



.svg)




.svg)
It all began with an apple, the ultimate snack.
The clerics proclaimed that the act doomed humanity, but we didn’t forget the habit.
A 2015 survey from Mintel on Snacking Motivations and Attitudes in the US states that 94% of Americans snack at least once daily, and 50% of adults snack two to three times each day. Additionally, Mintel highlights that in America, regular meals may be replaced soon by more frequent snacks, and Americans feel that anything can now be considered a snack. 1
This was well over 8 years ago, and the numbers have deteriorated further during the pandemic-induced lockdowns when most of the world found itself stuck inside homes and snacking became a kind of a "lifeline" for most, which is confirmed comprehensively by the State of Snacking survey done by Mondelez International.2 The habit also seems to have stuck post-covid.
So why is snacking so dangerous, you might ask? You may think of the usual suspects such as weight gain, obesity, blood sugar imbalances, or tooth decay, but one of the most unfortunate victims of our daily snacking habits happens to be our gut—such a surprise. It turns out that digestion is a complicated operation that includes interaction between multiple organs and systems, resulting in a series of complex processes and sub-processes that eventually culminate in the ultimate alchemy of turning food into energy. One of the most important processes in our digestive tract is the Migrating Motor Complex (MMC), which gets disrupted due to frequent meals, snacks, and other multiple factors. Let us explore together this often unknown but essential process and its major disruptors. So we can all live a much more gut-friendly and healthier life.
The migrating motor complex (MMC) is a series of coordinated contractions of the muscles in the gastrointestinal (GI) tract that occurs during periods of fasting. These contractions are important for the movement of food and debris through the GI tract and are regulated by a complex interplay of hormones, nerves, and neurotransmitters. It serves to clear the stomach and small intestine of residual food and debris, helping to maintain ideal digestive function. The MMC also prevents the accumulation of bacteria and waste material in the lower intestine, which can lead to infections and other complications. The Migrating Motor Complex (MMC) is divided into four distinct phases, each with its own unique pattern of contraction and purpose.
Phase 1
The first phase, known as the quiescent phase, begins shortly after eating and lasts about 90 minutes. There is little or no activity in the GI system during this phase as the body digests and absorbs the previously eaten meal.
Phase 2
The second phase of the MMC, known as the initiation phase, occurs after the quiescent phase ends. The smooth muscles of the stomach and small intestine begin to tighten in unison during this phase, creating small and irregular waves, driving any residual food and debris toward the large intestine.
Phase 3
The propulsive phase of the MMC is characterized by high-amplitude contractions of the small intestine that transport almost all leftover food and debris toward the large intestine. This phase usually lasts about 20-30 minutes.3
Phase 4
The fourth and final phase of the MMC begins immediately after the propulsive phase. Phase four is a transition phase between phases 1 and 3. During this phase, the contractions in the GI tract slow down and eventually stop, allowing the body to rest and recover before the next phase of the MMC begins. The total time duration for the completion of MMC is estimated to be about 130 minutes. 4
The Importance of the Migrating Motor Complex (MMC)
The MMC plays many important functions in our digestive systems. The contractions of the MMC help to mix and move the contents of the GI tract, allowing for the proper breakdown and absorption of nutrients. Without the MMC, food and nutrients would not be properly digested and absorbed into our bodies, leading to malnutrition and other deficiency-related diseases. Furthermore, the MMC is involved in appetite and satiety regulation. The MMC contractions assist in sending messages to the brain suggesting that the stomach is empty and it is time to eat. The body can manage hunger and prevent overeating by adjusting meal intervals with the time and frequency of the MMC. The MMC's role in limiting bacterial overgrowth in the small intestine is also one of its most significant roles. During fasting, the contractions of the MMC serve to eliminate any residual food and debris from the small intestine, preventing germs from growing in this area. If bacterial overgrowth occurs, it may result in a condition known as small intestine bacterial overgrowth (SIBO).5 The MMC cycle also keeps other digestive diseases and disorders at bay, such as Irritable Bowel Syndrome (IBS) and Inflammatory Bowel Disease (IBD). The MMC also plays a role in preventing reflux of stomach acid into the esophagus, which can cause symptoms such as heartburn and GERD (gastroesophageal reflux disease). This helps us understand that the MMC is a critical physiological process that ensures the proper function of the gastrointestinal tract, and it is indispensable for a healthy lifestyle to keep it running in ideal condition.

