



.svg)




.svg)
Dietary fiber is important for a healthy diet, but it is often forgotten despite its many health benefits. It's an essential part of a wholesome, balanced diet that has been proven to prevent disease, maintain digestive health, and promote overall well-being. This reading discusses the value of dietary fiber and the types of fiber, what it does in the body, the benefits to health, how much is needed and fiber food sources through comprehensive research.
Dietary fibre is the edible parts of plants or analogous carbohydrates that are resistant to digestion and absorption in the human small intestine with complete or partial fermentation in the large intestine. Unlike other carbs, such as starch and sugar, which are broken down into sugar, fiber goes through the body undigested, providing a number of health benefits.
Soluble Fiber: This type dissolves in water, creating a gel-like substance in the digestive system. It can help reduce cholesterol and stabilize blood sugar levels. Common sources include oats, beans, lentils, fruits, and psyllium husk.
Insoluble Fiber: This type does not dissolve in water and helps add bulk to stool, facilitating regular bowel movements. It is found in whole grains, nuts, seeds, and the skins of fruits and vegetables.
Digestive Health: Fiber supports regular bowel movements, lowering the risk of constipation and other digestive issues. Studies show that a high-fiber diet promotes a healthier gut microbiota, which is vital for digestion and immune health. A healthy gut microbiota relies on fiber to nourish beneficial bacteria, leading to improved digestion and reduced bloating.
Weight Management: Foods high in fiber are typically low in calories but high in volume, which helps promote feelings of fullness. Research suggests that increasing fiber intake can assist with weight loss and maintenance by lowering overall calorie consumption, thus minimizing overeating and unnecessary snacking.
Heart Health: Soluble fiber is effective in lowering cholesterol levels. It can decrease total blood cholesterol by reducing low-density lipoprotein (LDL) levels. Additionally, it helps manage blood pressure and decrease inflammation.
Blood Sugar Control: Eating fiber, particularly soluble fiber, aids in regulating blood sugar levels, which is crucial for diabetes management. A high-fiber diet can enhance glycemic control by slowing the absorption of sugar into the bloodstream. Meals rich in fiber help maintain steady blood sugar levels, preventing spikes and crashes.
While fiber may not be the most glamorous nutrient, it is undeniably vital for long-term health. From supporting digestion to preventing diseases and even enhancing mental well-being, fiber is a fundamental component of a balanced diet. Incorporate fiber into your meals to reap its significant benefits. The importance of fiber is immense making it a part of your daily nutrition is a straightforward yet powerful step toward improved health.




.svg)
Do you also feel you are a victim of raised, red, scaly patches on the skin usually called skin rash? Then there are the symptoms of Psoriasis, a chronic skin condition. When the immune system is overactive, it accelerates the development of skin cells, which leads to rapid build-up and inflammation known as plaques. Different body parts like the scalp, elbows, and knees are affected by Psoriasis. It can also lead to psoriatic arthritis. Some people mistake these symptoms for Eczema but you need to know that Psoriasis and Eczema have much in common. Hence, people usually get confused between them. Eczema rashes tend to affect skin folds and be itchier.
Around 2-3% of the global population seems to be in the clutches of Psoriasis, which is around 125 million people worldwide. In 2019, reports stated that there were 40.8 million cases worldwide. There has been a 20% drop since 1990. It was discovered that the age-standardized incidence rate per 100,000 people varied significantly by region.2 The highest rate of the age-standardized incidence rate of psoriasis was found in high-income countries and territories and vice versa was found in low SDI countries as they reported the lowest rate. Psoriasis is most common in people aged 60 to 69, and it is almost equally found in men and women.
If you have an itchy, dry rash, then it might be easy to be confused between the two. Eczema and Psoriasis lead to rashes that come and go, these are called flare-ups. 1 Sometimes it takes months or even years for these flare-ups to go. These two even have similar appearances. But do you know the difference between these two and how deep is Psoriasis skin deep? If not, then let’s examine it bit by bit. Here is the difference between psoriasis versus eczema:
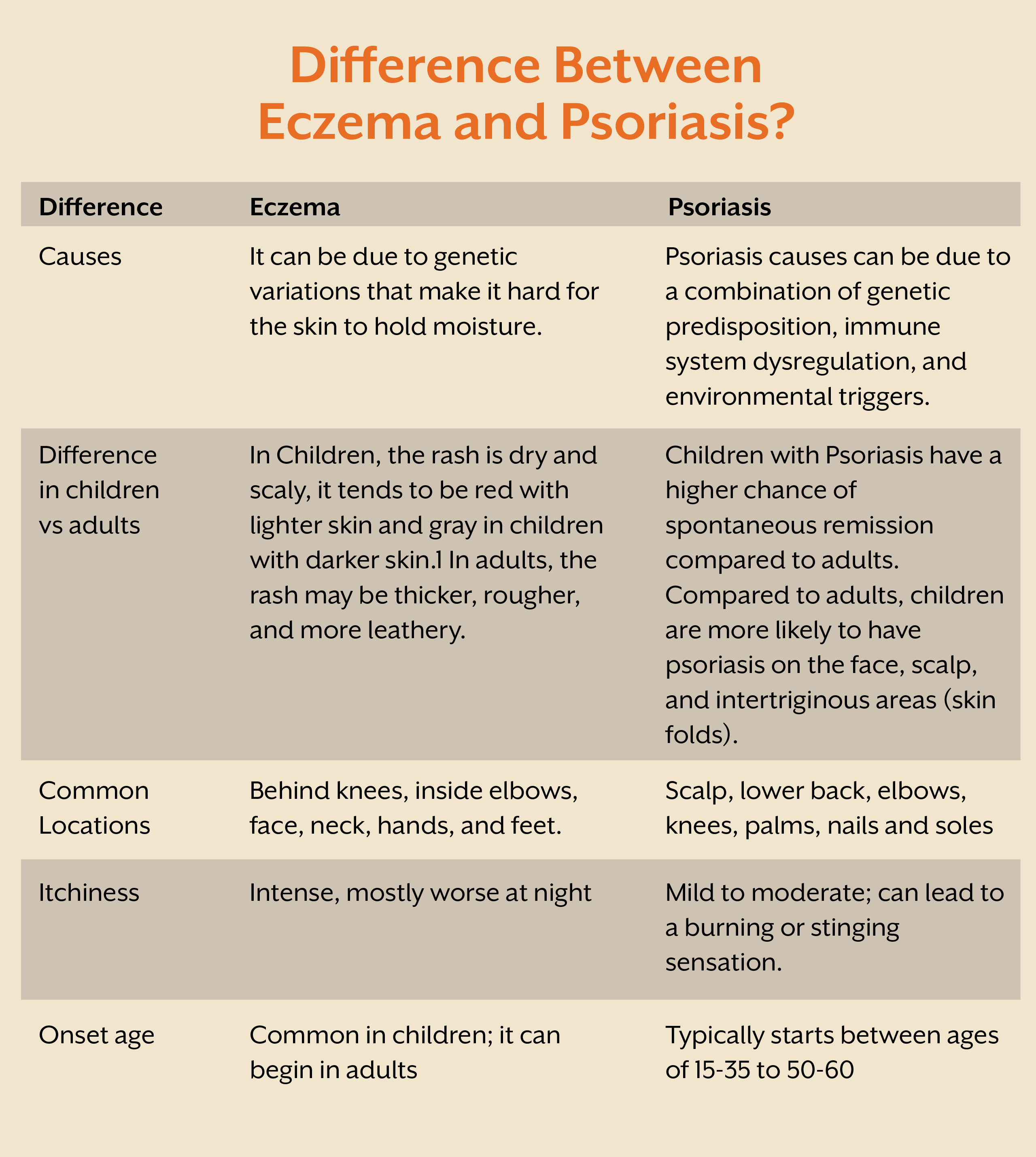

