



.svg)




.svg)
High blood pressure rarely announces itself loudly. It does not always cause pain. It does not always disturb sleep. It does not always make you feel unwell. And yet, it silently reshapes arteries, strains the heart, burdens the kidneys, and increases long term cardiovascular risk.
When someone is diagnosed, the immediate pathway usually begins with hypertension medications. This is often necessary. For many individuals, medication lowers numbers quickly and reduces immediate cardiovascular danger. But the larger question remains unanswered for most patients: is lowering the number the same as solving the problem?
At iThrive Alive, we approach high bp treatment differently. We recognise that blood pressure is not just a number on a monitor. It is an output of vascular tone, metabolic signalling, kidney function, nervous system balance, inflammatory load, micronutrient status, and lifestyle stressors.
This blog explores both pathways. Medicines. Root cause care. And what truly works best when long term health is the goal.
Blood pressure is the force exerted by circulating blood on arterial walls. When it remains chronically elevated, arteries gradually lose elasticity. The heart pumps against higher resistance. Microvascular damage accumulates.
However, hypertension is rarely a single organ disorder. It is usually a systems imbalance.
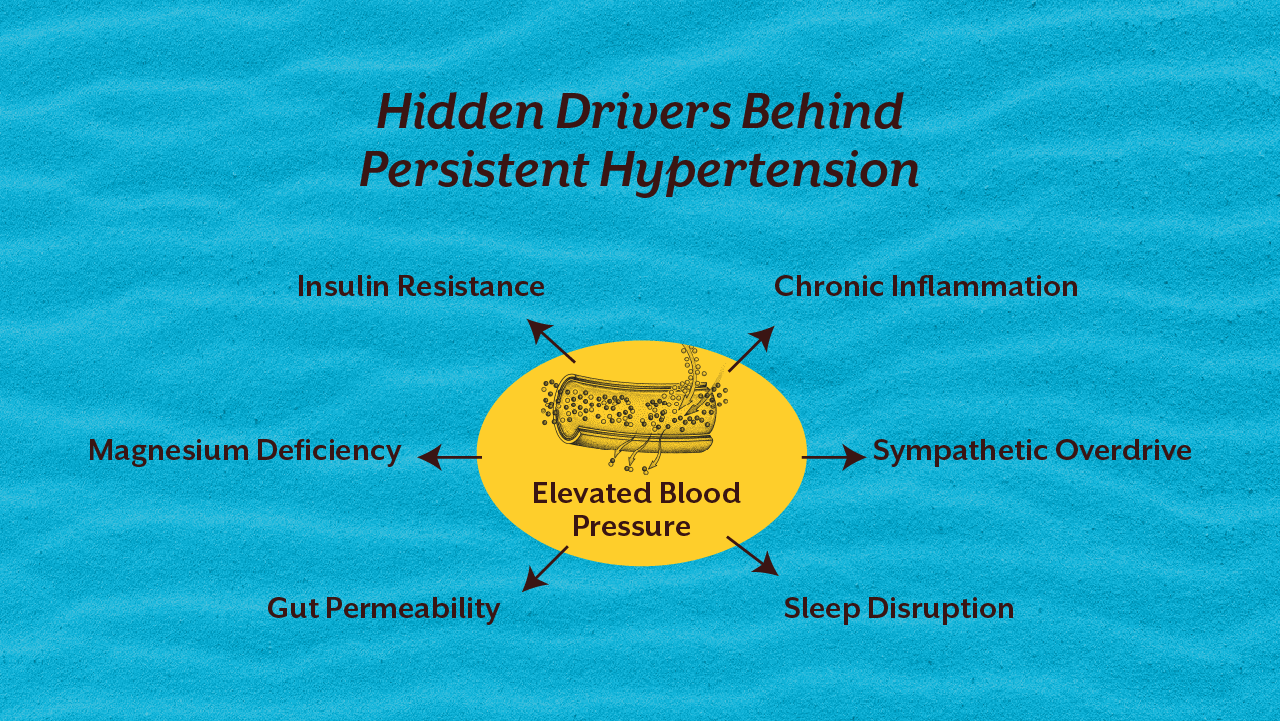
In clinical practice, we see several common drivers behind rising blood pressure levels. Insulin resistance stiffens arteries and increases sodium retention. Chronic stress activates the sympathetic nervous system, elevating vascular tone. Low magnesium impairs vascular relaxation. Inflammatory signalling alters endothelial function. Sleep deprivation raises cortisol and disrupts circadian rhythm.
The body does not randomly increase pressure. It responds to internal signals.
If you have read our earlier blog on insulin dysfunction, especially “Insulin Resistance: The Silent Phase Before Type 2 Diabetes”, you will recognise a pattern. Metabolic dysregulation rarely stays confined to one diagnosis. Blood sugar instability and high blood pressure often travel together.
For many patients, hypertension medications are lifesaving. In moderate to severe hypertension, delaying pharmacological treatment can increase cardiovascular risk. Medicines reduce stroke risk, lower cardiac workload, and protect kidneys in high risk individuals.
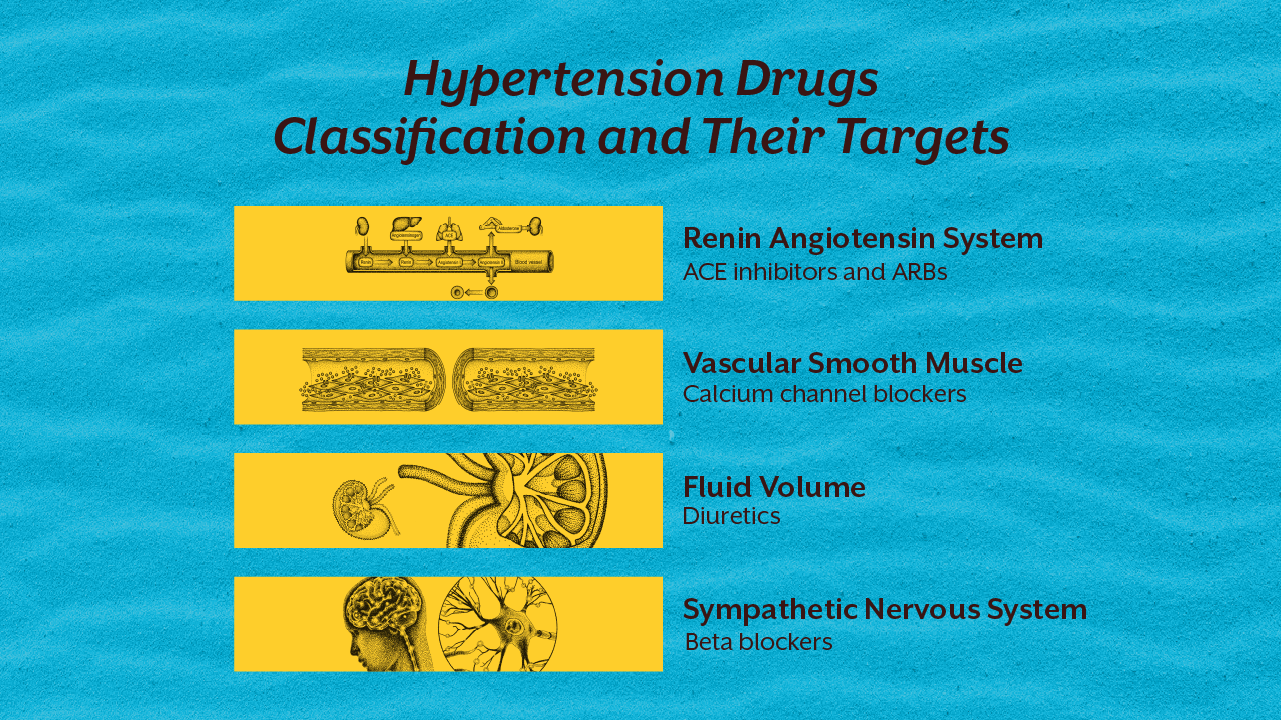
The hypertension drugs classification generally includes ACE inhibitors, ARBs, calcium channel blockers, beta blockers, diuretics, and others. Each class acts on a specific physiological pathway.
ACE inhibitors and ARBs influence the renin angiotensin aldosterone system. Calcium channel blockers reduce vascular contraction. Diuretics help eliminate excess sodium and fluid. Beta blockers reduce heart rate and sympathetic stimulation.
From a short term perspective, this approach works. Numbers drop. Risk decreases.
However, medication does not always address why the renin system was activated in the first place. It does not correct magnesium deficiency. It does not reverse insulin resistance. It does not repair endothelial inflammation. It does not regulate chronic sympathetic overdrive caused by stress.
This does not mean medicines are wrong. It means they are one layer of care.
At iThrive Alive, we often see individuals who have been on hypertension medications for years, yet metabolic dysfunction continues underneath. In some cases, dosages gradually increase because the underlying terrain was never addressed.
Medication is controlled. It is not always correct.
The root cause approach asks a deeper question. What physiological forces are pushing pressure upward?
At iThrive Alive, high bp treatment often begins with metabolic mapping. We evaluate fasting insulin, inflammatory markers, micronutrient levels, gut health, stress load, sleep quality, and dietary patterns.
Insulin resistance is one of the most under recognised contributors to hypertension. Elevated insulin promotes sodium retention and vascular smooth muscle growth. This increases resistance within arterial walls. Addressing insulin sensitivity through structured nutrition and strength training often shifts blood pressure more sustainably than sodium restriction alone.
Magnesium deficiency is another overlooked driver. Magnesium supports vascular relaxation and endothelial stability. Modern diets are frequently inadequate in magnesium rich foods. Correcting this can improve vascular tone naturally.
Chronic stress activates sympathetic dominance. Persistent adrenaline and cortisol signalling tighten blood vessels and elevate heart rate. Nervous system regulation, breath work, circadian correction, and resistance training become therapeutic tools, not lifestyle suggestions.
Gut health also plays a role. Endotoxins from intestinal permeability can increase systemic inflammation and impair nitric oxide production, reducing vasodilation capacity.
This systems biology model resembles the approach discussed in our published blog “A Systems Approach to Thyroid Health”. The principle remains the same. The gland is not isolated. The number is not isolated. The body is a network.
Root cause high bp treatment does not reject medicines. It builds the terrain so that dependence may reduce over time under medical supervision.
The root cause approach asks a deeper question. What physiological forces are pushing pressure upward?
At iThrive Alive, high bp treatment often begins with metabolic mapping. We evaluate fasting insulin, inflammatory markers, micronutrient levels, gut health, stress load, sleep quality, and dietary patterns.
Insulin resistance is one of the most under recognised contributors to hypertension. Elevated insulin promotes sodium retention and vascular smooth muscle growth. This increases resistance within arterial walls. Addressing insulin sensitivity through structured nutrition and strength training often shifts blood pressure more sustainably than sodium restriction alone.
Magnesium deficiency is another overlooked driver. Magnesium supports vascular relaxation and endothelial stability. Modern diets are frequently inadequate in magnesium rich foods. Correcting this can improve vascular tone naturally.
Chronic stress activates sympathetic dominance. Persistent adrenaline and cortisol signalling tighten blood vessels and elevate heart rate. Nervous system regulation, breath work, circadian correction, and resistance training become therapeutic tools, not lifestyle suggestions.
Gut health also plays a role. Endotoxins from intestinal permeability can increase systemic inflammation and impair nitric oxide production, reducing vasodilation capacity.
This systems biology model resembles the approach discussed in our published blog “A Systems Approach to Thyroid Health”. The principle remains the same. The gland is not isolated. The number is not isolated. The body is a network.
Root cause high bp treatment does not reject medicines. It builds the terrain so that dependence may reduce over time under medical supervision.

