



.svg)




.svg)
Vitamin D is essential for the intestinal absorption of calcium and phosphorus. These are minerals that are crucial for bone mineralization and remodelling. Without sufficient vitamin D, calcium absorption is impaired, leading to lower blood calcium levels, which in turn stimulates parathyroid hormone (PTH) release. Elevated PTH can cause bone resorption, weakening the skeletal structure over time. In children, vitamin D deficiency leads to rickets, characterized by soft, weak bones, skeletal deformities, and growth retardation. In adults deficiency can lead to osteomalacia (softening of bones) and contribute to osteoporosis, increasing fracture risk.
Vitamin D receptors (VDRs) are found on various of your immune cells, including T cells, B cells, and macrophages. These special immune cells fight off infections and control inflammation. These cells have "locks" (receptors) that vitamin D acts like a "key" for. When vitamin D is present, it helps these cells work better at fighting harmful germs and reduces unnecessary inflammation, keeping your immune system balanced and effective. Insufficient vitamin D status has been associated with an increased susceptibility to infections, including respiratory tract infections, and may influence the risk of autoimmune diseases.
Vitamin D receptors are widely distributed in brain regions that regulate mood and behaviour. Low levels of vitamin D have been repeatedly associated with an increased risk of depression and other mood disorders. A deficiency in vitamin D may contribute to or worsen depressive symptoms and has been linked to other mental health challenges.
Vitamin D is important for muscle function and overall energy metabolism. It supports muscle strength and performance, which in turn can help reduce feelings of fatigue. Inadequate vitamin D can lead to muscle weakness and general fatigue, impairing daily physical activities and overall energy levels.
Vitamin D plays a role in maintaining vascular health (the health of blood vessels) by supporting endothelial function. Good vascular health is essential for sexual function, particularly in men, as it aids in the regulation of blood flow necessary for erectile function. A deficiency in Vitamin D may contribute to suboptimal vascular function and hormonal imbalances, potentially increasing the risk of sexual dysfunction.
Vitamin K2‐MK7 helps keep your bones strong by activating a protein called osteocalcin, which makes sure that calcium is used to build and strengthen bones. This is especially important for older adults, like postmenopausal women, who are more at risk for fractures. At the same time, it activates another protein called Matrix Gla protein (MGP), which stops calcium from building up in your blood vessels, thus helping to keep your heart and arteries healthy.
Not getting enough Vitamin K2‐MK7 can mean your body doesn’t use calcium as well as it should. This can lead to weaker bones, increasing the risk of osteoporosis and fractures.
In conclusion, Vitamin D3 and Vitamin K2‐MK7 work together to ensure that calcium is used properly in the body. Vitamin D3 boosts the absorption of calcium from your diet, and Vitamin K2‐MK7 then directs that calcium to your bones, helping to strengthen them while keeping it from building up in your arteries. So taking both vitamins together can improve bone health and support heart health better than taking either one alone.





