolactin is the cause.
One of the more startling high prolactin symptoms in women is galactorrhea, the spontaneous production of breast milk in a woman who is not pregnant or breastfeeding. This occurs in roughly one third to half of women with hyperprolactinemia. Many women notice it and stay silent, assuming it is normal. It is not. It is a direct sign that prolactin is biologically elevated and active.
Elevated prolactin blocks ovulation and therefore blocks conception. Women who have been trying to conceive for over a year with irregular cycles should have prolactin tested as a first-line investigation. In Indian infertility studies, elevated prolactin was found in nearly 37% of women with endocrine-related infertility. Prolactin fertility interference is one of the most treatable causes of anovulatory infertility once properly identified.
Elevated prolactin suppresses estrogen, and low estrogen drives depression, poor libido, brain fog, and emotional flatness. Women describe a version of themselves they do not recognise: disinterested, flat, and disconnected. These are biological symptoms, not character changes. Some are placed on antidepressants that raise prolactin further, quietly worsening the very hormonal environment they are trying to correct.
Prolactin secretion is controlled primarily by dopamine, which is released continuously from the hypothalamus. Dopamine truly suppresses prolactin. When dopamine falls, prolactin rises promptly. This is not just pharmacology, rather it is nutritional biochemistry.
Dopamine synthesis requires tyrosine, vitamin B6, iron, and zinc. When a woman is chronically stressed, nutritionally depleted, or sleeping poorly, dopamine production suffers and prolactin climbs. Lifestyle and nutrition are not optional extras here. They sit directly at the root of the mechanism.
Think of dopamine as the valve and the prolactin as the water. When the valve is strong enough, the water stays controlled. When it weakens, everything overflows.
Medical treatment through dopamine agonists is the clinical standard for prolactinomas. But for women with idiopathic or mildly elevated prolactin, targeted nutritional support can produce meaningful change. Hyperprolactinemia natural treatment is not a replacement for medical investigation. It is the biological foundation that makes any treatment more effective.
Vitamin B6 is a critical cofactor in dopamine synthesis. Studies have shown that B6 supplementation can minimise elevated prolactin in women with idiopathic hyperprolactinemia. Without adequate B6, the enzymatic step that converts tyrosine into dopamine cannot complete efficiently, and prolactin suppression weakens over time.
Zinc plays a direct role in regulating pituitary function as well as prolactin release. Zinc deficiency impairs dopamine receptor sensitivity and has been linked to elevated prolactin. Women experiencing hair thinning or acne alongside cycle irregularity should have zinc status assessed as part of their hormonal investigation.
A hyperprolactinemia diet is a rebuilding plan, not a restriction list. Prioritise tyrosine-rich foods: eggs, chicken, nuts, and seeds. Add magnesium-rich foods like pumpkin seeds for dopamine receptor support. Include vitamin C rich fruits and vegetables to reduce oxidative stress at the pituitary level. Stable blood sugar is non-negotiable since cortisol spikes directly drive prolactin upward. Avoid alcohol, excessive caffeine, and ultra-processed foods that disrupt hypothalamic signalling.
Diagnosis begins with a fasting morning serum prolactin test, drawn at least 2 hours after waking and before any physical exertion. A single elevated reading is not sufficient for diagnosis. A second confirmatory test is needed before any treatment decision is made.
If prolactin remains elevated, a pituitary MRI is ordered to check for adenoma. Thyroid function and medication history are reviewed simultaneously. Finding the root cause, rather than simply suppressing the number, determines whether treatment will hold.
If you are experiencing irregular periods, unexplained infertility, or mood disruption alongside cycle changes, a root cause analysis can map the full hormonal picture rather than treating each symptom in isolation.
Hyperprolactinemia is not rare. It is one of the most common hormonal conditions in Indian women of reproductive age, hiding behind missed periods, unexplained infertility, and mood changes written off as stress for years.
A single prolactin blood test can begin to change an entire diagnostic story. Whether the driver is a pituitary adenoma, an underactive thyroid, B6 and zinc deficiency, or chronic dopamine depletion, this condition has clear mechanisms and clear pathways of support. It goes undertreated not because it is complex, but because it goes untested.
If your hormonal picture feels incomplete and the standard answers are not adding up, do not wait. Book a consult and let the right investigation finally begin.




