Introduction
Most people assume hypertension begins when a doctor diagnoses it. In reality, high blood pressure often develops silently for years before crossing the clinical threshold. During this time, the body continuously compensates for vascular resistance, metabolic strain, and hormonal imbalance way long before numbers on a report appear abnormal.
This is why understanding high BP symptoms is not just helpful, it is physiologically essential.
Blood pressure is not simply a measurement of cardiovascular force. It reflects the interaction of multiple regulatory systems: kidney fluid balance, vascular tone, insulin signaling, nervous system activity, circadian rhythm, liver detoxification, and inflammatory load. When these systems lose coordination, the body gradually shifts toward persistent vascular tension.
The problem is that early hypertension symptoms rarely feel dramatic. They are subtle, systemic, and often misattributed to stress, fatigue, or lifestyle overload.
At iThrive ALIVE, hypertension is viewed not as a single disorder but as a network imbalance. Recognizing early warning signals allows intervention before structural vascular damage occurs.
To understand this progression more deeply, you may also explore our clinical case analysis “Case Breakdown: How Correcting Metabolic Dysfunction Improved Thyroid Function Without Escalating Medication”, which explains how systemic dysfunction alters hormonal regulation long before laboratory thresholds shift.
What Is Considered High BP and Why Symptoms Appear Late
Understanding the High BP Range
Blood pressure reflects how strongly blood pushes against arterial walls. When vascular resistance increases or fluid volume expands, pressure rises.
General clinical categories:
- Normal: below 120/80 mmHg
- Elevated: 120 - 129 / <80
- Stage 1 hypertension: 130 - 139 / 80 - 89
- Stage 2 hypertension: ≥140 / ≥90
However, symptoms rarely correlate directly with numbers. Many individuals experience physiological strain even before entering the diagnostic range.
This happens because the body initially compensates by increasing heart rate, altering kidney sodium handling, tightening blood vessels, and elevating stress hormones. These adaptive responses produce subtle sensations that people rarely associate with blood pressure.
Why Hypertension Becomes a “Silent” Condition
Hypertension damages gradually. Arteries stiffen, endothelial signaling declines, and microcirculation becomes inefficient. These changes occur slowly, making early symptoms appear non-specific.
Instead of pain or acute dysfunction, individuals experience fatigue, tension, poor recovery, or metabolic disturbances.
In other words, symptoms are systemic, and not localized.
10 Early High BP Symptoms Most People Ignore
These signs do not occur randomly. Each reflects a specific physiological mechanism linked to vascular resistance, nervous system activity, or metabolic stress.
1. Persistent Morning Head Pressure
Elevated nighttime blood pressure reduces normal nocturnal dipping. This causes vascular tension in cerebral circulation, producing heaviness on waking.
2. Unexplained Fatigue Despite Adequate Sleep
Reduced microvascular perfusion limits oxygen delivery to tissues. Cells produce energy inefficiently, leading to constant low-grade exhaustion.
3. Resting Heart Rate Above Normal
Sympathetic nervous system activation increases cardiac workload even at rest often driven by insulin resistance or stress hormones.
4. Dizziness on Standing
Blood vessel stiffness reduces the body’s ability to adjust pressure quickly during posture change.
5. Frequent Anxiety or Internal Restlessness
Elevated cortisol and adrenaline raise vascular tone while overstimulating the nervous system.
6. Blurred Vision or Eye Pressure
Microvascular strain affects retinal circulation, often an early indicator of vascular dysfunction.
7. Poor Exercise Recovery
Delayed heart rate normalization and fatigue after activity indicate reduced cardiovascular efficiency.
8. Chronic Neck or Shoulder Tightness
Muscle tension often reflects sympathetic overactivation and restricted circulation.
9. Sleep Disturbances
Night-time cortisol elevation interferes with deep sleep phases required for cardiovascular repair.
10. Fluid Retention or Facial Puffiness
Kidney sodium retention increases blood volume, subtly raising pressure.
These symptoms often appear in combination and not in isolation.

What Causes These Symptoms? The Systems Biology View
Most explanations of hypertension focus on sodium intake or stress alone. In reality, early symptoms arise from network dysfunction.
Several major drivers interact:
Metabolic Dysfunction
Insulin resistance increases renal sodium retention, activates the sympathetic nervous system, and promotes vascular inflammation. This relationship is explored in depth in our educational article “Insulin Resistance: The Silent Phase Before Type 2 Diabetes.”
Endothelial Dysfunction
Healthy blood vessels produce nitric oxide to relax and dilate. Oxidative stress reduces this capacity, increasing vascular resistance.
Nervous System Overactivation
Chronic stress keeps the body in a constant alert state, preventing normal vascular relaxation.
Circadian Rhythm Disruption
Late-night light exposure, irregular sleep, and poor recovery impair hormonal regulation of blood pressure.
Micronutrient Deficiency
Magnesium, potassium, and vitamin D are essential for vascular flexibility and fluid balance.
When these systems drift out of synchrony, early symptoms begin to appear, way long before sustained hypertension develops.

