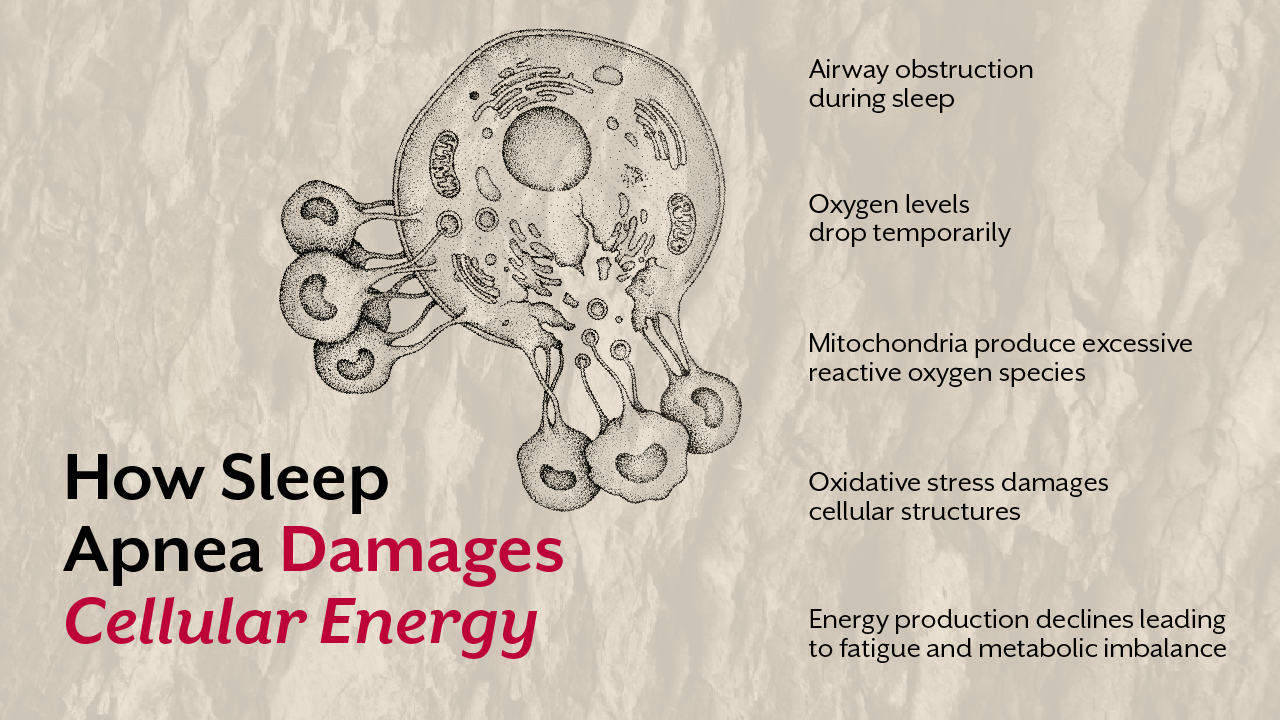
Introduction
For many people, high blood pressure appears suddenly, and mostly a routine check shows elevated numbers, medication begins, and monitoring becomes a lifelong habit. But very few are told why their blood pressure increased in the first place.
Hypertension rarely develops overnight. It emerges gradually from metabolic strain, vascular stiffness, hormonal imbalance, immune activity, and nervous system dysregulation. These processes evolve silently for years before crossing diagnostic thresholds.
This is why simply identifying a high reading does not explain what causes high BP. Blood pressure is not an isolated variable, rather it is a physiological output reflecting how multiple regulatory systems are functioning together.
Understanding the real causes of hypertension requires looking deeper than numbers. It requires asking what is driving vascular tension, fluid retention, stress signalling, and metabolic load inside the body.
At iThrive Alive, blood pressure is never viewed as a single disease entity. It is understood as a systems response, the one that reflects the cumulative effects of lifestyle, environment, inflammation, nutrition, and physiology.
Before discussing management, we must first understand the true drivers.
1. The Difference Between Essential and Root-Driven Hypertension
Most people diagnosed with high blood pressure are told they have essential hypertension, meaning no identifiable medical cause.