.svg)
You wake up exhausted even after eight hours of sleep. You crave salt so badly you find yourself adding it to everything, even fruit. The skin on your knuckles and elbows has been darkening for months with no explanation. Your blood pressure keeps dropping, and you feel dizzy every time you stand up too fast. You have seen three doctors, and each one hands you the same verdict: burnout, stress, or anxiety.
But what if your body is not reacting to a busy schedule? What if something far deeper is happening?
Addison's disease in women is one of the most underdiagnosed endocrine conditions in the world, not because it is rare, but because its early symptoms mirror the exact language of modern exhaustion so completely that both women and their doctors consistently miss it. This blog is about changing that. It is about understanding what Addison's disease actually does inside the female body, why low cortisol gets confused with adrenal fatigue, what the real warning signs look like, and what a smarter approach to healing involves.
Addison's disease, also called primary adrenal insufficiency, occurs when the adrenal glands stop producing enough cortisol and often aldosterone as well. Cortisol is not just a stress hormone. It regulates blood pressure, controls blood sugar, manages inflammation, and keeps the immune system in balance. When its production collapses, the entire hormonal ecosystem begins to destabilize.
The most important thing to understand about Addison's disease causes is that in roughly 70 to 90% of cases, the trigger is autoimmune. The immune system mistakenly attacks the adrenal cortex, the outer layer responsible for producing these critical hormones. This is why it is called autoimmune Addison disease, and this is why women are disproportionately affected. Estrogen tends to upregulate immune activity, which means the very biology that makes a woman's reproductive system resilient also makes her more susceptible to immune misfires.
The early symptoms of Addison's disease in women do not arrive loudly. They arrive quietly, over months or years, disguised as life stress.
This is not regular tiredness. Women with adrenal insufficiency describe a fatigue that sits in the bones. It is persistent, disproportionate to activity levels, and does not improve after rest, weekends off, or even vacations. The body is not producing enough cortisol to sustain energy metabolism, so cells cannot generate the fuel they need to function. Many women spend years attributing this to poor sleep habits before anyone thinks to test adrenal function.
When aldosterone production drops, the kidneys lose their ability to retain sodium effectively. The body compensates with intense cravings for salt. If you find yourself adding extra salt to every meal, craving salty snacks even when you are not hungry, or feeling noticeably worse on a low sodium diet, this is not a quirk. It is a physiological distress signal.
As cortisol production falls, the pituitary gland releases more ACTH in an attempt to stimulate the adrenals. ACTH shares a molecular structure with melanocyte stimulating hormone, which controls skin pigmentation. The result is a darkening of the skin at pressure points: knuckles, elbows, knees, inner lips, and gum lines. Women often attribute this to sun exposure or natural skin variation. In the context of other symptoms, it is a significant clinical flag.
Aldosterone helps maintain blood volume and vascular tone. Without adequate levels, blood pressure drops and the body struggles to respond to postural changes. Standing up quickly becomes an event. Dizziness, lightheadedness, and fainting episodes become regular occurrences, typically investigated through cardiology before anyone considers endocrinology.
The gastrointestinal system is exquisitely sensitive to cortisol levels. Low cortisol produces nausea, vomiting, abdominal pain, and diarrhea, symptoms that look indistinguishable from IBS or anxiety driven gut dysfunction. Combined with reduced appetite and altered metabolism, unexplained weight loss over months is another signal that rarely prompts adrenal investigation.
Cortisol plays a direct role in mood regulation through its interaction with serotonin, dopamine, and the HPA axis. When cortisol is consistently low, emotional regulation becomes difficult. Irritability, low mood, and a sense of profound emotional flatness are reported by many women with adrenal insufficiency long before any diagnosis is made.