Psoriasis is a chronic autoimmune condition that accelerates skin cell turnover, causing the skin's surface to rapidly accumulate skin cells. It can be caused due to a combination of genetic predisposition and environmental triggers. There are different types of Psoriasis such as
The most common psoriasis is Plaque, affecting 80-90% of the individuals suffering from Psoriasis. It presents itself as red patches, raised with silver-white scales. The scalp, trunk, and limbs—particularly the elbows and knees—are where these plaques typically grow on the body in a symmetrical pattern.2
If you have small, drop-shaped spots that look red on the torso or limbs. It is common in children and young adults and it might get triggered by a strep throat infection.
These are present beneath the breast or in the groin armpits, appearing to be smooth, red patches in folds of skin. Sweating and rubbing can trigger it and make it worse.
Pustular psoriasis is characterized by pus- filled bumps called pustules surrounded by red skin. It usually targets feet and hands, but there is a form that covers most of the body. It can get triggered by infections, stress, medications or certain chemicals.
This is a rare type of psoriasis that is differentiated by red, scaly skin over most of the body. A bad sunburn or certain medication can trigger it. It is usually found in people who struggle with different types of psoriasis that are not well controlled. Erythrodermic psoriasis can turn out to be very serious. 2
It is a non-contagious skin condition that is chronic. It develops thick and scaly patches on the scalp and sometimes the surrounding areas.

The exact cause of psoriasis is unclear but it can be triggered by environmental factors and can also be caused by family history. Here are the risk factors for psoriasis that can help individuals at high risk manage the condition easily-
Having a family history of psoriasis can increase your chances of developing it. The lifetime risk of psoriasis can be 14-28% if one parent has it. If both of the parents have it, then the risk increases up to 40-65%. If your sibling has it then it elevates it further. Psoriasis has been linked to genetic mutations, such as those in the CARD14 gene, albeit not all people who have these mutations go on to get the condition.3
It is recognized that certain drugs might contribute to or worsen psoriasis disease symptoms. These consist of:
Even small changes in lifestyle can trigger psoriasis-like-
Psoriasis can be triggered due to environmental factors in predisposed individuals such as
Psoriasis can be triggered because of varied infections like streptococcal throat infection. Infections like HIV may also increase the severity or risk of the condition.
Psoriasis is predominantly an immune-mediated condition in which healthy skin cells are mistakenly attacked by the immune system, causing a rapid turnover of skin cells. Environmental variables and genetic predisposition both have an impact on this dysfunction.
Psoriasis varies from skin to skin, it looks different on different skins. On darker skin types, Psoriasis may look dark brown, purple, violet, or salmon with grayish scales. It looks red with silver scales on top of lighter skin. Additionally, during a flare-up of psoriasis, some people with darker skin may develop post-inflammatory hyperpigmentation, a change in skin tone that can take months to recover. Individuals of color with psoriasis might have more severe cases that can cover their bodies fully. 4

Having Psoriasis comes with a risk of developing other conditions including;
1. Obesity
3. Psoriatic arthritis, leading to pain, stiffness, and swelling in and around joints
4. Temporary skin color changes
5. Eye conditions like Blespharistis, conjunctivitis and uveitis
6. High blood pressure
7. Cardiovascular Disease
8. Autoimmune diseases such as Celiac disease, sclerosis, and Crohn’s disease
9 Mental health conditions like depression
Reducing flare-ups is like a dream come true for people with psoriasis, but it can be reduced with the right approach like opting for functional nutrition, emotional well-being, and tackling stress. These three areas can help people immensely-
1. Opt for Functional nutrition: It goes a long way as it focuses on personalized dietary strategies. Functional nutrition makes sure that you avoid psoriasis triggers and that your body is full of nutrients through the right diet and correct supplements. Get your free consultation today on whether an anti-inflammatory diet is right for you.
2. Avoid Stress
Stress is known to be a major factor in triggering psoriasis patient flare-ups. Learning to manage stress is an art, which is also necessary here. You can consider trying the following to reduce stress:
3. Emotional health
Researchers believe that self-esteem issues and depression are sadly common symptoms in people dealing with psoriasis. 5 People dealing with this can try-

Psoriasis can be managed through a diet and a proper lifestyle. The diet focuses on anti-inflammatory foods while avoiding those that may trigger flare-ups along with psoriasis therapy. Here is a list of the things to include and avoid in your diet:
Psoriasis is a chronic inflammatory skin disorder rooted in the genes, found in 2-3% of the world’s population. It can be mistaken for eczema as they both share some similar features but they both are different and work on children and adults differently. There are a number of risk factors for psoriasis like genetics, medications, lifestyle, infections, and environmental triggers. This disease can also lead to complications So, living with it, individuals can focus on three areas: functional nutrition, stress, and emotional health to reduce its effects and avoid flare-ups. It might be an incurable disease but victory is just one day at a time.