What To Do If BP Is High or Symptoms Appear
The typical response to elevated blood pressure is medication adjustment. While sometimes necessary, symptom progression usually reflects deeper physiological imbalance.
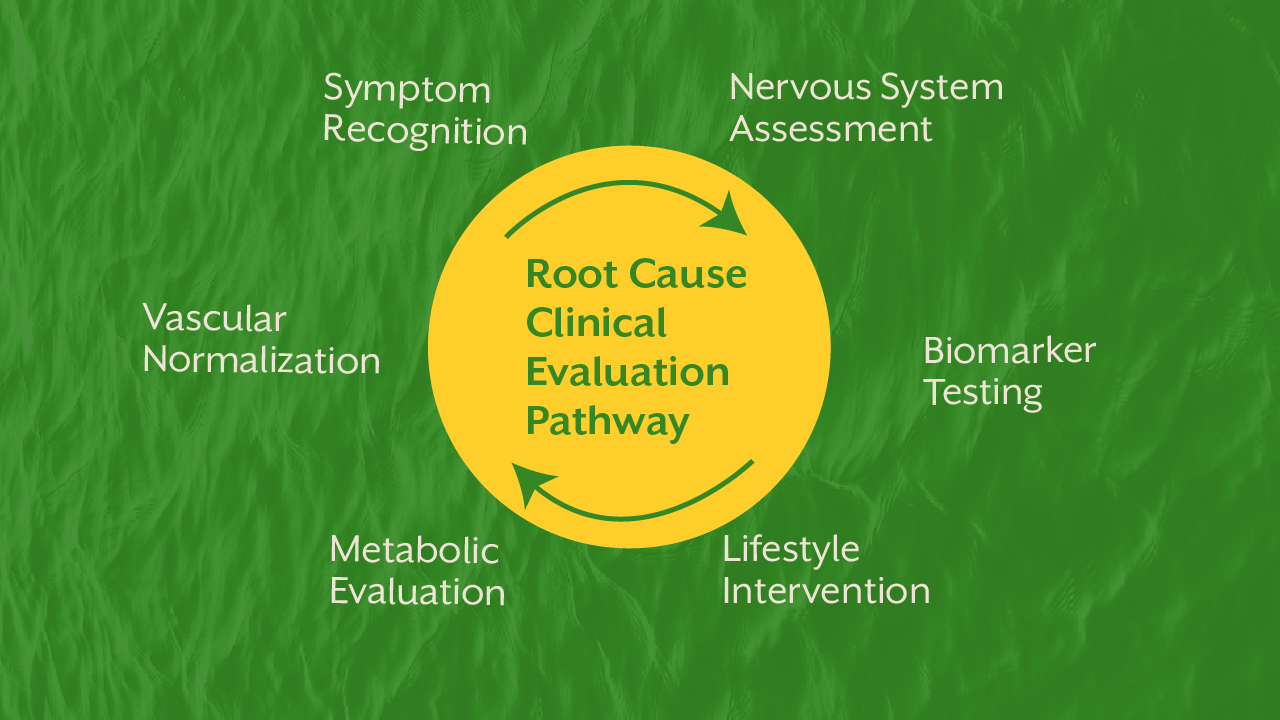
A clinically meaningful response includes evaluating:
- Metabolic markers
- Liver function and oxidative stress
- Micronutrient status
- Gut health
- Sleep physiology
- Stress regulation
- Environmental exposure
This is why iThrive ALIVE emphasizes comprehensive physiological assessment rather than isolated BP management.
If symptoms are persistent, the most effective approach is to book a root cause analysis to identify regulatory breakdowns before structural vascular damage develops.
Why Early Detection Changes Outcomes
Blood vessels adapt continuously. When elevated pressure persists, structural remodeling begins like arterial thickening, stiffness, and reduced elasticity.
Once these changes occur, reversal becomes more difficult.
Early symptom recognition allows intervention during the functional stage, when regulatory systems can still be recalibrated.
Lifestyle restructuring, targeted micronutrient support, circadian alignment, and metabolic correction can restore vascular balance before irreversible damage develops.
Key Takeaway
High blood pressure rarely begins with a diagnosis, it begins with subtle physiological signals that reflect systemic imbalance. Early high BP symptoms such as fatigue, tension, poor sleep, and morning head pressure are not random discomforts; they are regulatory warnings from the cardiovascular network. Hypertension is fundamentally a systems disorder involving metabolism, nervous system activity, hormonal rhythms, and vascular health. Recognizing early signs allows intervention before structural damage occurs. A root-cause clinical model that evaluates metabolic health, micronutrient status, sleep physiology, and inflammatory load provides the most effective strategy for long-term cardiovascular stability.


.svg)
.svg)















.webp)