The term adrenal fatigue has become widely popular in wellness circles. It describes a state in which chronic stress is said to deplete adrenal output, producing suboptimal cortisol levels that cause fatigue and burnout. While stress absolutely disrupts HPA axis function, adrenal fatigue as a distinct diagnosable medical condition is not currently recognized by mainstream endocrinology.
Adrenal fatigue vs Addison's is a comparison that matters because the two sit at very different points on the severity spectrum. With adrenal fatigue, cortisol is described as suboptimally low but not absent. With Addison's disease, the adrenal cortex has been structurally damaged, and cortisol production is genuinely and measurably deficient.
The consequences of confusing the two are serious. Someone managing what they believe to be adrenal fatigue with lifestyle changes and adaptogens, when they actually have Addison's disease, is at real risk of an adrenal crisis. This is a medical emergency in which cortisol levels drop so severely that blood pressure collapses, vomiting occurs, and the body enters shock. It can be life threatening within hours without emergency hydrocortisone.
Low cortisol vs adrenal fatigue symptoms can appear similar on the surface: fatigue, salt craving, mood changes, and digestive discomfort appear in both. The difference lies in the degree, the progression, and the presence of hallmark signs like hyperpigmentation and postural hypotension that point toward true primary adrenal insufficiency rather than functional HPA dysregulation.

Studies suggest the average time from symptom onset to diagnosis ranges from one to ten years. In women, the delay is often longer.
Several factors drive this. The symptoms overlap almost perfectly with conditions women are routinely diagnosed with, including depression, anxiety, chronic fatigue syndrome, IBS, and burnout. When a woman presents with tiredness, low mood, stomach issues, and dizziness, medicine has historically looked toward psychological explanations first.
Additionally, standard blood tests ordered in primary care do not include an early morning cortisol or an ACTH stimulation test, which are the investigations needed to identify adrenal insufficiency. A normal complete blood count or metabolic panel will not catch Addison's disease.
Women are also more likely to rationalize symptoms as a function of busy lives. The cultural narrative that exhaustion is normal for women managing careers, households, and family responsibilities creates an internal dismissal that delays help seeking for years.
While Addison's disease requires medical management with hormone replacement therapy, nutritional support plays a meaningful role in managing symptoms and reducing flare risk.
An Addison's disease diet centers on a few core principles. Sodium intake must remain consistently adequate since aldosterone deficiency means the body is chronically at risk of sodium depletion, particularly during exercise, illness, or stress. A low sodium diet is actively counterproductive in this condition.
Blood sugar stability is equally essential. Without adequate cortisol, the liver cannot maintain stable glucose between meals. Small, frequent meals rich in complex carbohydrates, protein, and healthy fats help prevent the blood sugar dips that trigger symptom flares. Refined sugar and processed carbohydrates amplify the glucose instability that the adrenal compromised body cannot recover from easily.
Because autoimmune Addison disease involves immune dysfunction, an anti-inflammatory dietary approach is broadly supportive. Omega 3 rich foods, colorful antioxidant dense vegetables, and the reduction of processed food all help lower the inflammatory burden on the immune system. Vitamin D, magnesium, vitamin B5, and vitamin C are nutrients specifically involved in adrenal hormone production and immune regulation, and at iThrive we commonly see these depleted in women with both autoimmune and adrenal conditions.
.webp)
At iThrive Alive, the approach to adrenal conditions begins by asking what made the immune system attack the adrenal glands in the first place. Autoimmune triggers rarely arise in isolation. Gut permeability, chronic infections, heavy metal burden, nutrient deficiencies, and unresolved inflammatory patterns are common upstream contributors to autoimmune activation.
For women already diagnosed and on cortisol replacement therapy, a functional nutrition approach does not aim to replace the medication. It aims to reduce the total inflammatory and immune burden so the body is not fighting on multiple fronts simultaneously. Better gut health, lower inflammatory signaling, stable blood sugar, and optimized nutrient status all contribute to fewer flares and a more stable daily life.
If you are noticing a persistent pattern of unexplained fatigue, intense salt cravings, postural dizziness, or skin changes that has never been adequately explained, it is worth asking whether adrenal function has truly been assessed. You can book a root cause consultation with our nutritionist to get a clearer picture of what is actually driving your symptoms.
Addison's disease in women is a real, measurable, and manageable condition that gets buried beneath years of misdiagnosis not because it is invisible but because medicine has not been trained to look for it where women carry it. Fatigue is not laziness. The salt cravings are not a personality trait. The dizziness is not anxiety. The skin changes are not cosmetic. They are a coherent biological story told by a body whose adrenal glands are struggling to keep up. Understanding the difference between low cortisol vs adrenal fatigue symptoms, recognizing the adrenal insufficiency symptoms women actually experience, and knowing that autoimmune Addison disease is far more common in women than the medical system acknowledges are the first steps toward finally getting the right answer. From there, a root cause approach that addresses the immune environment, supports adrenal nutritional needs, and stabilizes the hormonal terrain can meaningfully improve the experience of living with this condition.