.svg)
Among carbohydrates, fats, and proteins, protein is one of the three primary macronutrients necessary for life and healthy living. In its simplest form, a protein is defined as a sequence of amino acids, which are organic molecules containing nitrogen, carbon, hydrogen and oxygen. Any protein is broken into amino acids during digestion which are categorized into 20 known types: nine essential (cannot be synthesized by the body) and 11 non-essential (our body makes them from other compounds).
As the amino acids undergo recombination, they undertake various biological functions. This means that each protein is vital to a wide range of bodily physiological functions and processes, making it fundamental for the delivering organizing nutrition concept which shifts the focus from the essential food nutrients balance toward optimizing functional systems of the body while supporting health, balance, and energy.
Protein supports the repair and growth of tissues in the body as it forms the base for such activities. Our human body is always experiencing the changes in cells, and protein is important to ensure that this continues to happen. After performing physical exercise, the muscle tissue especially goes through a process of breaking down and rebuilding which is referred to as muscle protein turnover. The new proteins that come from dietary protein are used for repairing the damaged tissue and aid in muscle growth, which is referred to as hypertrophy. Such processes are influenced by various signals such as after performing exercises or having nutrients, especially the case when one eats after strength workouts or endurance activities.
Different biochemical reactions are exercised with the aid of proteins that take its initial form as the aid in digestion of insulin, a protein released by the pancreas is known to be the hormone responsible for glucose metabolism. Metabolism is the set of life-sustaining chemical transformations within the cells of organisms, also have other proteins ( amylase, lipase and kinase ) serving as the main operator. As well known, waste from cells must be eliminated which is where the rest of the proteins turned to be an enzyme, acting as the executor of protease. All of these biochemical activities aid in sustaining the body and it’s efficient performance.
The immune system heavily depends upon proteins for its functioning. Antibodies or immunoglobulins, are special types of proteins that get attached to the antigens like viruses or bacteria and get produced by the B lymphocyte. Their function is to destroy both the virus and bacteria. Furthermore, they were cut out. These immune responses are regulated by certain protein based molecules called cytokines, which regulate inflammation and immune cells signaling cytokines. These proteins are needed for both primary and secondary immunodeficiency, defending the patient against germs.
Cellular structures are largely made of proteins. Protein filaments make up the cell shape and structure with the cytoskeleton. Moreover, maintaining the tissue’s integrity and elasticity is also provided with structural protein collagen found in connective tissue skin, tendons and cartilage, and keratin which is found in hair and nails. While certain macro and micro-structural proteins, along with carbohydrates form the tissue and cell architecture, these structural integrally polysaccharides also allow the cells to communicate and signal one another in the extracellular matrix.
Proteins serve as carriers and transporters of various molecules throughout the body. Hemoglobin, a protein in red blood cells, binds and transports oxygen from the lungs to tissues and organs. Similarly, transferrin transports iron, and lipoproteins transport lipids (fats) in the bloodstream. Proteins also serve as storage molecules for certain nutrients, such as ferritin, which stores iron in the liver and spleen, ensuring its availability when needed.
Proteins are not the primary source of energy for the body and do not store starch and fat. In case of an emergency, they may be utilized as an energy substrate. During a fast or extensive games or exercises, protein are catabolized into amino acids, which are later transformed into glucose through gluconeogenesis to satisfy the energetic requirements. This is much more costly in energy than carbohydrates and fat, but is extremely important during periods of malnutrition.
Certain proteins, in particular albumin in blood plasma, have a significant role in regulating fluid balance, and osmotic pressure. The water of the body compartments by oncotic pressure in blood vessels. This assists in averting the buildup of excessive fluid in body tissues, a condition called edema. Besides in cell membranes, proteins also regulate the flow of electrolytes which aid in neuron and muscle function.
Protein consumptions create a feeling of fullness and assist in weight management, which is essentially called as having a “high satiety value.” This occurs because of the slow digestion of protein compared to carbohydrates. It helps manage hunger hormones such as leptin and Ghrelin. It is also a well-known fact that protein has a higher thermic effect on food
Therefore, protein is undoubtedly a key to staying at the peak of health and well-being. From aiding muscle growth and repair to enhancing immune function and healthy skin, its uses are enormous. Getting a sufficient amount of protein from a healthy diet can enhance energy, physical performance, and overall long-term health. No matter if you are an athlete, a working professional, or someone who just wants to live healthier, making protein a priority in your diet is a wise and essential decision for overall wellness.




.svg)
For most of us, the bathroom has become a second home in our digital lives. Swiping through social media, messaging back, or watching videos while sitting on the toilet has become second nature. But what appears to be harmless might be compromising your health at a very high price.
Medical experts are alarmed at the number of cases involving hemorrhoids and anal fistulas, which are conditions linked with prolonged sitting on the toilet seat. Although diet, water intake, and exercise each have significant implications for gastrointestinal functioning, studies now suggest that prolonged phone use on the toilet could be one of the primary causes of such agonizing illness.
In this blog, we will discuss the risks of prolonged toilet time, how it contributes to hemorrhoids and other anal conditions, and what you can do to avoid these health dangers.

Let's first see why people take their phones into the bathroom in the first place.
While these reasons may seem harmless, the physical consequences of excessive toilet time can be far from trivial.

The human body is not meant to sit on a toilet seat for long. Compared to sitting on a normal chair, sitting on a toilet applies unnecessary pressure to the rectal veins, resulting in inflammation and severe medical issues.
Hemorrhoids arise when the rectal and anal veins become swollen as a result of too much pressure. This condition may result in:
Prolonged periods on the toilet make people more prone to hemorrhoids as gravity and seated pressure stop the proper circulation of the blood, making the veins congested.
Anal fistulas are infected tracts that develop between the anus and the overlying skin, usually due to untreated abscesses. They may produce:
Prolonged toilet time leads to fistula development by exposing bacteria and straining.
Excessive toilet sitting breaks the normal urge to have a bowel movement, leading to irregular bowel habits. This leads to constipation and straining, which in turn increases the possibility of anal disorders.
Apart from hemorrhoids and anal fistulas, long-term sitting on the toilet has other serious risks:
Now that you are aware of the risks, here's how to make healthier choices:

Your bathroom is not a living room, and your phone should not be your bathroom friend. Regular sitting, combined with too much phone use, greatly raises the risk of hemorrhoids, anal fistulas, and other gastrointestinal issues. Shaking this habit will require some effort, but taking care of your health over a few extra minutes of scrolling is worth it.
So, the next time you grab your phone in the bathroom, ask yourself: Is it worth the risk?
If you are in any of the situations like hemorrhoids or other gastrointestinal problems, you can book a free consultation with iThrive. At iThrive we help you reverse chronic diseases with a functional nutrition approach by treating the root causes of your issues with the right diet, supplementation, and personalised care.




