Introduction
A high blood pressure reading can feel alarming especially when it appears unexpectedly. One moment everything feels normal, and the next, a monitor displays numbers that seem far outside a safe range. For many individuals, the immediate question is simple but urgent: what to do if BP is high right now?
Yet this question has two very different answers.
One answer focuses on immediate stabilisation like what helps bring pressure down safely in the moment.
The other focuses on long-term regulation like why blood pressure rose and how to prevent it from happening again.
Most people receive guidance only for the first. But blood pressure is not a temporary fluctuation for most individuals. It reflects ongoing physiological strain. Without addressing underlying mechanisms, readings may repeatedly rise, even if temporarily controlled. Understanding how to control high BP therefore requires both acute response and long-term strategy. Blood pressure must be stabilised, but regulation must also be restored.
This blog explains both what to do immediately, and how to build a sustainable care plan for hypertension that supports vascular stability over time.
1. First - Understanding When High BP Is an Emergency
Not every elevated reading is dangerous, but some require urgent attention.
Blood pressure becomes concerning when:
- systolic pressure rises sharply above normal baseline
- symptoms appear (headache, dizziness, chest discomfort, breathlessness)
- readings remain elevated despite rest
Sudden spikes may reflect acute nervous system activation, fluid imbalance, or vascular constriction. However, when pressure rises extremely high or symptoms appear, medical evaluation becomes essential.
The first step in high BP treatment is therefore correct interpretation of severity. Numbers alone do not determine risk, in fact physiological response does.
2. What To Do Immediately If BP Is High
When blood pressure rises suddenly, the body is usually in a state of heightened vascular tension. Immediate actions should focus on reducing physiological stress and improving circulation.
2.1 Slow the Nervous System Response
The fastest way to reduce vascular constriction is to calm sympathetic activation. Slow breathing, especially extended exhalation patterns, reduces heart workload and relaxes arterial tension.
2.2 Sit Upright and Rest Quietly
Physical activity increases circulatory demand. Sitting upright supports optimal blood flow without adding strain.
2.3 Avoid Sudden Movement or Panic
Anxiety further activates stress signalling, amplifying pressure elevation. Calm observation is physiologically protective.
2.4 Recheck After Rest
Transient spikes often normalise once the body settles. Reassessment prevents unnecessary alarm.
These steps do not treat hypertension, they stabilize the moment. Long-term control requires deeper intervention.
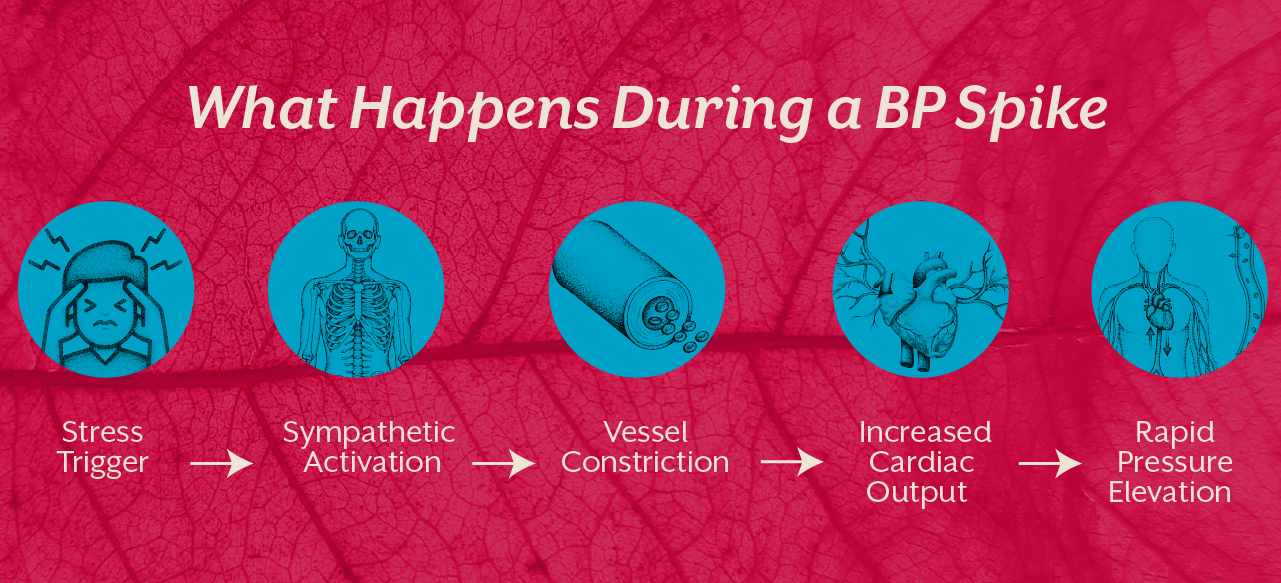
3. Why Blood Pressure Rises Repeatedly
Many individuals experience recurring elevations because the body remains in a state of chronic regulatory strain.