Disruptors
The migrating motor complex (MMC) is a process that is easily susceptible to disruption by a variety of factors. One of the most common disruptors of the MMC is food intake. The motor complexes are activated during periods of fasting, and frequent eating disrupts the process by stimulating the release of certain digestive hormones. These hormones make the muscles of the GI tract relax instead of continuing the MMC contractions. Snacking between meals is one of the main culprits for the disruption in MMC rhythms, keeping appropriate fasting periods between meals of about 4-5 hours can help the process function smoothly. Longer fasting periods of up to 12 hours or more are required for the thorough cleaning of the colon which can be achieved through overnight fasting between dinner and breakfast. The longer fasting periods help the MMC to run multiple times clearing the GI tract completely of any residue. Eating large meals and consuming high-fat or high-protein meals can also disrupt the MMC process and are to be avoided.
All physical systems in our body are psychosomatic, and digestion is no exception. Lifestyle and emotional factors such as stress and anxiety can also disrupt the proper functioning of the MMC. Chronic stress and anxiety can lead to prolonged disruptions of the MMC, which can lead to conditions such as irritable bowel syndrome (IBS). Certain drugs can potentially interfere with the MMC. Opioids and antibiotics are well known to impede GI motility and reduce MMC activity. It is extremely important for all individuals to understand the MMC rhythms and keep them running, ideally to lead a more fulfilling life devoid of any gut issues.
Indexed References
Other References
Mintel. (n.d.). A snacking nation: 94% of Americans snack daily. Www.prnewswire.com. Retrieved April 26, 2023, from https://www.prnewswire.com/news-releases/a-snacking-nation-94-of-americans-snack-daily-300111225.html
Gagliardi, N. (n.d.). The New Way Americans Are Snacking. Forbes. Retrieved April 26, 2023, from https://www.forbes.com/sites/nancygagliardi/2014/10/13/the-new-way-americans-are-snacking/?sh=26dd71ef52e4
Consumers say snacking is a “lifeline” during pandemic, with 88% doing it more or the same. (n.d.). Food Dive. https://www.fooddive.com/news/consumers-say-snacking-is-a-lifeline-during-pandemic-with-88-doing-it-m/588779/
Deloose, E., Janssen, P., Depoortere, I., & Tack, J. (2012). The migrating motor complex: control mechanisms and its role in health and disease. Nature Reviews Gastroenterology & Hepatology, 9(5), 271–285. https://doi.org/10.1038/nrgastro.2012.57
Migrating Motor Complex - an overview | ScienceDirect Topics. (n.d.). Www.sciencedirect.com. https://www.sciencedirect.com/topics/medicine-and-dentistry/migrating-motor-complex
Deloose, E., & Tack, J. (2016). Redefining the functional roles of the gastrointestinal migrating motor complex and motilin in small bacterial overgrowth and hunger signaling. American Journal of Physiology-Gastrointestinal and Liver Physiology, 310(4), G228–G233. https://doi.org/10.1152/ajpgi.00212.2015
Deloose, E., Janssen, P., Depoortere, I., & Tack, J. (2012). The migrating motor complex: control mechanisms and its role in health and disease. Nature Reviews Gastroenterology & Hepatology, 9(5), 271–285. https://doi.org/10.1038/nrgastro.2012.57
Hasler, W. L. (2004, January 1). Duodenal Motility (L. R. Johnson, Ed.). ScienceDirect; Elsevier. https://www.sciencedirect.com/science/article/abs/pii/B0123868602001969




.svg)
Contents from this article were shared in an article published in Healthsite on 18.4.2023 featuring Mugdha. This article was written to serve as input for the same following a query from Healthsite.
Emotional trauma can get repressed and stored in the body if it is not properly processed and resolved. This can lead to physical health symptoms such as chronic pain, fatigue, gut problems, thyroid imbalances, fibromyalgia, as well as joint and bone aches. In fact, many autoimmune issues can arise from unresolved emotional trauma.
The fascia, a complex layer of nerve-rich connective tissue surrounding our organs, can hold onto stress and trauma, resulting in stiffness and pain in the body.
A healthy nervous system moves up and down naturally through states of agitation and relaxation. These are known as the sympathetic state and the parasympathetic state in medical science. When people suffer from post-traumatic issues, their nervous system gets permanently stuck in an “on” mode where it is constantly over-stimulated or an “off” mode where it is constantly depressed:
Symptoms the nervous system is stuck in “on” mode:
-anxiety
-panic
-hyperactivity
-easily startled
-inability to relax
-restlessness
-hypervigilance
-chronic pains
-sleeplessness
-digestive problems
Symptoms the nervous system is stuck in “off” mode:
-depression
-lethargy
-exhaustion
-disorientation
-chronic pain
-low blood pressure
-poor digestion
Medical literature has documented psychosomatic disorders, which are psychological conditions that result in physical symptoms that cannot be explained by medical tests or examinations. Clinical case studies have demonstrated the powerful physical effects of trauma, such as the story of a woman who became completely blind shortly after having an argument with her husband. Although medical examinations could not explain her blindness, it was eventually resolved through psychotherapy.
Conventional medicine recognizes a condition called PTSD or post-traumatic stress disorder. It is mainly though of as a mental health condition, but it is also said to affect the body in various ways. For instance, chronic pain is a common physical symptom of PTSD, and it can manifest as headaches, joint pain, muscle pain, and back pain. Gastrointestinal problems, such as irritable bowel syndrome (IBS), nausea, vomiting, and diarrhea, are also common physical symptoms of PTSD. Fatigue, respiratory issues, and cardiovascular problems, such as high blood pressure and heart disease, can also be caused or exacerbated by PTSD.
Individuals with PTSD may also experience sensory overload, which can manifest as hypersensitivity to light, sound, touch, and other stimuli. Musculoskeletal issues, such as stiffness, weakness, and reduced range of motion, may also be present in those suffering from PTSD. Dermatological issues, such as psoriasis, eczema, and hives, may also be related to PTSD. Sleep disturbances, such as insomnia and nightmares, are also common physical symptoms of PTSD. Finally, autoimmune disorders, such as lupus, rheumatoid arthritis, and multiple sclerosis, may be related to PTSD.
It is important to note that not everyone with PTSD will experience physical symptoms, and the severity of symptoms can vary widely.




