Introduction
Many people assume fatigue simply means being tired after a long day. Rest, sleep, or a short break usually restores energy. But individuals living with chronic fatigue syndrome describe something very different. Their exhaustion does not disappear with sleep. Even simple activities such as walking, working, or concentrating can feel overwhelming.
Chronic fatigue syndrome symptoms often extend far beyond tiredness. People report persistent brain fog, headaches, muscle pain, reduced stamina, and difficulty recovering after physical or mental exertion. The experience can feel confusing because medical tests frequently appear normal, leaving patients without clear explanations for their symptoms.
Increasingly, research suggests that the answer may lie deeper inside the body at the cellular level. The body’s ability to produce energy efficiently depends heavily on mitochondria, the microscopic structures inside cells that generate ATP. ATP is the biological fuel that powers muscle contraction, nerve signaling, immune regulation, and cognitive function.
When mitochondrial efficiency declines, the body struggles to maintain energy across multiple systems. What initially appears as fatigue may actually reflect widespread disruption in cellular energy production.
Understanding this biological layer changes how chronic fatigue syndrome is viewed. Instead of being dismissed as unexplained exhaustion, it becomes a condition that may involve metabolic stress, immune dysfunction, and impaired mitochondrial activity.
Understanding Chronic Fatigue Syndrome Beyond Tiredness
Chronic fatigue syndrome is sometimes referred to as chronic fatigue immune dysfunction syndrome. The name itself reflects the complexity of the condition. It does not involve only fatigue but also disturbances in immune activity, neurological signaling, and metabolic function.
Individuals experiencing chronic fatigue syndrome symptoms frequently report a cluster of overlapping issues. These may include persistent exhaustion, poor exercise tolerance, headaches, sleep disturbances, and cognitive slowing often described as brain fog.
Unlike normal fatigue, the exhaustion seen in chronic fatigue syndrome often worsens after exertion. Even mild activity can trigger prolonged fatigue lasting hours or days. This phenomenon is often referred to as post exertional malaise.