High bp treatment is not a debate between medicines and lifestyle. It is a decision about depth. Hypertension medications lower risk and save lives when appropriately prescribed. But if metabolic dysfunction, nutrient deficiencies, chronic stress, gut derived inflammation, and insulin resistance remain active, the body continues to generate pressure internally. A systems driven approach, as practiced at iThrive Alive, recognises blood pressure as an output of whole body physiology. When the terrain improves, vascular health improves. Medicines may still have a role, but they are no longer the only pillar holding the structure.




.svg)
Most people are familiar with high blood pressure. It is widely discussed, frequently screened, and commonly treated. But a different and often more confusing pattern affects many individuals quietly like low BP and high pulse rate occurring together.
You may notice it when standing up suddenly and feeling lightheaded. Or when fatigue appears without explanation. Or when your heart seems to beat rapidly even though blood pressure readings appear low. For many people, this combination feels unsettling because it seems contradictory. If pressure is low, why is the heart working harder?
The body is not malfunctioning, it is compensating.
A low bp high pulse pattern is often the circulatory system’s attempt to maintain oxygen delivery when pressure is insufficient. When blood pressure drops, tissues may receive less perfusion. The heart responds by beating faster to preserve circulation. This is not a disease in itself, it is a regulatory response.
But when this pattern repeats frequently, it signals that the body is under persistent physiological strain.
Understanding what this combination means requires shifting perspective. Instead of viewing blood pressure and pulse separately, we must view them as coordinated outputs of a larger regulatory system involving circulation, nervous system signalling, fluid balance, and metabolic demand.
If you are experiencing low BP and high pulse rate repeatedly, your body is communicating something important. The goal is not to silence the signal, it is to understand why the signal exists.
Blood pressure and pulse rate work together to maintain tissue perfusion. When pressure falls, the body activates rapid compensatory mechanisms.
The nervous system detects reduced vascular tension and immediately increases heart rate. Faster heartbeats attempt to maintain blood flow despite lower pressure.
In short, when pressure drops, the heart speeds up to maintain oxygen delivery.
This explains why low bp and high pulse rate often appear together. The heart is not overreacting, rather it is protecting circulation.
However, when compensation becomes chronic, it indicates that the system is repeatedly forced to stabilize itself rather than operating smoothly.

Occasional drops in pressure are normal. But persistent low bp high pulse patterns suggest regulatory strain across one or more physiological systems.
This may involve fluid imbalance, nervous system dysregulation, metabolic stress, or vascular responsiveness.
Many people first notice symptoms during transitions like standing, exertion, emotional stress, or after meals. These are moments when the body must rapidly redistribute circulation. If regulation is impaired, compensation becomes exaggerated.
Circulatory instability often reflects broader metabolic patterns. For example, individuals who experience unstable energy regulation or insulin fluctuations may also experience vascular instability. Readers interested in metabolic regulation and systemic energy balance may find deeper context in “Is Your Desk Job Making You Insulin Resistant?”, which explains how sedentary physiology alters regulatory efficiency across multiple systems.
Similarly, environmental stressors affecting inflammatory load and vascular function are explored in “The Truth About Toxins: What’s Hiding in Your Daily Routine.” Circulation does not operate in isolation, it reflects total physiological burden.
Blood pressure regulation depends heavily on autonomic balance. The autonomic nervous system constantly adjusts heart rate and vascular tone in response to posture, temperature, stress, and metabolic demand.
When regulatory signalling becomes inconsistent, the body struggles to maintain steady circulation. Pressure may drop suddenly, and heart rate rises to compensate.
Chronic stress, poor recovery, and disrupted circadian rhythms can shift the nervous system toward persistent alertness. Over time, regulatory flexibility decreases.
The result is instability rather than disease but instability itself creates symptoms.

Blood pressure is strongly influenced by fluid balance. If circulating volume is reduced, pressure falls. The heart must beat faster to maintain perfusion.
Fluid imbalance may result from dehydration, electrolyte shifts, hormonal regulation changes, or impaired vascular tone.
Many individuals underestimate how strongly hydration, mineral balance, and vascular responsiveness interact. Circulation is not simply about heart function, in fact it is about volume distribution and vessel behaviour.
Circulation serves metabolism. When tissues require more oxygen or energy, cardiovascular output increases. If metabolic demand fluctuates unpredictably, circulatory regulation must adapt rapidly.
Energy instability, mitochondrial inefficiency, or inflammatory load can all influence vascular responsiveness.
This is why some individuals experience low bp high pulse alongside fatigue, poor recovery, or temperature sensitivity. These are not separate issues, they are interconnected outputs of systemic regulation.

Support begins with stabilisation, not suppression.
When symptoms arise, the goal is to help circulation re-equilibrate:
Long-term support requires strengthening regulatory capacity further improving vascular responsiveness, metabolic stability, and nervous system recovery.
Managing low bp and high pulse rate effectively requires moving beyond symptom management toward regulatory restoration.
This is the clinical model used at iThrive Alive, where circulatory patterns are evaluated within a broader physiological framework. Rather than focusing only on numbers, assessment includes metabolic efficiency, inflammatory load, autonomic regulation, and vascular responsiveness.
Lifestyle interventions, structured nutrition, and targeted supplementation are used to stabilise systemic regulation rather than merely reacting to episodes.
If you feel your body is frequently compensating rather than stabilising, you may consider choosing to book a root cause analysis to understand the underlying drivers or book a consult to explore personalised support strategies.
Because when the body repeatedly compensates, it is asking for restoration, not temporary control.
Experiencing low BP and high pulse rate together is not random and not contradictory. It is a coordinated physiological response designed to maintain circulation when pressure falls. But when this pattern occurs repeatedly, it signals that the regulatory systems responsible for vascular tone, fluid balance, nervous system signalling, and metabolic stability are under strain. Supporting the body requires more than reacting to symptoms, it requires strengthening the systems that maintain steady circulation in the first place. When regulation improves, compensation becomes unnecessary, and stability returns naturally.




.svg)
A high blood pressure reading can feel alarming especially when it appears unexpectedly. One moment everything feels normal, and the next, a monitor displays numbers that seem far outside a safe range. For many individuals, the immediate question is simple but urgent: what to do if BP is high right now?
Yet this question has two very different answers.
One answer focuses on immediate stabilisation like what helps bring pressure down safely in the moment.
The other focuses on long-term regulation like why blood pressure rose and how to prevent it from happening again.
Most people receive guidance only for the first. But blood pressure is not a temporary fluctuation for most individuals. It reflects ongoing physiological strain. Without addressing underlying mechanisms, readings may repeatedly rise, even if temporarily controlled. Understanding how to control high BP therefore requires both acute response and long-term strategy. Blood pressure must be stabilised, but regulation must also be restored.
This blog explains both what to do immediately, and how to build a sustainable care plan for hypertension that supports vascular stability over time.
Not every elevated reading is dangerous, but some require urgent attention.
Sudden spikes may reflect acute nervous system activation, fluid imbalance, or vascular constriction. However, when pressure rises extremely high or symptoms appear, medical evaluation becomes essential.
The first step in high BP treatment is therefore correct interpretation of severity. Numbers alone do not determine risk, in fact physiological response does.
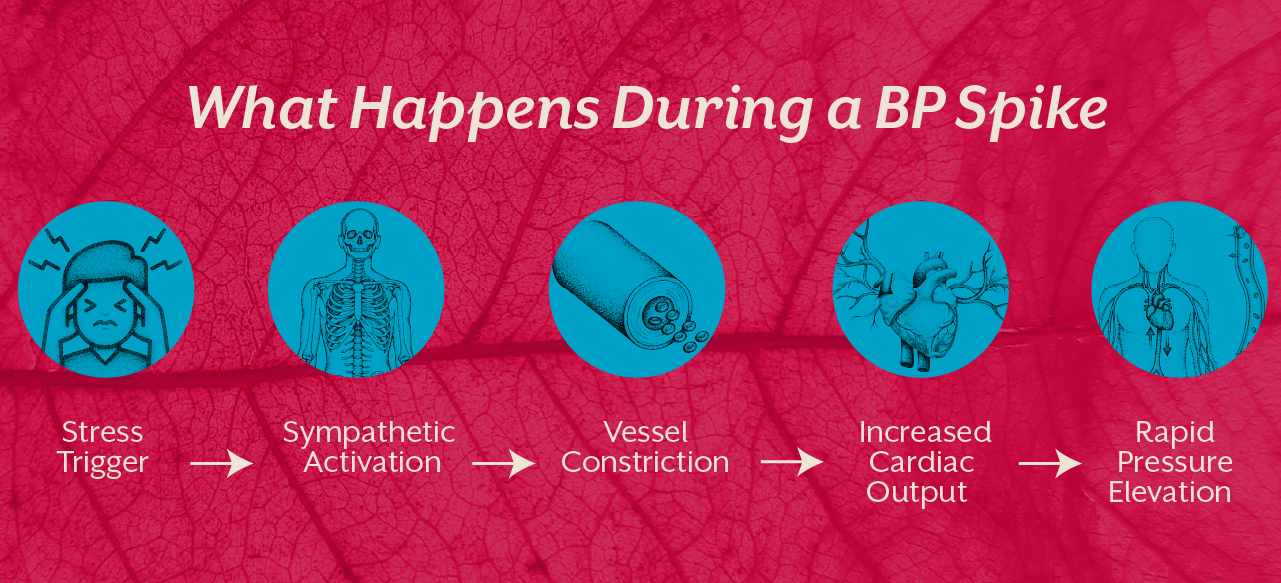
When blood pressure rises suddenly, the body is usually in a state of heightened vascular tension. Immediate actions should focus on reducing physiological stress and improving circulation.
The fastest way to reduce vascular constriction is to calm sympathetic activation. Slow breathing, especially extended exhalation patterns, reduces heart workload and relaxes arterial tension.
Physical activity increases circulatory demand. Sitting upright supports optimal blood flow without adding strain.
Anxiety further activates stress signalling, amplifying pressure elevation. Calm observation is physiologically protective.
Transient spikes often normalise once the body settles. Reassessment prevents unnecessary alarm.
These steps do not treat hypertension, they stabilize the moment. Long-term control requires deeper intervention.
Many individuals experience recurring elevations because the body remains in a state of chronic regulatory strain.
These processes operate continuously in modern lifestyles.
Readers who want deeper insight into how daily patterns influence metabolic stress may explore “Is Your Desk Job Making You Insulin Resistant?”, which explains how sedentary physiology alters vascular signalling long before disease appears.
Understanding what to do if BP is high therefore requires understanding why the regulatory system lost balance.
Short-term control lowers numbers. Long-term care restores regulation.
A sustainable care plan for hypertension must address the physiological systems that determine vascular pressure.
Healthy arteries expand with each heartbeat. Loss of elasticity increases resistance and pressure load.
Lifestyle rhythm, nutrition, and metabolic stability all influence arterial behaviour.
Energy metabolism determines how efficiently tissues utilise oxygen and nutrients. When cellular energy production becomes inefficient, vascular signalling becomes erratic.
Metabolic restoration improves vascular responsiveness, fluid balance, and nervous system stability simultaneously.
Chronic stress changes baseline vascular tone. The nervous system gradually adapts to constant alertness, maintaining mild constriction even at rest.
Restoring parasympathetic recovery phases is essential for blood pressure regulation.
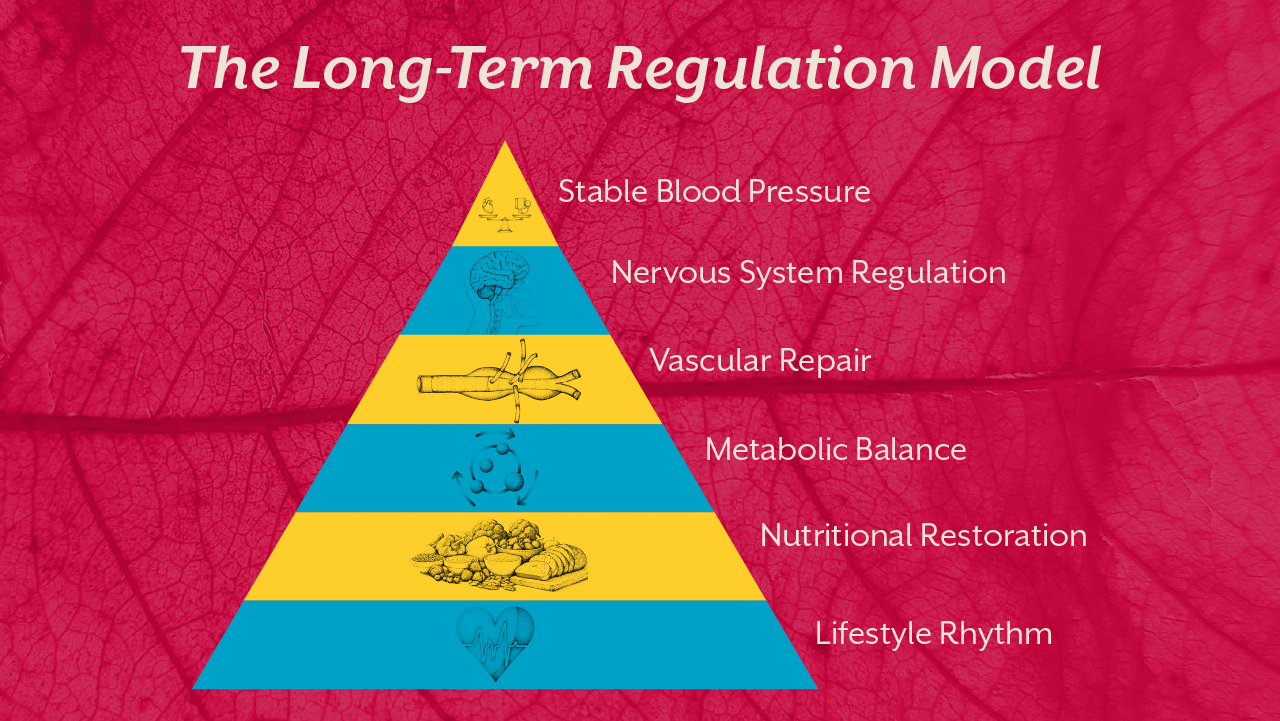
Dietary advice often focuses on reducing salt intake alone. But vascular regulation depends on far more than sodium.
A strategic nutritional approach therefore supports pressure regulation rather than merely restricting intake.
This includes restoring micronutrient sufficiency, supporting vascular repair, and stabilising metabolic rhythms.
Regular movement improves vascular responsiveness through mechanical stimulation of blood vessel lining.
Importantly, consistent moderate movement stabilises baseline pressure more effectively than occasional intense exertion.
Blood pressure fluctuates throughout the day. Single readings provide limited insight.
Pattern analysis reveals regulatory efficiency.