.svg)
The thyroid, a small butterfly-shaped gland in your neck, plays a massive role in regulating the body’s metabolism, energy levels, mood, and overall well-being. When it malfunctions, whether it's hypothyroidism (underactive) or hyperthyroidism (overactive), the impact can be significant. But what if you could address the root causes of thyroid dysfunction through targeted nutrition? That's where functional nutrition for thyroid health comes in. If you are struggling with thyroid issues try booking a free consult with iThrive and get a lasting solutions to reverse your disease.
Practitioners often focus on managing thyroid hormone levels with medication. While this is important, healing thyroid dysfunction ( hypothyroid, hyperthyroid, or Thyroid hormone insufficiency ) naturally requires a deep dive. Functional nutrition takes a holistic approach, recognizing that thyroid health is interconnected with various systems in the body, including the gut, immune system, and adrenal glands. Therefore, understanding the root cause becomes the primary focus to treat any Thyroid Disorders.

Functional nutrition swoops in like a detective, figuring out what’s off and fixing it with real and everyday choices.

Food’s huge, but it’s not the whole story. Lifestyle habits are equally important, like stress, sleep, and movement, are thyroid sidekicks:

By adopting a functional nutrition approach, you can take control of your thyroid health and empower yourself to live a vibrant and fulfilling life. Remember, nutrition and thyroid balance is a journey, therefore Key to the victory is : Be patient, consistent, and celebrate the small victories along the way.




.svg)
Aging is a natural and multifaceted process controlled by both genetics and the environment. While we cannot control our genes, we can certainly make choices that impact how we age. Lifestyle factors such as diet, physical activity, exposure to toxins, and stress levels play a significant role in determining our overall health as we grow older. One of the most crucial aspects of healthy aging is ensuring that our bodies receive adequate nutrition to maintain functionality and prevent decline.
If you're unsure about nutritional needs for seniors, iThrive provides a free consultation to enlighten you about your body's needs and set you on the path to maximum health. Schedule a free consultation today!
When addressing aging, it is essential to focus on the years before we would traditionally consider ourselves "aged." Typically, the late 40s to early 60s are crucial decades where lifestyle choices significantly impact how we age in our 70s and 80s. Although our body habits during the 20s and 30s do bear some influence, it is specifically in these 20 years that we should primarily focus on supporting the optimal level of functioning for the body.
Aging basically is a smooth progression toward, ultimately, complete body shutdown. Tissues start to deteriorate, and different systems in the body start malfunctioning. But with specific interventions, we can retard this process and keep our physiological systems functional for a longer period. Most individuals are able to keep their bodies functional until the age of 60, but thereafter, the deterioration tends to happen very fast. The secret to aging well is to keep the functionality of essential systems in the body intact.
As we grow older, our bodies also experience a number of physiological changes that influence the way we absorb and utilize nutrients. This implies that even though our nutritional needs do not change or may even be higher, our capacity for nutrient absorption and utilization tends to reduce.

The immune response declines with age, rendering older adults vulnerable to infections and chronic inflammation. Key nutrients like B-complex vitamins, zinc, vitamin D, magnesium, and iron are important for immune support. Adequate intake of high-quality protein is also important to preserve immune integrity.
For optimal immune support, use iThrive Essentials Zinc Defense and Vitamin D3 K2, which are formulated to support immunity strengthening.
Aging contributes to progressive muscle mass and bone loss, thereby leading to fracture risk and osteoporosis. Some of the key nutrients for building strong bones and muscles include calcium, protein, iron, magnesium, and vitamin D. Sustained strength training and weight-bearing activity are capable of arresting muscle wasting and enhancing bone integrity.
If you're in need of targeted support, iThrive Essentials Magnesium, Vitamin D3 K2 and EAA Protein Support are great additions to your regimen for bone and muscle health.
With age, the blood vessels and the heart stiffen, thus contributing to arterial stiffness and developing a higher chance of heart disease. Antioxidants like vitamins E and C protect against oxidative stress, and omega-3 fatty acids play a beneficial role in maintaining a healthy heart. Whole foods, fiber, and good fats comprise the best diet for elders and reduce chances of cardiovascular diseases.
If you wish to improve cardiovascular health, iThrive Essentials CoQ10 is a potent supplement that supports cardiovascular health and energy production in elderly individuals.
Cognitive impairment, such as decreased processing ability and memory loss, are hallmarks of aging. Essential nutrients like B vitamins (B1, B6), omega-3 fatty acids, and antioxidants support maintaining brain function and preventing neurodegenerative disease.
For brain and energy supplementation, try iThrive Essentials B-Complex for necessary nutrients for cognitive function and general health.
Aging tends to result in decreased gut motility and lower digestive efficiency, which makes it more difficult to absorb essential nutrients such as protein, iron, and calcium. Fiber intake from foods, probiotics, and digestive enzymes can enhance nutrient absorption and overall health. Fermented foods like yogurt, kefir, and kimchi can help promote a healthy balance of gut microbiome.