.svg)
Coffee is a beverage prepared using the brewed seeds of coffee plants. Coffee is enjoyed worldwide. It is one of the top three drinks in the world. Coffee is available in all stores and breweries and is typically derived from both Coffea arabica and Coffea canephora. Arabica is considered a milder form of coffee with more flavours and aromas. While Robusta the main variety of canephora is strong in flavours. (https://www.britannica.com/topic/coffee/Processing-the-bean )
Sometimes, variation is displayed by many individuals in terms of coffee metabolism. There are some individuals who are slow coffee metabolisers, on the other hand, few individuals can metabolise coffee at a faster rate. This has raised questions in many people's minds. “Why is there a variation in coffee metabolism in populations”?
Let us try to delve deeper and gain a better understanding of the situation.
One of the main compounds found in coffee is caffeine. The caffeine molecule is the one that stimulates our nervous system. Individuals do consume coffee in order to improve their performance and get a boost as soon as they wake up in the morning.
Caffeine, on the whole, is metabolised entirely by the body. Only 3 per cent or slightly less of the caffeine is passed through the urine without being metabolised. The route of caffeine metabolism (70-80 per cent) in humans is through N-3-demethylation to paraxanthine. This reaction is carried out in the liver by CYP1A2. (Cytochrome P450 family 1; subfamily A member 2) The cytochrome P450 proteins are monooxygenases which catalyze many reactions involved in drug metabolism and synthesis of cholesterol, steroids, and other lipids. Since coffee is a form of xenobiotics, it is metabolised by CYP1A2 in the liver for the same reason.
(https://www.ncbi.nlm.nih.gov/gene/1544 )
In order to study this, human liver microsomes were studied in labs, and it was found that 1-N-demethylation to theobromine accounts for 7 to 8 percent (percent) of caffeine metabolism. While caffeine metabolism with 7-N-demethylation to theophylline accounts for 8 per cent. 1,3,7-trimethyluric acid is formed from C-8 hydroxylation, which adds up to 15 percent percent of caffeine metabolism.
Previous studies conducted to understand coffee metabolism have elucidated that on average coffee has a half-life of 2.5 to 5 hours in the system. Similarly, half-lives from 2.5 to 9.9 hours have been recorded based on interindividual variations.
As discussed in the above paragraphs, CYP1A2 carries out the conversion of caffeine in the liver. However, there are individual variations observed. These individual variations make a person either a slow or fast metaboliser. An SNP (Single Nucleotide Polymorphism) from A to C at the 163rd of the CYP1A2 gene plays a role in this. Those individuals who have “C” are slow metabolisers, which means caffeine would take 10-12 hours to get metabolised in their system. This causes dizziness and jitteriness in these individuals. On the other hand, individuals with type “A” will metabolise caffeine within 3–4 hours and don’t experience dizziness and jitteriness symptoms.
There are various factors that affect the coffee metabolism of individuals. Age, hormones, liver diseases, genetics and even diet could play a role in how caffeine is metabolised. Let's go over these elements in more detail below.
Age:
In neonates (under 28 days old), it is observed that caffeine clearance is slightly slower compared to adults. It is shown that their coffee metabolism takes 65 to 105 hours. This could be the fact that the organs are still developing in neonates. In humans, age does not appear to affect caffeine clearance, whereas, in rats, the caffeine half-life increases in an age-related manner.
(https://pharmrev.aspetjournals.org/content/70/2/384)
Sex and Hormones:
Studies have shown that the CYP1A2 enzyme is more active in males compared to females. However, there is no difference in the urinary metabolites observed in terms of the metabolites excreted from the urine.
(https://pharmrev.aspetjournals.org/content/70/2/384 )
Along this, it is observed that during pregnancy, the metabolism of coffee is slowed down. Once the pregnancy is over, the metabolism returns to its preconception state. This is because the CYP1A2 CYP1A2 activity decreases during late pregnancy.
(https://pharmrev.aspetjournals.org/content/70/2/384)
Liver Diseases:
Individuals with hepatitis B, C, or cirrhosis take longer to clear coffee from their systems. This is primarily due to the synthesis of paraxanthine in the liver. This is primarily due to the fact that these diseases affect the various activities of the liver, and since CYP1A2 activity is highest in liver there is increased half-life of coffee which can go upto 50-160 hours. Thus, the synthesis of paraxanthine is hampered which is the first step in caffeine breakdown.
(https://pharmrev.aspetjournals.org/content/70/2/384)
Diet:
Caffeine clearance and its half-life are quite significantly affected by grapefruit consumption. The difference that is observed is 23% increase in clearance and 31% increase in half-life. Consumption of foods rich in vitamin C helps increase the clearance of coffee. Apiaceous vegetables (such as carrots, celery, parsley, caraway, fennel, etc) decrease CYP1A2 activity.
(https://pharmrev.aspetjournals.org/content/70/2/384 )
In South Asian countries, the activity of CYP1A2 is significantly decreased since they cook their foods with ingredients containing curcumin, which downregulates the activity of CYP1A2.
(https://pharmrev.aspetjournals.org/content/70/2/384)
Similarly, it is advisable to consume coffee 60-90 minutes after waking up in the morning. This is because once we wake up there are still adenosine receptors which need to be cleared out and caffeine acts as an adenosine blocker. If this is not followed, the remaining adenosine receptors are blocked. These will get activated in the afternoon, or the caffeine effects will be washed off, causing “the afternoon crash” observed by many coffee drinkers. Thus, it again depends on individuals genetic make up and well being.
To sum up the discussion, we can say that there are various interindividual differences that dictate the way in which coffee will be metabolised in the system. It is advisable to discuss with your healthcare healthcare provider or nutritionist the ups and downs of coffee for yourself in particular.