Managing hypertension effectively requires integrating multiple physiological domains rather than targeting numbers alone.
This is the clinical philosophy used at iThrive Alive, where blood pressure is evaluated as an output of metabolic, vascular, inflammatory, hormonal, and nervous system function combined.
Lifestyle interventions, structured nutrition, and targeted supplementation are used to restore regulation rather than simply suppress symptoms.
Individuals seeking structured evaluation can book a root cause analysis to identify mechanisms influencing their blood pressure patterns or book a consult to understand personalised care planning.
Knowing what to do if BP is high requires two levels of response. Immediate actions help stabilize vascular tension and prevent acute risk, but lasting control depends on restoring the physiological systems that regulate pressure continuously. Blood pressure reflects vascular flexibility, metabolic efficiency, nervous system balance, fluid regulation, and inflammatory load working together. A meaningful care plan for hypertension must therefore extend beyond temporary reduction and focus on long-term regulatory restoration. When underlying mechanisms are stabilised, blood pressure becomes not just manageable, but predictable and sustainable.




.svg)
For many people, high blood pressure appears suddenly, and mostly a routine check shows elevated numbers, medication begins, and monitoring becomes a lifelong habit. But very few are told why their blood pressure increased in the first place.
Hypertension rarely develops overnight. It emerges gradually from metabolic strain, vascular stiffness, hormonal imbalance, immune activity, and nervous system dysregulation. These processes evolve silently for years before crossing diagnostic thresholds.
This is why simply identifying a high reading does not explain what causes high BP. Blood pressure is not an isolated variable, rather it is a physiological output reflecting how multiple regulatory systems are functioning together.
Understanding the real causes of hypertension requires looking deeper than numbers. It requires asking what is driving vascular tension, fluid retention, stress signalling, and metabolic load inside the body.
At iThrive Alive, blood pressure is never viewed as a single disease entity. It is understood as a systems response, the one that reflects the cumulative effects of lifestyle, environment, inflammation, nutrition, and physiology.
Before discussing management, we must first understand the true drivers.
Most people diagnosed with high blood pressure are told they have essential hypertension, meaning no identifiable medical cause.
However, “no identifiable cause” often reflects limitations in testing, not absence of dysfunction.
When any of these systems lose balance, pressure rises as a compensatory response.
This is why many individuals with “essential hypertension” actually have measurable upstream disturbances like metabolic, inflammatory, hormonal, or neurological that are rarely evaluated.
Understanding what causes high BP therefore requires shifting from diagnosis-based thinking to mechanism-based thinking.
One of the most powerful yet overlooked reasons for high BP is metabolic dysfunction.
When insulin signalling becomes inefficient, several vascular changes occur:
These changes collectively increase vascular resistance.
This explains why hypertension frequently coexists with abdominal fat accumulation, fatigue, and fluctuating energy levels.
Readers who want to explore how modern lifestyle patterns influence metabolic strain may connect this mechanism with insights discussed in the blog titled “Is Your Desk Job Making You Insulin Resistant?”
Sedentary physiology changes vascular behaviour long before blood sugar becomes abnormal.
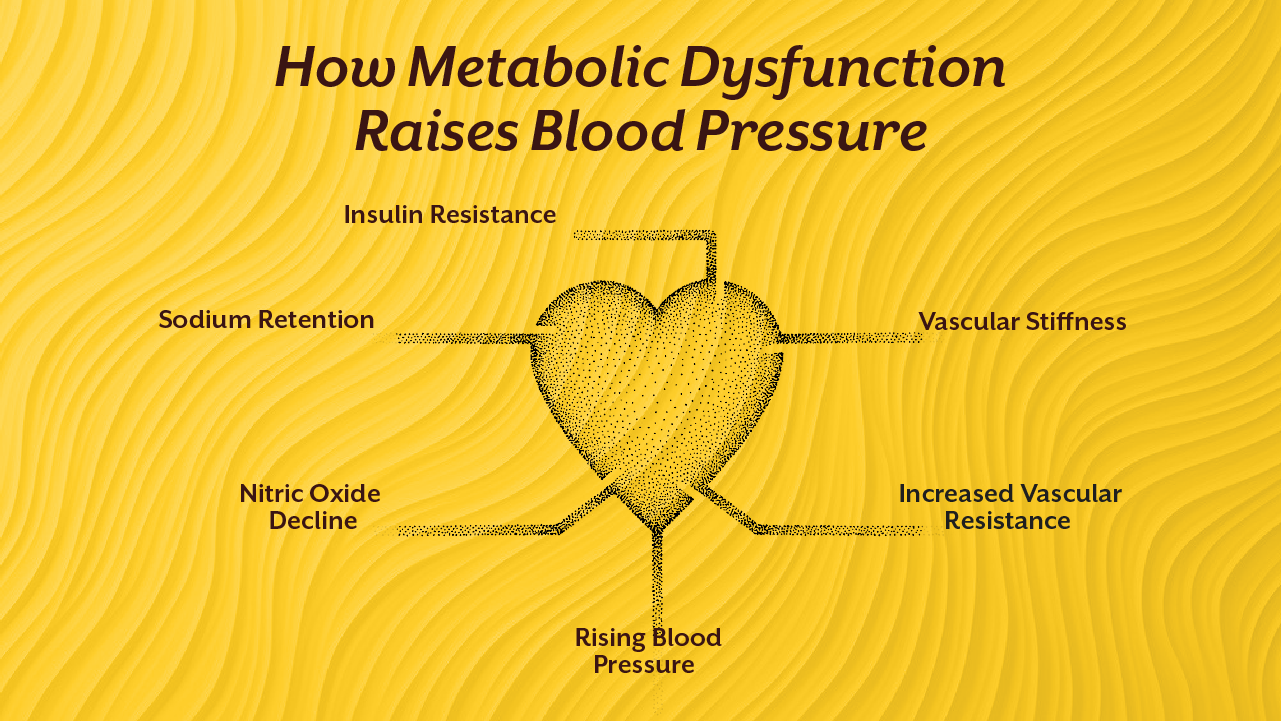
Low-grade inflammation alters blood vessel structure and function.
Over time, vessels lose their ability to expand and relax appropriately.
This makes inflammation one of the most consistent hidden causes of hypertension.
Environmental exposure plays a major role here, something explored further in the blog “The Truth About Toxins: What’s Hiding in Your Daily Routine.” Chemical exposure, food additives, and air pollutants all influence vascular inflammation.
Blood pressure is tightly controlled by the autonomic nervous system.
When stress signalling becomes persistent, the sympathetic branch remains activated. This causes:
This pattern is common in individuals experiencing chronic psychological stress, poor sleep, or irregular daily rhythms.
Over time, the body adapts to sustained tension as the new baseline.

