What Is Fibromyalgia?
Fibromyalgia is a chronic condition that causes widespread musculoskeletal pain, along with fatigue, sleep problems, memory issues, and mood disturbances. Unlike regular muscle pain that comes from injury or overexertion, fibromyalgia pain is persistent and often described as a deep ache, tenderness, or burning sensation that doesn’t go away even with rest.
Scientists believe it is linked to nervous system dysfunction, where the brain and spinal cord amplify pain signals, making everyday sensations feel painful.
Could It Be Fibromyalgia? Recognizing the Signs
Many people mistake fibromyalgia for “just stress” or “overwork.” But if you are dealing with:
- Constant widespread pain (on both sides of the body, above and below the waist)
- Extreme fatigue, even after sleeping
- Morning stiffness and muscle tightness
- Sleep disturbances (light, unrefreshing sleep or insomnia)
- Brain fog (difficulty concentrating, memory lapses)
- Heightened sensitivity to touch, temperature, lights, or sounds
- Mood changes, anxiety, or depression,
Then it may be more than simple muscle pain. These are hallmark symptoms of fibromyalgia and should not be ignored.
Why Conventional Treatment Doesn’t Always Work

When someone is diagnosed with fibromyalgia, doctors usually recommend a mix of medications to control symptoms. These include:
- Painkillers and NSAIDs: They reduce pain signals temporarily but don’t fix what’s causing the pain. Since fibromyalgia pain comes from an overactive nervous system, not tissue damage, these drugs often fall short.
- Antidepressants or anti-seizure drugs: These are prescribed to calm nerve activity and improve mood. While they may provide short-term relief, they don’t address why the nervous system is misfiring in the first place.
- Sleeping pills: Poor sleep is a hallmark of fibromyalgia, but relying on sedatives doesn’t improve sleep quality. It just forces the body into a sleep-like state, often leaving patients groggy the next day.
The Limitations
- Symptom Management, Not Root Healing
Medications are designed to mask pain, boost mood, or induce sleep, but fibromyalgia is a multi-system condition involving the brain, immune system, gut, hormones, and stress response. Without addressing these imbalances, the condition persists. - Side Effects add to the Burden
Long-term use of these drugs can cause problems like weight gain, digestive discomfort, hormonal changes, fatigue, or even dependency, adding new challenges on top of existing pain. - Decreasing Effectiveness Over Time
Many patients report that after months or years on medication, the benefits wear off. The nervous system adapts, leaving them still in pain but now with added side effects. - Emotional Toll
Because these treatments don’t lead to true healing, patients often feel unheard, misunderstood, or told their condition is “in their head,” which adds mental stress and worsens flare-ups.
Functional Approaches to Ease Fibromyalgia Naturally

