Introduction
You have had psoriasis for years. The plaques come and go and you have learned to live with the skin flares. But lately something else has started. Your fingers swell in the morning. Your lower back aches in a way that feels entirely different from muscle soreness. Your nails have begun to pit and crumble at the edges. You mention this to your dermatologist and they refer you to a rheumatologist. The rheumatologist sends you back. And somewhere in that handoff, nobody explains what is actually happening inside your body.
What is happening is psoriatic arthritis. And in India, where psoriasis affects an estimated 0.44 to 2.8% of the population, studies show that 8.7 in every 100 people with psoriasis will go on to develop this joint condition, most of them between the ages of 30 and 50. That is not a small number. That is a significant portion of the psoriasis population developing a condition that can cause permanent joint damage if left unaddressed for too long.
This blog is for anyone living with psoriasis who has started noticing unexplained changes in their joints, nails, spine, or face. It is also for anyone with joint inflammation whose skin has been treated as a separate problem. These are not two separate problems. They are one autoimmune story told across two organs.
The Numbers Behind Psoriatic Arthritis in India
Before understanding the condition itself, it helps to understand how common and how underdiagnosed it actually is in the Indian context.

That nail involvement figure stands out. In 87% of Indian PsA patients, the nails show visible changes. This is a symptom that dermatologists see every day and that is almost universally attributed to fungal infection or nutritional deficiency. The missed diagnosis happens right there, in plain sight, under the nail plate.
Psoriatic Arthritis Meaning: What Is This Condition Really

Psoriatic arthritis meaning, at its most fundamental, is an inflammatory arthritis occurring in association with psoriasis. It is seronegative, meaning unlike rheumatoid arthritis, it does not produce a positive rheumatoid factor on blood testing. This single fact is why it gets missed so often. A doctor runs a standard arthritis panel, RF comes back negative, and the joint symptoms are attributed to something else entirely.
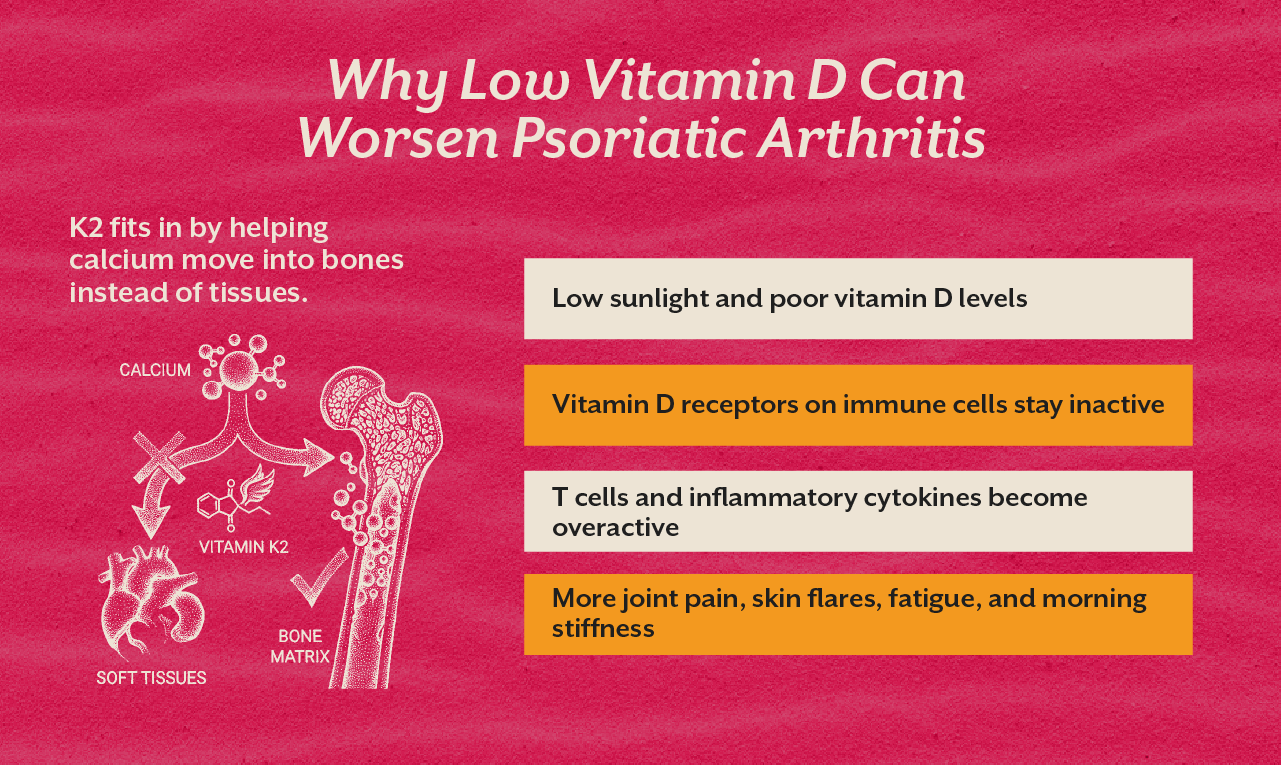
The condition is autoimmune at its core. The same immune dysregulation driving inflammatory skin plaques also drives inflammation at the joints, tendons, and entheses, the points where tendons and ligaments attach to bone. The immune system, in a state of chronic activation, attacks the body's own tissue across multiple sites simultaneously. The skin is the most visible site. The joints, spine, and nails suffer in parallel.
Psoriatic Arthritis Symptoms: Far More Than Swollen Joints