.svg)
Many people believe poor sleep happens suddenly. One week you sleep well and the next week insomnia appears out of nowhere. In reality, sleep deprivation usually develops slowly through lifestyle habits that quietly disrupt the biological systems responsible for deep restorative sleep.
Sleep quality is not controlled by one single organ or hormone. It is the result of a complex interaction between circadian rhythm, brain chemistry, metabolic health, stress regulation, and cellular energy production. At the center of these processes lies mitochondrial function. Mitochondria produce the cellular energy required for neurological signaling, hormone balance, and tissue repair during sleep.
When lifestyle habits disrupt mitochondrial function, the body gradually loses its ability to regulate sleep cycles effectively. Over time this can lead to insomnia, fragmented sleep, chronic fatigue, and even metabolic disorders.
Many individuals searching for insomnia natural remedies focus only on supplements or quick fixes. While magnesium for sleep or L theanine sleep supplements can support relaxation, long term sleep quality depends heavily on everyday habits.
At iThrive Alive we often observe that sleep deprivation effects are rarely isolated problems. They are usually the result of metabolic imbalance, circadian disruption, and chronic stress patterns that develop silently over time.
Understanding the habits that affect sleep is the first step toward restoring healthy sleep hygiene and learning how to sleep better naturally.
Sleep may appear passive, but the body performs intense biological work while we sleep. The brain detoxifies metabolic waste, tissues repair microscopic damage, and hormones regulating metabolism and immunity are released.
All these processes require cellular energy.
Mitochondria supply the ATP needed for neuronal signaling that maintains stable sleep cycles. When mitochondrial function becomes impaired, the brain may struggle to regulate sleep stages effectively.
Research on mitochondrial dysfunction and sleep deprivation has shown that reduced cellular energy can disrupt circadian signaling pathways in the brain. This leads to fragmented sleep patterns and reduced deep sleep.
For readers interested in the scientific mechanisms behind this connection, the white paper titled Mitochondrial Dysfunction Sleep Deprivation Sleep Disorders explores how mitochondrial stress influences sleep architecture.