Medical conditions such as osteoporosis, arthritis, and heart disease are caused by a combination of genetic factors and environmental factors. For example, osteoporosis may be caused by diet that is low in protein and calcium, added to menopause in women when estrogen decreases, causing the loss of bone. Thus, genetics and environmental factors, including diet and hormonal fluctuations, are a major contributor to the causation of these diseases.
Boost calcium and vitamin D consumption through diet and supplements if necessary. Weight-bearing exercises support bone density. Good quality protein consumption is important to maintain bone and muscle strength.
Eat anti-inflammatory foods with omega-3 fatty acids, including fatty fish, and supplements such as krill oil. Turmeric and ginger possess natural anti-inflammatory effects that minimize joint pain. Processed foods and high sugar intake must be avoided since they can intensify inflammation.
Emphasize heart-healthy fats in the form of butter, ghee, fatty fish, and avocados. Decrease refined sugar, processed foods, and trans fats to reduce inflammation and enhance cardiovascular function. Add fiber-rich foods like whole grains, legumes, and vegetables to maintain heart health.
Dehydration plays a major role in the aging process, with most practitioners claiming that it is one of the main causes that speed up aging. Hydration is important since our bodies contain a high percentage of water, and poor hydration can cause cellular dehydration. Cellular dehydration can greatly speed up aging, such that an individual in their 50s biologically can look like someone much older, say in their 70s, because of the negative effects of dehydration.

In addition to adequate nutrition and hydration for older adults, the following lifestyle habits can also enhance the normal aging process:
We all age, but we can control how we age. By choosing the best diet for older people, controlling inflammation, drinking enough water, and maintaining vital bodily functions, we can improve our health and vitality well into our older years. The secret is to take early action in middle age to promote a healthy and easy aging process so that we can live life with strength and resilience.
If you are looking for information about your elderly nutrition requirements, schedule a free consultation with iThrive today!




.svg)
Ozempic, or the weight loss drug, as you might have heard, has taken everyone by storm! The brand name for semaglutide, is all over social media and is currently the talk of town. The drug was originally developed as a treatment for Type 2 Diabetes. However, its side effect of weight loss has garnered more attention than its actual use. The tiktokers, influencers and pop culture are raving about Ozempic without completely understanding it! Is it really the miracle it claims to be or are we missing the wider picture? Let’s have a closer look at it and decode everything you need to know about Ozempic.
.webp)
Ozempic is the brand name for the drug ‘semaglutide’. It belongs to the class of GLP-1 (glucagon- like- peptide-1) drugs. Ozempic is an injection that needs to be taken on a weekly basis for managing diabetes. It helps to lower the blood sugar levels by helping the pancreas to make more insulin. However, this is not the only effect it has. Like most of the drugs, Ozempic also has side effects. The one that is being masked as a use of this drug is ‘weight loss’. When a person is on Ozempic, their appetite decreases and the process of digestion slows down. This is because Ozempic works by mimicking the GLP-1 hormone in our body.
The most common misconception people have about this drug is that they think getting on Ozempic is all that they need. People report significant weight loss with little effort. Sounds like a dream, doesn’t it?? But, there is more to it than that.
The weight loss effects of Ozempic are not permanent. Once you stop taking Ozempic, the weight loss stops. Moreover, the lost weight is gained back and in some cases, more quickly than it was lost. Ozempic is just a short term fix for obesity. This does more harm than good. The user starts relying on the medicine. Once the drug is stopped, the user finds it very difficult to maintain the weight since it requires major lifestyle changes. Now, since the person is dependent on Ozempic, it is more likely that they won’t follow the required lifestyle changes for maintaining weight. This has more to do with the user’s psychology. The medicine makes the process of weight loss look very simple when it is actually not.
.webp)
Not many people are aware of the fact that Ozempic comes with a boxed warning in the USA. A boxed warning, also known as, Black Box Warning, is the strictest warning the U.S. Food and Drug Administration can issue. A boxed warning implies that the medicine might have serious side effects. This itself tells a lot about the seriousness of adverse effects that the drug might have. The most important fact is that Ozempic is not approved for weight loss by the FDA.
Apart from the milder side effects like nausea, vomiting, diarrhea, abdominal pain, Ozempic has potential serious side effects like pancreatitis, diabetic retinopathy, gall bladder disease, hypoglycemia, thyroid cancer and kidney problems. While these side effects are not universal, it demands serious consideration before starting the drug, especially the ones with pre-existing health conditions. The boxed warning on the drug is regarding the risk of thyroid cancer, raising concern about its long term use.
Ozempic and other weight loss medications have given rise to a quick fix mentality. People have started seeing treatment of obesity as a quick fix rather than a lasting lifestyle change. This is concerning on many levels since it completely ignores addressing the root cause of obesity and metabolic diseases. Treatment of a complex disease like obesity cannot be done solely by a drug. With a continuous rise in obesity across the globe, people are getting into this short-cut trap. A pill can never be the answer for any disease, let alone a highly complex problem like obesity.
The fact that people are now referring to Ozempic as a weight loss drug and not a Diabetes drug is a reflection of people’s inclination towards rapid results, which is definitely not a healthy choice.
As many other conventional treatments, Ozempic is not for a common man. Since the generic versions of this drug are not available at the moment, the cost is much higher. The drug can cost anywhere around $800 to $1000 per month. Keeping in mind that it is required to take these medicines for a long period of time, it is not an affordable option. Moreover, since the effects last only as long as the person is on the drug, it can hardly be counted as an investment into better health. The danger of side effects makes Ozempic an expensive affair, not only money wise but health wise as well.
Ozempic is just a very small part of the ‘weight loss quick fix’ picture. There are other such drugs that have now started attracting a lot of eyeballs. People are convincing their healthcare providers to prescribe them the ‘magic weight loss’ pills. It is just a matter of time that the patent for these branded drugs will expire and the medicines will be available at reduced costs. Having said that, the price that people will pay in the long term needs to be assessed before opting for these medicines.
One of the most concerning things about Ozempic is the lack of data on long term use of these drugs. While they may show quick results, research on when to stop the medicines is insufficient, especially for the people that are consuming these drugs solely for cosmetic purposes. The healthcare professionals say that these weight loss drugs alone are not enough for losing weight. The user has to consider lifestyle changes as well. However, since the pills show quick effects, people are under the impression that it is only due to medicines. When such users stop taking medicines, they gain the lost weight because they get so used to the pills that the body does not respond to lifestyle changes as quickly as they want them to. This effect is known as the Ozempic rebound and it still needs to be researched.
Given the high-profile nature of the drug, more research is definitely in the pipeline. However, until the long-term effects of the drug are better understood, the users are in a way subjecting themselves for a large-scale clinical trial. For all the people that are blatantly using Ozempic and other such drugs, the risk may not be worth it, especially when there are more long lasting and safer ways to manage weight.
While Ozempic may offer rapid results, it can never match a well rounded holistic approach. It is important to know that working on a highly complex chronic disease like weight loss, or any other chronic disease for that matter is a marathon and not a sprint. Medicines can never be a replacement to a well rounded holistic approach supported with right guidance and lifestyle changes. As the popularity of quick fixes continues to grow, one should always remember that no drug can solve any chronic disease without addressing its root causes.




