It starts with a cramp that won’t quit …
You curl up on the couch clutching a hot‑water bottle, telling yourself it’s “just period pain.” But the relief never comes. A week later you’re doubled over after a bowel movement during intimacy the stabbing ache returns, and the fatigue feels bone‑deep. Friends say it’s normal. Your gut says otherwise. That gut feeling matters because endometriosis also called the “missed disease” takes an average of 8 - 9 years to be diagnosed.
1. What is Endometriosis?
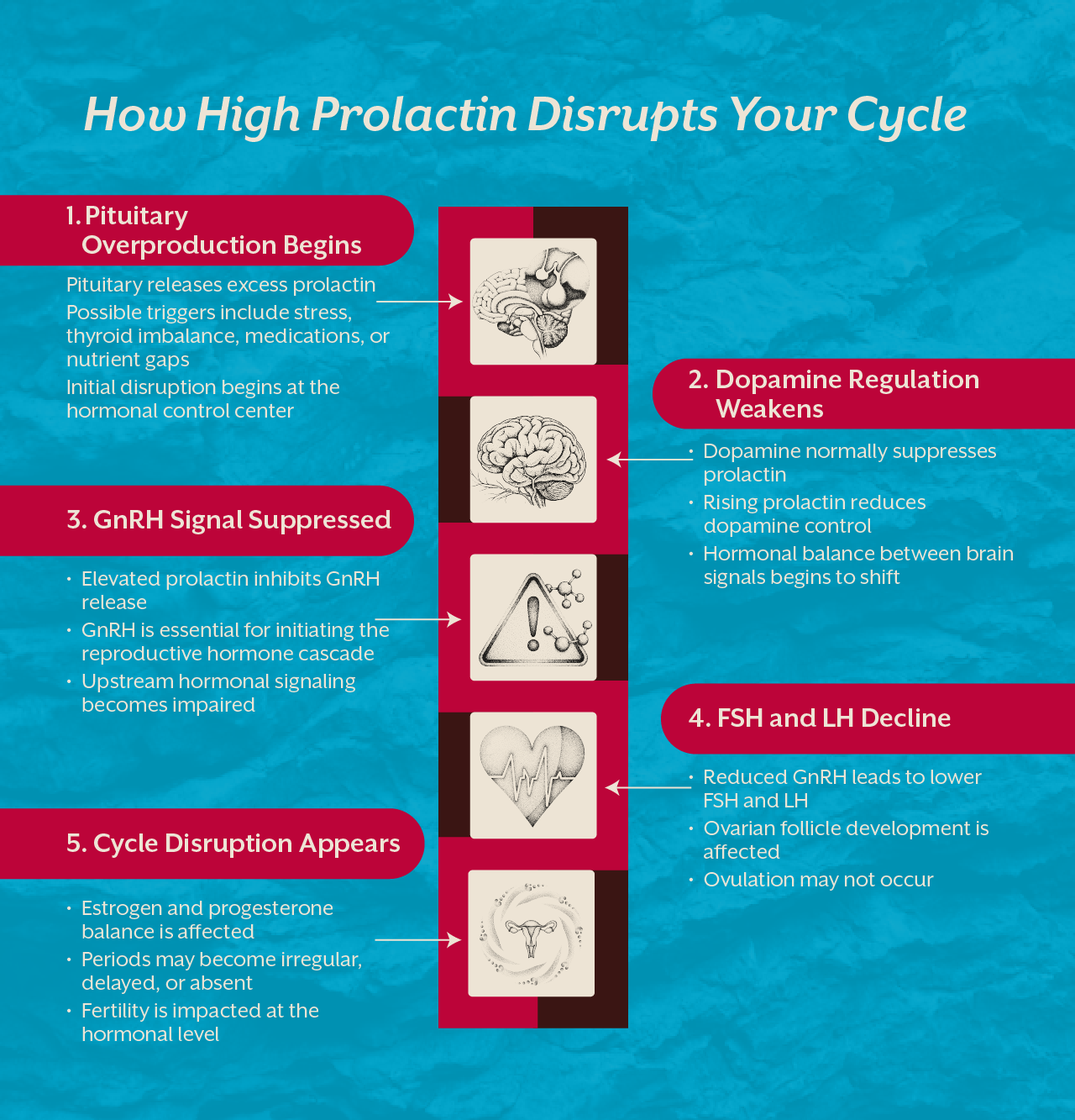
Endometriosis is an estrogen‑driven inflammatory disease in which tissue that looks and acts like the uterine lining that is “endometrium” implants itself outside the uterus on ovaries, fallopian tubes, bowel, bladder, even the diaphragm. Every cycle these rogue cells respond to hormones, bleed, and trigger scar‑forming inflammation, leading to pain, infertility, and organ dysfunction. About 1 in 10 menstruating people world‑wide are affected.