Blue light and sleep disruption is one of the most widely studied causes of poor sleep. Digital screens emit wavelengths that suppress melatonin production. Melatonin signals the brain that it is time to sleep.
When screen time extends late into the evening, circadian rhythm becomes delayed. The brain receives signals that mimic daylight even when the body should be preparing for sleep.
Prolonged circadian disruption can alter mitochondrial gene expression and reduce cellular energy production in brain cells.
Stress activates the hypothalamic pituitary adrenal axis and increases cortisol levels. Cortisol prepares the body for alertness rather than sleep.
When cortisol remains elevated at night, the brain struggles to transition into deep sleep stages.
Chronic stress increases oxidative stress within mitochondria, impairing cellular energy production needed for sleep repair processes.
Circadian rhythm functions like a biological clock that coordinates hormone release and metabolic activity.
When sleep timing changes frequently, the brain loses synchronization with environmental light signals. This confusion affects sleep hygiene and reduces sleep quality.
Caffeine blocks adenosine receptors in the brain. Adenosine accumulates during the day and signals sleep pressure at night.
When caffeine remains in the bloodstream during evening hours, the brain cannot recognize fatigue signals.
Certain nutrients support neurotransmitter production and relaxation pathways.
Magnesium for sleep plays a role in regulating the nervous system. Deficiency can lead to restless sleep patterns.
Similarly L theanine sleep supplements may help support calm brain activity.
However nutrients alone cannot compensate for damaging lifestyle habits.
Digestion requires metabolic energy and increases body temperature. When large meals are consumed late at night the body remains metabolically active during hours meant for recovery.
Morning sunlight is essential for circadian rhythm alignment. Light exposure early in the day signals the brain to begin the biological day cycle.
Without this signal, sleep timing becomes delayed.
Physical movement supports mitochondrial biogenesis. When daily activity levels remain low, cellular energy systems weaken.
Lower mitochondrial capacity may contribute to fatigue and poor sleep quality.
Alcohol initially induces sleepiness but disrupts REM sleep cycles later in the night. This results in fragmented sleep and reduced recovery.
Sleep disorders are often symptoms of deeper metabolic disturbances. Insulin resistance, inflammation, and mitochondrial dysfunction frequently appear in individuals with chronic sleep problems.
The case study titled Functional Nutrition Obesity Hypertension Sleep Apnea Case Study highlights how metabolic dysfunction can influence sleep apnea and overall sleep quality.

While identifying habits that affect sleep is important, long term improvement in sleep quality requires a structured biological approach. Sleep is influenced by circadian rhythm signaling, metabolic stability, nervous system balance, and cellular energy production. When these systems are supported simultaneously, the body can naturally restore healthy sleep patterns.
A functional nutrition approach does not focus only on managing insomnia symptoms. Instead, it works to correct the underlying drivers of poor sleep such as metabolic stress, circadian disruption, and mitochondrial dysfunction. At iThrive Alive, improving sleep hygiene often begins by stabilizing daily lifestyle patterns, supporting metabolic health through smart eating, and providing targeted nutrients that assist cellular energy and nervous system regulation.
This approach can be understood in three interconnected steps:
Consistent sleep timing, exposure to morning sunlight, and stress regulation help reset the circadian rhythm that controls melatonin release and sleep cycles.
Whole food based eating patterns that stabilize blood sugar and reduce inflammation support the metabolic environment required for deep restorative sleep.
Nutrients such as magnesium, L theanine, and mitochondrial support compounds may assist relaxation pathways, neurotransmitter balance, and cellular energy production.

Poor sleep rarely appears suddenly. It develops gradually through everyday habits that disturb circadian rhythm, stress regulation, and mitochondrial energy production. Modern lifestyle patterns such as excessive screen exposure, irregular sleep timing, chronic stress, and nutrient deficiencies silently disrupt the biological systems responsible for restorative sleep. Addressing these factors requires more than temporary insomnia remedies. A comprehensive approach that combines lifestyle alignment, smart nutrition, and targeted supplementation can restore sleep hygiene and support mitochondrial health. By understanding how daily habits influence sleep biology, individuals can begin to rebuild the natural rhythms that allow the body to experience deep restorative sleep again.