.svg)
Inflammatory Bowel Disease (IBD) is now a significant global health concern, affecting over 0.3% of the world’s population. Among its types, Ulcerative Colitis (UC) is rapidly emerging as a major health challenge. While the prevalence of IBD in India may be lower compared to Western countries, the sheer size of India’s population means that millions are now struggling with Ulcerative Colitis symptoms and its impact on daily life. Many patients face a critical crossroads in their healthcare journey when conventional treatments start losing their effectiveness.1
For those battling ulcerative colitis, the decision about surgery might be the last step. However, did you know that functional treatment can be a better alternative for this? How? This comprehensive guide will explore the complex decision-making process surrounding ulcerative colitis and how functional nutrition can be a great choice.
Recent studies analyzing global health data have shown a sharp increase in IBD cases over the past three decades. Between 1990 and 2019, the number of people living with IBD jumped from 3.3 million to 4.9 million. China now has the highest number of cases, followed by the United States. While some countries have seen a plateau in cases, newly industrialized nations, including India are experiencing a rise in Ulcerative Colitis cases. 1
The latest data estimates that there are 2.7 lakh IBD patients in India, up from 1.3 lakh in 1990. However, clinical observations suggest that the real number may be much higher. Some earlier studies estimated that 1.4 million people in India were affected by IBD in 2010, placing India second only to the United States in terms of disease burden.1
Ulcerative Colitis is a chronic inflammatory bowel disease (IBD) that affects the colon and rectum. This condition causes inflammation and painful ulcers in your large intestine, leading to discomfort and digestive issues. Unlike sudden illnesses, Ulcerative Colitis develops gradually, often making it difficult to pinpoint when the symptoms started.