1. Psoriasis vs. Eczema: How to Tell the Difference. (2024, December 9). WebMD. https://www.webmd.com/skin-problems-and-treatments/psoriasis/psoriasis-or-eczema
2. Branch, N. S. C. a. O. (2025, January 8). Psoriasis. National Institute of Arthritis and Musculoskeletal and Skin Diseases. https://www.niams.nih.gov/health-topics/psoriasis?
3. Barhum, L. (2024, January 6). Is psoriasis hereditary? Verywell Health. https://www.verywellhealth.com/is-psoriasis-hereditary-5191433?
4. Pfizer. (n.d.). Psoriasis Overview: Types, causes, symptoms, and treatment | Pfizer. https://www.pfizer.com/disease-and-conditions/psoriasis
5. Sahi, F. M., Masood, A., Danawar, N. A., Mekaiel, A., & Malik, B. H. (2020). Association between psoriasis and Depression: A traditional review. Cureus. https://doi.org/10.7759/cureus.9708




.svg)
The term sounds technical, but bioregulators are one of the most fascinating and natural ways to support your body’s healing and regeneration processes at the root level.
In this blog, we’ll break it down in simple words so that anyone, even without a medical background, can understand what bioregulators are, how they work, and why they’re different from supplements or medicines.
Bioregulators are tiny natural compounds, made up of just 2 to 4 amino acids (the building blocks of protein). These tiny chains are called short-chain peptides.
They come from animal tissues like the thymus, brain, or lungs. But they’re processed in a way that makes them safe and clean for human use.
They are like body messengers and send signals to specific parts of your body (like your immune system or your brain). They tell them to work better, heal faster, or regenerate cells.
Most supplements (like multivitamins or herbs) give your body general support- they boost overall health but don’t always solve a specific problem.
Bioregulators, on the other hand, are targeted. Each one is made to help a particular organ or system in your body. For example:
Bioregulators don’t just "add" something to your body like most supplements. Instead, they communicate with your cells, almost like reminding your body of how it's supposed to function.
Here’s how they work, step by step:
They bind to your DNA and switch on or off certain genes. This affects how your cells behave, especially when it comes to producing proteins.
Your body is made up of proteins. Every function, whether it’s healing, immunity, digestion, or even mood, depends on protein creation. Bioregulators help normalise this process.
Each bioregulator knows exactly where to go. The one for the lungs won’t go to the kidneys. It finds its exact target and starts working there.
Our body always tries to stay in balance. But with age, stress, or disease, this balance is disturbed. Bioregulators help restore that natural balance without forcing the body.
Most bioregulators are extracted from the organs and tissues of young animals (like calves or pigs) because their tissues are rich in active peptides.
For example:
These peptides are purified, cleaned, and tested for safety before they’re used in supplements or treatments.
Very small! Bioregulators are made up of just 2 to 4 amino acids. For comparison, your regular protein shake might have protein molecules made of 20 amino acids.
Because they are so tiny, they can:
Bioregulators are especially helpful when:
They are also being explored in anti-ageing therapies, immune support, and chronic disease management.
Here are a few real-world examples of how different bioregulators support different organs:

Vladonix A-6 (Thymus-based)
Cerluten A-5 (Brain cortex-based)
Thyreogen A-2
Chelohart A-14 (Heart tissue)
Taxorest A-19
Gotratix A-18
Visoluten & Pinalex
Yes, when sourced from reputable companies and used correctly, bioregulators are considered safe. They are non-toxic, non-allergenic, and have been studied for decades.
Still, always talk to your functional nutritionist or health care practitioner before starting any new supplement, especially if you have a medical condition or are on medication.
Bioregulators are not like painkillers. They don’t give instant results. They work slowly and naturally by helping your body heal from within. Some people notice changes in:
Bioregulators are mostly available as capsules or tablets. Some people take one type, while others take a stack (multiple peptides for different organs).
In a world full of quick fixes and synthetic drugs, bioregulators offer a natural, safe, and science-backed approach to healing.
Whether you’re trying to recover from stress, illness, or ageing or just want to support your organs in a targeted way, these could become a powerful part of your wellness journey.




.svg)
Does your mouth water too when you think of bread, cereals, processed food, and more but you can hear your stomach grumbling? Do you think you have gluten sensitivity? Could it be something else too? Celiac disease is very similar to gluten sensitivity as in this disease the small intestine is attacked by gluten. Celiac Disease affects 0.7% of the world’s population. About one-third of Indians are genetically predisposed to celiac disease. It is indeed a global disease, which is known to be a hereditary illness. This disease has become a cycle now and you can be the first one to break this cycle. It can end with you using functional nutrition and Ithrive. This blog sheds light on what it is and how you can get through this not as a survivor but as a winner. Let’s get into it.
Celiac disease is a persistent autoimmune disorder in which the small intestine is hypersensitive to gluten (a protein found in barley, rye, and wheat), which leads to indigestion. In this disease, gluten triggers an immune response that damages the intestine. Due to these attacks, Villi (small finger-like projections that lie in the small intestine) get damaged. When it gets damaged the body is not able to soak in the nutrients properly. That usually leads to malnourishment and weakened bones miscarriage and hormonal imbalance.
This disease usually runs in the family; it also means that a person’s chance of getting this disease is one in ten if they have parents, siblings, or other first-degree relatives who have this condition. other than that some of the causes for it are immune system dysregulation, environmental toxins and pollutants, gut microbiota imbalance, and moreIt can turn into a big health concern if not treated on time and anyone can inculcate it at any age.
Gluten intolerance (Non-Celiac gluten sensitivity) and Celiac disease are both responses to gluten, although they both differ in their seriousness and basic cause. In this disease, the body is attacked by gluten which leads to damage of the small intestine and it also leads to the body not being able to absorb nutrients whereas in gluten sensitivity, the body is unable to digest gluten but it doesn’t lead to any damage.