However, “no identifiable cause” often reflects limitations in testing, not absence of dysfunction.
Blood pressure regulation depends on:
- vascular elasticity
- kidney filtration efficiency
- hormonal signalling
- nervous system tone
- metabolic energy production
- inflammatory activity
When any of these systems lose balance, pressure rises as a compensatory response.
This is why many individuals with “essential hypertension” actually have measurable upstream disturbances like metabolic, inflammatory, hormonal, or neurological that are rarely evaluated.
Understanding what causes high BP therefore requires shifting from diagnosis-based thinking to mechanism-based thinking.
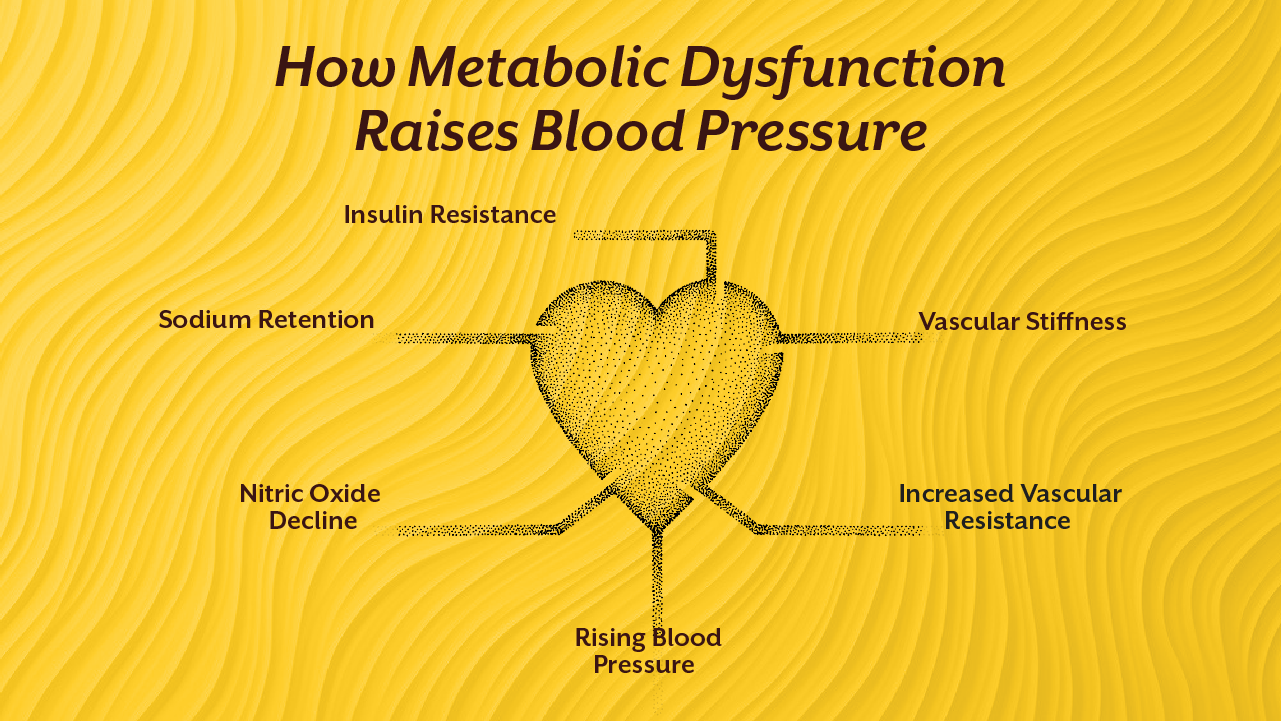
2. Metabolic Dysfunction and Insulin Resistance
One of the most powerful yet overlooked reasons for high BP is metabolic dysfunction.
When insulin signalling becomes inefficient, several vascular changes occur:
- sodium retention increases
- arterial walls thicken
- sympathetic nervous system activity rises
- nitric oxide availability declines
These changes collectively increase vascular resistance.
This explains why hypertension frequently coexists with abdominal fat accumulation, fatigue, and fluctuating energy levels.