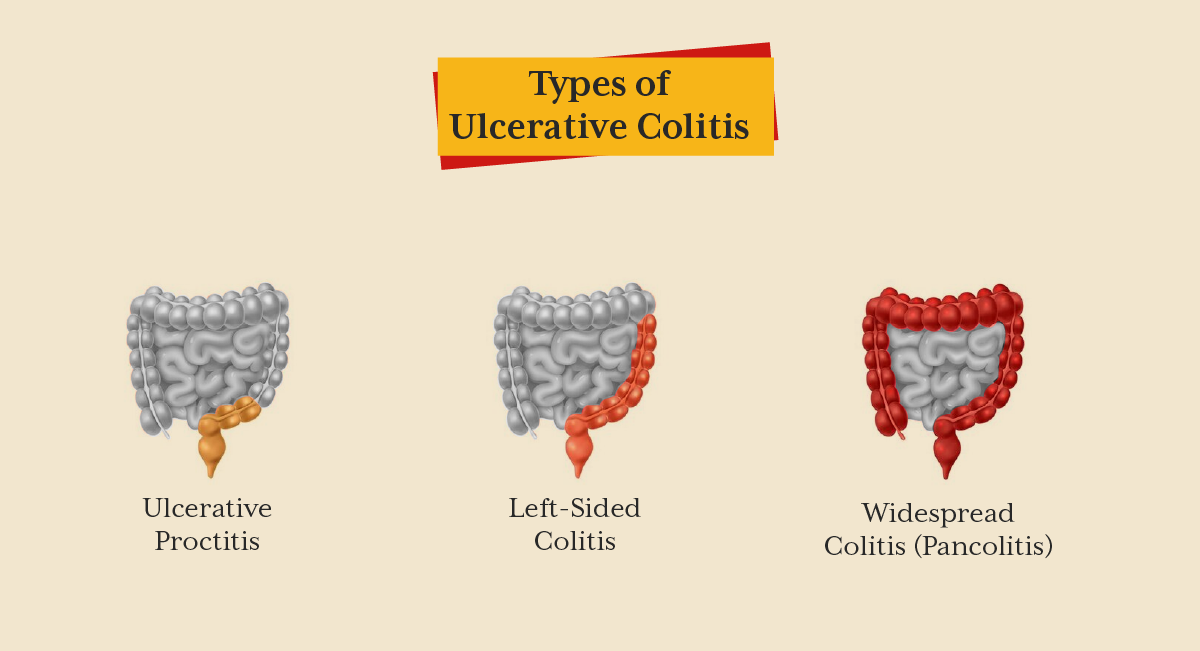
In this type, inflammation is limited to the rectum (the last part of your digestive tract). If you experience rectal bleeding, urgency, or difficulty passing stool, this could be your diagnosis.
Here, inflammation spreads from the rectum up through the sigmoid and descending colon. You may experience:
This is the most severe type of UC, affecting the entire colon. It often leads to:
One major theory is that an abnormal immune response plays a big role in Ulcerative Colitis. Normally, your immune system protects you from harmful bacteria and viruses. But in people with Ulcerative Colitis, the immune system mistakenly attacks the healthy cells in the digestive tract, leading to chronic inflammation.
If you have a family member with Ulcerative Colitis, your risk is higher. Scientists have found specific genetic markers linked to the condition. While genetics alone may not cause Ulcerative Colitis, it does make some people more susceptible.1
Certain environmental factors, such as infections, pollutants, and even lifestyle choices, may contribute to Ulcerative Colitis. While diet and stress do not cause the disease, they can definitely make symptoms worse.
When diagnosed with Ulcerative Colitis, the first thing most doctors do is prescribe medications. But do they really solve the problem? Or do they just suppress symptoms while creating new issues? Let’s take a closer look at the conventional treatment for Ulcerative Colitis and their drawbacks.
These are commonly given for mild to moderate Ulcerative Colitis symptoms. While they may reduce inflammation, they don’t stop the disease from progressing. Many people find themselves taking higher doses over time, leading to dependency without addressing the root cause of Ulcerative Colitis.
For moderate to severe Ulcerative Colitis flare-ups, corticosteroids like prednisone are often used. While they may provide quick relief, they come with serious side effects like weight gain, weakened bones, high blood sugar, and even dependency. Many patients end up feeling worse in the long run.
These drugs aim to calm down the overactive immune system, but they also leave your body defenceless against infections. If your immune system is already struggling, why weaken it further? Many people experience fatigue, nausea, and a higher risk of infections while on these drugs.
Biologics target specific immune pathways to reduce inflammation. But they don’t come without risks- serious infections, allergic reactions, and even increased chances of certain cancers have been reported. Plus, they’re incredibly expensive, making them an unsustainable long-term option for many patients.
When medications fail, doctors often suggest Ulcerative Colitis surgery as the next step. But surgery is not a cure, it comes with risks, complications, and a long recovery period. While some people do experience symptom relief, others struggle with post-surgical complications, digestive issues, and even the need for additional surgeries.

Unlike conventional medicine, which focuses on suppressing symptoms, Functional Medicine takes a root-cause approach to Ulcerative Colitis treatment. Instead of just calming inflammation, it identifies WHY the inflammation is happening in the first place and works on reversing it naturally.
Functional Medicine looks at the entire body, not just the gut. It considers factors like nutrition, gut health, stress, toxins, and lifestyle to create a customized healing plan. Instead of relying on medications with side effects, it focuses on real solutions that bring long-term relief.
Your gut microbiome plays a huge role in Ulcerative Colitis management. Instead of damaging the gut further with medications, Functional Medicine aims to restore balance naturally:
Living with Ulcerative Colitis can be overwhelming, but the right approach can change everything. We’ve explored different Ulcerative Colitis Treatment Options, including diet, medication, and lifestyle changes.
If you’re looking for a way to avoid surgery and manage your symptoms naturally, Functional Nutrition could be your best bet. Instead of just treating symptoms, it focuses on finding and fixing the root cause of your condition. With a personalized plan, you can improve digestion, reduce inflammation, and support gut healing without immediately jumping to Ulcerative Colitis surgery alternatives that may not be right for you.




.svg)
Have you been feeling constantly exhausted, even after a full night’s sleep or struggling with brain fog, anxiety, or unexplained body aches? You might be dealing with adrenal fatigue- a condition that throws your hormonal balance off track. While it’s not always recognised by mainstream medicine, thousands of people, especially women, experience relentless fatigue with no clear diagnosis.
In India, nearly 1 in 4 women report feeling weak or tired for months. Often, doctors prescribe iron or vitamin supplements, but is that enough? Adrenal fatigue and nutrition go hand in hand. The right foods for adrenal health can help restore energy, balance stress hormones, and improve overall well-being.1
Through a carefully planned adrenal fatigue diet, you can support your body naturally. Let’s explore the best ways to nourish your adrenal glands and reclaim your energy!
Your adrenal glands sit on top of your kidneys, quietly working to keep you energized and balanced. They produce essential hormones like cortisol, which helps manage stress, metabolism, and even sleep.
But when you're constantly under pressure- whether it’s work deadlines, poor sleep, or an unbalanced diet- your adrenals start overworking. Over time, they can get “burned out,” leading to hormonal imbalance and fatigue.