The symptoms of this disease are over two hundred but it depends from person to person. People at times do not even notice the symptoms until their intestine is damaged or their bones start to weaken. You might notice digestive symptoms right after eating or drinking something that has gluten, it is your wake-up call. If you do have these symptoms that means that it is time for you to get your root cause analysis done today. Here are some of the symptoms:

When Celiac disease goes unnoticed and untreated it can lead to long-term health conditions like:

Functional nutrition is a holistic approach that binds diet and lifestyle together and provides an individual with a better way to live. It addresses the root cause of health issues by going deep into 55+ blood parameters and working on them through supplementation, food changes, and lifestyle interventions. It aims to repair and rebuild the body that is damaged due to ailment.
It is a personalized approach that is science-based weaves functional medicine to autoimmune disease and conventional nutrients together. Here are the reasons why it is a great solution for this disease-
1. Focusing on Gut Health: An individual is provided with a list of things to eat and not to eat according to your reports by your personalized nutritionist.
2. Functional Nutrition Approach: Functional nutrition provides an individualized and comprehensive approach to managing Celiac disease helping to make your gut healthy again.

iThrive believes in turning your life around three sixty degrees with the right approach. Through booking a free consultation for Alive 2.0 an individual can get a better idea about how to improve his/ her digestive system and heal their gut with the help of functional nutrition. iThrive’s Alive 2.0 program helps in reviving the balance of your gut and improves it. Ithrive has been a part of more than 6000 people’s journeys and has helped reverse more than 174 diseases. Ithrive offers several facilities that others don't like-
Holistic approach with the help of root cause analysis
Celiac disease is an autoimmune disorder in which indigestion of gluten becomes difficult and that leads to hampering of intestine lining. It gives birth to other medical problems that if remained undiagnosed and untreated can become harmful. In India, there are very limited options to maintain a gluten-free diet with a lack of gluten labeling on packaged foods, etc. Traditional Indian diet contains wheat-based staples making it hard for individuals to look for substitutes. By adopting functional nutrition strategies, individuals can focus on their condition more effectively which helps them have a better quality of life and makes their progress sustainable. It is important to work with dietitians and nutritionists to get a personalized plan to fill the nutrition gaps.
1. Debnath, B. (2017b, September 10). About Six to Eight Million Indians Suffer from Celiac Disease. Medindia. https://www.medindia.net/news/about-six-to-eight-million-indians-suffer-from-celiac-disease-172924-1.htm
2. Urszula Krupa-Kozak, Pathologic bone alterations in celiac disease: Etiology, epidemiology, and treatment,Nutrition, Volume 30, Issue 1, 2014, Pages 16-24, ISSN 0899-9007, https://doi.org/10.1016/j.nut.2013.05.027.(https://www.sciencedirect.com/science/article/pii/S089990071300289X)
3. What is Celiac Disease? | Celiac Disease Foundation. (n.d.). Celiac Disease Foundation. https://celiac.org/about-celiac-disease/what-is-celiac-disease/
4. Calabriso, N., Scoditti, E., Massaro, M., Maffia, M., Chieppa, M., Laddomada, B., & Carluccio, M. A. (2022). Non-Celiac gluten sensitivity and protective role of dietary polyphenols. Nutrients, 14(13), 2679. https://doi.org/10.3390/nu14132679




.svg)
Your gut is not just a digestive organ but a central hub influencing your entire well-being. The trillions of microorganisms residing in your gastrointestinal tract, collectively known as the gut microbiome, maintain digestive health. It impacts your brain, skin, and liver functions.
This intricate network, often referred to as the gut-brain-skin-liver axis, underscores the profound interconnectedness of these systems.
An imbalance in your gut flora can manifest in various health issues, from mood disorders and cognitive impairments to skin conditions and liver diseases. Understanding and nurturing this connection is essential for achieving optimal health.
In this blog, we delve into how your gut microbiome influences these critical organs and provide actionable strategies to enhance your gut health, including the benefits of probiotics, dietary recommendations, and lifestyle modifications. By the end, you'll have a comprehensive understanding of the gut-body connection and practical steps to improve your overall well-being.
Your gut and brain are more connected than you think! The gut-brain axis is a two-way communication system that links your digestive system and nervous system.
A healthy gut can boost your mood, sharpen your memory, and even reduce stress, while an imbalanced gut can lead to anxiety, depression, and neurodegenerative diseases.

The gut and brain are constantly sending signals through:
A balanced gut microbiome lowers stress and anxiety by regulating the production of cortisol (the stress hormone). When your gut is inflamed or imbalanced, it can trigger mood disorders, brain fog and even increase the risk of Alzheimer’s.
Chronic gut inflammation triggers an immune response, leading to excessive cytokine production, which can harm brain cells.
SCFAs are powerful compounds produced by good gut bacteria when they break down fiber. They help:
Studies show that aging reduces SCFA levels, which may contribute to neurodegenerative diseases. However, a high-fiber diet restores SCFA production and improves brain health.1
As we age, our gut microbiome loses diversity, making it more vulnerable to harmful bacteria. Researchers found that transplanting a young gut microbiome into older mice improved their cognitive function and stroke survival rates.1
When we think about skin health, we often focus on skincare routines, expensive creams, and dermatology treatments. But what if the secret to clear, glowing skin isn’t just about what you apply externally but rather what’s happening inside your gut?
If you've been struggling with acne, eczema, psoriasis, or dry, irritated skin, your gut health might be the missing piece of the puzzle.
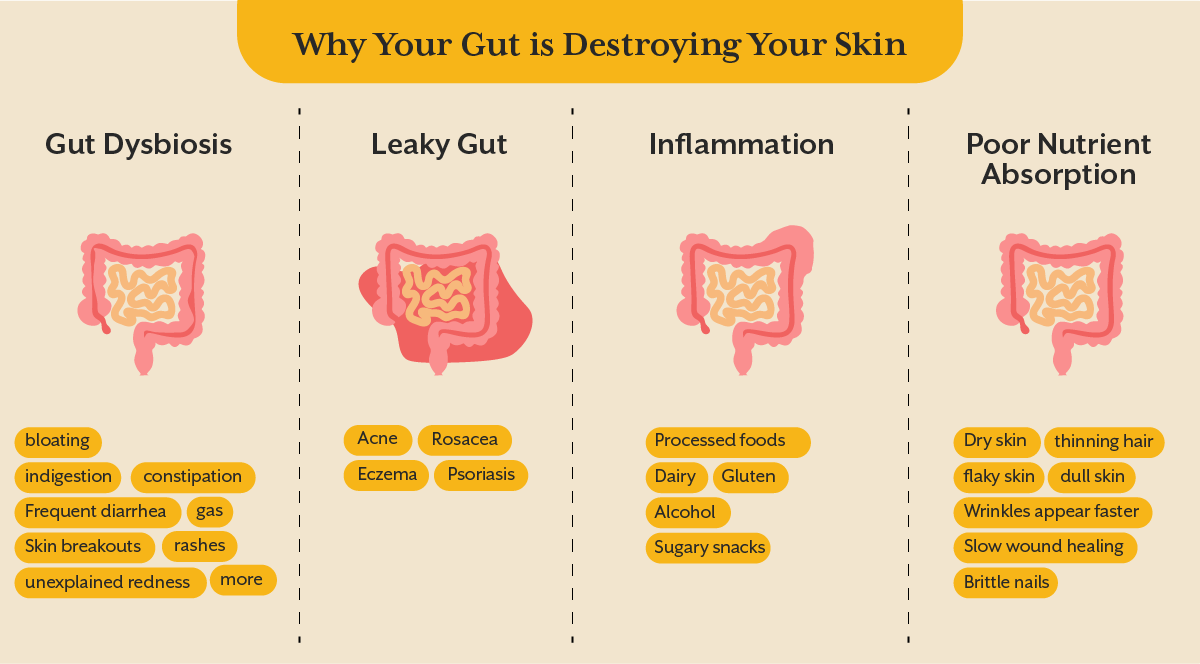
The gut and skin are deeply connected through what is known as the gut-skin axis. This means that an unhealthy gut can lead to skin problems, and poor skin health can indicate underlying digestive issues. When your gut microbiome falls out of balance, your skin is often one of the first places you’ll notice the damage.
A healthy gut contains good bacteria that support digestion, nutrient absorption, and immune function. But due to poor diet, stress, antibiotics, and toxins, this delicate balance gets disrupted.
When harmful bacteria take over, it leads to gut dysbiosis, a condition that wreaks havoc on your body, including your skin.
When dysbiosis occurs, your gut lining becomes weak and inflamed, leading to a condition called leaky gut syndrome.
Imagine your gut lining as a protective barrier. It should only allow beneficial nutrients to pass into your bloodstream while keeping toxins, undigested food, and bacteria out.
But when you have leaky gut, tiny gaps in your intestinal wall let harmful substances enter your bloodstream. Your immune system freaks out and starts an inflammatory response, causing breakouts, rashes, and skin conditions like eczema or psoriasis.
Chronic inflammation is at the core of almost every skin issue. Where does it start? Your gut. When your gut microbiome is imbalanced, inflammatory compounds spread through your bloodstream, affecting your skin’s ability to heal and regenerate.
These foods disrupt your gut bacteria, trigger blood sugar spikes, and increase inflammation, leading to more breakouts, redness, and irritation.
If your gut isn’t absorbing key nutrients, your skin can’t repair itself. Collagen, biotin, zinc, and omega-3 fatty acids are essential for keeping skin youthful and hydrated, but gut issues rob your body of these skin-saving nutrients.
If your gut is unhappy, your skin will show it. However, you can heal your gut naturally through diet and lifestyle changes.