.svg)
Most people think of snoring as a harmless nuisance. A noisy sleep habit that disturbs partners but rarely raises serious medical concern. In reality, persistent snoring can be a warning sign of deeper metabolic dysfunction taking place inside the body.
Behind the vibration of airway tissues during sleep lies a complex biological story involving energy metabolism, inflammation, hormonal imbalance, and mitochondrial stress. In many individuals, snoring is not just about the throat or airway. It reflects systemic disturbances that affect how the body produces energy, regulates blood sugar, and responds to stress.
Conditions such as obstructive sleep apnea have traditionally been approached from a mechanical perspective. Treatments often focus on airway devices or breathing support during sleep. While these approaches are important, they rarely address why the body develops this condition in the first place.
Emerging research suggests that mitochondrial dysfunction plays a central role in sleep disorders including obstructive sleep apnea. Mitochondria are the energy producing structures within our cells. When they become stressed or inefficient, the consequences ripple through metabolic pathways, inflammatory responses, and even sleep regulation in the brain.
At iThrive Alive, we approach sleep disorders through a root cause lens. Rather than treating snoring as an isolated symptom, we explore the metabolic drivers that may be quietly shaping sleep quality. Understanding these drivers can transform how we view chronic snoring and open the door to more sustainable solutions.
Snoring occurs when airflow through the upper airway becomes partially obstructed during sleep. Soft tissues in the throat vibrate as air passes through, producing the familiar sound. However, the narrowing of the airway rarely happens in isolation.
In many individuals, metabolic factors play a decisive role. Excess fat deposition around the neck and airway is one of the most obvious contributors. Yet deeper physiological disturbances often exist beneath this surface level explanation.
Hormonal regulation during sleep plays a key role in maintaining airway stability. Hormones such as leptin, ghrelin, and cortisol influence appetite, fat storage, and breathing patterns. When sleep becomes fragmented due to snoring or apnea events, these hormonal rhythms become disrupted. The result is a cycle in which metabolic dysfunction worsens sleep and poor sleep further aggravates metabolic stress.
Inflammation is another major driver. Chronic low grade inflammation can lead to swelling and fluid retention in airway tissues, increasing the likelihood of obstruction during sleep. Inflammatory cytokines circulating in the body also affect neurological signals that regulate breathing.
Perhaps the most overlooked factor is cellular energy metabolism. Neurons controlling breathing require substantial energy to maintain stable respiratory rhythms during sleep. When mitochondrial function becomes compromised, these neurons may struggle to maintain consistent signaling patterns.
This is why snoring often appears alongside metabolic conditions such as obesity, insulin resistance, hypertension, and fatty liver disease. The airway symptom may simply be the visible expression of deeper systemic imbalance.
Mitochondria are often described as the powerhouses of the cell, but their role extends far beyond energy production. They regulate oxidative balance, cellular signaling, inflammation, and metabolic coordination across multiple organs.
In obstructive sleep apnea, repeated episodes of airway obstruction lead to intermittent hypoxia. This means the body repeatedly experiences short periods of reduced oxygen followed by reoxygenation when breathing resumes. This cycle places intense stress on mitochondria.
During these hypoxic events, the mitochondrial electron transport chain becomes disrupted. Electrons leak from the system and react with oxygen to generate reactive oxygen species. In controlled amounts these molecules play useful signaling roles. However chronic overproduction leads to oxidative stress.
Over time oxidative stress damages mitochondrial DNA and impairs cellular respiration. ATP production declines, meaning cells generate less energy for normal physiological functions.
Neurons in the brainstem that regulate breathing are particularly sensitive to energy shortages. When their energy supply becomes inconsistent, respiratory control during sleep can become unstable. This instability may increase the frequency of apnea events and worsen snoring patterns.
Mitochondrial dysfunction also affects metabolic tissues such as muscle and liver. Reduced mitochondrial efficiency impairs glucose metabolism and increases fat accumulation. These changes further contribute to insulin resistance and weight gain, both of which increase the severity of sleep apnea. The result is a vicious cycle where sleep apnea damages mitochondria and mitochondrial dysfunction worsens sleep apnea.
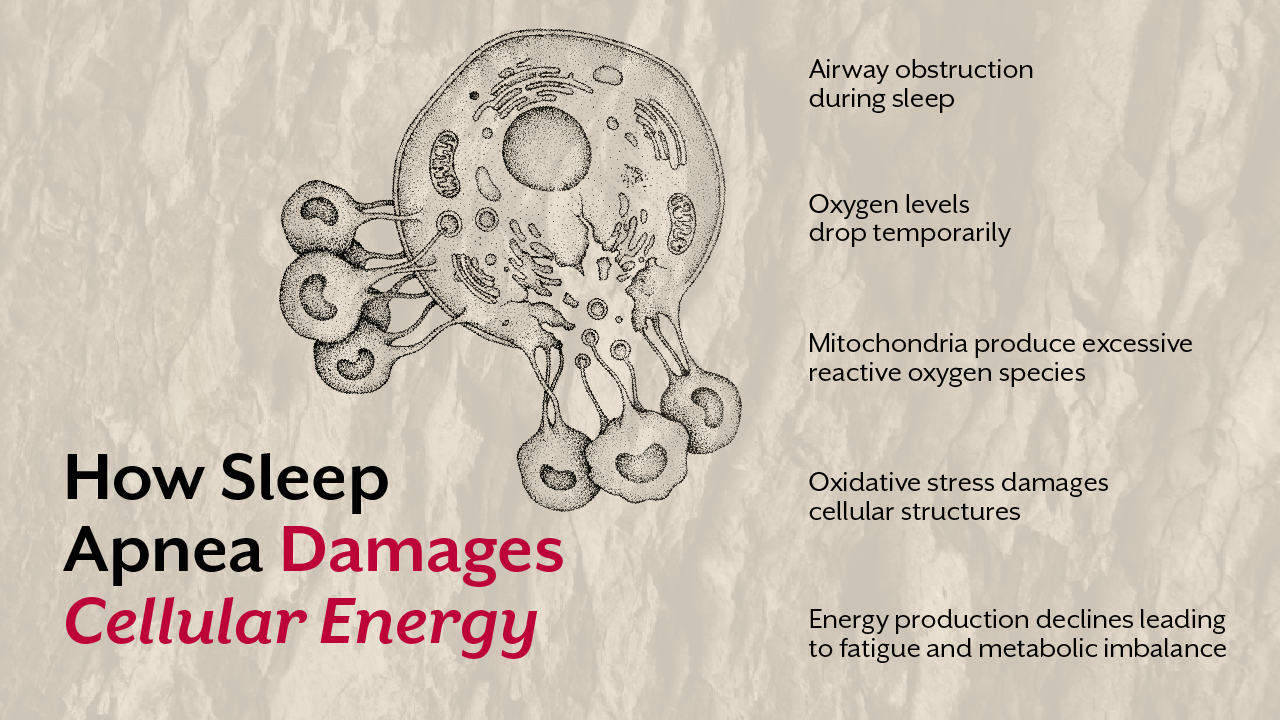
Many individuals who snore regularly also experience symptoms that seem unrelated at first glance. Persistent fatigue, brain fog, difficulty losing weight, and elevated blood pressure are commonly reported. These symptoms often indicate underlying metabolic disruption.
One of the strongest metabolic links to sleep apnea is insulin resistance. When cells become less responsive to insulin signals, glucose remains elevated in the bloodstream. The pancreas compensates by producing more insulin.
Chronically elevated insulin promotes fat storage particularly around the abdomen and neck region. This fat deposition increases airway pressure during sleep.
For readers interested in understanding this mechanism more deeply, our earlier article titled What Is Insulin Resistance and Why It Matters for Your Health explains how metabolic signaling gradually becomes impaired long before diabetes is diagnosed.
Inflammation also plays a critical role. Elevated markers such as CRP and ESR frequently appear in individuals with sleep apnea. Inflammation affects vascular health, oxygen transport, and neurological function.
Another lesser known contributor is gut microbiome imbalance. Research suggests that altered gut bacteria may influence inflammatory signaling and metabolic hormones that regulate appetite and sleep cycles. At iThrive Alive we often observe that addressing metabolic health through functional nutrition leads to improvements not only in weight and blood sugar but also in sleep quality.