Hormones regulate how much fluid the body retains and how vessels respond to pressure.
Disruptions in cortisol rhythm, thyroid signalling, and aldosterone balance can significantly alter blood pressure.
When hormonal signalling becomes dysregulated, the body may:
This makes hormonal evaluation essential when investigating reasons for high BP.
Kidneys regulate long-term blood pressure by controlling sodium and water balance.
Even subtle changes in kidney filtration efficiency can elevate pressure gradually.
Importantly, dysfunction may exist before laboratory markers become abnormal. Reduced filtration efficiency can silently increase vascular load for years.
This makes kidney-vascular interaction one of the central mechanisms behind hypertension.
Arteries are designed to expand with each heartbeat.
When structural proteins degrade due to oxidative stress or glycation, vessels stiffen.
This explains why hypertension often appears with advancing age, but biological aging is heavily influenced by lifestyle patterns.
Blood vessels depend on micronutrients to maintain elasticity and signalling efficiency.
Insufficient intake of minerals involved in vascular relaxation, mitochondrial energy production, and antioxidant defence can impair blood pressure regulation.
Nutritional status therefore plays a direct role in determining vascular tone and reactivity.
Blood pressure follows a daily rhythm. It naturally drops during deep sleep and rises during waking hours.
When sleep quality declines or circadian timing becomes irregular, this restorative dip disappears.
Persistent elevation then becomes the new physiological baseline.
Emerging research shows that intestinal permeability influences systemic inflammation and vascular signalling.
When gut barrier integrity weakens, inflammatory molecules enter circulation and influence vascular tone.
This gut-vascular connection is an important modern contributor to hypertension.
Endocrine-disrupting compounds interfere with hormonal regulation and vascular signalling.
Chronic exposure alters metabolic efficiency, inflammatory activity, and fluid regulation simultaneously.
This creates long-term pressure elevation through multiple pathways.
Genetics influence susceptibility, but expression depends heavily on lifestyle and environment.
Genes set the threshold. Physiology determines whether that threshold is crossed.
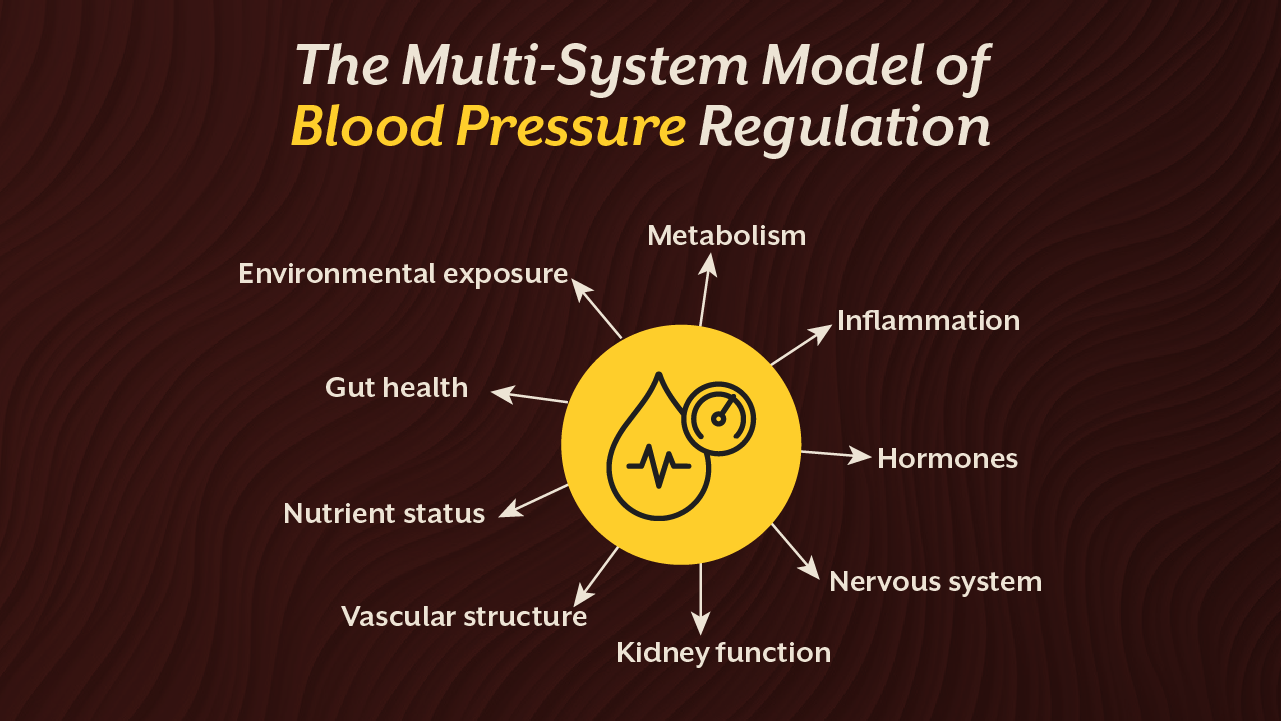
Blood pressure is not generated by one organ or one behaviour. It emerges from a network of regulatory systems working together or failing to.
This is why identifying reasons for high BP requires examining metabolism, inflammation, hormones, nervous system activity, vascular structure, nutrient status, and environmental exposure simultaneously.
At iThrive Alive, evaluation is not limited to measuring blood pressure. The clinical model focuses on identifying upstream drivers that alter vascular regulation.
Through lifestyle interventions, smart eating strategies, and targeted supplementation, the goal is not just to manage readings but to restore physiological balance.
Individuals seeking deeper insight can book a root cause analysis or book a consult to evaluate the mechanisms influencing their blood pressure patterns.
High blood pressure is rarely a random event. It is the visible expression of invisible physiological strain. Metabolic dysfunction, inflammation, nervous system overactivation, hormonal imbalance, vascular aging, nutrient deficiency, sleep disruption, environmental exposure, and gut dysfunction all interact to shape vascular pressure. Understanding what causes high BP requires shifting from symptom management to systems understanding. When upstream drivers are identified and addressed, blood pressure becomes not just controllable, but explainable.



.svg)
Most people assume hypertension begins when a doctor diagnoses it. In reality, high blood pressure often develops silently for years before crossing the clinical threshold. During this time, the body continuously compensates for vascular resistance, metabolic strain, and hormonal imbalance way long before numbers on a report appear abnormal.
This is why understanding high BP symptoms is not just helpful, it is physiologically essential.
Blood pressure is not simply a measurement of cardiovascular force. It reflects the interaction of multiple regulatory systems: kidney fluid balance, vascular tone, insulin signaling, nervous system activity, circadian rhythm, liver detoxification, and inflammatory load. When these systems lose coordination, the body gradually shifts toward persistent vascular tension.
The problem is that early hypertension symptoms rarely feel dramatic. They are subtle, systemic, and often misattributed to stress, fatigue, or lifestyle overload.
At iThrive ALIVE, hypertension is viewed not as a single disorder but as a network imbalance. Recognizing early warning signals allows intervention before structural vascular damage occurs.
To understand this progression more deeply, you may also explore our clinical case analysis “Case Breakdown: How Correcting Metabolic Dysfunction Improved Thyroid Function Without Escalating Medication”, which explains how systemic dysfunction alters hormonal regulation long before laboratory thresholds shift.
Blood pressure reflects how strongly blood pushes against arterial walls. When vascular resistance increases or fluid volume expands, pressure rises.
However, symptoms rarely correlate directly with numbers. Many individuals experience physiological strain even before entering the diagnostic range.
This happens because the body initially compensates by increasing heart rate, altering kidney sodium handling, tightening blood vessels, and elevating stress hormones. These adaptive responses produce subtle sensations that people rarely associate with blood pressure.
Hypertension damages gradually. Arteries stiffen, endothelial signaling declines, and microcirculation becomes inefficient. These changes occur slowly, making early symptoms appear non-specific.
Instead of pain or acute dysfunction, individuals experience fatigue, tension, poor recovery, or metabolic disturbances.
In other words, symptoms are systemic, and not localized.
These signs do not occur randomly. Each reflects a specific physiological mechanism linked to vascular resistance, nervous system activity, or metabolic stress.
Elevated nighttime blood pressure reduces normal nocturnal dipping. This causes vascular tension in cerebral circulation, producing heaviness on waking.
Reduced microvascular perfusion limits oxygen delivery to tissues. Cells produce energy inefficiently, leading to constant low-grade exhaustion.
Sympathetic nervous system activation increases cardiac workload even at rest often driven by insulin resistance or stress hormones.
Blood vessel stiffness reduces the body’s ability to adjust pressure quickly during posture change.
Elevated cortisol and adrenaline raise vascular tone while overstimulating the nervous system.
Microvascular strain affects retinal circulation, often an early indicator of vascular dysfunction.
Delayed heart rate normalization and fatigue after activity indicate reduced cardiovascular efficiency.
Muscle tension often reflects sympathetic overactivation and restricted circulation.
Night-time cortisol elevation interferes with deep sleep phases required for cardiovascular repair.
Kidney sodium retention increases blood volume, subtly raising pressure.
These symptoms often appear in combination and not in isolation.

Most explanations of hypertension focus on sodium intake or stress alone. In reality, early symptoms arise from network dysfunction.
Insulin resistance increases renal sodium retention, activates the sympathetic nervous system, and promotes vascular inflammation. This relationship is explored in depth in our educational article “Insulin Resistance: The Silent Phase Before Type 2 Diabetes.”
Healthy blood vessels produce nitric oxide to relax and dilate. Oxidative stress reduces this capacity, increasing vascular resistance.
Chronic stress keeps the body in a constant alert state, preventing normal vascular relaxation.
Late-night light exposure, irregular sleep, and poor recovery impair hormonal regulation of blood pressure.
Magnesium, potassium, and vitamin D are essential for vascular flexibility and fluid balance.
When these systems drift out of synchrony, early symptoms begin to appear, way long before sustained hypertension develops.

The typical response to elevated blood pressure is medication adjustment. While sometimes necessary, symptom progression usually reflects deeper physiological imbalance.
This is why iThrive ALIVE emphasizes comprehensive physiological assessment rather than isolated BP management.
If symptoms are persistent, the most effective approach is to book a root cause analysis to identify regulatory breakdowns before structural vascular damage develops.
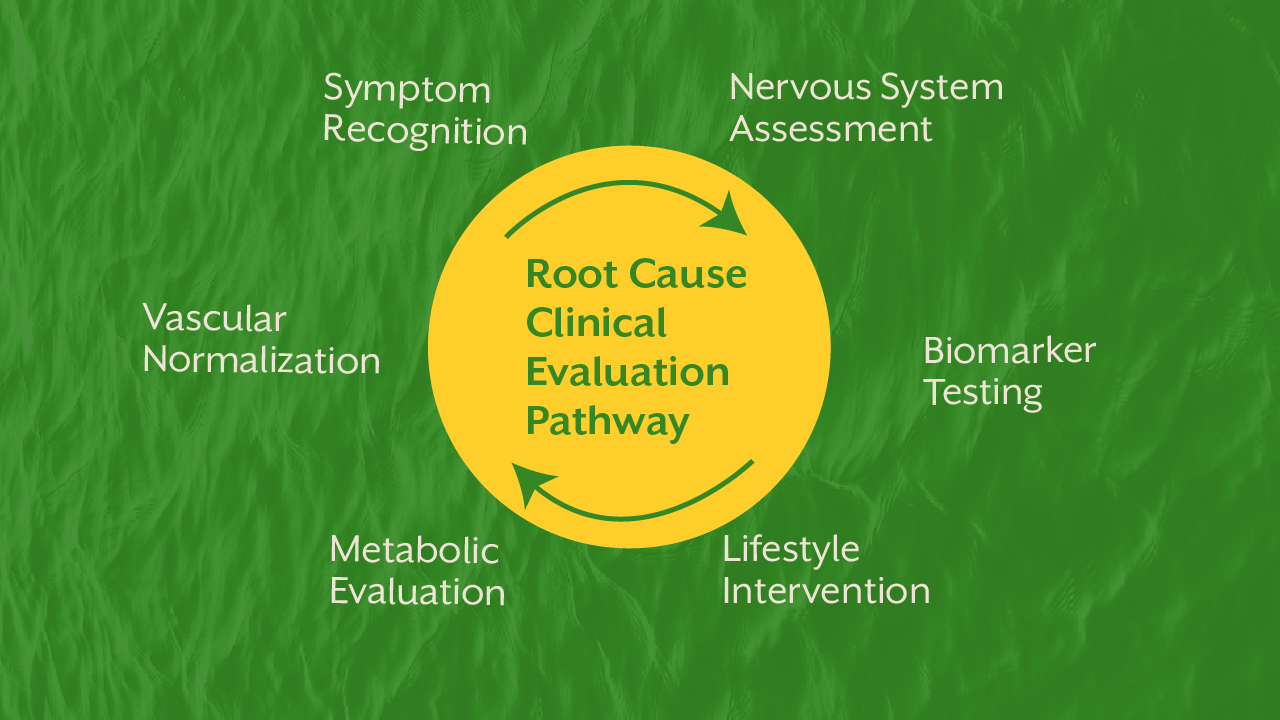
Blood vessels adapt continuously. When elevated pressure persists, structural remodeling begins like arterial thickening, stiffness, and reduced elasticity.
Once these changes occur, reversal becomes more difficult.
Early symptom recognition allows intervention during the functional stage, when regulatory systems can still be recalibrated.
Lifestyle restructuring, targeted micronutrient support, circadian alignment, and metabolic correction can restore vascular balance before irreversible damage develops.
High blood pressure rarely begins with a diagnosis, it begins with subtle physiological signals that reflect systemic imbalance. Early high BP symptoms such as fatigue, tension, poor sleep, and morning head pressure are not random discomforts; they are regulatory warnings from the cardiovascular network. Hypertension is fundamentally a systems disorder involving metabolism, nervous system activity, hormonal rhythms, and vascular health. Recognizing early signs allows intervention before structural damage occurs. A root-cause clinical model that evaluates metabolic health, micronutrient status, sleep physiology, and inflammatory load provides the most effective strategy for long-term cardiovascular stability.