2. Endometriosis Symptoms - How It Shows Up

- Pelvic or lower‑back pain that is cyclical or constant
- Painful, heavy, or longer‑than‑usual periods
- Pain with during or after sex - dyspareunia
- Painful urination or bowel movements, especially around menstruation
- Unexplained bloating or IBS‑like gut issues
- Chronic fatigue, brain fog
- Infertility or repeated pregnancy losses
- Occasional chest or shoulder‑tip pain
Remember: The severity of pain does not always match the amount of visible disease. Tiny lesions can hurt just as much as extensive ones.
3. Why Does Tissue Wander? Understanding the Causes
There is no single culprit, think of endometriosis as a perfect storm of hormonal, immune, genetic, and environmental factors.
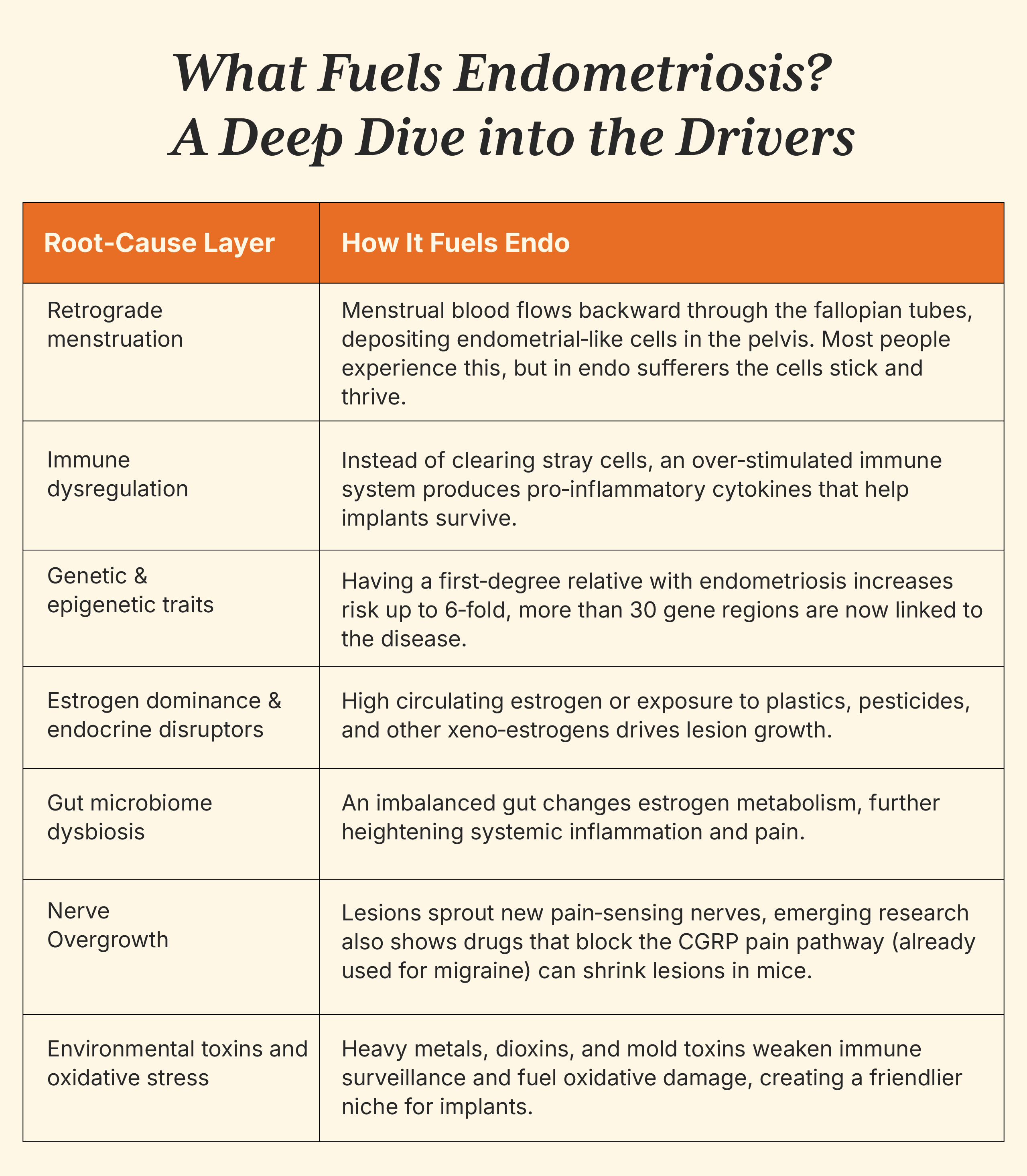
4. Who’s Most at Risk?
- Early menarche (< 12 years)
- Short cycles (< 26 days) or heavy menstrual flow
- Nulliparity (never having given birth)
- Low BMI or rapid weight loss
- Family history of endometriosis or adenomyosis
- Environmental toxin exposure in utero or childhood
Important: Endometriosis is dangerous not because it is cancer, but because unchecked inflammation can damage the ovaries, bowels, bladder, and nerves, drastically impacting quality of life and fertility.
5. iThrive’s Functional Healing Lens
Conventional therapies often chase symptoms, but at iThrive Alive we ask, Why is your body creating an inflammatory playground for these cells? Our Root‑Cause Analysis (RCA) uses advanced labs to probe:
- Hormonal imbalances through advanced blood markers and DUTCH hormone testing
- Gut‑microbiome & leaky‑gut markers
- Heavy‑metal, mold‑mycotoxin & chemical toxin load
- Inflammatory cytokine and immune profiles
Diet & Supplementation - Food as Medicine

Eliminate gluten, conventional dairy, processed soy, refined sugar, alcohol, and seed oils, as all of these are linked to gut permeability and estrogen imbalance.