.svg)
Are you a morning person? Do you take an afternoon nap? Do you like to sleep in until the afternoon? All these are the different sleep preferences that differ among people. Did you ever think your sleeping pattern might affect your dietary intake? It's becoming increasingly obvious that what you eat matters just as much as what you consume. The timing of our meals affects our capacity to break down, digest, and metabolise food and our physical and mental functions.
Everyone has different sleeping habits, behaviours, and personality traits based on factors such as age, activity level, and sleeping environment. The individual circadian cycles that characterise people's degrees of alertness and activity throughout the day, known as "chronotypes," are used to categorise these activities.
Due to Earth's rotation around its axis, almost all life on the planet employs an internal biological clock. Animals can really "know" the time of day because of natural daily cycles known as "circadian rhythms" (1). There is an endogenous time system in the suprachiasmatic nuclei (SCN) in the hypothalamus area of mammals' brains. The SCN of the brain's anterior hypothalamus receives signals of light and dark over a 24-hour period and serves as the "central clock" for this internal clock system (2).
Chronotype displays choices for when to carry out everyday tasks (3). A person's attitude defining personal preference for a circadian rhythm in behavioural and biological rhythm in relation to the external light-dark cycle is known as their "chronotype. Based on the variations in circadian behavioural phenotypes, chronotypes may be divided into three main categories: morning, evening, and intermediate chronotypes (4). Studies have shown that people with a morning chronotype tend to wake up early and enjoy activities earlier in the day. In contrast, people with an evening chronotype often wake up late and choose to perform activities later in the afternoon and evening. The intermediate chronotype is for people who follow the sun; they work well during office hours and also don't have any problem keeping a social nightlife. People with the evening type of chronotype are more likely to have greater rates of metabolic dysfunction, cardiovascular illness, and mental symptoms (5).
The relationship between circadian cycles, metabolic functions, and nutritional intake is unbreakable. The timing of food intake may be altered as a temporal cue for the circadian system and is subject to various influences, such as an individual's chronotype (6). A study done on the association between chronotype and timing of energy and macronutrient intakes showed that the evening type had a generally lower intake of energy and macronutrients in the morning and a greater intake in the evening than the morning type, which was related to delayed energy and macronutrient intake timing (7).The synchronisation of our internal central and peripheral clocks with the external environment's light and darkness controls our circadian rhythms, thus helping us to sleep at night and even regulate our dietary intake during the day. Key metabolic functions also follow a circadian cycle to correspond with this behaviour, which explains why morning levels of glucose tolerance, insulin sensitivity, and food's thermic effects are higher than afternoon and evening levels (8).
Adults have circadian patterns of eating, as well as comparable cycles of gut motility, the production of digestive juices, the absorption of meals that have been digested, and blood levels of lipids, amino acids, and carbs (9). Evidence shows that in evening chronotype people, those who have insufficient, disruptive, and late sleep are linked to a low intake of carbohydrates and a low dietary quality but a high fat intake (10).
A study done on the dietary intake of people with different chronotypes showed that, in comparison to other chronotypes, evening types are more frequently physically inactive and have worse subjective health (11). Evening chronotype is linked to higher BMI, binge eating patterns, and higher evening energy intake, especially from less fresh produce and more fast food and alcohol. Contrarily, the morning chronotype is inversely correlated with disinhibition and sensitivity to hunger and positively correlated with cognitive restraint. The chronotype affects the link between meal timing and BMI. This raises the possibility of an interaction between chronotype and meal time on hunger and eating behaviour (12).
Recent research has linked sleep deprivation and later bedtimes to an increased risk of obesity. Other weight-related behaviours may be influenced by circadian preference. People with evening chronotypes typically exercise less frequently, watch TV more, and consume fast food more frequently. The timing of meals and exercise also affects metabolism and the likelihood of gaining weight (13).
We attempt to comply with societal expectations by eating and sleeping at specific times. Still, in the end, we are all unique, and we need to identify our optimal state and make every effort to achieve it. Try eating before 9 p.m.; otherwise, it may affect your metabolism, according to the literature, so try eating early. You can schedule your meals to maintain a healthy metabolism and lower health risks by being conscious of your eating and sleeping patterns.