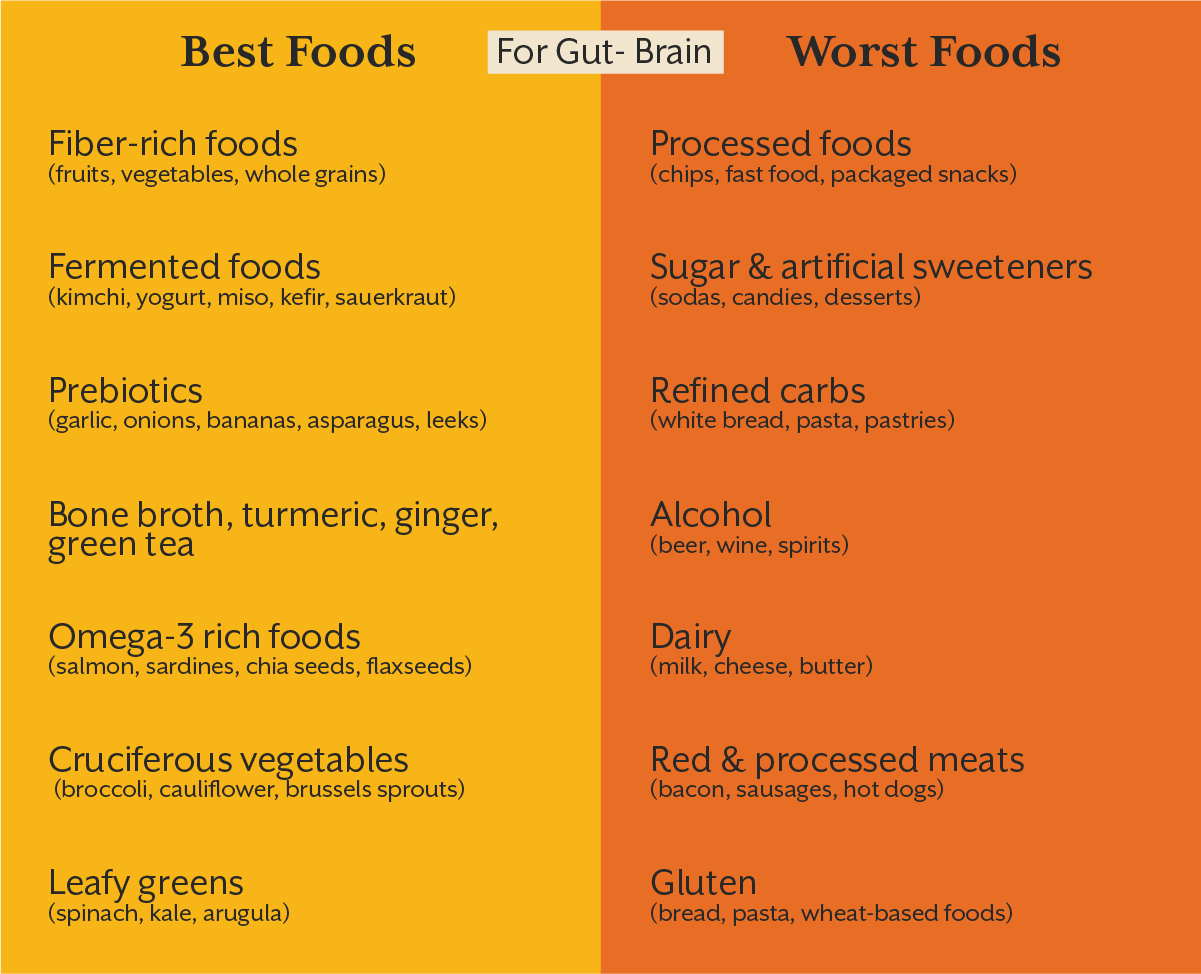
Eating the right foods can nourish your gut and improve your skin at the same time. Here’s what to add to your plate:
Probiotics help restore balance in the gut microbiome and reduce inflammation. They can improve conditions like acne, eczema, and rosacea.
These foods calm gut inflammation, which in turn improves skin clarity.
Omega-3 fatty acids reduce skin dryness and irritation while supporting gut function.
The gut-liver axis represents the bidirectional relationship between the gastrointestinal tract and the liver, primarily facilitated by the portal vein, which transports substances absorbed in the intestines directly to the liver.
This close anatomical and functional connection means that changes in the gut microbiome can significantly impact liver health.