Your adrenal glands use a lot of Vitamin C to produce cortisol. When you're constantly stressed, your body depletes Vitamin C faster. Vitamin C reduces oxidative stress, supports adrenal function, and helps regulate cortisol. Replenish it with:
B- vitamins (especially B5 and B6) are essential for adrenal hormone production and energy metabolism. They help convert food into energy, making them CRUCIAL for beating adrenal fatigue and avoiding crashes. Load up on:
Stress depletes magnesium, and without enough, you might experience anxiety, muscle cramps, and poor sleep. Magnesium calms the nervous system, reduces stress, and supports hormonal balance. Consume:
Fats aren’t the enemy- they are ESSENTIAL for adrenal fatigue recovery and hormone production. Healthy fats keep your body fueled and reduce inflammation. These fats provide long-lasting energy, balance cortisol levels, and help your body heal from stress.
Protein is a MUST for adrenal support. It stabilizes blood sugar, prevents energy crashes, and provides amino acids needed for hormone production.
Unlike refined carbs (which increase blood sugar), complex carbs provide slow-releasing energy that keeps you going without the afternoon slump. Keeping blood sugar stable prevents adrenal exhaustion, mood swings, and sugar cravings.
Did you know your adrenals regulate sodium levels? When they’re fatigued, you might experience low blood pressure, dizziness, and salt cravings. Adding sea salt (in moderation) helps maintain electrolyte balance. It supports hydration, and electrolyte balance, and prevents dizziness from adrenal fatigue.

Foods loaded with white sugar- such as cakes, cookies, and candy, cause rapid blood sugar spikes, followed by crashes that leave you feeling drained and moody. These fluctuations put extra pressure on your adrenal glands, forcing them to produce more cortisol to balance your energy levels. Over time, this can lead to chronic fatigue, cravings, and hormonal imbalances.
Foods made with white flour, such as bread, pasta, and pastries, act similarly to sugar. They are quickly broken down into glucose, spiking blood sugar levels and forcing the adrenal glands to overwork. This can lead to fatigue, brain fog, and difficulty maintaining energy throughout the day. If you’re following an adrenal fatigue diet, swap white flour for whole grains like quinoa, millet, or buckwheat for steady energy.
Sodas, energy drinks, and even fruit juices packed with sugar might seem refreshing, but they do more harm than good. The combination of high sugar and caffeine overstimulates the adrenal glands, leading to cortisol imbalances and chronic exhaustion. Instead of sugary drinks, go for coconut water, herbal teas, or lemon-infused water to stay hydrated without the crash.
Fried and processed foods contain unhealthy trans fats that trigger inflammation, weight gain, and sluggish digestion, all of which negatively affect hormonal balance. Fast food, deep-fried snacks, and packaged meals are loaded with preservatives and additives that force the adrenals to work harder to detoxify the body, worsening symptoms of adrenal fatigue.
You might think switching to artificial sweeteners like aspartame or sucralose is a good idea, but they can trick your body into craving more sugar, leading to blood sugar imbalances and adrenal exhaustion. These chemicals also interfere with gut health, which plays a crucial role in adrenal fatigue and nutrition.
Did you know that achieving hormonal balance isn’t just about cutting out caffeine or getting more sleep, but rather about addressing the root cause with the right Adrenal Fatigue diet? This is where Functional Nutrition plays a crucial role. Instead of just masking symptoms, it helps nourish the body deeply, targeting imbalances at their core.
No two people experience adrenal fatigue in the same way. That’s why a one-size-fits-all diet won’t work. A functional nutrition approach starts by assessing your body’s unique needs, stress levels, and deficiencies. The goal is to create a sustainable, adrenal fatigue-friendly diet that focuses on whole, unprocessed foods to restore adrenal health.
Adaptogens are nature’s way of helping your body cope with stress—something your adrenal glands desperately need. These powerful herbs support cortisol balance, prevent burnout, and improve overall hormonal health.
Balancing your hormones is possible with the right guidance. Through Alive 2.0, restore your hormone health with the power of Functional Nutrition. Address the root causes, eliminate fatigue, and take charge of your well-being. Book a free consultation today and start your journey to vibrant energy!