Functional nutrition views fibromyalgia not just as a pain disorder but as a system-wide imbalance involving the nervous system, gut, immune function, hormones, and mitochondria (the energy factories of your cells). Instead of suppressing symptoms, functional approaches dig into root causes and support healing at multiple levels.
Relying solely on medications often creates a cycle of temporary relief and long-term side effects, leaving the underlying imbalances untouched. Natural healing, on the other hand, focuses on restoring balance within the body, supporting better sleep, reducing inflammation, calming the nervous system and strengthening resilience. By working with the body instead of against it, natural approaches not only ease pain but also empower lasting health and energy.
Here are the key areas:
1. Nutrition & Gut Health
Food is medicine, depending on what you eat. Research shows people with fibromyalgia often have gut imbalances, leaky gut, and food sensitivities, all of which increase inflammation and pain.
- Anti-inflammatory diet: Focus on fresh vegetables, fruits, and clean protein sources.
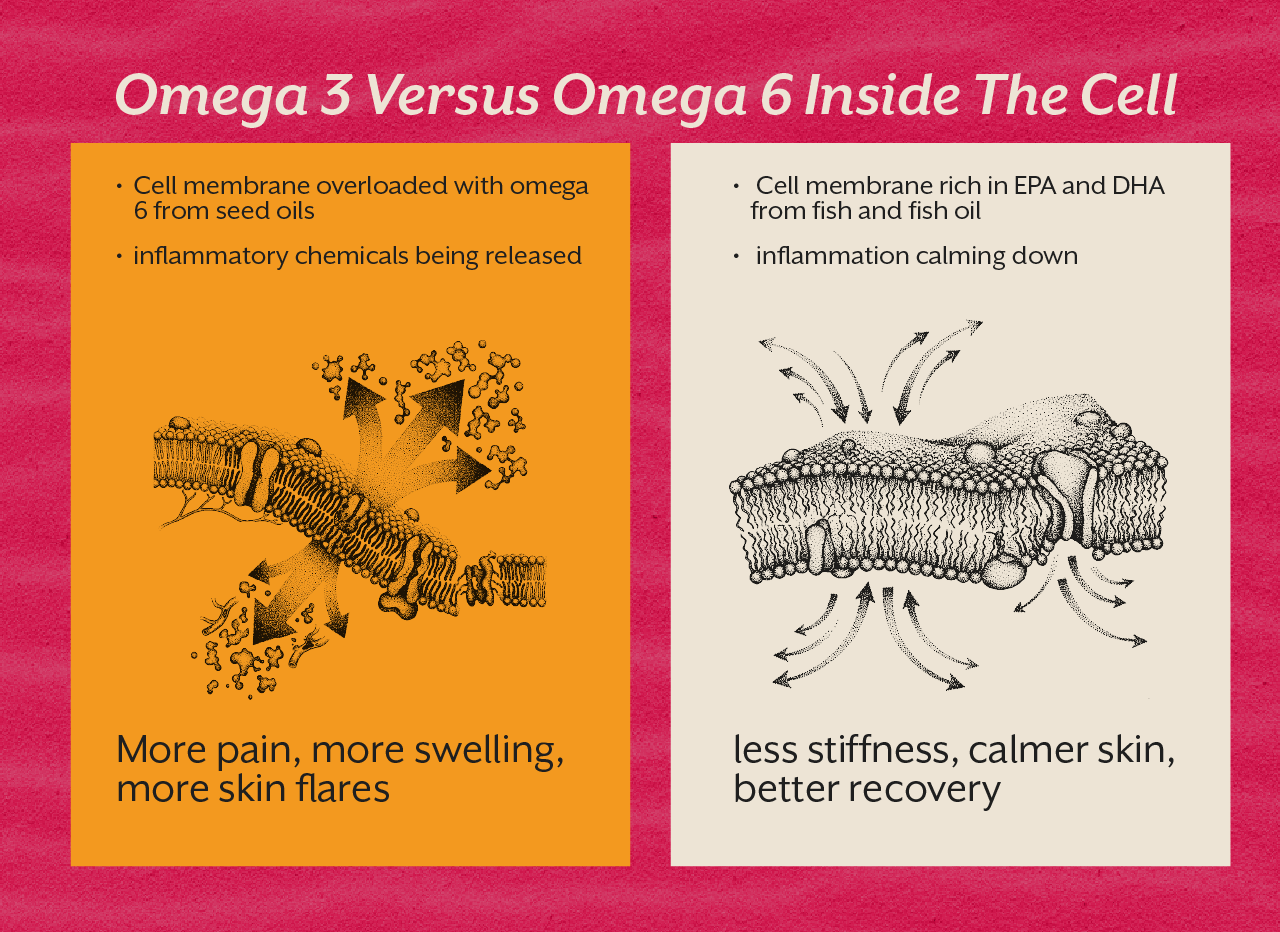
- Omega-3 fatty acids (from fish) help calm inflammation and nerve pain.
- Eliminate triggers: Gluten, dairy, processed sugar, and refined foods often worsen symptoms.
- Gut repair: Probiotic-rich foods and prebiotic fibers help restore healthy gut bacteria. You can also supplement with probiotics with prebiotics to get best results.
By healing the gut, you reduce the inflammatory signals that trigger pain and fatigue.
2. Restorative Sleep & Stress Management
Fibromyalgia is often called a “stress-related disorder” because the nervous system stays stuck in fight-or-flight mode. Poor sleep and chronic stress make the condition worse.
- Sleep hygiene: Consistent bedtime, dark room, no late-night screens.
- Natural aids: Magnesium, chamomile tea, lavender oil to relax before bed.
- Stress reduction: Yoga, tai chi, meditation, or even short breathing exercises calm the overactive nervous system.
- Trauma release practices: Techniques like somatic therapy or guided relaxation can reset nervous system patterns.
Restful sleep and reduced stress lower cortisol levels and help reset pain sensitivity.
3. Gentle Movement & Physical Therapy
Exercise may seem impossible when you’re in pain, but gentle, regular movement can actually rewire the nervous system and reduce stiffness.
- Low-impact exercises like walking, swimming, cycling, or tai chi improve circulation.
- Stretching & mobility work reduces muscle tightness without overexertion.
- Strength training (gradual) can help stabilize joints and support muscle function.
The key is consistency, not intensity, small, regular movement helps retrain the body to handle physical stress better.
4. Targeted Supplementation