.svg)
In clinical practice, thyroid dysfunction is rarely an isolated glandular disorder. It is more often a downstream reflection of systemic dysregulation in the form of metabolic, inflammatory, neurological, and cellular.
Yet conventional treatment models frequently operate within a hormone-replacement paradigm. When symptoms persist or worsen, medication dosage is adjusted. When lab markers fluctuate, dosing is recalibrated. The underlying assumption is simple: thyroid dysfunction equals thyroid hormone deficiency.
However, emerging metabolic and systems biology research suggests a more complex reality. Thyroid physiology is tightly integrated with glucose metabolism, mitochondrial activity, immune signaling, gut integrity, and neuroendocrine stress responses. Disruption in any of these systems can impair hormone signaling even when circulating hormone levels appear adequate.
This case breakdown examines a clinical scenario where thyroid function improved significantly without escalating medication, simply by correcting metabolic dysfunction.
The objective is not to argue against medication when needed but to demonstrate how addressing systemic drivers can restore regulatory efficiency, often reducing physiological strain on the thyroid axis itself.
This system's perspective aligns closely with the clinical model discussed in Healing Hypothyroidism: The Functional Role of Nutrition in Thyroid Health, where thyroid regulation is viewed through nutritional and systemic modulation rather than gland-centric intervention.
Thyroid hormones function less like isolated endocrine outputs and more like metabolic coordinators. They regulate:
When metabolic signaling becomes inefficient, thyroid hormone action becomes compromised, not always because hormone production is low, but because hormone utilization is impaired.

One of the most powerful modulators of thyroid signaling is insulin sensitivity. Insulin resistance alters hepatic enzyme activity responsible for T4-to-T3 conversion, modifies inflammatory cytokine profiles, and influences receptor responsiveness at tissue level.
This interrelationship is also explored in Causes of Insulin Resistance, which describes how inflammatory signaling and metabolic stress interfere with endocrine communication across multiple systems.
When insulin signaling is impaired, tissues become metabolically inflexible. In this environment, thyroid hormone cannot effectively stimulate energy production, even if circulating levels appear normal.
The result is functional hypothyroid physiology without overt hormone deficiency.
The individual in this case had been diagnosed with hypothyroidism and maintained on stable medication for several years. Laboratory values remained within reference range, yet symptoms persisted:
Despite medication adherence, metabolic function continued to decline.
Importantly, thyroid hormone levels were not severely abnormal. The issue was not production failure, it was signaling inefficiency.
This distinction is critical.
The thyroid axis was functioning, but the metabolic environment was hostile to hormone activity.
Detailed assessment identified three major regulatory disruptions.
Elevated insulin levels suppress lipolysis, increase inflammatory signaling, and impair hepatic hormone conversion. The metabolic environment becomes energy-inefficient despite caloric sufficiency.
Pro-inflammatory cytokines interfere with receptor binding and intracellular signaling cascades. Hormones reach tissues but fail to trigger metabolic response.
This inflammatory-metabolic relationship is also discussed in What Causes Obesity?, where endocrine disruption is linked to inflammatory and environmental stressors.
Chronic stress alters hypothalamic signaling, modifies cortisol rhythms, and shifts energy allocation toward survival rather than regeneration.
When these drivers coexist, thyroid hormone becomes biologically underutilized.

Rather than escalating medication, intervention targeted systemic regulation.
Structured macronutrient timing to stabilise insulin dynamics and support mitochondrial energy generation. Anti-inflammatory nutrient density prioritised micronutrient sufficiency required for enzymatic conversion.
Muscle tissue is the largest glucose disposal organ. Increasing lean mass improves insulin sensitivity and enhances metabolic responsiveness to thyroid hormone.
Stress reduction protocols aimed to restore hypothalamic signaling integrity and reduce cortisol-driven metabolic disruption.
Specific nutrients involved in thyroid conversion, receptor function, and mitochondrial activity were optimised.
The intervention did not target the thyroid gland directly, it restored the environment in which thyroid hormones operate.

Over several months, measurable changes occurred:
Most notably, thyroid medication dose remained unchanged yet functional markers improved.
This demonstrates a key physiological principle:
Hormone function depends as much on cellular responsiveness as on hormone quantity.
This case illustrates that thyroid dysfunction is often a systems disorder expressed through endocrine signaling.
Treating the gland without addressing metabolic context may stabilise lab values but fail to restore physiological function.
A systems-based evaluation including metabolic, inflammatory, gut, and stress parameters enables identification of regulatory bottlenecks that conventional testing may overlook.
This integrative clinical perspective forms the foundation of evaluation models that prioritise functional restoration rather than isolated hormone correction.
Individuals seeking deeper investigation into persistent symptoms despite treatment may benefit from structured metabolic assessment, such as a Book a Root Cause Analysis evaluation or Book a Consult to explore regulatory drivers.
This case demonstrates that improving thyroid function does not always require increasing medication. When metabolic dysfunction, inflammatory signaling, and neuroendocrine stress are corrected, hormone efficiency can improve naturally. Thyroid physiology is not governed solely by glandular output but by the biological environment in which hormones operate. A clinically effective strategy therefore focuses on restoring systemic balance, further improving insulin sensitivity, reducing inflammation, enhancing mitochondrial function, and stabilising nervous system signaling. When the regulatory network becomes efficient, thyroid hormone can perform its role effectively, often reducing the need for pharmacological escalation. True endocrine recovery is therefore not about forcing hormone levels upward, but about rebuilding the physiological systems that allow hormones to function properly.