A balanced gut microbiome plays a crucial role in maintaining liver function. Disruptions in this microbial community, known as dysbiosis, can lead to increased intestinal permeability, allowing bacteria and their by-products to enter the liver. This can trigger inflammation and contribute to various liver diseases, including:

A healthy gut means a healthier liver. The right foods can restore gut balance, support liver detox, and reduce inflammation.
These foods boost good gut bacteria, repair the gut lining, and enhance liver function:
These foods disrupt gut bacteria, damage the gut lining, and make the liver work harder:
Your gut health is the foundation of your overall well-being. The gut microbiome isn’t just about digestion- it’s deeply linked to your brain, skin, and liver health. A balanced gut keeps your mind sharp, your skin glowing, and your liver functioning at its best.
But when your gut health is compromised, it can lead to digestive issues, brain fog, acne, hormonal imbalances, and even liver problems.
So, if you’ve been struggling with bloating, poor digestion, skin breakouts, fatigue, or unexplained health issues, it’s time to look at the root cause- your gut. But now you can heal your gut and take control of your health!
We know how frustrating it can be to deal with digestive problems every day. The discomfort, the bloating, the unpredictable gut issues- it affects your energy, mood, and confidence.
But you don’t have to live like this. Healing your gut is possible, and that’s exactly what iThrive’s ALIVE 2.0 program is designed to do.
Your health is in your hands, and iThrive is here to guide you. If you’re tired of digestive discomfort, skin issues, low energy, and struggling to find answers, it’s time to take action.
Book a free consultation today and start your journey to better gut health! Let’s restore your gut microbiome and health so you can feel healthier, happier, and more alive than ever before!
.webp)




.svg)
Imagine taking your child for a routine check-up, only to hear that they have fatty liver disease. As a parent, it might be very shocking and overwhelming. But this is becoming a harsh reality for many parents today. Non-alcoholic fatty liver disease (NAFLD) in kids is rising at an alarming rate, making it one of the most common chronic liver diseases in children.
Why is this happening? The answer lies in our lifestyle. Excessive junk food consumption, lack of physical activity, and poor eating habits are leading causes of fatty liver in children. Today's kids consume more sugary drinks, processed foods, and unhealthy snacks than ever. Combine this with long hours of screen time and minimal exercise, and you have a perfect recipe for liver damage.
This blog will help you understand the causes of fatty liver in children, early warning signs, and how to prevent it. Let’s take action before it’s too late!
Fatty liver disease, medically known as steatotic liver disease (SLD), is characterised by excess fat accumulation in liver cells.
While it's normal for the liver to contain some fat, it signifies fatty liver disease when it comprises more than 5% to 10% of the liver's weight. This condition can impair liver function and lead to more severe liver complications if left unaddressed.1
Metabolic Dysfunction-Associated Steatotic Liver Disease (MASLD): Previously known as non-alcoholic fatty liver disease (NAFLD), MASLD occurs in individuals who consume little to no alcohol. It's often associated with metabolic conditions such as obesity and type 2 diabetes.2
NAFLD has become the most common liver disease among children and adolescents globally. Studies estimate that it affects approximately 7.6% of the general pediatric population. However, the prevalence rises dramatically among obese children, with over 30% affected.3
A systematic review and meta-analysis highlighted that the prevalence of NAFLD in children and adolescents has increased from 19.34 million in 1990 to 29.49 million in 2017, representing an annual increase of 1.35% regardless of sex, age, or region.
In India, the prevalence of pediatric NAFLD is alarmingly high. A study found that about one in three (35%) suffer from metabolic dysfunction-associated steatotic liver disease (MASLD), the updated term for NAFLD in children.
Further research indicates that the prevalence of fatty liver among overweight children in India is 45.6%, nearly double that of normal-weight children at 18.9%. The prevalence increases with age, from 13.1% in 5-6-year-olds to 31% in 9-10-year-olds.4
Data on hospitalization rates for pediatric NAFLD are limited. However, a study analyzing data from 2009 to 2018 revealed that the incidence of NAFLD diagnoses in children aged 9 to 18 increased from 36.0 per 100,000 in 2009 to 58.2 per 100,000 in 2018. This significant rise underscores the growing burden of NAFLD among the pediatric population.

As a parent, you want the best for your child, including their health. But did you know that an unhealthy diet and lack of movement can put your child at serious risk for fatty liver in children? Let’s explore the major causes of fatty liver in children and what you can do to prevent it.
If your child is overweight, their liver may already be struggling. Excess fat in the body leads to fat accumulation in the liver, causing NAFLD in kids. Studies show that overweight children are much more likely to develop fatty liver disease than those with a healthy weight.
If your child loves fast food, soda, and processed snacks, their liver could be suffering. The modern diet is loaded with unhealthy fats, sugars, and additives that make fatty liver in children worse.
Does your child spend hours on the phone, gaming, or watching TV? A sedentary lifestyle and liver disease go hand in hand. Lack of movement slows down metabolism, making fat accumulate in the liver.
If fatty liver, diabetes, or metabolic disorders run in your family, your child could be at higher risk. Genetics play a role in how the body processes fat, making some children more prone to NAFLD in kids.