Emphasize on proteins involving chickpeas, free range eggs, and chicken. Also focus on omega‑3‑rich foods such as walnuts, ghee, coconut oil, seafood, and pumpkin seeds. Lastly, ensure to have herbs such as turmeric, ginger, black pepper, and garlic.
Targeted supplementation - based on LAB TESTS, not TRENDS
- Magnesium bisglycinate to calm nerves and cramps
- Probiotics to restore the estrobolome
- Detox binder and detox tea for detoxification
- CoQ10 for antioxidant defense
- Vitamin D as it is eminent due to its anti-inflammatory nature
- Immune support for gut dysbiosis
Lifestyle Interventions That Support Healing
- Restorative sleep of around 7–9 hrs: melatonin is anti‑estrogenic
- Daily movement & strength training: improves insulin sensitivity and lowers estrogen
- Stress‑relief rituals: breath‑work, grounding, sunlight exposure, and journaling.
- Toxin‑light living: switch to glass or stainless steel, filter drinking water, choose fragrance‑free body care, and also avoid the products that contain SLS and parabens.
6. Final Thoughts - Your Pain Has a Reason
Endometriosis is not “just bad cramps”, rather it is a complex whole‑body disease that demands a whole‑body solution. When you decode your drivers, that are hormonal, immunal, gut-related, or environmental, and the body often knows how to recalibrate.
Ready to uncover the “why” behind your pain and reclaim vibrant health?
Book a Free Consult with iThrive Alive today and start a personalized roadmap to relief, fertility, and a life no longer ruled by the calendar.
Reference
Lamceva, J., Uljanovs, R. and Strumfa, I., 2023. The main theories on the pathogenesis of endometriosis. International journal of molecular sciences, 24(5), p.4254.
Guo, C. and Zhang, C., 2024. Role of the gut microbiota in the pathogenesis of endometriosis: a review. Frontiers in microbiology, 15, p.1363455.



.svg)
.svg)