Scientists believe this pattern may occur because the body cannot produce or distribute energy efficiently during stress. Instead of generating adequate ATP, cells begin to operate under metabolic strain. As a result, the nervous system, muscles, and immune system may all struggle to maintain normal function.
This explains why chronic fatigue syndrome symptoms appear so widespread. The condition is not limited to one organ but reflects a deeper problem in cellular energy regulation.
The Mitochondrial Connection To Chronic Fatigue
Mitochondria are often described as the energy engines of the cell. Their primary role is to convert nutrients and oxygen into ATP through a process known as oxidative phosphorylation.
This energy is essential for nearly every biological activity including muscle movement, nerve communication, immune defense, and brain function. When mitochondrial efficiency declines, the body begins to experience a subtle but widespread energy shortage.
In individuals with chronic fatigue syndrome, researchers have observed signs of impaired mitochondrial function. Cells appear less capable of generating adequate ATP during periods of stress. As a result, the body becomes more vulnerable to fatigue, inflammation, and poor recovery after exertion.
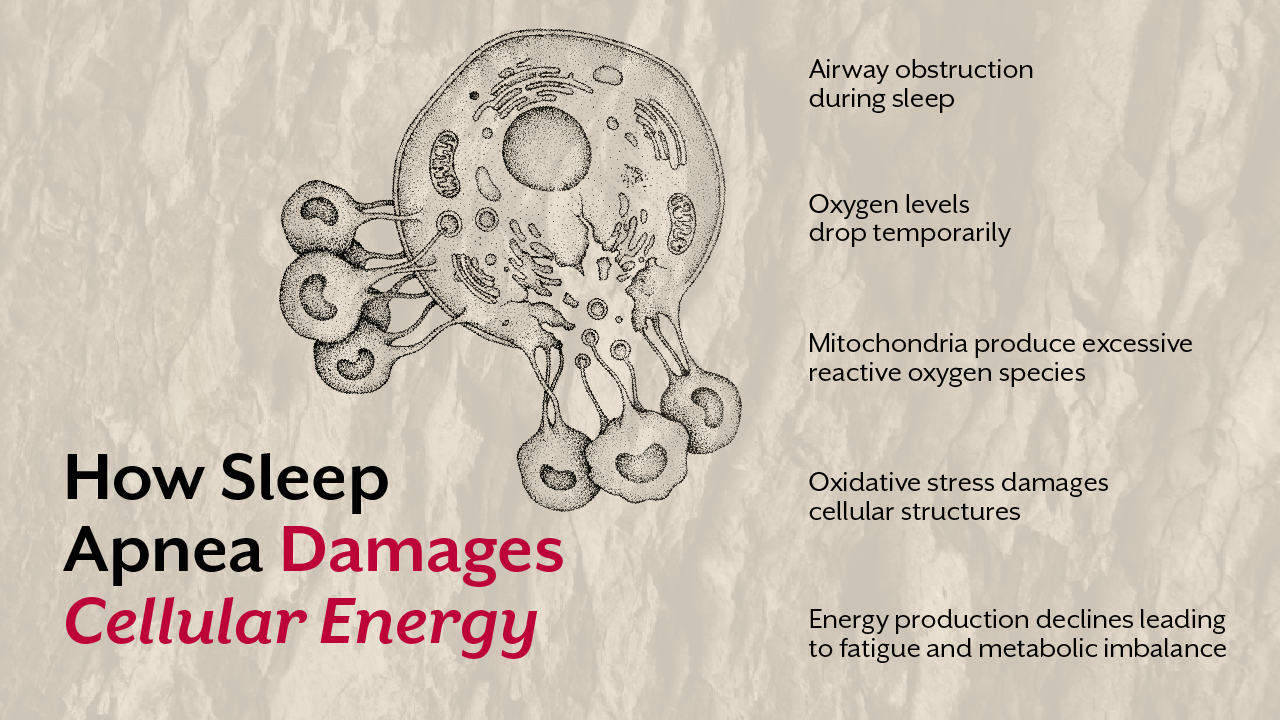
Another important factor is oxidative stress. When mitochondria struggle to produce energy efficiently, they can generate excessive reactive oxygen species. These unstable molecules damage cellular structures and further reduce mitochondrial efficiency.
Over time, this creates a cycle in which reduced energy production leads to more oxidative stress, and oxidative stress further weakens mitochondrial performance.
This cycle may explain why fatigue in chronic fatigue syndrome feels so persistent and difficult to resolve.

Immune Dysfunction and Post Viral Fatigue
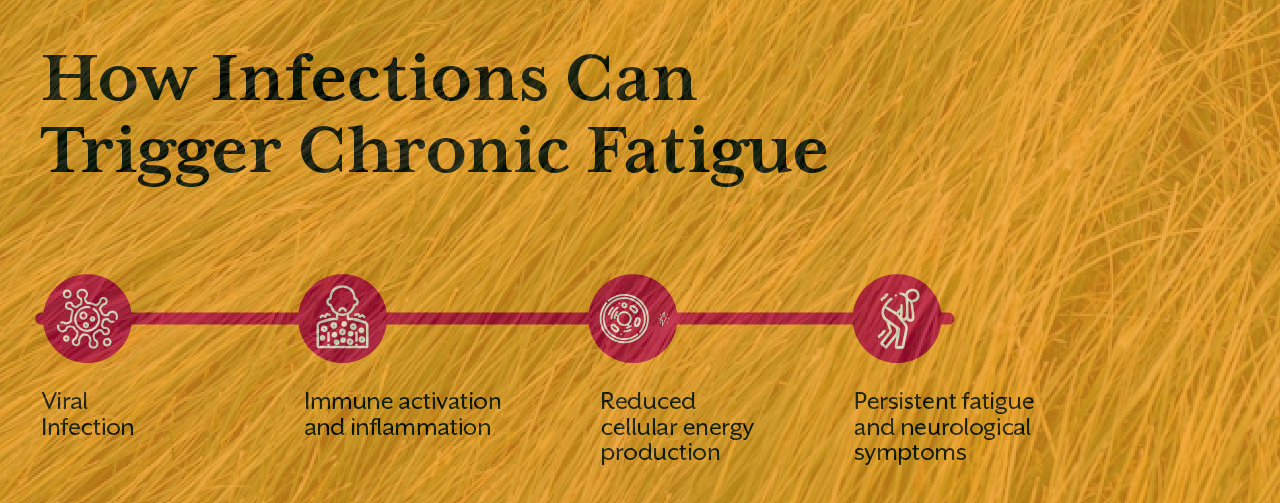
Many individuals report that their symptoms began after an infection. Viral illnesses such as influenza, Epstein Barr virus, or other infections have been linked to post viral chronic fatigue syndrome.
During an infection, the immune system activates a powerful inflammatory response to eliminate pathogens. While this response is necessary for protection, prolonged immune activation can place significant stress on cellular metabolism.
