Introduction
Multiple sclerosis is often described as a neurological disease where the immune system attacks the brain and spinal cord. For decades the focus of research and treatment has been centered almost entirely on the nervous system. Yet emerging evidence suggests that the earliest drivers of this condition may begin far from the brain.
Many researchers are now exploring a deeper question. What if the biological origins of multiple sclerosis start in the gut.
The human digestive system is not only responsible for breaking down food. It also houses trillions of microorganisms, regulates immune responses, and communicates continuously with the brain through what scientists call the gut brain axis.
When this communication system is disrupted, inflammation, immune dysfunction, and metabolic stress can develop across the body. In individuals with the multiple sclerosis disease, these systemic disturbances may create conditions that allow the immune system to mistakenly attack the protective myelin sheath surrounding nerve fibers.
Understanding the causes of MS therefore requires looking beyond the nervous system and exploring the metabolic and microbial environment of the entire body.
This broader perspective is central to the clinical model used at iThrive Alive, where chronic illness is approached through a systems biology framework rather than an organ isolated view.
Understanding Multiple Sclerosis Beyond The Brain
Multiple sclerosis is classified as an autoimmune condition of the central nervous system. In this MS disorder the immune system mistakenly attacks the myelin sheath that surrounds nerve fibers. Myelin acts as an insulating layer that allows electrical signals to travel rapidly between the brain and the rest of the body.
When myelin is damaged, communication between nerve cells slows down or becomes disrupted. Over time this can lead to symptoms such as muscle weakness, coordination problems, fatigue, and cognitive changes.
While these symptoms appear neurological, the biological processes driving them often involve immune dysfunction and chronic inflammation.
Many individuals diagnosed with the MS medical condition also show systemic imbalances including gut dysbiosis, nutrient deficiencies, and metabolic stress. These underlying disruptions may influence immune signaling long before neurological symptoms appear.
In other words, the brain may be the site where symptoms appear, but the biological triggers can originate elsewhere.
The Gut Brain Axis In Multiple Sclerosis
The gut brain axis describes the communication network between the digestive system and the central nervous system. This communication occurs through immune signaling molecules, the vagus nerve, microbial metabolites, and inflammatory pathways.
The gut microbiome plays an important role in regulating immune tolerance. Certain beneficial bacteria help train immune cells to recognize the difference between harmful invaders and the body’s own tissues.
When the gut microbiome becomes imbalanced, a state known as gut dysbiosis, immune regulation can weaken.
Research in the multiple sclerosis disease has identified patterns of microbiome disruption including the reduced presence of protective bacteria such as Akkermansia muciniphila. This bacterium helps maintain the protective mucosal layer of the intestine and supports intestinal barrier integrity.
When these protective organisms decline, the gut lining can become more vulnerable to inflammation and permeability changes.
This process is often referred to as intestinal permeability or leaky gut.
Once the intestinal barrier becomes compromised, microbial fragments and undigested food proteins may enter the bloodstream. These molecules can trigger immune activation and systemic inflammation that affects distant organs including the brain.
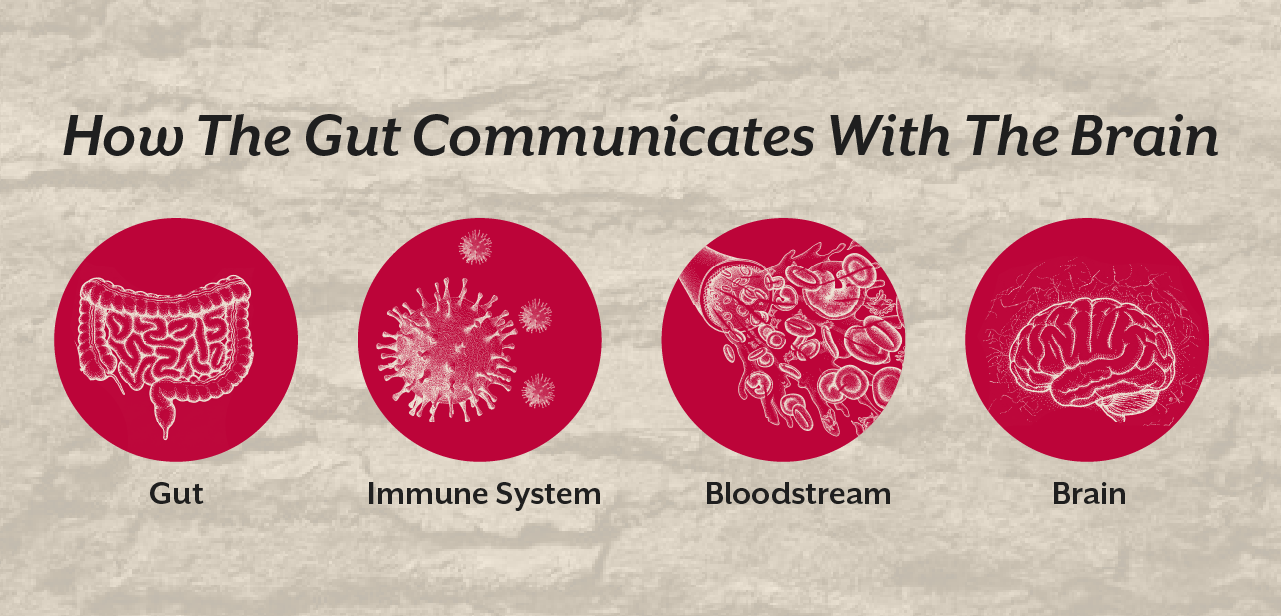
Intestinal Permeability And Immune Activation
One of the most important mechanisms linking gut health to the causes of MS is intestinal permeability.
The intestinal lining normally acts as a selective barrier that allows nutrients to pass into the bloodstream while preventing toxins and pathogens from entering circulation.
In individuals with chronic inflammation, the proteins that regulate intestinal tight junctions can become disrupted. One biomarker associated with this process is zonulin.
Elevated zonulin levels are commonly observed in individuals experiencing increased intestinal permeability.
When tight junctions open excessively, foreign molecules can enter the bloodstream and stimulate the immune system. This immune activation can become chronic, creating a pro-inflammatory environment throughout the body.
Over time this inflammatory state may weaken the blood brain barrier, the protective layer that normally shields the brain from circulating immune cells.
When this barrier becomes compromised, inflammatory signals can reach the central nervous system and contribute to the demyelination process characteristic of multiple sclerosis.