.svg)
For many individuals diagnosed with thyroid dysfunction, treatment begins and ends with medication. Hormone replacement or suppression can normalize laboratory values, but it does not always resolve persistent thyroid symptoms such as fatigue, weight changes, hair loss, brain fog, or temperature sensitivity. This gap between biochemical correction and physiological recovery is becoming increasingly recognized in clinical practice.
The thyroid gland does not function in isolation. Thyroid hormone function depends on nutrient availability, cellular energy production, immune stability, metabolic health, circadian rhythm integrity, and stress signaling. When these regulatory systems are disrupted, medication alone cannot fully restore thyroid physiology.
This explains why individuals with “normal thyroid levels” may continue to experience thyroid disease symptoms. It also explains why thyroid problems are rising globally, particularly among young adults and women. The issue is not simply hormone deficiency, it is regulatory dysfunction.
Lifestyle interventions influence the very mechanisms that determine how thyroid hormones are produced, converted, transported, and used by cells. Understanding these mechanisms transforms how we approach thyroid treatment. Instead of managing hormone levels alone, we begin restoring the biological environment that allows thyroid regulation to occur naturally.
This systems-based approach is central to clinical work at iThrive Alive, where thyroid physiology is evaluated as part of a broader metabolic and regulatory network rather than as an isolated endocrine problem.
Medication replaces or modifies hormone levels. But thyroid regulation is more complex than hormone presence in the bloodstream.
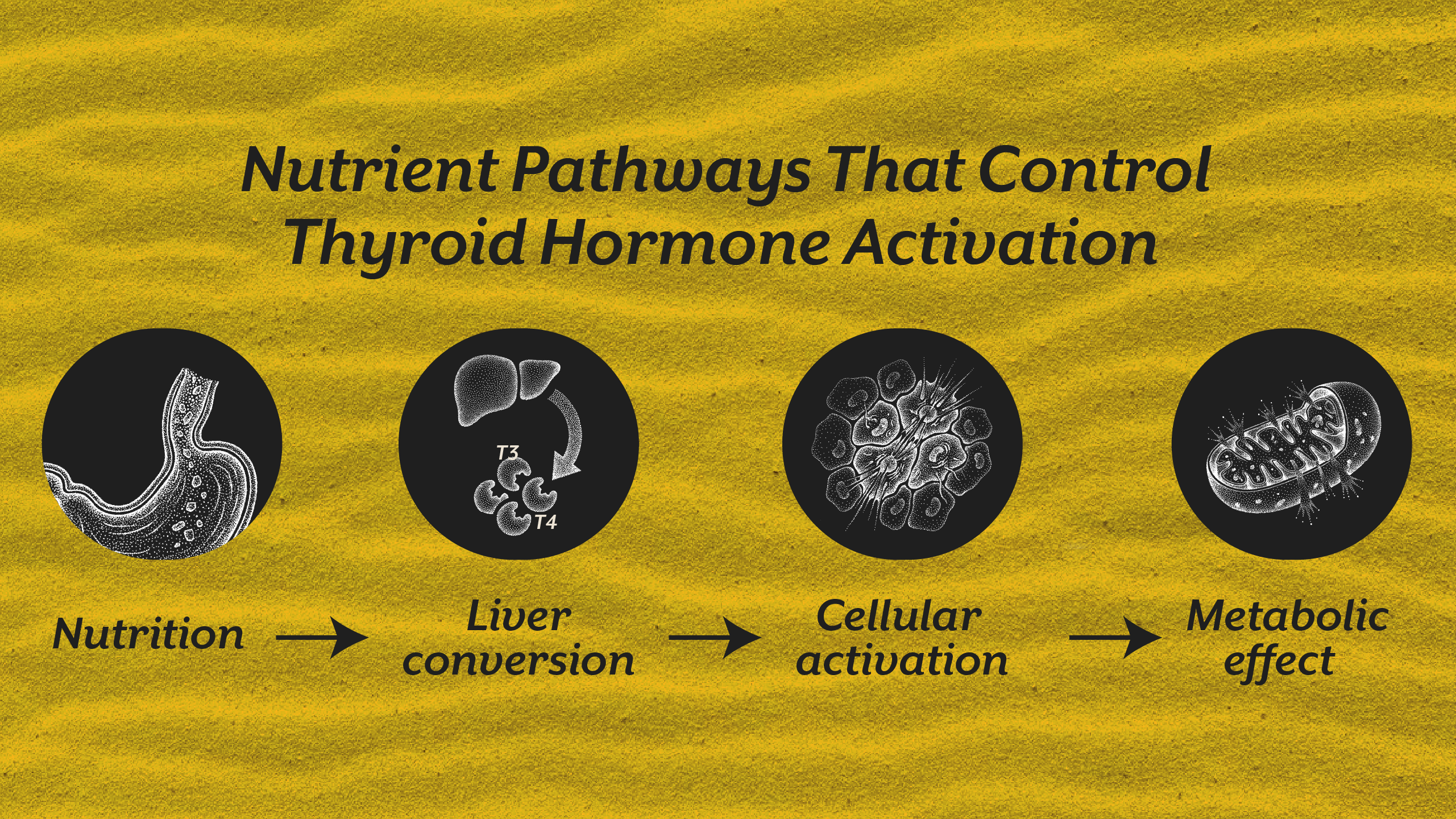
Thyroid hormones must be absorbed, converted, transported into cells, and activated at the mitochondrial level to produce metabolic effects. Disruption at any step can produce thyroid symptoms even when laboratory values appear normal.
The most circulating thyroid hormone is T4, an inactive precursor. Cells require T3, the active form. Conversion depends on liver function, gut health, micronutrient sufficiency, and inflammatory load. When conversion is impaired, individuals may experience symptoms of hypothyroidism despite normal thyroid levels.
Hormone signaling depends on receptor sensitivity and mitochondrial energy production. Chronic stress, insulin resistance, and inflammation reduce cellular responsiveness, meaning hormones cannot exert full metabolic effects.
Sleep quality, circadian rhythm, and nervous system balance influence hormone release patterns. Disrupted rhythms alter metabolic signaling and contribute to thyroid causes that standard treatment does not address.
Medication corrects hormone concentration. Lifestyle interventions restore regulatory function.
Nutrition influences thyroid health far beyond iodine intake. Hormone production, conversion, and cellular utilization depend on multiple nutrient-dependent pathways.
Selenium supports T4 to T3 conversion. Zinc influences receptor binding. Iron supports thyroid enzyme activity. Deficiency in any of these alters hormone efficiency rather than hormone quantity.
Adequate protein intake supports hepatic hormone processing and stabilizes blood glucose. Metabolic instability disrupts thyroid signaling through stress hormone activation.
Chronic inflammatory signaling interferes with hormone conversion and increases reverse T3 production, a metabolically inactive form that slows cellular energy production.
For many individuals searching “diet for thyroid patients” or “best food for thyroid patients,” the relevant question is not simply what to eat, but what metabolic environment food creates.
Stress is one of the most underestimated thyroid causes. It directly alters hormone conversion, receptor sensitivity, and metabolic signaling.
Elevated cortisol reduces T4 to T3 conversion and increases reverse T3 production. This slows metabolism and contributes to fatigue and weight gain.
Chronic sympathetic activation prioritizes survival over energy expenditure. The body conserves energy by reducing thyroid activity.
Poor sleep alters hypothalamic-pituitary signaling, affecting hormone release timing and metabolic efficiency.
Individuals searching “how to control thyroid naturally” often overlook stress physiology as a primary regulatory factor.
Thyroid function is tightly linked to metabolic health. Insulin resistance alters hormone transport and cellular energy availability.
When cells cannot effectively use glucose, metabolic signaling changes. The body reduces energy expenditure, which is reflected in altered thyroid hormone activity.
This connection explains why individuals with weight changes, fatigue, and hair loss often experience overlapping metabolic and thyroid disease symptoms.
Metabolic regulation is therefore a critical component of natural thyroid treatment.
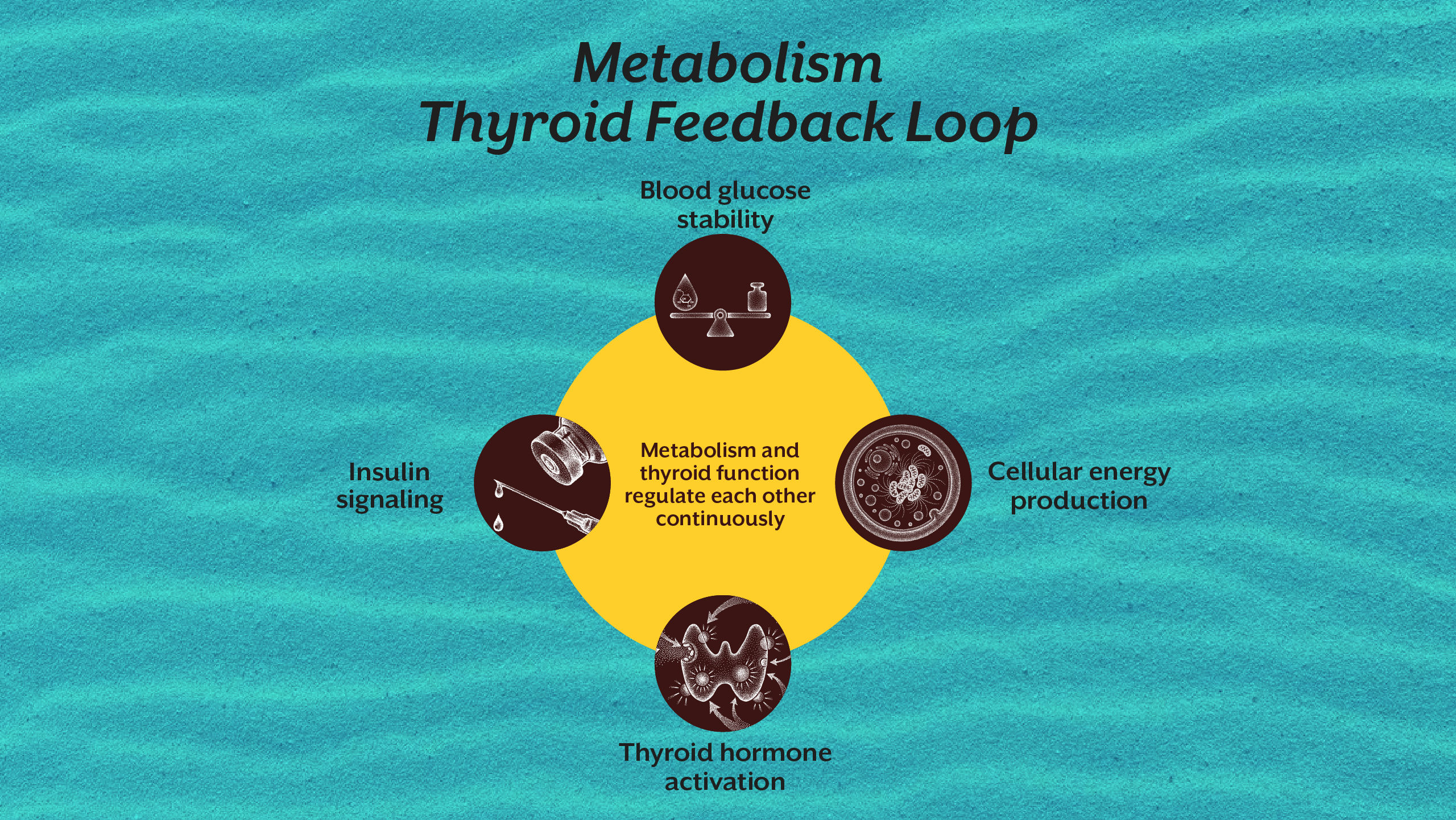
Thyroid hormones follow daily rhythmic patterns. Light exposure, sleep timing, and meal timing influence hormone release and metabolic efficiency.
Circadian disruption alters endocrine communication between the brain and thyroid gland. Shift work, irregular sleep, and late-night eating interfere with this coordination.
Many individuals with persistent thyroid symptoms also show circadian misalignment, yet this remains rarely addressed in standard thyroid treatment.
Physical activity influences mitochondrial function, hormone receptor sensitivity, and metabolic flexibility. Sedentary behavior reduces cellular energy production and slows thyroid-mediated metabolism.
Resistance training, in particular, improves glucose utilization and enhances tissue responsiveness to thyroid hormones.
Movement therefore functions as a metabolic regulator rather than merely a calorie-burning tool.

No single lifestyle change restores thyroid function for everyone. Each individual’s regulatory imbalance differs like their nutrient deficiency, metabolic dysfunction, immune activation, or stress physiology.
This is why comprehensive evaluation is essential. Identifying specific drivers allows targeted lifestyle interventions rather than generalized advice.
Individuals seeking deeper understanding of persistent thyroid disease symptoms often choose to book a root cause analysis or book a consult to evaluate regulatory factors beyond hormone levels.
Lifestyle interventions do not replace medication when clinically required. Instead, they enhance physiological responsiveness and improve long-term regulation.
This integrative perspective is explored in greater depth in:
• “Why Thyroid Disorders Are Rising: The Hidden Root Causes Conventional Testing Misses”
• “The Thyroid-Gut Axis: How Microbiome Imbalance Disrupts Hormone Conversion”
Together, these frameworks explain why natural treatment for thyroid must address regulatory networks rather than isolated hormone levels.
Thyroid regulation is not determined solely by the gland or by hormone concentration in blood tests. It emerges from the coordinated function of metabolic signaling, nutrient availability, stress physiology, circadian rhythm, immune balance, and cellular energy production. Medication can correct hormone levels, but it cannot independently restore the biological systems that regulate hormone activation and responsiveness. Sustainable thyroid health therefore requires a systems-level approach that integrates nutrition, sleep, stress regulation, metabolic stability, and personalized clinical evaluation. When these regulatory networks are supported, the body regains the capacity to maintain thyroid balance naturally rather than relying exclusively on external hormone control.