In the initial phases, NAFLD typically presents no noticeable symptoms. This silent progression makes early diagnosis challenging.
As fatty liver disease advances, certain signs may emerge, including:
In more severe cases, children might experience:

A balanced, nutrient-rich diet is fundamental in managing fatty liver disease. Encourage your child to consume:
Certain foods can promote inflammation and worsen liver health. It's advisable to avoid:
Physical activity helps reduce liver fat and improves overall metabolic health. Aim for at least 30 minutes of moderate exercise most days of the week. Encourage activities your child enjoys, such as:
Achieving and maintaining a healthy weight is crucial. Gradual weight loss, through a combination of diet and exercise, can reduce liver fat and inflammation. Consult with a functional nutrionist to set realistic weight goals for your child.
Quality sleep is vital for metabolic health. Establish a consistent sleep schedule, aiming for 8-10 hours per night, depending on your child's age.
Chronic stress can negatively impact liver health. Teach your child stress-reducing techniques such as:
Reducing sedentary activities like excessive screen time encourages more physical movement and reduces the risk of obesity. Set reasonable limits on screen time and promote active play.
Regular visits to your child's healthcare provider are essential to monitor liver health and adjust care plans as needed. Early detection of changes can prevent progression to more severe conditions.
As a parent, nothing is more important than your child’s health. The rise of fatty liver in children is alarming, but it’s preventable! By reducing junk food and fatty liver risks, encouraging active play, and choosing whole, nutritious foods, you can protect your child from non-alcoholic fatty liver disease (NAFLD) in kids. Don’t let a sedentary lifestyle and liver disease steal their health. Small changes today can mean a healthier future.
.webp)



.svg)
Maida, also known as refined flour or all-purpose flour, is a common ingredient in Indian cooking, found in everything from rotis and snacks to biscuits, pizzas, and pastries. It is made by stripping wheat of its bran and germ, leaving behind only the starchy part. Since maida has a naturally yellowish color, it is often treated with chemicals to make it appear bright white and more appealing. 1
While maida makes food soft and tasty, the refining process removes all its nutrients, making it low in fiber, vitamins, and minerals. 2 It is also a rich source of gluten, the main storage protein in wheat. While gluten helps give dough its stretchy texture, it has been linked to various health concerns, especially for those with sensitivities. 3
Because of this, regular consumption of maida may not be the best choice for overall health. Let's explore how it affects the body and why switching to healthier alternatives can make a big difference!
Maida is made by removing the bran and germ, leaving only the starchy part of the wheat grain. This makes it high in starch, low in fiber, and a high-glycemic food. Eating maida causes rapid spikes in blood sugar levels, leading to blood sugar crashes that make you feel tired and hungry soon after. Over time, these constant fluctuations can increase insulin resistance, making it harder for your body to control blood sugar, which is a major risk factor for Type 2 diabetes and heart disease. 4
Refined carbohydrates like maida are quickly digested, leading to sudden hunger and cravings shortly after eating. This can make you eat more, leading to overeating and weight gain. Maida-based foods like white bread, biscuits, and pastries also lack fiber, which means they don’t keep you full for long. 5 Plus, processed foods with maida can trigger leptin resistance, making it harder for your brain to recognize when you’re full. This leads to uncontrolled appetite and obesity over time. 6, 7
The shift from traditional fiber-rich Indian foods to a Western-style diet high in maida and refined carbs has damaged gut health. These processed foods lack prebiotic fiber, which is essential for good gut bacteria. A poor gut microbiome leads to gut inflammation, bloating, acidity, and digestive issues. Over time, this can contribute to chronic gut problems and weakened immunity. 8, 9
Maida is stripped of fiber, vitamins, and essential nutrients, making it an empty calorie food. This lack of fiber plays a big role in raising bad cholesterol (LDL), increasing inflammation, and causing insulin resistance—all of which are major risk factors for heart disease. Studies show that replacing refined grains with whole grains can lower cholesterol, improve blood circulation, and protect the heart. 10, 11
Eating too much maida can lead to frequent blood sugar spikes, which trigger oxidative stress, inflammation, and insulin resistance—all of which contribute to high blood pressure. 12 Excess insulin further worsens the situation by making the kidneys retain more salt and water, causing fluid buildup that raises blood pressure. It also overactivates the nervous system, tightening blood vessels and making it harder for blood to flow smoothly. 13 Over time, these effects increase the risk of hypertension and heart problems. This is why people who consume a diet high in refined carbs like maida are more likely to struggle with blood pressure issues. 12
PCOS, a common hormonal disorder in women of reproductive age, affects many Indian women. One major factor is the consumption of refined carbohydrates, which have a high glycemic index (GI) and glycemic load (GL) but lack fiber. 14 These diets are linked to PCOS and insulin resistance, which often go hand in hand. 15
7. Acne
A diet high in sugar and refined grains (common in the Western diet) can worsen acne by quickly raising blood sugar levels. This increases insulin and IGF-1, which trigger excess oil production and boost hormones that lead to breakouts. 16
By now, it’s clear that maida doesn’t just add fluffiness to your favorite foods—it also strips away essential nutrients and harms your health in multiple ways.
That’s why switching to complex carbohydrates is a smarter choice. Whole grains like millets, quinoa, and brown rice, along with fiber-rich legumes and vegetables, provide slow-releasing energy, keep blood sugar stable, and support a healthy gut microbiome.
By making this simple switch, you’re not just avoiding the harmful effects of maida but also setting the foundation for long-term health and wellness. Small dietary changes can make a big impact—so why not start today?




.svg)
We all know that excessive drinking can harm the liver, but did you know that alcohol and cancer risk go far beyond that? Most people only associate alcohol and liver cancer, but research shows that alcohol consumption is also linked to breast cancer, colorectal cancer, head and neck cancers, and esophageal cancer. The real question is: does alcohol cause cancer? Science says yes, and even small amounts can increase your risk.
India is the world’s third-largest market for alcoholic beverages, valued at a staggering $35 billion, and the industry is only growing. The spirit segment (whisky, rum, etc.) reached $41 billion by 2022. But with increasing alcohol consumption, are we also seeing a rise in cancer cases?1
In this blog, we’ll explore the hidden dangers of alcohol, how it contributes to different types of cancers beyond the liver, and what you need to know to protect yourself. If you think moderate drinking is safe, you might want to read this till the end!

India is drinking more than ever before. From social gatherings to casual evenings, alcohol has become a regular part of urban and rural lifestyles. But have you ever wondered why alcohol consumption is rising so rapidly? Is it just about celebrations, or is there something deeper at play?
A 2019 government survey found that one in seven Indians between 10-75 years old consumes alcohol- a number that keeps growing. The reasons? 2
While beer and wine are gaining popularity, Indians still love their whisky, rum, and vodka. The country remains one of the world’s largest whisky consumers! 2