The Joints
Psoriatic arthritis symptoms present in several distinct patterns. Some people develop a symmetrical polyarthritis that closely resembles rheumatoid arthritis, affecting multiple joints on both sides of the body. Others develop asymmetric oligoarthritis, where one or two joints flare in an unpredictable pattern. Indian research shows that symmetrical polyarthritis is the most common pattern, accounting for 58% of cases, while asymmetric oligoarthritis appears in 21%.
One of the most characteristic joint signs is dactylitis, diffuse swelling of an entire finger or toe. The digit swells uniformly from base to tip, giving the classic sausage appearance. This is not seen in most other forms of arthritis and should immediately raise suspicion for psoriatic arthritis when present alongside skin or nail changes.
Psoriatic Arthritis Nails: The Most Overlooked Clue
Nail involvement is one of the most diagnostically important features of this condition and one of the most frequently misread. Psoriatic arthritis nails show pitting (small depressions across the nail surface), onycholysis (separation of the nail from the nail bed), subungual hyperkeratosis (thickening under the nail), and oil drop discolouration (a yellowish patch visible through the nail). These changes affect 87% of Indian PsA patients. They are almost never caused by fungal infection alone. If your nails look this way and you have psoriasis, you need a rheumatology assessment, not another antifungal prescription.
Psoriatic Arthritis Face
Psoriatic arthritis face involvement is less widely discussed but clinically real. Uveitis, inflammation of the eye's middle layer, causes redness, pain, and light sensitivity in a subset of patients. Temporomandibular joint involvement causes jaw pain and difficulty chewing. Psoriatic plaques on the scalp, around the ears, and along the hairline are frequently dismissed as seborrheic dermatitis rather than recognised as part of the wider psoriatic disease picture.
Psoriatic Arthritis Spondylitis: When the Spine Is Involved
Psoriatic arthritis spondylitis refers to inflammatory involvement of the spine and sacroiliac joints. In Indian studies, 49% of PsA patients show spondyloarthropathy patterns. The hallmark is morning stiffness lasting more than 30 minutes that improves with movement rather than rest. This is the opposite of mechanical back pain. Inflammatory back pain beginning before age 45 that responds to anti-inflammatory treatment warrants sacroiliac joint imaging and a rheumatology assessment.
Psoriatic Arthritis Radiology and Hand X-Ray: What the Imaging Shows