.svg)
Most conversations around thyroid dysfunction focus on hormone levels, medication, and symptom management. Yet emerging systems biology research shows that thyroid physiology does not operate in isolation. Hormone production in the thyroid gland is only one part of a much larger regulatory network that includes immune signalling, liver metabolism, and increasingly, the gut microbiome.
The concept of the thyroid-gut axis reflects a deeper biological reality: intestinal microbes participate directly in hormone activation, immune tolerance, nutrient absorption, and inflammatory regulation. When microbial balance is disrupted, the effects extend far beyond digestion. Hormone conversion efficiency declines, immune surveillance shifts, and inflammatory signals begin interfering with endocrine communication.
This is why individuals may present with persistent thyroid symptoms despite “normal thyroid levels” on laboratory testing. The gland may be producing hormones, but downstream activation and cellular utilisation may be compromised by gut dysfunction.
Understanding the microbiome and thyroid connection helps explain rising thyroid disorders, especially autoimmune thyroiditis and metabolic thyroid resistance. It also clarifies why comprehensive thyroid treatment must extend beyond the gland itself.
The thyroid gland primarily produces thyroxine (T4), a storage hormone. Only a small fraction of circulating hormones exists as triiodothyronine (T3), the metabolically active form that regulates cellular energy production, temperature regulation, and metabolic signalling.
Activation from T4 to T3 is not controlled solely by the thyroid gland. It depends on deiodinase enzymes distributed throughout the body and particularly in the liver, peripheral tissues, and importantly, the gastrointestinal system.
A significant portion of thyroid hormone metabolism occurs through enterohepatic circulation. Hormones are conjugated in the liver, secreted into bile, and then processed again by intestinal bacteria. Specific microbial enzymes help deconjugate hormone metabolites, allowing them to be reabsorbed and reused.
When microbial diversity is reduced, this recycling pathway becomes inefficient. Hormone clearance may increase, active hormone availability declines, and metabolic signalling weakens even when hormone production appears adequate.
This explains why gut dysbiosis and hypothyroidism frequently coexist, not merely as parallel conditions but as mechanistically linked processes.
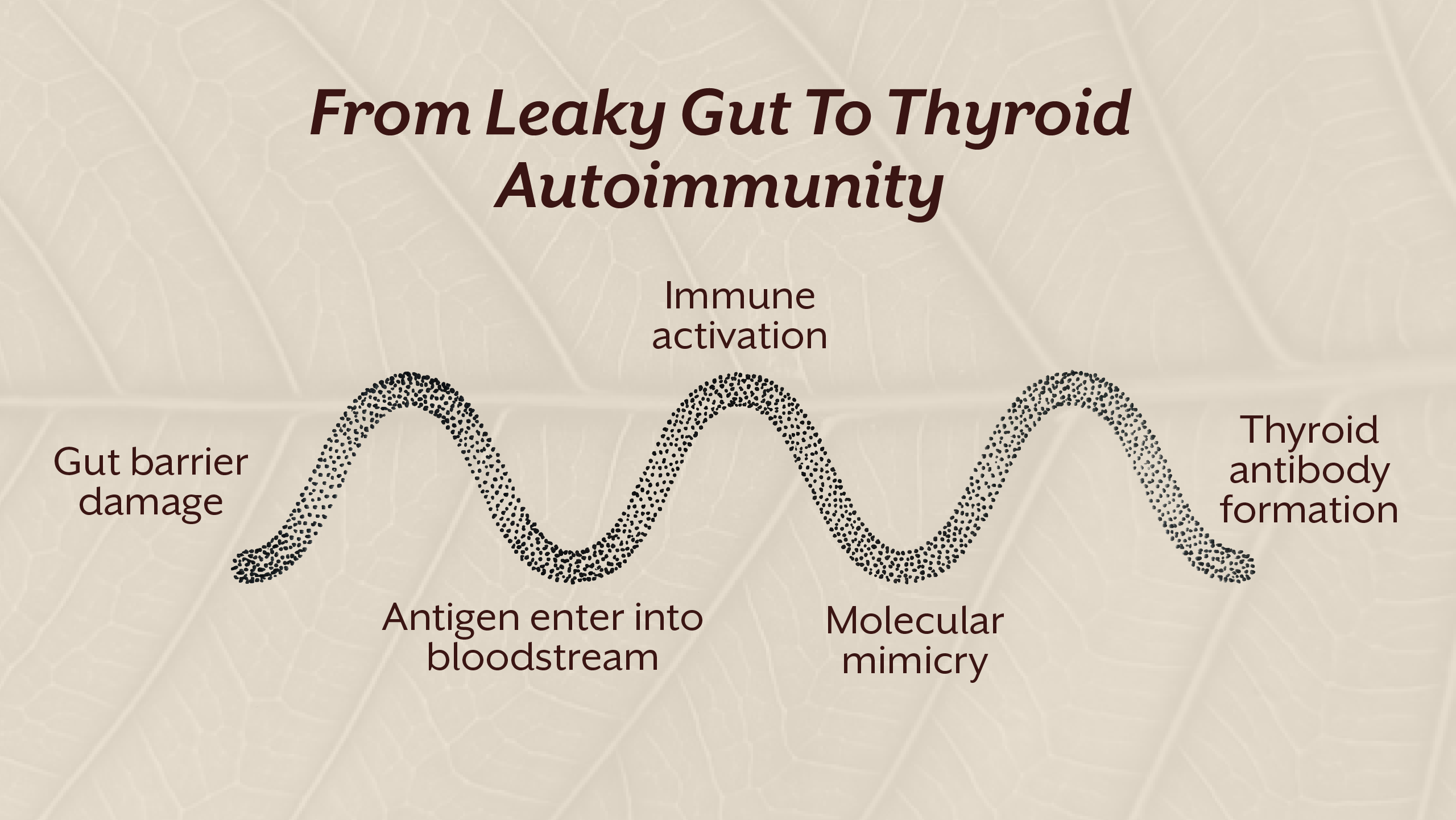
Nearly seventy percent of immune activity originates within the gastrointestinal system. The intestinal barrier acts as both a physical and immunological filter, determining which molecules enter systemic circulation.
When microbial balance is stable, immune tolerance is maintained. Regulatory immune cells prevent unnecessary inflammatory responses, protecting self-tissues including endocrine glands.
When dysbiosis develops, inflammatory signalling increases. Gut permeability rises. Antigen exposure expands. Immune regulation becomes unstable.
This environment increases the likelihood of thyroid antibodies forming, a defining feature of autoimmune thyroid disorders such as Hashimoto’s thyroiditis and other forms of thyroiditis.
Certain intestinal bacteria produce enzymes such as beta-glucuronidase that influence hormone reactivation. These enzymes regulate how efficiently conjugated thyroid hormones are reabsorbed rather than eliminated.
When microbial diversity declines, enzyme activity becomes unpredictable. Hormones may be excessively eliminated or improperly reactivated. The result is functional hormone deficiency at the tissue level.
This is one of the lesser discussed thyroid causes meaning altered microbial enzyme activity affecting endocrine signalling.
Inflammatory stress alters hormone conversion pathways. Instead of converting T4 into active T3, the body may increase production of reverse T3, an inactive molecule that blocks receptor activity.
Gut inflammation is a major contributor to this shift. Inflammatory cytokines suppress deiodinase activity while activating stress signalling pathways that favour energy conservation.
This physiological adaptation may be protective during acute illness. However, chronic gut inflammation can sustain high reverse T3 levels, slowing metabolism despite adequate hormone production.
Thyroid hormone synthesis and activation depend heavily on micronutrients such as selenium, zinc, iodine, iron, and tyrosine. These nutrients are absorbed primarily in the gastrointestinal tract.
Dysbiosis reduces absorption efficiency. Inflammatory changes impair transport mechanisms. Enzymatic digestion becomes inconsistent.
Even with an optimal diet, individuals with gut imbalance may develop functional nutrient deficiency, impairing thyroid hormone function and contributing to persistent thyroid disease symptoms.

Certain intestinal bacteria produce enzymes such as beta-glucuronidase that influence hormone reactivation. These enzymes regulate how efficiently conjugated thyroid hormones are reabsorbed rather than eliminated.
When microbial diversity declines, enzyme activity becomes unpredictable. Hormones may be excessively eliminated or improperly reactivated. The result is functional hormone deficiency at the tissue level.
This is one of the lesser discussed thyroid causes meaning altered microbial enzyme activity affecting endocrine signalling.
Inflammatory stress alters hormone conversion pathways. Instead of converting T4 into active T3, the body may increase production of reverse T3, an inactive molecule that blocks receptor activity.
Gut inflammation is a major contributor to this shift. Inflammatory cytokines suppress deiodinase activity while activating stress signalling pathways that favour energy conservation.
This physiological adaptation may be protective during acute illness. However, chronic gut inflammation can sustain high reverse T3 levels, slowing metabolism despite adequate hormone production.
Thyroid hormone synthesis and activation depend heavily on micronutrients such as selenium, zinc, iodine, iron, and tyrosine. These nutrients are absorbed primarily in the gastrointestinal tract.
Dysbiosis reduces absorption efficiency. Inflammatory changes impair transport mechanisms. Enzymatic digestion becomes inconsistent.
Even with an optimal diet, individuals with gut imbalance may develop functional nutrient deficiency, impairing thyroid hormone function and contributing to persistent thyroid disease symptoms.
Standard thyroid treatment typically focuses on hormone replacement or suppression depending on clinical presentation. While this approach can stabilize circulating hormone levels, it does not address upstream regulatory disturbances.
If gut inflammation persists, conversion pathways remain impaired. If microbial imbalance continues, immune activation remains elevated. If nutrient absorption is compromised, hormone utilisation remains inefficient.
Patients may therefore achieve laboratory normalisation without full physiological restoration.
This explains why many individuals with thyroid symptoms continue experiencing fatigue, metabolic slowing, and immune activation despite treatment.
A clinically effective thyroid strategy must address the entire regulatory network.
Interventions targeting microbial diversity, intestinal barrier repair, inflammatory modulation, and micronutrient repletion influence hormone conversion more profoundly than gland-focused interventions alone.
This systems-biology perspective is central to the clinical model used at iThrive Alive, where thyroid physiology is evaluated as part of an integrated metabolic and immune framework.
Rather than isolating the gland, assessment includes gut health, inflammatory load, nutrient status, and stress physiology. This enables identification of root drivers behind hormone dysregulation.
Individuals seeking deeper evaluation can book a root cause analysis or book a consult to explore underlying regulatory imbalances rather than focusing solely on hormone levels.

The thyroid-gut axis represents one of the most clinically significant yet under-recognised regulatory pathways in endocrine physiology. Hormone production within the thyroid gland is only the beginning of metabolic signalling. Activation, recycling, immune tolerance, and cellular response depend heavily on microbial balance, intestinal integrity, and inflammatory regulation. When gut dysbiosis develops, hormone conversion shifts, reverse T3 increases, immune reactivity intensifies, and nutrient availability declines. These processes can sustain thyroid dysfunction even when laboratory values appear stable. Understanding thyroid physiology through the lens of systems biology reveals why comprehensive treatment must extend beyond hormone replacement toward restoration of microbial balance, immune stability, and metabolic resilience.




.svg)
Across the world, thyroid disorders are increasing at an unprecedented rate. Clinics are reporting more cases of hypothyroidism, autoimmune thyroid disease, and unexplained thyroid symptoms in people who were previously considered low risk including young adults, adolescents, and individuals with no family history of endocrine disease.
This rise is not simply a matter of better diagnosis. It reflects a deeper shift in human physiology.
Many individuals today experience fatigue, hair fall, weight changes, mood fluctuations, and metabolic slowdown despite “normal thyroid levels” on laboratory reports. This disconnect between symptoms and test results has created confusion for both patients and practitioners.
To understand why thyroid problems are increasing, we must move beyond viewing the thyroid as an isolated gland. The thyroid is not an independent organ working in isolation. It is a regulatory node within a vast metabolic communication network involving the immune system, gut microbiome, liver detoxification, cellular energy production, and brain signaling.
When these systems destabilize, thyroid hormone function is affected long before standard diagnostic markers change.
At iThrive Alive, thyroid dysfunction is rarely viewed as the starting problem. It is often the downstream consequence of deeper biological stressors that conventional testing does not fully capture.
Understanding these hidden drivers is the first step toward meaningful thyroid recovery.
Most people understand the thyroid as a gland that produces hormones controlling metabolism. While this is true, it is incomplete.
Thyroid hormones regulate mitochondrial activity, the rate at which cells convert nutrients into usable energy. Every tissue in the body depends on this process, especially the brain, liver, reproductive organs, and muscles. When thyroid hormone function changes, the body does not simply “slow down.” Cellular energy efficiency shifts, altering everything from glucose metabolism to inflammation signaling.
This explains why thyroid disease symptoms extend far beyond weight gain or fatigue. They influence fertility, mood stability, cardiovascular function, immune activity, and even detoxification capacity.
However, hormone production is only one layer of thyroid physiology. The body must also convert, transport, activate, and utilize these hormones correctly. Many individuals with thyroid symptoms do not have a hormone production problem, they rather have a hormone utilization problem.
This distinction is rarely assessed in routine screening.
Most thyroid evaluations focus on TSH and sometimes T3 and T4 levels. While these markers provide useful information, they represent only a narrow window into thyroid physiology.
Several critical processes are rarely measured:
The body must convert T4 into active T3. Stress, inflammation, nutrient deficiencies, and liver dysfunction can impair this conversion. When this happens, thyroid levels appear normal, but cellular metabolism slows.
Autoimmune activity often begins years before hormone disruption. Elevated thyroid antibodies signal immune-mediated gland damage even when thyroid levels remain within reference range.
This is a major reason thyroid problems in young adults are rising, and immune dysregulation is increasing globally.
Cells must respond to hormonal signals. Chronic inflammation and metabolic dysfunction can reduce receptor sensitivity, creating functional hypothyroidism without abnormal lab values.