Inflammatory molecules released by immune cells can interfere with mitochondrial energy production. Instead of efficiently generating ATP, mitochondria begin to operate less effectively.
At the same time, inflammation may alter the way the brain regulates fatigue signals. The nervous system becomes more sensitive to physical stress, making even small tasks feel exhausting.
This interaction between immune activity and mitochondrial metabolism may explain why chronic fatigue immune dysfunction syndrome often develops after infections.
Why Brain Fog And Headaches Often Occur
One of the most frustrating symptoms reported by individuals with chronic fatigue syndrome is brain fog. People describe difficulty concentrating, memory lapses, slower thinking, and mental exhaustion.
The brain consumes an enormous amount of cellular energy. Although it represents only a small percentage of body weight, it requires a constant supply of ATP to maintain neural signaling and cognitive performance.
When mitochondrial energy production declines, the brain may struggle to maintain normal function. This can lead to cognitive fatigue and difficulty processing information.
Chronic fatigue syndrome headaches may also arise from metabolic stress in the nervous system. Reduced energy availability combined with inflammation can alter pain signaling pathways, making headaches more frequent or persistent.
These neurological symptoms highlight how deeply energy metabolism influences cognitive health.
The Metabolic Environment Behind Energy Loss
Energy production inside the body depends on more than just mitochondria. It is influenced by the broader metabolic environment including nutrition, inflammation, hormonal balance, and gut health.
Nutrient deficiencies can reduce the availability of key cofactors required for mitochondrial function. Nutrients such as magnesium, B vitamins, and CoQ10 are involved in multiple stages of ATP production.
Chronic inflammation also disrupts cellular metabolism. Inflammatory signaling diverts energy away from normal physiological functions and toward immune activation.
Gut health plays a role as well. Disturbances in the gut microbiome can influence immune regulation and nutrient absorption, both of which impact cellular energy pathways.
For individuals living with chronic fatigue syndrome, these overlapping factors can gradually reduce the body’s ability to sustain healthy energy production.
A Systems Based Approach To Energy Restoration
Because chronic fatigue syndrome involves multiple biological systems, addressing it often requires a broader approach than simply treating fatigue symptoms.
At iThrive Alive, the focus is on identifying the underlying drivers that may be affecting cellular energy systems. This may include evaluating nutrient status, metabolic markers, gut health, and lifestyle patterns that influence mitochondrial efficiency.
Lifestyle interventions play an important role. Regular movement can stimulate mitochondrial growth and improve metabolic flexibility. Sleep quality supports cellular repair processes that occur overnight.
Nutrition also provides essential substrates for mitochondrial function. Whole foods rich in micronutrients support enzymatic pathways involved in energy production.
Targeted supplementation may help replenish nutrients that support mitochondrial respiration and antioxidant defense.
For individuals experiencing persistent fatigue, exploring deeper metabolic patterns may offer valuable insights. Many people begin this process by choosing to book a root cause analysis through the iThrive Alive program to understand what may be influencing their symptoms.

When Fatigue Becomes A Signal From The Body
Persistent fatigue can feel frustrating and isolating. Many individuals struggle for years without understanding why their energy levels remain low.
However, chronic fatigue syndrome symptoms may serve as an important signal from the body. When cellular energy production begins to decline, the body often reduces activity levels as a protective mechanism.
Recognizing this signal allows individuals to explore deeper biological factors that may be influencing their health. Addressing mitochondrial function, immune balance, and metabolic resilience can help restore the body’s natural energy systems over time.
For individuals looking for personalized guidance, iThrive Alive also offers the option to book a consult to explore strategies that may support energy recovery.
Key Takeaway
Chronic fatigue syndrome is far more complex than simple tiredness. The condition reflects a deeper disruption in the body’s energy producing systems. Mitochondria play a central role in this process because every biological function depends on adequate cellular energy. When mitochondrial efficiency declines due to inflammation, infections, nutrient deficiencies, or metabolic stress, the body begins to struggle with energy distribution across multiple systems. This can lead to persistent fatigue, brain fog, headaches, and poor recovery after exertion. Understanding chronic fatigue syndrome through the lens of cellular energy metabolism offers a more comprehensive way to approach the condition. By supporting mitochondrial health through nutrition, lifestyle adjustments, and targeted metabolic strategies, it may be possible to gradually restore the body’s capacity for sustainable energy.



.svg)
.svg)















.webp)