Did you know that in 2020 alone, 40,000 new breast cancer cases were caused by alcohol in this region? Even more alarming, globally, breast cancer is now the most common cancer. Over 2 million cases were diagnosed in 2020, and 100,000 of those were directly linked to alcohol consumption.3
But here’s the worst part- many women don’t even know alcohol causes breast cancer. That’s right! It’s not just genetics or lifestyle but something as simple as that glass of wine or beer you enjoy after work.
Colorectal cancer (CRC) is the third most common cancer in men and the second most common in women worldwide.4
Alcohol plays a major role in increasing the risk of colorectal cancer. It disrupts gut health, damages DNA, and promotes inflammation- creating the perfect environment for cancer to grow.
If you drink regularly, your risk of colorectal cancer skyrockets. Is that extra drink really worth the risk?
If you think moderate drinking (one drink per day) is safe, think again! Research shows that even people who drink occasionally have a higher risk of head and neck cancer. 5
Head and neck cancers affect your mouth, throat, and voice box, making eating, drinking, and even speaking difficult. If you drink regularly, you’re feeding cancer without even realising it.
Esophageal cancer is the 7th most common cancer worldwide and the 6th leading cause of cancer-related deaths.6
One of the biggest risk factors? Alcohol.
It damages the cells lining your esophagus, increasing the risk of squamous cell carcinoma, a deadly type of esophageal cancer. Regions from China to the Middle East are known as the "Esophageal Cancer Belt" because of their high alcohol consumption.
Alcohol, combined with tobacco, makes things even worse. If you smoke and drink, your risk of esophageal cancer multiplies!

When you drink alcohol, your body breaks it down into acetaldehyde, a toxic chemical that directly damages DNA and prevents your body from repairing itself. Acetaldehyde is a known carcinogen, meaning it can cause cancer. This substance accumulates in your liver, mouth, throat, and even your gut, increasing the risk of several cancers.
Acetaldehyde is not just produced inside your body- it can also come from bacteria in your mouth and gut. Poor oral hygiene and smoking increase this buildup, making the risk even worse. Studies show that alcohol drinkers who also smoke have a significantly higher chance of developing esophageal and oral cancers.7
Certain alcoholic drinks like calvados (a type of brandy) naturally contain acetaldehyde, increasing your exposure even before alcohol is metabolized in your body.
Every sip of alcohol triggers oxidative stress- a process that releases harmful molecules called reactive oxygen species (ROS). These molecules damage your cells, cause inflammation, and contribute to cancer growth. When oxidative stress is combined with acetaldehyde exposure, it creates the perfect storm for cancer to develop.
Studies show that chronic alcohol consumption weakens the body's ability to fight free radicals, leaving you vulnerable to diseases like cancer.8
Alcohol increases estrogen levels, which is directly linked to a higher risk of breast cancer. Research shows that women who drink just three alcoholic beverages per week have a 15% higher chance of developing breast cancer. If you drink daily, this risk jumps even higher.
For women, alcohol can be more dangerous than they realize. Even if you don’t drink heavily, the risk of hormone-related cancers goes up.
Not everyone’s body processes alcohol the same way. Your genes determine how efficiently your body breaks down alcohol, and for some people, the process is far more dangerous.9
The link between alcohol and cancer risk goes far beyond just liver damage. Yet, many people remain unaware of this silent danger. Cutting down or eliminating alcohol can significantly reduce your cancer risk and improve your overall health. Small lifestyle changes today can protect you from severe health issues tomorrow. Your health is in your hands. Don't let a habit dictate your future. Choose awareness over ignorance. Choose health over harm. It's time to take control- because every sip counts!




.svg)
Insulin is a vital hormone in the body that helps regulate blood sugar levels. When you eat food, your body converts carbs into glucose (sugar) that goes into the bloodstream. The pancreas responds by secreting insulin, which assists with bringing this glucose into your cells, especially into muscles, fat, and the liver to utilize as energy or store for future use. It helps in maintaining normal blood sugar levels and keeps them from experiencing hazardous spikes or drops.
Insulin resistance is when the cells of the body are no longer responding to insulin. This results in glucose not being able to enter the cells, so the pancreas secretes more insulin to make up for this. Although this can maintain normal blood sugar levels for a while, overproduction of insulin will ultimately cause high blood sugar levels, which can then advance to prediabetes and type 2 diabetes if not treated.

While scientists continue to discover the specific causes of insulin resistance, they have determined that there are several factors that contribute to it:

In most cases, individuals with insulin resistance or prediabetes will not feel symptoms. Some warning signs might signal a problem:
Unattended insulin resistance has more severe long-term effects that include:

Insulin resistance is treatable, and in most instances, reversible with lifestyle modification. Here's what you can do:-
Eat a Healthy Diet: A diet composed of whole, unprocessed foods can greatly enhance insulin sensitivity. Consider adding:
Stay away from refined carbohydrates, processed foods, and trans fats, which aggravate insulin resistance.
Exercise daily: Exercise helps maintain insulin sensitivity. Aerobic exercise (brisk walking, jogging and cycling) and resistance exercise (weightlifting, bodybuilding) help muscle cells uptake glucose better.
Control Stress and Sleep Quality: Practicing stress-reducing activities like yoga, meditation, and deep breathing can improve insulin function. Additionally, aim for 7-9 hours of quality sleep each night to support metabolic health.
Quit Alcohol and Smoking: Quitting alcohol and smoking can reduce inflammation and improve insulin sensitivity over time.
Regular Health Checkups: Monitoring your blood sugar levels through routine checkups can help detect insulin resistance early, allowing for proactive intervention.
Insulin resistance is a quiet disease that has serious long-term health effects if it's not treated. But by taking a healthier lifestyle, being active, and eating diligently, you can take away most of your risk and feel better overall. If you're wondering if you have insulin resistance or have already been detected with insulin resistance and want the right support, Book a free consultation with iThrive. At iThrive, we aim to reverse chronic diseases by treating the root causes of health issues and suggesting personalised and long-lasting solutions.



The blog covers functional nutrition, chronic conditions, gut health, hormonal health, autoimmune conditions, sleep, mental health, and root cause analysis. Every article is written to help you understand what is actually happening inside your body, not just manage symptoms.

All articles are written by the content writers in collaboration with iThrive's clinical team of functional nutritionists, guided by the same methodology used in the ALIVE programme. The content is rooted in functional medicine and real clinical experience, not generic health advice.

No. The blog is an educational resource to help you understand your health more deeply. If you are experiencing symptoms or managing a chronic condition, a personalized Root Cause Analysis with a functional nutritionist is the right next step.

Book a Root Cause Analysis. For ₹2,500, a dedicated functional nutritionist will assess 60+ blood markers using optimal ranges and explain exactly what is driving your condition. It is the natural next step after reading about what might be happening in your body.

Yes. Many of our readers come with existing diagnoses and find the blog helps them understand why their condition developed and what their body actually needs. The articles are designed to give you clarity, not replace the guidance of a practitioner.