Readers who want to explore how modern lifestyle patterns influence metabolic strain may connect this mechanism with insights discussed in the blog titled “Is Your Desk Job Making You Insulin Resistant?”
Sedentary physiology changes vascular behaviour long before blood sugar becomes abnormal.
3. Chronic Inflammation and Immune Activation
Low-grade inflammation alters blood vessel structure and function.
Inflammatory mediators:
- damage endothelial lining
- reduce arterial flexibility
- increase oxidative stress
- promote fluid retention
Over time, vessels lose their ability to expand and relax appropriately.
This makes inflammation one of the most consistent hidden causes of hypertension.
Environmental exposure plays a major role here, something explored further in the blog “The Truth About Toxins: What’s Hiding in Your Daily Routine.” Chemical exposure, food additives, and air pollutants all influence vascular inflammation.
4. Nervous System Overactivation
Blood pressure is tightly controlled by the autonomic nervous system.
When stress signalling becomes persistent, the sympathetic branch remains activated. This causes:
- constant vascular constriction
- elevated heart output
- reduced recovery capacity
- altered kidney filtration
This pattern is common in individuals experiencing chronic psychological stress, poor sleep, or irregular daily rhythms.
Over time, the body adapts to sustained tension as the new baseline.

5. Hormonal Imbalance and Fluid Regulation
Hormones regulate how much fluid the body retains and how vessels respond to pressure.
Disruptions in cortisol rhythm, thyroid signalling, and aldosterone balance can significantly alter blood pressure.
When hormonal signalling becomes dysregulated, the body may:
- retain excess sodium
- constrict vessels excessively
- alter vascular responsiveness
This makes hormonal evaluation essential when investigating reasons for high BP.
6. Kidney Function and Fluid Balance
Kidneys regulate long-term blood pressure by controlling sodium and water balance.
Even subtle changes in kidney filtration efficiency can elevate pressure gradually.
Importantly, dysfunction may exist before laboratory markers become abnormal. Reduced filtration efficiency can silently increase vascular load for years.
This makes kidney-vascular interaction one of the central mechanisms behind hypertension.
7. Vascular Aging and Structural Stiffness
Arteries are designed to expand with each heartbeat.
When structural proteins degrade due to oxidative stress or glycation, vessels stiffen.
Stiffer vessels:
- absorb less pressure
- transmit higher force downstream
- increase systolic readings
This explains why hypertension often appears with advancing age, but biological aging is heavily influenced by lifestyle patterns.
8. Nutrient Deficiency and Vascular Function
Blood vessels depend on micronutrients to maintain elasticity and signalling efficiency.
Insufficient intake of minerals involved in vascular relaxation, mitochondrial energy production, and antioxidant defence can impair blood pressure regulation.
Nutritional status therefore plays a direct role in determining vascular tone and reactivity.
9. Sleep Disruption and Circadian Misalignment
Blood pressure follows a daily rhythm. It naturally drops during deep sleep and rises during waking hours.
When sleep quality declines or circadian timing becomes irregular, this restorative dip disappears.
Persistent elevation then becomes the new physiological baseline.
10. Gut Barrier Dysfunction and Systemic Load
Emerging research shows that intestinal permeability influences systemic inflammation and vascular signalling.
When gut barrier integrity weakens, inflammatory molecules enter circulation and influence vascular tone.
This gut-vascular connection is an important modern contributor to hypertension.
11. Environmental Chemical Burden
Endocrine-disrupting compounds interfere with hormonal regulation and vascular signalling.
Chronic exposure alters metabolic efficiency, inflammatory activity, and fluid regulation simultaneously.
This creates long-term pressure elevation through multiple pathways.
12. Genetic Predisposition - But Only Part of the Story
Genetics influence susceptibility, but expression depends heavily on lifestyle and environment.
Genes set the threshold. Physiology determines whether that threshold is crossed.