.svg)
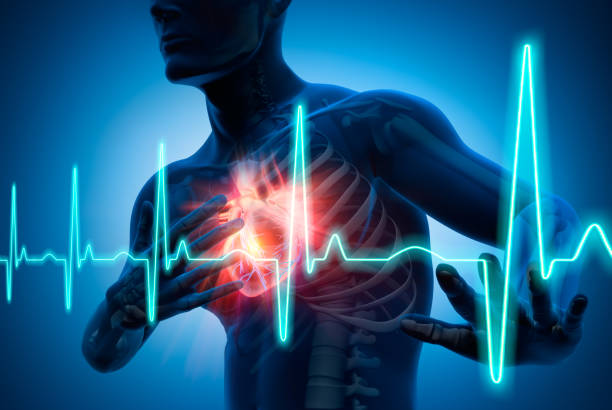
Hypertension can be a sneaky condition. You might not even know you have it until it's been present for a while. But don't let its silent nature fool you; it can have serious consequences if left untreated.
In simple terms, hypertension occurs when the pressure of your blood against your artery walls is consistently too high. Think of it like a balloon that's being over-inflated. While a normal blood pressure reading is 120/80 mmHg, hypertension is diagnosed when it consistently exceeds 140/90 mmHg.
This chronic medical condition is quite common, affecting millions of people around the globe. Unfortunately, Hypertension is a common health problem that affects millions of people worldwide. According to the World Health Organization (WHO), hypertension is a leading risk factor for cardiovascular disease, stroke, and kidney disease. So it's important to be aware of the signs and symptoms, and to take steps to manage your blood pressure if necessary.

Hypertension comes in two types, each with its own causes.
Pulmonary hypertension is another type of hypertension that affects the arteries in the lungs and right side of the heart. In one form, called pulmonary arterial hypertension (PAH), blood vessels in the lungs are narrowed, blocked, or destroyed. This slows blood flow through the lungs, causing the blood pressure in lung arteries to rise. The heart must work harder to pump blood, eventually causing the heart muscles to weaken and fail. Although there is no cure for some types of pulmonary hypertension, early detection and treatment can help manage symptoms and improve quality of life.
To help reverse pulmonary hypertension at home, limit salt intake and avoid excess water consumption. People with PAH tend to retain water, which can cause painful fluid retention in the abdomen and legs. Avoid high-sodium foods like chips, lunch meat, canned foods, frozen foods, and fast food. Light exercise and restful sleep are also helpful in managing pulmonary hypertension.
Portal hypertension is caused by high pressure in the portal venous system, which leads to the liver. The most common cause of portal hypertension is cirrhosis of the liver. People with advanced liver disease, such as cirrhosis, have an increased risk. Report any unusual symptoms to your doctor, such as gastrointestinal bleeding, ascites (abdominal swelling), encephalopathy (confusion), jaundice (yellowing of skin and eyes), leg swelling, or caput medusa (visible network of dilated veins around the navel).
Hypertension is often referred to as the "silent killer" because it may not cause any noticeable symptoms until it has reached a dangerous level. However, some common symptoms of hypertension may include:
It is essential to monitor your blood pressure regularly to catch hypertension early before it leads to severe health problems.
Diagnosing hypertension is easy and straightforward. Your doctor can check your blood pressure during a routine visit. If they don't check your blood pressure, feel free to ask for it.
If your blood pressure is high, your doctor may ask you to have more readings over several days or weeks. They usually don't diagnose hypertension after just one reading. That's because your blood pressure can be influenced by different factors, like stress or the time of day.
If your blood pressure remains elevated, your doctor may perform some tests to rule out any underlying conditions that might be causing it. These tests can include cholesterol screening, blood tests, an electrocardiogram, an ultrasound of your heart or kidneys, or monitoring your blood pressure at home for 24 hours.
These tests can help your doctor identify any secondary issues causing your high blood pressure and evaluate the effects it might have had on your organs.
During this process, your doctor may begin treating your hypertension. Early treatment can help reduce your risk of lasting damage.
Hypertension can be managed through lifestyle changes, medication, or a combination of both. Making healthy lifestyle changes can help control blood pressure levels, and some changes may include:
If lifestyle changes alone are not enough to control hypertension, medication may be necessary. Several types of medication can lower blood pressure, including:
If you're concerned about developing hypertension, there are some simple lifestyle changes you can make to lower your risk and avoid complications.
1. What is the medical term meaning high blood pressure?
Hypertension is the medical term given to High Blood Pressure. High blood pressure or “BP” has sadly become a household term these days. One should know the exact biochemical processes that occur in the body, which leads to the conclusion that someone has hypertension.
2. How does pulmonary arterial hypertension affect the lungs?
It is a type of high blood pressure that affects the arteries in the lungs and the right side of the heart. In one form of pulmonary hypertension, called pulmonary arterial hypertension (PAH), blood vessels in the lungs are narrowed, blocked or destroyed. The damage slows blood flow through the lungs, which results in the blood pressure increase.
3. What is high blood pressure measured in?
Blood pressure is measured in millimetres of mercury (mm Hg), and it has two numbers:
• Top number (systolic pressure). The first, or upper, number measures the pressure in your arteries when your heart beats.
• Bottom number (diastolic pressure). The second, or lower, number measures the pressure in your arteries between heart beats
4. What are the stages of hypertension?
Stage 1 hypertension: The systolic number is between 130 and 139 mm Hg, or the diastolic number is between 80 and 89 mm Hg. Stage 2 hypertension: The systolic number is 140 mm Hg or higher, or the diastolic number is 90 mm Hg or higher.
5. What do the blood pressure numbers mean?
Blood pressure is measured in millimetres of mercury (mm Hg), and it has two numbers :
• Top number (systolic pressure) - The first, or upper, number measures the pressure in your arteries when your heart beats.
• Bottom number (diastolic pressure) - The second, or lower, number measures the pressure in your arteries between heart beats.
6. How is blood pressure determined?
Blood pressure is determined both by the amount of blood the heart pumps out as well as the amount of resistance to blood flow in the arteries. The more blood your heart pumps and the narrower your arteries, the higher your blood pressure. This is essentially known as High BP or hypertension.