Blood pressure increases when:
- vessels remain constricted
- fluid balance shifts upward
- stress signalling stays active
- metabolic efficiency declines
- inflammation alters vascular structure
These processes operate continuously in modern lifestyles.
Readers who want deeper insight into how daily patterns influence metabolic stress may explore “Is Your Desk Job Making You Insulin Resistant?”, which explains how sedentary physiology alters vascular signalling long before disease appears.
Understanding what to do if BP is high therefore requires understanding why the regulatory system lost balance.
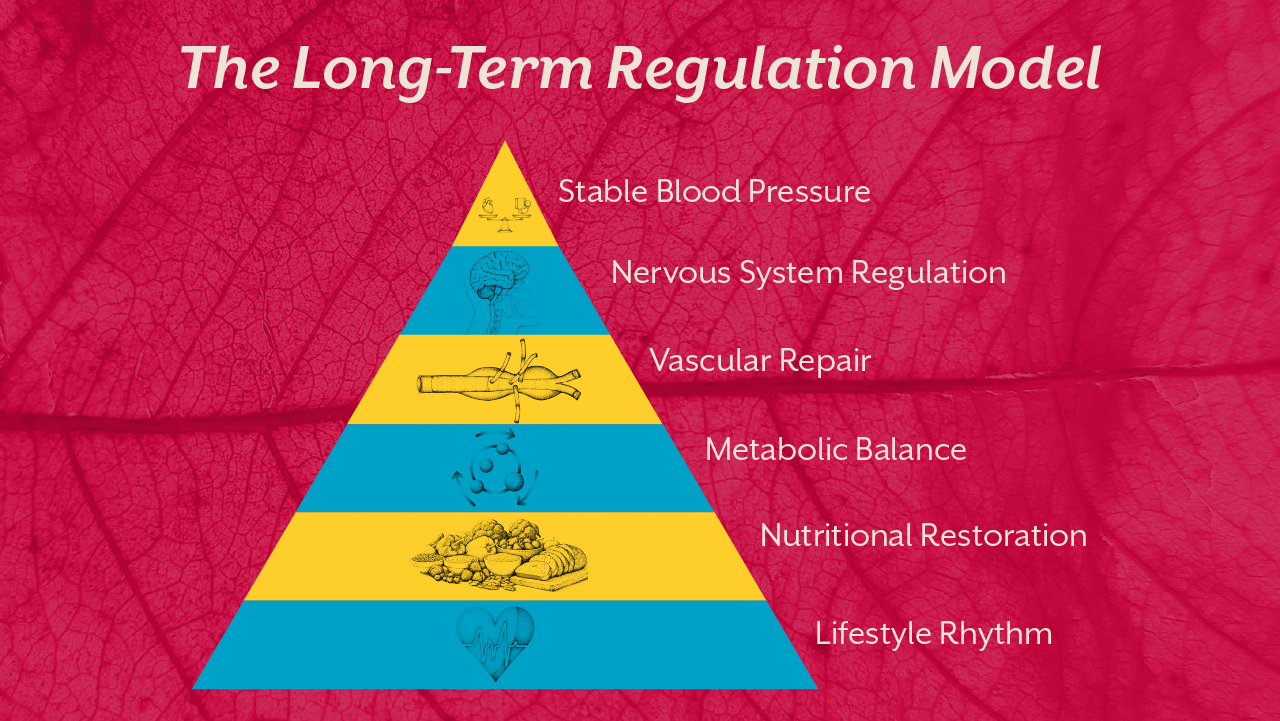
4. The Long - Term Care Plan for Hypertension
Short-term control lowers numbers. Long-term care restores regulation.