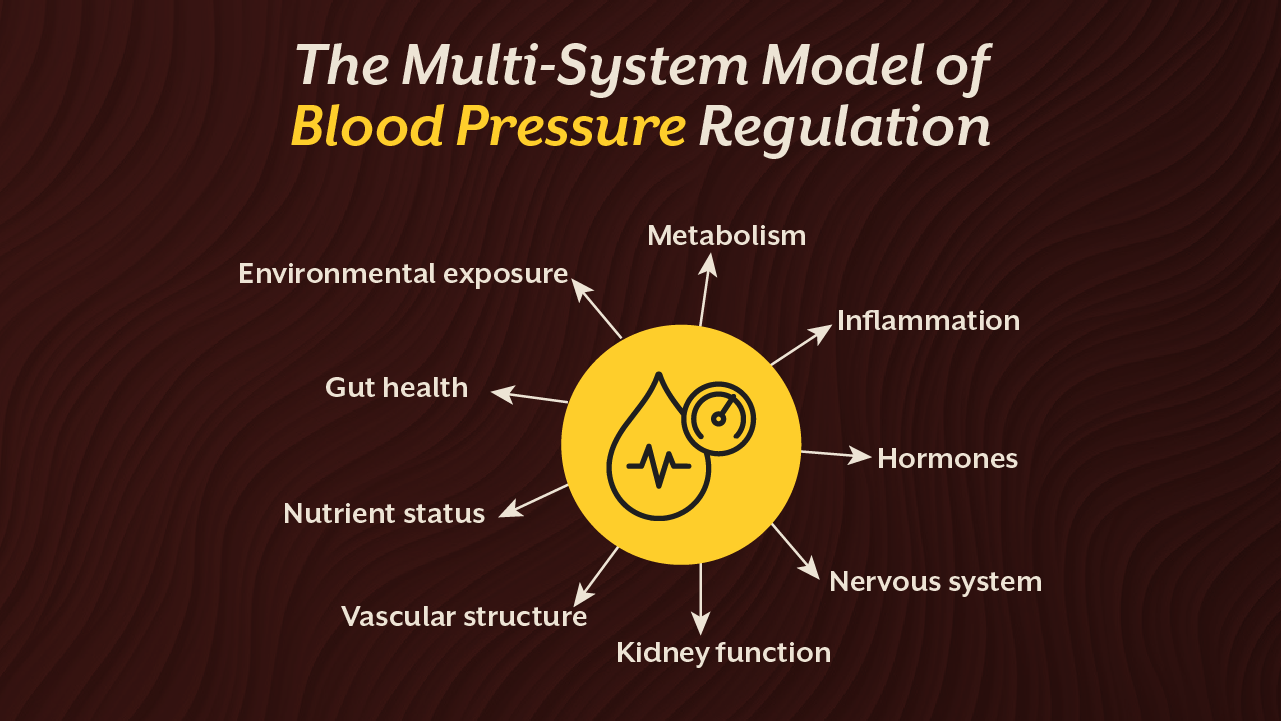
A Systems Approach to Understanding What Causes High BP
Blood pressure is not generated by one organ or one behaviour. It emerges from a network of regulatory systems working together or failing to.
This is why identifying reasons for high BP requires examining metabolism, inflammation, hormones, nervous system activity, vascular structure, nutrient status, and environmental exposure simultaneously.
At iThrive Alive, evaluation is not limited to measuring blood pressure. The clinical model focuses on identifying upstream drivers that alter vascular regulation.
Through lifestyle interventions, smart eating strategies, and targeted supplementation, the goal is not just to manage readings but to restore physiological balance.
Individuals seeking deeper insight can book a root cause analysis or book a consult to evaluate the mechanisms influencing their blood pressure patterns.
Key Takeaway
High blood pressure is rarely a random event. It is the visible expression of invisible physiological strain. Metabolic dysfunction, inflammation, nervous system overactivation, hormonal imbalance, vascular aging, nutrient deficiency, sleep disruption, environmental exposure, and gut dysfunction all interact to shape vascular pressure. Understanding what causes high BP requires shifting from symptom management to systems understanding. When upstream drivers are identified and addressed, blood pressure becomes not just controllable, but explainable.



.svg)
.svg)














.webp)