Imaging is where psoriatic arthritis reveals its most distinctive features and where a skilled radiologist can clearly differentiate it from rheumatoid and osteoarthritic changes.
Psoriatic Arthritis Hand X-Ray Findings
A psoriatic arthritis hand x-ray shows findings that appear almost paradoxical: bone erosion alongside new bone formation occurring simultaneously. The classic pencil-in-cup deformity, where the end of one bone erodes into a point and the adjacent bone cups around it, is pathognomonic for severe PsA. Periostitis which is the inflammation of the bone lining causing a fluffy appearance along the bone edge, and enthesophytes (bone spurs at tendon attachment points) are also frequently visible.
Psoriatic Arthritis Radiology Beyond the Hands
Psoriatic arthritis radiology of the sacroiliac joints shows asymmetric sacroiliitis, distinguishing it from ankylosing spondylitis which affects both sides equally. MRI is increasingly used to detect early bone marrow oedema at entheses before structural damage is visible on plain X-ray. Ultrasound of tendons and entheses can show thickening and power Doppler activity confirming active inflammation. These imaging tools are available in most Indian tertiary centres and should be requested when clinical suspicion is high.
What Is Actually Driving Psoriatic Arthritis
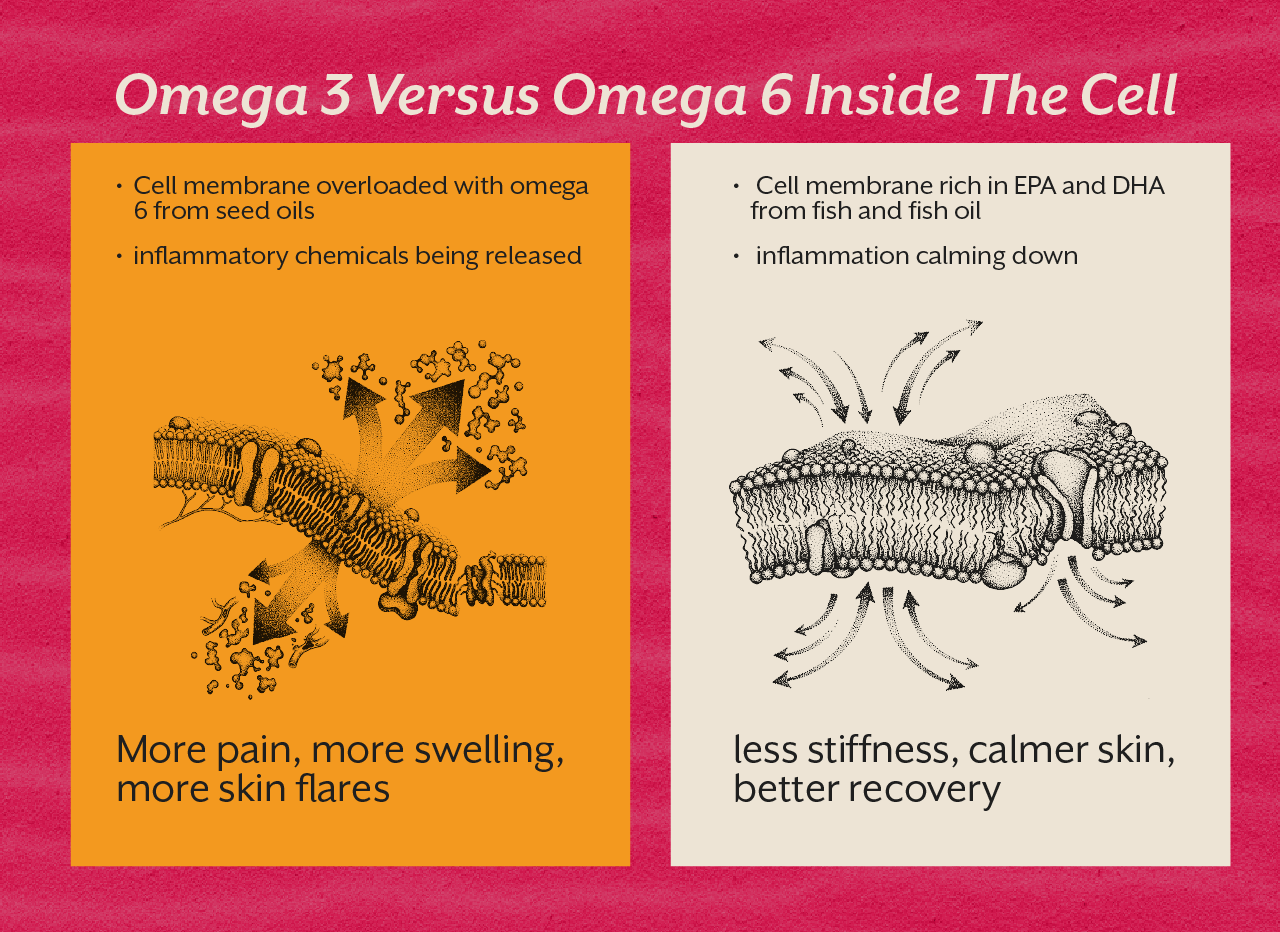
Psoriatic arthritis is not simply the result of having psoriasis for a long time. It reflects a deeper immune imbalance involving the IL-17 and IL-23 inflammatory pathways, gut microbiome dysbiosis, genetic predisposition (HLA-B27 and related alleles), and environmental triggers including trauma, infection, and metabolic dysfunction.
The gut connection is particularly significant. Research consistently shows that intestinal permeability and microbiome imbalance precede and perpetuate psoriatic disease activity. Immune cells educated in a dysbiotic gut carry inflammatory memory into the skin and joints. This is why dietary patterns, stress regulation, and gut health are not peripheral to PsA management. They sit at its biological centre.
If you are experiencing a cluster of autoimmune symptoms across multiple body systems alongside joint and skin changes, a root cause analysis can map the full inflammatory picture rather than managing each organ in isolation.
Key Takeaway
Psoriatic arthritis is a whole-body autoimmune condition wearing two faces, one on the skin and one in the joints. The fact that 83% of Indian PsA patients are newly diagnosed at the time of rheumatology referral tells us the years between psoriasis onset and arthritis diagnosis are filled with missed signals the body was already sending.
The nails were pitting. The fingers were swelling. The back was stiff every morning. And nobody connected the dots because skin and joints are treated as separate departments in a system that was not designed to see the whole person.
Understanding psoriatic arthritis symptoms, recognising psoriatic arthritis nails, knowing what psoriatic arthritis spondylitis looks like, and understanding what imaging can and cannot reveal all contribute to shortening the diagnostic gap. The earlier this condition is identified, the greater the chance of preventing the joint damage that makes it irreversible.
If the symptoms described in this blog feel familiar and you are not sure where to start, book a consult and begin with the right questions rather than another prescription for a condition that has not yet been properly named.



.svg)
.svg)