.svg)
Have you ever felt constantly fatigued, struggled with digestive issues, or experienced unexplained joint pain? These could be signs of silent inflammation in your body. According to studies, over 5% of people with lower gastrointestinal symptoms in India suffer from inflammatory bowel disease (IBD).1
Hidden inflammation triggers like poor diet, pollution, toxins, and stress can keep your body in a constant state of fire, leading to chronic diseases such as diabetes, heart disease, and autoimmune disorders. In this blog, we will understand inflammation, its different triggers, and how to mitigate them.
Inflammation is your body’s natural defense mechanism. When you get injured or catch an infection, your immune system activates an inflammatory response to heal and protect you. This is called acute inflammation!
But when inflammation becomes long-term (chronic), it turns against your body instead of healing it. This is where the problem begins. Chronic inflammation quietly builds up in your system, damaging cells, tissues, and organs. It can take years to show clear symptoms, which is why it’s often called a silent killer.
Some of the most common autoimmune inflammatory conditions include:
Did you know that causes of chronic inflammation are directly linked to major lifestyle diseases? Chronic inflammation plays a key role in some of the most common long-term health problems, including:
Ignoring hidden inflammation triggers can have long-term consequences. Over time, chronic inflammation:

Consuming too much added sugar doesn't just affect your waistline; it can disrupt your gut health. Excessive sugar fosters the growth of harmful bacteria, leading to an imbalance known as gut dysbiosis. This imbalance has been linked to gastrointestinal disorders like irritable bowel syndrome (IBS) and inflammatory bowel disease (IBD). Moreover, a high-sugar diet can also cause glucose metabolism, and increase inflammation, further compromising your gut lining.2
While meat can be a source of essential nutrients, frequent consumption of processed and processed meats has been associated with an increased risk of chronic diseases. Studies have shown that a daily intake of 100 grams of processed meat can elevate the risk of stroke and certain cancers. Processed meats, even in smaller amounts, have been linked to higher risks of colorectal cancer and heart disease.3
Indulging in fried and ultra-processed foods might satisfy your taste buds, but these foods often contain advanced glycation end products (AGEs). AGEs are compounds that form when proteins or fats combine with sugars during high-heat cooking. Accumulation of AGEs in the body can lead to oxidative stress and inflammation, contributing to chronic health conditions.
Opting for artificial sweeteners as a sugar substitute might seem like a healthier choice, but some studies suggest they can disrupt the delicate balance of your gut microbiota. This disruption may lead to chronic low-grade inflammation and contribute to insulin resistance.
Avoid these inflammation-causing foods:

Every time you step outside, you're exposed to harmful air pollutants- fine particulate matter (PM2.5), carbon monoxide, nitrogen dioxide, and other toxins. When you breathe in these pollutants, they enter your lungs and bloodstream, triggering an immune response. Over time, this constant exposure leads to respiratory inflammation and other serious health conditions.
Signs of Silent Inflammation from Pollution
How to Protect Yourself from Inflammation Caused by Pollution
You may think your home is your safe space, but did you know that Chaetomium molds that look cottony in texture lurking in damp corners could be one of the biggest hidden inflammation triggers?
Mold releases microscopic spores into the air, which, when inhaled, can irritate the respiratory system and trigger the immune system’s inflammatory response. Over time, repeated mold exposure can cause chronic respiratory inflammation and lead to severe conditions like asthma, allergies, and even autoimmune disorders.
Signs of Silent Inflammation from Mold Exposure
How to Reduce Inflammation from Mold Exposure

Ever wondered why you feel sluggish, irritable, or even sick after a few nights of poor sleep? It’s because sleep deprivation increases pro-inflammatory cytokine production- a key factor in chronic inflammation.
Solution
Sitting for long hours might seem harmless, but did you know it can worsen inflammatory conditions? A sedentary lifestyle contributes to systemic inflammation by slowing down circulation, impairing metabolism, and increasing oxidative stress.
How Lack of Exercise Leads to Inflammation
Solution
We all know smoking is harmful, but it’s also a hidden inflammation trigger that accelerates damage to your cells and tissues.
How Smoking Increases Inflammation
Solution
Excess alcohol intake can wreak havoc on your health. Alcohol-induced tissue damage is a major driver of chronic inflammatory conditions, affecting the liver, gut, and brain.
Inflammatory conditions don’t just happen overnight- they build up silently due to hidden inflammation triggers like poor diet, lack of sleep, toxins, and stress. If you’ve been experiencing signs of silent inflammation- persistent fatigue, brain fog, bloating, or unexplained weight gain, it’s time to take action. Book a free consultation with iThrive today, and let our expert Functional Nutritionists help you find the root cause of your inflammation!


The blog covers functional nutrition, chronic conditions, gut health, hormonal health, autoimmune conditions, sleep, mental health, and root cause analysis. Every article is written to help you understand what is actually happening inside your body, not just manage symptoms.

All articles are written by the content writers in collaboration with iThrive's clinical team of functional nutritionists, guided by the same methodology used in the ALIVE programme. The content is rooted in functional medicine and real clinical experience, not generic health advice.

No. The blog is an educational resource to help you understand your health more deeply. If you are experiencing symptoms or managing a chronic condition, a personalized Root Cause Analysis with a functional nutritionist is the right next step.

Book a Root Cause Analysis. For ₹2,500, a dedicated functional nutritionist will assess 60+ blood markers using optimal ranges and explain exactly what is driving your condition. It is the natural next step after reading about what might be happening in your body.

Yes. Many of our readers come with existing diagnoses and find the blog helps them understand why their condition developed and what their body actually needs. The articles are designed to give you clarity, not replace the guidance of a practitioner.