Certain nutrients directly support energy production, muscle relaxation and nervous system balance.
- Magnesium: Relaxes muscles, improves sleep, and reduces cramps.
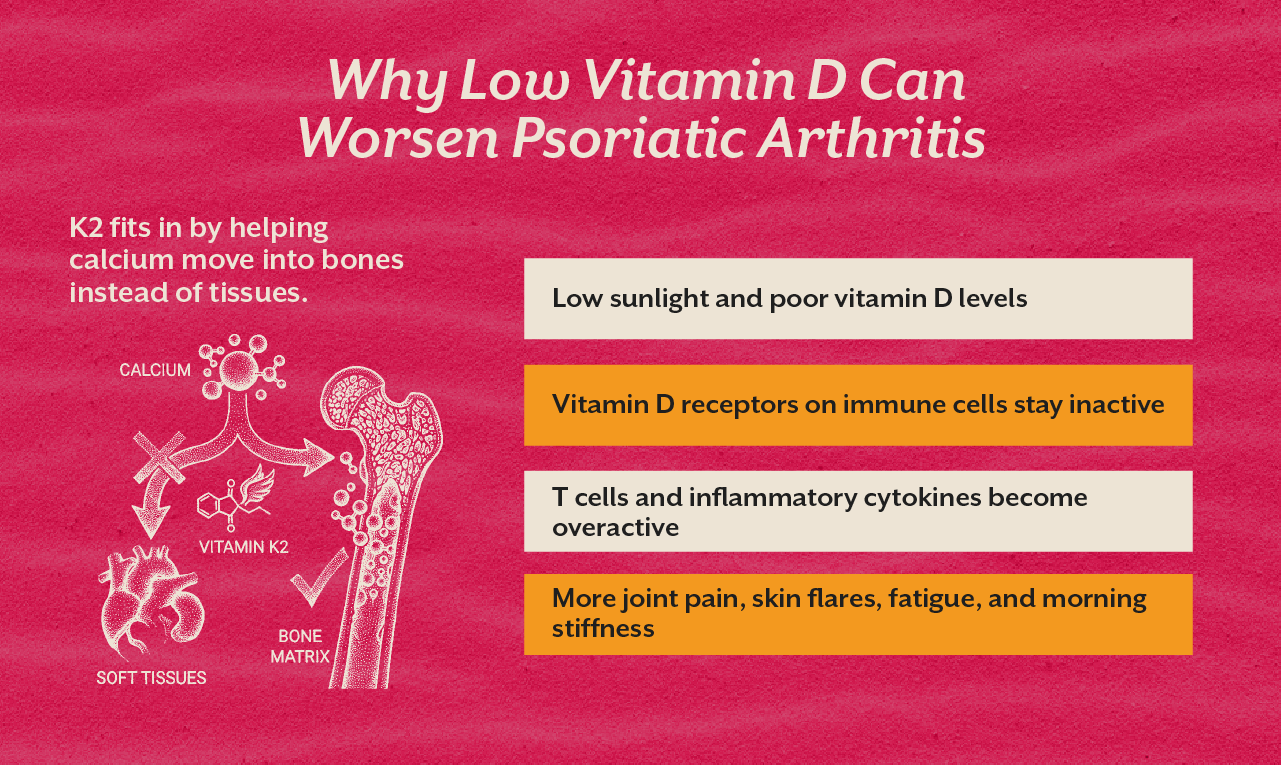
- Vitamin D3 + K2: Strengthens bones, modulates immunity, and helps regulate pain perception.
- B-Complex Vitamins: Essential for energy production in mitochondria; deficiency worsens fatigue.
- CoQ10: Supports mitochondrial function, reducing brain fog and chronic fatigue.
- Omega-3s: Anti-inflammatory, helpful for joint pain and brain health.
5. Mind-Body & Alternative Therapies
Pain perception is deeply linked to how the brain processes signals. These therapies calm the nervous system and retrain pain pathways.
- Acupuncture: Stimulates energy flow, reduces pain sensitivity.
- Massage therapy: Improves blood flow, reduces stiffness, and lowers cortisol.
- Chiropractic care or physiotherapy: Restores mobility and corrects posture imbalances.
- Mindfulness practices: Reduce “central sensitization,” where the brain amplifies pain signals.
6. Detoxification
Fibromyalgia patients often show higher levels of toxins and oxidative stress, which worsen inflammation and pain. Supporting the body’s detox pathways can help.
- Stay hydrated: Water flushes toxins and supports kidney function.
- Fiber-rich foods: Help eliminate toxins via digestion.
- Binders (under guidance) like activated charcoal or chlorella, can reduce toxic load.
- Sauna therapy & sweating: Aid detox through skin.
Lowering toxin burden reduces inflammation and relieves pressure on the immune system.
7. Emotional & Social Support
Chronic illness takes a mental toll. Emotional well-being directly affects pain sensitivity and healing.
- Therapy & support groups help reduce feelings of isolation.
- Cognitive-behavioral therapy (CBT) helps patients reframe pain and reduce anxiety.
- Community & connection improve resilience and reduce stress hormones.
How Can We Help

At iThrive, we go beyond just masking fibromyalgia symptoms; we help you uncover and heal the root causes. Through detailed blood work, personalized nutrition, targeted supplementation, and lifestyle support, we guide you step by step to reduce pain, restore energy, improve sleep, and bring your body back into balance naturally.



.svg)
.svg)