Conventional approaches to sleep apnea focus primarily on mechanical solutions such as breathing devices or airway support. These tools are extremely helpful for managing symptoms, but they rarely address the biological environment that allowed the disorder to develop.
A functional nutrition approach asks a different question.
Why did the body become vulnerable to this condition?
At iThrive Alive we examine several biological systems simultaneously. Mitochondrial energy production, metabolic flexibility, inflammatory signaling, circadian rhythm regulation, and gut health all interact to shape sleep quality.
Lifestyle interventions form the foundation of this approach. Smart eating patterns that stabilize blood sugar reduce metabolic stress on mitochondria. Nutrient dense diets rich in antioxidants support mitochondrial repair and reduce oxidative damage.
Strategic supplementation may further enhance cellular energy metabolism. Nutrients such as magnesium, coenzyme Q10, and B Complex support mitochondrial respiration and neurological function involved in sleep regulation.
Circadian rhythm alignment also plays an important role. Exposure to morning sunlight, consistent sleep timing, and reduced evening screen exposure help synchronize the biological clock that governs hormone release.
Our clinical programs integrate these strategies within structured protocols such as the 3 months Alive Program. This framework allows individuals to gradually restore metabolic balance while addressing the deeper drivers behind chronic symptoms including snoring and sleep disruption.
For individuals who wish to explore their underlying metabolic drivers more thoroughly, our Root Cause Analysis consultation offers a comprehensive evaluation of metabolic markers, lifestyle factors, and nutrient status.