.svg)
Contents from this article were shared in an article published in TV9 Hindi on 9.3.2023 featuring Mugdha. This article was written to serve as input for the same following a query from TV9.
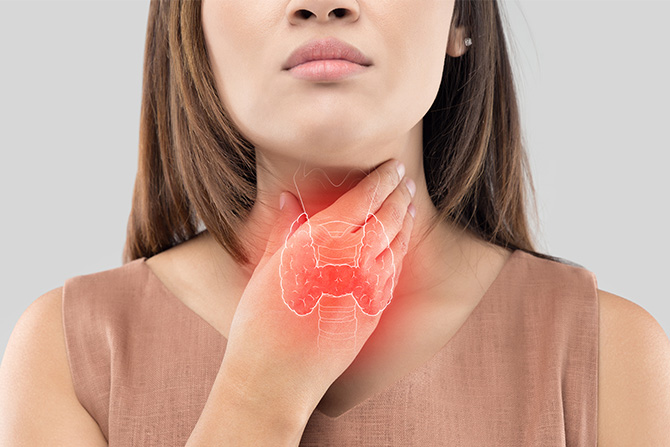
The thyroid gland is a small butterfly-shaped gland in our neck. It produces thyroid hormones which play critical roles in our body function. In particular, they control the rate of metabolism or the rate at which our body is running and burning energy.
The thyroid gland and its associated hormones make a very complex, sophisticated system. This is why it isn't easy to treat thyroid dysfunction. There are a number of different things that could go wrong and the reason for the same is much more so. This is why it can often be difficult to uncover the root cause of thyroid dysfunction.
Thyroid issues, particularly hypothyroidism are known to have a much higher prevalence among women than men. According to the Cleveland Clinic, women are about 5 to 8 times more likely to be diagnosed with a thyroid condition.
But what is the reason for this vast disparity? There isn’t a single big reason for it. Some of the different ways in which women differ from men make them more prone to this condition:




.svg)
Water chestnut, or singhara, or shengada, is an aquatic tuber that grows in freshwater marshes. It is not a nut, as the name suggests. It is native to Asia, tropical Africa, and Oceania. Fresh water chestnuts are crisp and delicately sweet. It is rich in various vitamins, phosphorus, magnesium, calcium, iron, iodine, and ample dietary fibre1. It is a great source of antioxidants and helps fight free radicals, thus preventing cell damage 2.
Water chestnut is known to have effects on the thyroid gland because of its high nutrient composition. The thyroid gland is a ductless endocrine gland that is situated at the front of the neck, releasing two thyroid hormones, T3 (Triiodothyronine) and T4 (Tetraiodothyronine).
The proper functioning of thyroid hormone is beneficial for the proper functioning of the overall body. Factors like food habits, lifestyle, hormonal imbalance, medications, and environment can affect the secretion of thyroid hormone. Over secretion of thyroid hormone leads to hyperthyroidism, whereas a decrease in thyroid hormone secretion gives rise to hypothyroidism 3.
Your metabolism may increase as a result of hyperthyroidism. A quick pulse, weight loss, increased hunger, and anxiety are all signs of hyperthyroidism. Antithyroid medications, radioactive iodine, beta blockers, and surgery are all options for treating hyperthyroidism. The physical symptoms of hypothyroidism frequently range across individuals and might be challenging to pinpoint. The timing and intensity of the signs and symptoms are also influenced by the condition's severity. Fatigue and weight increase are two early signs. Note that regardless of how well your thyroid is functioning, these both grow more prevalent as you age.
One of the most important micronutrients, iodine, is important for thyroid hormone biosynthesis 4. Iodine deficiencies remain unnoticed for years. Over time, one might feel fatigue and slow down their metabolism.
Water chestnuts are rich in iodine, which is required for the proper functioning of the thyroid gland. It keeps the thyroid levels in check 5. Thyroid hormone production requires two main ingredients, thyroglobulin and iodine. Thyroglobulin is an important thyroid hormone precursor protein that is released from follicular cells after binding to and releasing thyroid stimulating hormone (TSH) into the colloid. Iodine is a dietary supplement that is absorbed from our intestine into the bloodstream as iodide. This iodide is then further transported to the colloid for the synthesis of thyroid hormone 6.
Shengada, or the water chestnut, is thus a convenient source of iodine. Cooked or uncooked shengada can be kept for 4-5 days.
Winter is here with your crispy and crunchy friend, thus taking care of your butterfly gland!