Understanding thyroid causes requires looking beyond the gland itself.
Insulin resistance alters hormonal signaling across the endocrine system. It promotes inflammation, disrupts liver metabolism, and interferes with thyroid hormone activation.
This metabolic connection is explored in our blog “Hyperinsulinemia: Hidden Cause of Weight Gain and Diabetes.” The same mechanism that drives metabolic disease also contributes to thyroid dysfunction.
Autoimmune thyroid disease is now one of the most common thyroid disorders globally. Environmental triggers, gut permeability, chronic infections, and micronutrient deficiencies alter immune tolerance.
The immune system begins identifying thyroid tissue as foreign.
Modern exposure to plastics, pesticides, heavy metals, and synthetic chemicals interferes with hormone receptors and iodine metabolism. These compounds can mimic or block thyroid signaling.
Despite abundant food availability, micronutrient intake has declined. Selenium, zinc, iodine balance, iron, and tyrosine are essential for thyroid hormone synthesis and activation.
Many individuals eating adequate calories still lack the biochemical building blocks for thyroid health.
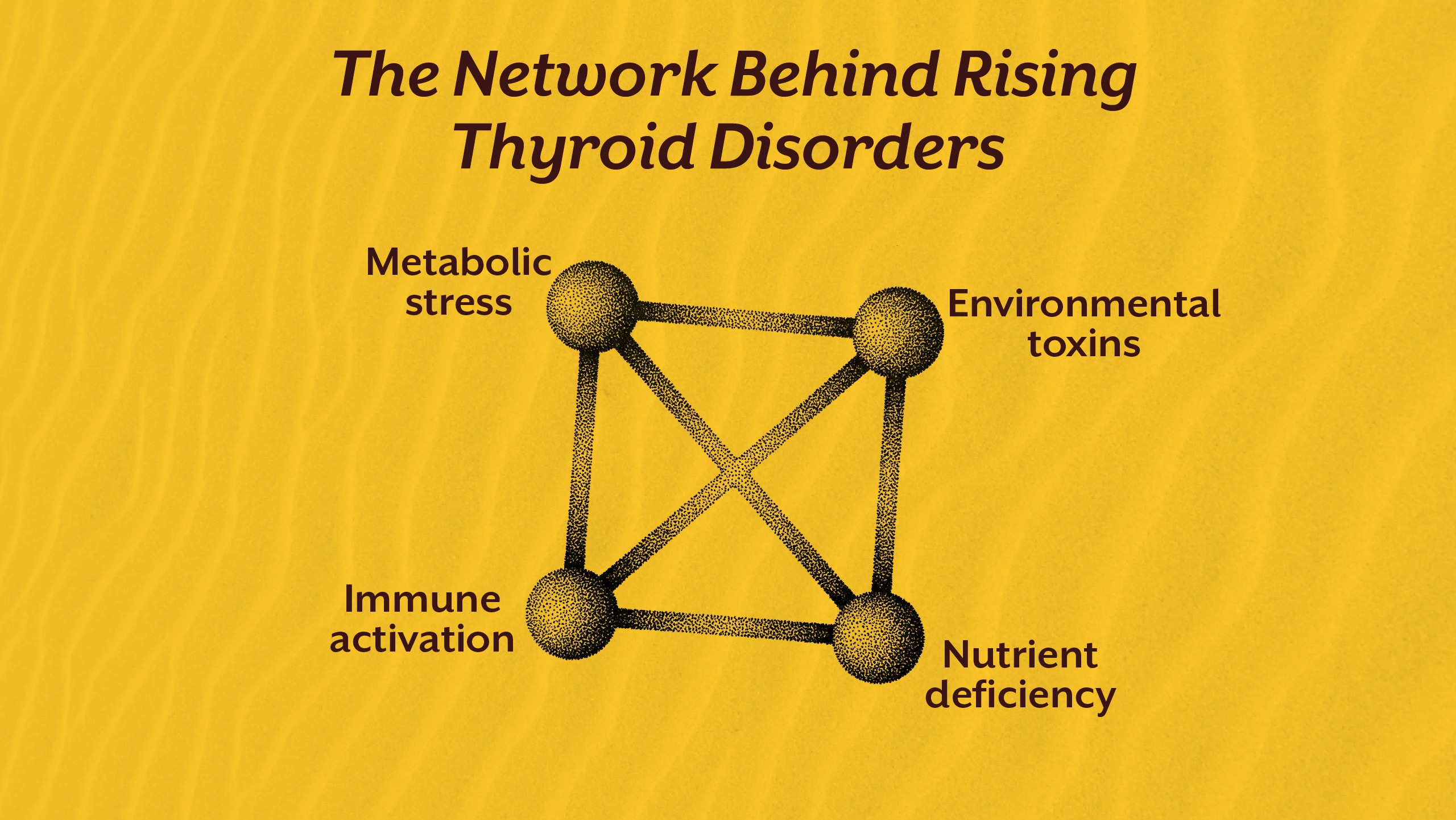
Emerging research shows that gut health plays a central role in thyroid regulation.
The gut microbiome influences nutrient absorption, immune balance, inflammation control, and hormone recycling. When gut integrity is compromised, immune activation increases, and thyroid antibodies often rise.
Additionally, a significant portion of thyroid hormone conversion occurs in peripheral tissues influenced by microbial activity.
This is why many individuals with persistent thyroid symptoms also experience digestive discomfort, food sensitivities, or unexplained inflammation.
Dietary patterns therefore matter deeply. Questions like thyroid me kya khana chahiye or best food for thyroid patients cannot be answered without understanding gut function first.
Many individuals search for thyroid symptoms in female or thyroid symptoms in male populations because they experience persistent unexplained health changes despite “normal” results.
This occurs because biological systems fail gradually. Cellular stress accumulates. Hormone signaling becomes inefficient. Immune activity escalates. But laboratory reference ranges detect change only after significant physiological disruption.
Symptoms such as fatigue, cold sensitivity, mood instability, and metabolic slowdown often reflect early regulatory dysfunction rather than advanced disease.
By the time traditional thresholds shift, dysfunction may have been present for years.
This concept is explored further in “What Most Nutrition Courses Miss About Obesity and Metabolic Disease,” where metabolic adaptation is shown to precede diagnosable illness.
Rather than viewing thyroid dysfunction as purely hormonal deficiency, the iThrive Alive model evaluates the systems that regulate thyroid signaling.
Assessment includes metabolic health, inflammation load, gut integrity, micronutrient sufficiency, immune activation, and stress physiology.
Interventions emphasize:
• Structured nutrition designed for metabolic stability
• Smart supplementation targeting biochemical deficiencies
• Lifestyle interventions that restore circadian rhythm and cellular energy
Hormonal support may be considered, but only within a broader physiological framework.
Individuals seeking deeper evaluation can book a root cause analysis to understand the drivers behind their thyroid imbalance rather than simply managing laboratory values.
The rising prevalence of thyroid disorders reflects more than glandular malfunction. It represents systemic physiological stress affecting immune balance, metabolic signaling, environmental adaptation, and cellular energy production. Conventional testing captures only the final stages of dysfunction, often missing early disruption in hormone conversion, receptor sensitivity, and immune activation. True thyroid health depends on the integrity of interconnected biological systems including gut, metabolism, immunity, and cellular energy pathways. When these foundations are restored, thyroid regulation becomes more responsive and resilient. Understanding this integrated physiology shifts thyroid care from symptom management toward genuine biological recovery.


A complete blood panel of 60+ parameters, collected from your home by a phlebotomist. Analysis by a dedicated functional nutritionist using optimal ranges, not the standard reference ranges your doctor uses. Your symptoms, lifestyle, and health history factored into the analysis. And a 60 to 90-minute one-on-one video consultation where your nutritionist walks you through everything they found. The blood tests are included in the price. There are no hidden charges or extra cost for anything.

A complete blood panel of 60+ parameters, collected from your home by a phlebotomist. Analysis by a dedicated functional nutritionist using optimal ranges, not the standard reference ranges your doctor uses. Your symptoms, lifestyle, and health history factored into the analysis. And a 60 to 90-minute one-on-one video consultation where your nutritionist walks you through everything they found. The blood tests are included in the price. There are no hidden charges or extra cost for anything.

A complete blood panel of 60+ parameters, collected from your home by a phlebotomist. Analysis by a dedicated functional nutritionist using optimal ranges, not the standard reference ranges your doctor uses. Your symptoms, lifestyle, and health history factored into the analysis. And a 60 to 90-minute one-on-one video consultation where your nutritionist walks you through everything they found. The blood tests are included in the price. There are no hidden charges or extra cost for anything.

A complete blood panel of 60+ parameters, collected from your home by a phlebotomist. Analysis by a dedicated functional nutritionist using optimal ranges, not the standard reference ranges your doctor uses. Your symptoms, lifestyle, and health history factored into the analysis. And a 60 to 90-minute one-on-one video consultation where your nutritionist walks you through everything they found. The blood tests are included in the price. There are no hidden charges or extra cost for anything.

A complete blood panel of 60+ parameters, collected from your home by a phlebotomist. Analysis by a dedicated functional nutritionist using optimal ranges, not the standard reference ranges your doctor uses. Your symptoms, lifestyle, and health history factored into the analysis. And a 60 to 90-minute one-on-one video consultation where your nutritionist walks you through everything they found. The blood tests are included in the price. There are no hidden charges or extra cost for anything.

A complete blood panel of 60+ parameters, collected from your home by a phlebotomist. Analysis by a dedicated functional nutritionist using optimal ranges, not the standard reference ranges your doctor uses. Your symptoms, lifestyle, and health history factored into the analysis. And a 60 to 90-minute one-on-one video consultation where your nutritionist walks you through everything they found. The blood tests are included in the price. There are no hidden charges or extra cost for anything.

A complete blood panel of 60+ parameters, collected from your home by a phlebotomist. Analysis by a dedicated functional nutritionist using optimal ranges, not the standard reference ranges your doctor uses. Your symptoms, lifestyle, and health history factored into the analysis. And a 60 to 90-minute one-on-one video consultation where your nutritionist walks you through everything they found. The blood tests are included in the price. There are no hidden charges or extra cost for anything.