Snoring is often dismissed as a minor inconvenience, yet it can reveal deeper metabolic disturbances unfolding beneath the surface. Mitochondrial dysfunction, insulin resistance, chronic inflammation, and circadian disruption all interact to influence breathing patterns during sleep. When cellular energy systems become compromised, the effects ripple through hormonal regulation, airway stability, and neurological control of breathing. Addressing these underlying mechanisms requires more than symptom management. A root cause approach that integrates functional nutrition, lifestyle alignment, and targeted metabolic support offers a more comprehensive pathway toward restoring healthy sleep and long term metabolic resilience.


A complete blood panel of 60+ parameters, collected from your home by a phlebotomist. Analysis by a dedicated functional nutritionist using optimal ranges, not the standard reference ranges your doctor uses. Your symptoms, lifestyle, and health history factored into the analysis. And a 60 to 90-minute one-on-one video consultation where your nutritionist walks you through everything they found. The blood tests are included in the price. There are no hidden charges or extra cost for anything.

A complete blood panel of 60+ parameters, collected from your home by a phlebotomist. Analysis by a dedicated functional nutritionist using optimal ranges, not the standard reference ranges your doctor uses. Your symptoms, lifestyle, and health history factored into the analysis. And a 60 to 90-minute one-on-one video consultation where your nutritionist walks you through everything they found. The blood tests are included in the price. There are no hidden charges or extra cost for anything.

A complete blood panel of 60+ parameters, collected from your home by a phlebotomist. Analysis by a dedicated functional nutritionist using optimal ranges, not the standard reference ranges your doctor uses. Your symptoms, lifestyle, and health history factored into the analysis. And a 60 to 90-minute one-on-one video consultation where your nutritionist walks you through everything they found. The blood tests are included in the price. There are no hidden charges or extra cost for anything.

A complete blood panel of 60+ parameters, collected from your home by a phlebotomist. Analysis by a dedicated functional nutritionist using optimal ranges, not the standard reference ranges your doctor uses. Your symptoms, lifestyle, and health history factored into the analysis. And a 60 to 90-minute one-on-one video consultation where your nutritionist walks you through everything they found. The blood tests are included in the price. There are no hidden charges or extra cost for anything.

A complete blood panel of 60+ parameters, collected from your home by a phlebotomist. Analysis by a dedicated functional nutritionist using optimal ranges, not the standard reference ranges your doctor uses. Your symptoms, lifestyle, and health history factored into the analysis. And a 60 to 90-minute one-on-one video consultation where your nutritionist walks you through everything they found. The blood tests are included in the price. There are no hidden charges or extra cost for anything.

A complete blood panel of 60+ parameters, collected from your home by a phlebotomist. Analysis by a dedicated functional nutritionist using optimal ranges, not the standard reference ranges your doctor uses. Your symptoms, lifestyle, and health history factored into the analysis. And a 60 to 90-minute one-on-one video consultation where your nutritionist walks you through everything they found. The blood tests are included in the price. There are no hidden charges or extra cost for anything.

A complete blood panel of 60+ parameters, collected from your home by a phlebotomist. Analysis by a dedicated functional nutritionist using optimal ranges, not the standard reference ranges your doctor uses. Your symptoms, lifestyle, and health history factored into the analysis. And a 60 to 90-minute one-on-one video consultation where your nutritionist walks you through everything they found. The blood tests are included in the price. There are no hidden charges or extra cost for anything.