.svg)
Our emotional, psychological, and social well-being are all parts of our mental health. It influences our thoughts, emotions, and behaviors. Additionally, it influences how we respond to stress, interact with others, and make good decisions. Mental health is important at every stage of life, from childhood and adolescence through adulthood. These days, unstable mental health is fairly prevalent.
Both physical and mental health are crucial aspects of overall health. For instance, depression raises the danger of many different physical health issues, especially chronic diseases like diabetes, heart disease, and stroke. In a similar way, having chronic illnesses can raise the chances of mental disease.
Athletes frequently neglect their mental health in an effort to maintain their physical health and performance at their highest levels, leaving them susceptible to mental diseases like depression and anxiety. Most often, athletes worry about competing and winning, which might make them more anxious.
Many college players and professional athletes suffer from mental health issues in one way or another. Although depression is the most prevalent mental health condition among professional athletes, many of them also frequently experience stress, anxiety, a variety of eating disorders, and signs of burnout.
Due to their problems, they find it challenging to attend regular practice sessions, which makes them more likely to neglect their physical health. In this situation, athletes should focus on mental health, which is just as important as keeping up their optimal physical health.
Finding a player who may be struggling with mental health issues is the hardest hurdle. The pressure to serve as a role model for their fans, following, and even peers is frequently placed on athletes and professional players. As a result, they are reluctant to seek assistance or professional support or to open up to someone about the problems that trouble them.
The first step in helping someone with a mental health illness is to be there for them. Even just listening without making judgements can be quite beneficial.
The most crucial steps towards recovery involve enabling athletes to control their stress levels with simple but efficient stress management techniques and helping them in creating healthy coping mechanisms moving forward. In the long run, making a consistent effort to put their mental health above everything else can have the biggest impact.
We are all aware of the connection between mental wellness and optimum performance. Any changes in behavior, attitudes, or feelings that adversely affect a person's thoughts, feelings, or behaviors are referred to as a mental illness. Athletes experience a special set of pressures that are associated with mental illness, despite the fact that exercise and athletics have numerous good effects on mental health, including boosting self-esteem, social support, and connectivity. There are several instances, including increased academic pressure, longer playing seasons, coach pressure to win, injuries, identity defined by athletic performance, and body weight.
Depending on the individual and the unique mental health challenge, different mental health issues have different effects on an athlete's performance. But it is well known that issues with mental health have a significant impact on sports performance. Athletic performance is impacted by stress, anxiety, depression, eating disorders, trauma, drug addiction.
Sports performance can be impacted by stress in a variety of ways. Lack of sleep can make it more difficult to deal with stress both within and outside of sport. The stress put on by the pressures of competition can affect the quality and quantity of sleep. Stress can impair concentration and heighten muscle tension, making athletes more susceptible to injury and sporting injury is a big stressor in and of itself. Athletes who have been injured may face loneliness, worry, sadness, and fear of sustaining another injury or losing their spot on the team while undergoing recovery.
A typical response to the pressures of competition, performance anxiety is common in sports. Additionally, in some cases, help athletes in concentrating their energy and concentration on the competition. At a point worry stops helping and actually starts to hurt athletic performance. It can have an impact on an athlete's focus and sense of self-worth, leading them to act erratically, which can exacerbate their anxiety and self-doubt. If untreated, anxiety associated with sports can continue to have a negative effect on an athlete's ability to perform well in both practice and competition.
An athlete's ability to perform can be impacted by depression in a number of ways. A sign of depression is a loss of interest in activities, and depressed athletes struggle to perform effectively in their sport. Sleep patterns that are disturbed can also be a sign of depression. For athletes to function at their best, they must get enough sleep. Aches, pains, and cramps are some of the physical side symptoms of depression that can make training and competition challenging. Because it can progress to suicidal thoughts and attempts if depression is not addressed, it is a particularly serious mental health disorder.
For athletes to be able to sustain their performance, it is crucial that they should learn good coping mechanisms for stress. One of the main objectives of stress management in sports is to enable athletes to control competition-related stress effectively to enhance psychological well-being and optimal performance.
There are various methods and strategies that can help with stress management. Even so, the objective of any successful stress management strategy is to identify techniques that one will regularly apply and which reduce potential levels of stress. In order to identify when they need to take a break and make a change in order to prevent becoming chronically stressed, it is crucial for athletes and coaches to understand what stress looks like. This information is crucial because it can direct people towards stress-reduction strategies that are tailored to their requirements.
Any professional athlete can benefit from some useful coping mechanisms when it comes to stress.
All athletic effort and success are built on a foundation of motivation. All other mental aspects, such as confidence, intensity, attention, and emotions, are meaningless if you don't have the motivation and commitment to enhance your athletic performances. You must have the desire to put in the necessary effort to realize your potential and achieve your goals if you want to be the best athlete. Sports motivation is crucial since it requires you to continue through fatigue, boredom, discomfort, and the need to do other things. Everything that affects your athletic performance will be impacted by motivation.
There are four signs of less motivation in athletes-
Having the highest level of motivation involves giving your sport everything you have got—all of your time, attention, focus, and energy. It involves putting every effort to improve your athletic prowess. When you experience lack of motivation, concentrate on your long-term goals. Remind yourself of the purpose of your efforts. Tell yourself that the only way you will be able to achieve your goals is to keep working hard. Visualize exactly what you want to accomplish.