Mitochondrial Dysfunction And Neuroinflammation
Another layer of complexity in the causes of MS involves mitochondrial dysfunction.
Mitochondria are the energy producing structures inside cells that generate ATP, the molecule that powers cellular activity.
In the nervous system, neurons require enormous amounts of energy to transmit electrical signals and maintain structural integrity.
When mitochondrial function declines, neurons become more vulnerable to oxidative stress and inflammatory damage.
Studies in the MS disorder have identified markers of oxidative stress and mitochondrial impairment in both immune cells and neurons.
Elevated homocysteine levels, often associated with impaired methylation pathways, can further increase oxidative stress in the nervous system.
When energy production becomes inefficient, the nervous system struggles to repair damaged myelin and maintain normal nerve function.
This metabolic vulnerability may contribute to the progression of neurological symptoms seen in multiple sclerosis.
Microbial Imbalance And Chronic Inflammation
The composition of the gut microbiome can strongly influence immune balance.
Beneficial bacteria produce short chain fatty acids and other metabolites that help regulate inflammation and support intestinal barrier function.
When these beneficial microbes decline, harmful bacteria may gain dominance. This imbalance can amplify inflammatory signaling throughout the body.
Research in individuals with the multiple sclerosis disease has identified increased levels of certain inflammatory bacterial species along with reduced microbial diversity.
The absence of protective microbes such as Akkermansia muciniphila may weaken the gut barrier while allowing inflammatory signals to travel through the vagus nerve toward the brain.
This microbial imbalance creates a persistent loop of inflammation between the gut and the nervous system.
Why Symptoms Often Appear Years Later
One of the most confusing aspects of MS disease is the delay between biological dysfunction and visible symptoms.
Gut barrier disruption, microbiome imbalance, and metabolic stress may develop gradually over many years. During this time the immune system remains chronically activated even before neurological damage becomes obvious.
When the cumulative burden of inflammation and mitochondrial stress reaches a certain threshold, symptoms begin to emerge.
Fatigue, muscle weakness, and cognitive difficulties may appear slowly before a formal diagnosis of the MS medical condition is made.
Understanding this long biological timeline is essential because it suggests that the origins of the disease may precede symptoms by many years.
A Systems Approach To Multiple Sclerosis
Conventional multiple sclerosis treatment primarily focuses on suppressing immune activity to slow disease progression.
While these therapies can reduce relapse frequency, they often do not address the metabolic and microbial drivers that may influence immune dysregulation.
A systems approach evaluates multiple physiological layers including gut health, nutrient status, mitochondrial function, and inflammatory signaling.
At iThrive Alive this broader perspective forms the foundation of the 3 months Alive program. The goal is not only symptom management but also restoration of metabolic balance across interconnected biological systems.
This approach often includes strategies that support intestinal barrier integrity, improve microbiome diversity, replenish micronutrients, and optimize cellular energy metabolism.
For individuals experiencing persistent neurological symptoms, exploring these deeper biological factors can offer valuable insights into their condition.

When Root Causes Are Explored
If you or someone you know is living with multiple sclerosis symptoms, it is important to remember that chronic illness rarely develops from a single factor.
Instead it often emerges from the interaction between immune signaling, metabolic stress, gut health, and cellular energy systems.
By understanding these deeper biological layers, individuals may gain a clearer picture of the mechanisms influencing their health.
For those seeking a deeper evaluation of their metabolic and immune status, it may be helpful to book a root cause analysis with iThrive Alive. This process looks beyond surface level symptoms to identify the drivers influencing long term health.
Key Takeaway
Multiple sclerosis is often viewed purely as a neurological condition, yet growing research suggests that its biological roots may extend far beyond the nervous system. Gut barrier dysfunction, microbial imbalance, immune activation, and mitochondrial stress can interact over many years before symptoms appear. The gut brain axis provides an important framework for understanding how disturbances in digestive health may influence neuroinflammation and immune dysregulation. By approaching the multiple sclerosis disease through a systems perspective that includes gut health, metabolism, and cellular energy production, new opportunities may emerge for supporting long term neurological resilience and improving overall quality of life.


.svg)
.svg)
































.svg)