A sustainable care plan for hypertension must address the physiological systems that determine vascular pressure.
4.1 Restoring Vascular Flexibility
Healthy arteries expand with each heartbeat. Loss of elasticity increases resistance and pressure load.
Improving vascular responsiveness depends on:
- nitric oxide availability
- oxidative stress reduction
- structural protein integrity
Lifestyle rhythm, nutrition, and metabolic stability all influence arterial behaviour.
4.2 Stabilising Metabolic Energy Regulation
Energy metabolism determines how efficiently tissues utilise oxygen and nutrients. When cellular energy production becomes inefficient, vascular signalling becomes erratic.
Metabolic restoration improves vascular responsiveness, fluid balance, and nervous system stability simultaneously.
4.3 Rebalancing Stress Physiology
Chronic stress changes baseline vascular tone. The nervous system gradually adapts to constant alertness, maintaining mild constriction even at rest.
Restoring parasympathetic recovery phases is essential for blood pressure regulation.
5. Nutrition as a Regulatory Tool, Not Just Restriction
Dietary advice often focuses on reducing salt intake alone. But vascular regulation depends on far more than sodium.
Nutritional patterns influence:
- endothelial function
- inflammatory load
- mitochondrial efficiency
- hormonal signalling
- fluid balance
A strategic nutritional approach therefore supports pressure regulation rather than merely restricting intake.
This includes restoring micronutrient sufficiency, supporting vascular repair, and stabilising metabolic rhythms.
6. Movement - Mechanical and Metabolic Reset
Regular movement improves vascular responsiveness through mechanical stimulation of blood vessel lining.
Movement also improves:
- glucose utilisation
- autonomic balance
- circulation efficiency
- inflammatory regulation
Importantly, consistent moderate movement stabilises baseline pressure more effectively than occasional intense exertion.
7. Monitoring Patterns Instead of Isolated Numbers
Blood pressure fluctuates throughout the day. Single readings provide limited insight.
Meaningful evaluation requires observing patterns:
- morning vs evening variation
- response to stress
- recovery after rest
- post-meal changes
Pattern analysis reveals regulatory efficiency.

8. A Systems-Based Model of Blood Pressure Care
Managing hypertension effectively requires integrating multiple physiological domains rather than targeting numbers alone.
This is the clinical philosophy used at iThrive Alive, where blood pressure is evaluated as an output of metabolic, vascular, inflammatory, hormonal, and nervous system function combined.
Lifestyle interventions, structured nutrition, and targeted supplementation are used to restore regulation rather than simply suppress symptoms.
Individuals seeking structured evaluation can book a root cause analysis to identify mechanisms influencing their blood pressure patterns or book a consult to understand personalised care planning.
Key Takeaway
Knowing what to do if BP is high requires two levels of response. Immediate actions help stabilize vascular tension and prevent acute risk, but lasting control depends on restoring the physiological systems that regulate pressure continuously. Blood pressure reflects vascular flexibility, metabolic efficiency, nervous system balance, fluid regulation, and inflammatory load working together. A meaningful care plan for hypertension must therefore extend beyond temporary reduction and focus on long-term regulatory restoration. When underlying mechanisms are stabilised, blood pressure becomes not just manageable, but predictable and sustainable.



.svg)
.svg)















.webp)