.svg)
Toxins are compounds that damage an organism upon exposure. Toxins can be as simple as an ion or an atom, and they interfere with normal cell function. Toxins can also take the form of complex molecules, such as snake poison 1.
Toxins can be found in almost all the compounds present on the planet. Water molecules can also be toxic if taken in large amounts. Excess water in the body can cause cells to burst open due to the increased pressure in the cells 1.
Toxins can be found as simple charged particles, and they cause havoc in the reactions occurring in the human body. Toxins can also be proteins, which can affect the nervous system. Animals produce toxins to "restrain" or defend themselves from predators. Thus, evolutionary research concluded that organisms that produce toxins are so intelligent that they can identify the predator that poses a threat to their survival, and as a result, animals have developed toxins to counteract these predators 1.
Let's take an example to understand this better. Snake venom is composed of different types of proteins. These proteins attack the organism's cells in various ways. In some snakes, the venom attacks the nervous system, while in others, the venom attacks the tissues of the organism. Pesticides, for example, are designed to kill insects but not other animals because they are tailored to the anatomy of the target organism. Pesticides are observed to accumulate in organisms after decades of use. According to research, the eggshells of birds have thinned over time. DDT is a pesticide used in fields to protect crops from insects, and as a result, DDT is consumed by insects. After their deaths, these insects are in turn consumed by organisms of higher trophic levels, with the DDT starters biomagnifying in the food chain. Since birds are part of this food chain, DDT biomagnifies in birds, affecting their Ca-ATpase pump and leading to thinning of the egg shells and resulting in reproductive issues.
Toxins can also be found in food. Sometimes toxins can arise in food due to processing, handling, or contamination. These toxins can cause havoc in our bodies. It can lead to nausea, vomiting, abdominal pain, and diarhhoea 2.
Seafood and the toxins found in it are pretty much a hot topic all throughout the world. Seafood poisoning includes ciguatera, scombroid fish poisoning, puffer fish poisoning, and paralytic shellfish poisoning. Seafood poisoning occurs when a person consumes a tissue from a fish that contains heat-resistant toxins that enter the body 3.
Let's look into these seafood toxins in depth to get a better understanding.
This type of toxin is usually found in coral reef fishes such as leopard coral grouper, two-spot red snapper, lyretail grouper, flowery grouper, moray eel, spotted coral grouper, tiger grouper, and humphead wrasse. Toxins ingestion through fish causes the following symptoms: numbness of the mouth and limbs, vomiting, diarrhoea and pain in joints and muscles 3.
Paralytic shellfish poisoning usually occurs after consuming bivalve fish such as scallops, mussels, oysters, clams, cockles, and xanthid crabs. If a person becomes ill as a result of eating these shellfish, they may experience symptoms such as tingling or numbness throughout their bodies, as well as respiratory paralysis 3
Toxins cannot be eliminated through processing. Ciguatera toxins, for example, cannot be removed even by boiling or steaming the fish. The same is true for paralytic shellfish poisoning as well. While in the case of scrombiod toxins, the best way to avoid the toxins' formation is to refrigerate the fish with proper hygiene as soon as the fish is caught. Similarly, cooking does not decrease the risk of these toxins. One cannot identify fish containing toxins just by looking at the fish, as toxins are odourless and tasteless.
One way to avoid the risk of seafood poisoning is to avoid consuming the intestine, head, and liver of fish, which could be harbouring these toxins. Similarly, in terms of shellfish, make sure to avoid purchasing shellfish from sources that might have reported a past history of paralytic shellfish poisoning. Another way is to maintain hygiene during fish capture, transportation, and storage, which might reduce the risk of toxin formation.
References:-


The blog covers functional nutrition, chronic conditions, gut health, hormonal health, autoimmune conditions, sleep, mental health, and root cause analysis. Every article is written to help you understand what is actually happening inside your body, not just manage symptoms.

All articles are written by the content writers in collaboration with iThrive's clinical team of functional nutritionists, guided by the same methodology used in the ALIVE programme. The content is rooted in functional medicine and real clinical experience, not generic health advice.

No. The blog is an educational resource to help you understand your health more deeply. If you are experiencing symptoms or managing a chronic condition, a personalized Root Cause Analysis with a functional nutritionist is the right next step.

Book a Root Cause Analysis. For ₹2,500, a dedicated functional nutritionist will assess 60+ blood markers using optimal ranges and explain exactly what is driving your condition. It is the natural next step after reading about what might be happening in your body.

Yes. Many of our readers come with existing diagnoses and find the blog helps them understand why their condition developed and what their body actually needs. The articles are designed to give you clarity, not replace the guidance of a practitioner.



